Vitamin D in The Treatment of Breast Cancer
Vitamin D in The Treatment of Breast Cancer
By Maria Cayelli. Dr. Cayelli is Family Medicine Specialist, Anderson, SC; she reports no financial relationships relevant to this field of study. This article was first published in the August 2008 issue of Alternative Therapies in Women's Health.
An estimated 182,460 new cases of invasive breast cancer, and approximately 40,930 breast cancer deaths (40,480 women, 450 men), are expected to occur among women in the United States during 2008.1 While breast cancer in men is rare, breast cancer is the most frequently diagnosed cancer in women, ranking second among cancer death in women.1 In light of this, many factors have been studied in relation to altering breast cancer risk.2 Breast cancer is a multifactorial disease. While the cause of breast cancer is not completely understood, the major risk factors are being a woman, family history, increasing age, age of menarche, age of menopause, age of first live birth, use of oral contraceptive pill, and hormone replacement.3 Prevention may be based on a healthy lifestyle including diet and exercise.1
Normal body cells grow, divide, and die in an orderly fashion, replacing worn out or injured cells.1 Cancer cells have damaged DNA that makes it evolve abnormally.1 Vitamins, which are nutrients that must be ingested through diet, may play a role in the possible prevention of breast cancer.4 Decreased intake of certain vitamins have been implicated in an increased risk of chronic diseases.4 Calcium and vitamin D have anticinogenic properties that have been studied related to breast cancer.5
Calcium
Calcium is a vital mineral with several important functions in bone and muscle health.6 In adults, 99% of calcium is found in bones and teeth, while the rest is in the blood and extra cellular fluid.6 Blood levels of calcium is helped regulated by vitamin D 1,25 dihydroxyvitamin D via a feed back loop.2 Calcium anticarcinogenic properties include regulating cell proliferation and differentiation.2
Calcium Source
Supplements and dairy products are the main calcium source for humans.2 Other foods high in calcium include sardines, salmon, kale, Chinese cabbage, broccoli, and calcium fortified foods.6
Clinical Effect of Calcium
Abbas et al found a moderate risk reduction for premenopausal breast cancer associated with higher dietary calcium intake but was not statistically significant.7 In a prospective cohort study of 7,847 women, Almquist et al found an insignificant inverse relationship between serum calcium levels and premenopausal breast cancer risk.8 High calcium levels were positively related to increased breast cancer risk in overweight peri/postmenopause women.8 McCullough et al found a moderate risk reduction breast cancer with high calcium intake and low fat dairy products in postmenopausal women.5 In addition, McCullough et al found intake of calcium was inversely related to estrogen receptor (ER) positive tumors but not ER negative tumors.5
Vitamin D
Vitamin D is a fat soluble vitamin metabolically inter related to calcium.2,4 Vitamin D status depends on sun exposure, leading to its skin synthesis as well as dietary intake.8 With adequate mounts of sun exposure, vitamin D3 (cholecalciferol) is produced in the skin from 7-dehydrocholesterol.4 Vitamin D3 is then metabolized into 25-hydroxyvitamin D in the liver.4 In the kidney, 25-hydroxyvitamin D is converted into 1,25-dihydroxyvitamin D.4 This vitamin D active metabolite inhibits cellular proliferation of breast cancer cells mainly through binding to a nuclear vitamin D receptor (VDR) and induce differentiation of malignant breast cells.2,4,7 25-hydroxyvitamin D may also circulate to breast tissue and be locally converted to 1,25 dihydroxyvitamin D, which then exerts its anticarcinogenic actions.2
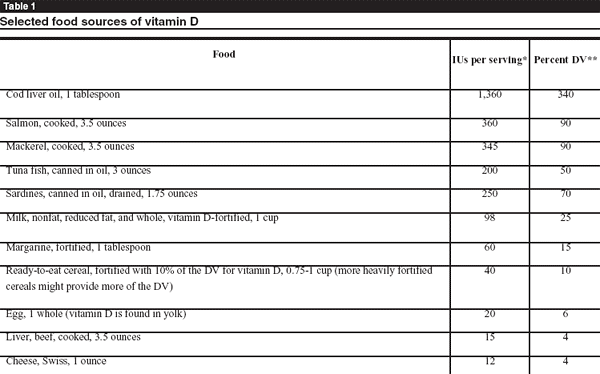 |
Vitamin D Source
Although diet plays a role, the main source of vitamin D in humans is sun exposure.9 A daily ten-minute unprotected sun exposure of hands and face may be sufficient to maintain adequate levels of vitamin D.10 In the United States, the dietary source of vitamin D are vitamin D fortified dairy products, orange juice, fish, eggs, and supplements.2 Vitamin D3, which is more efficient in raising the levels of the active metabolites, comes from animal sources, and vitamin D2 is synthetically made from plants.2,4
Clinical Effect of Vitamin D
According to the National Health and Nutrition Examination Survey Epidemiologic Follow-up Study, there was no statistically significant association between dietary and supplemental vitamin D intake and breast cancer.11 Overall, Bertone et al also found insignificant inverse association between plasma levels of 25(OH)D and breast cancer risk.12 However, Bertone et al concluded that postmenopausal women, and older women (> 60-years-old) with higher levels of vitamin D, may be at lower risk for breast cancer.12
On the basis that vitamin D3 status is predominately correlated to sun exposure, Robsahm et al studied the effect of solar-induced vitamin D levels on the prognosis of breast, colon, and prostate cancer. Robsahm et al found that the highest endogenous cutaneous synthesis of vitamin D was associated with the lowest risk for cancer death. In addition, the highest survival rate was with those who were diagnosed during the fall.10
Garland et al assessed the association between the serum levels of 25(OH)D and breast cancer risk through a pooled analysis of two studies involving 1,760 individuals.13 They found at levels of 52 ng/mL (corresponding to an intake of 4000 IU a day), there was a 50% lower risk of breast cancer.13 Lowe et al had similar results, reporting a significant association of low vitamin D levels with breast cancer risk in the United Kingdom Caucasian population.14 Colston et al found that lower serum levels (less than 50 nM) of vitamin D was associated with five times the risk for breast cancer than those with over 150 nM.3
In trying to find the link between vitamin D and breast cancer, studies have looked at the VDR and its link to certain types of cancer.14 Lowe et al and Colston et al found that polymorphisms in the VDR may increase risk of breast cancer.3,14 In addition, both studies found a greater risk of breast cancer with the combination of lower vitamin D levels and VDR polymorphism.3,14
High intake of dietary vitamin D was associated with a significantly decreased risk of developing breast cancer in premenopausal women.7,15,16 Up to age 69 in women, Knight et al found an inverse association between vitamin D intake and breast cancer.15
In postmenopausal women, Robien et al found a lower incidence of breast cancer with vitamin D intake of greater than 800 IU a day than with less than 400 IU a day.17 Shin et al found, among premenopausal women with more than 500 IU a day of vitamin D intake, a lower risk for breast cancer.16 They also found significantly lower incidence of in situ breast cancer with higher total vitamin D intake.17
Adverse Effect
Vitamin D is generally well tolerated, but toxicity can occur causing nausea, vomiting, poor appetite, weakness and weight loss.6 Excess intake of vitamin D can lead to hypercalcemia. Hypercalcemia may lead to impaired kidney function and decreased absorption of other vitamins and minerals.6
Conclusion
The results of epidemiologic studies of vitamin D and calcium intake and breast cancer risk are inconsistent. Vitamin D and calcium are metabolically inter-related, and may have anticarcinogenic properties. Limited research shows an inverse relationship between vitamin D and the risk of breast cancer in premenopausal women. In postmenopausal women, vitamin D and calcium may play a role in decreasing the risk of breast cancer.
Recommendation
Adult women older than 50-years-old are recommended to ingest a total of 1200 mg calcium (dietary and supplemental). The current adult upper limit of vitamin D3 is 2000 IU/day.6
References
1. Cancer facts and figures 2008. American Cancer Society; 2008
2. Cui Y, Rohan TE. Vitamin D, calcium, and breast cancer risk: a review. Cancer Epidemiol Biomarkers Prev. 2006;15:1427-1437.
3. Colston KW, et al. Vitamin D status and breast cancer risk. Anticancer Res. 2006;26:2573-2580.
4. Zhang SM. Role of vitamins in the risk, prevention, and treatment of breast cancer. Curr Opin Obstet Gynecol. 2004;16:19-25.
5. McCullough ML, et al. Dairy, calcium, and vitamin D intake and postmenopausal breast cancer risk in the Cancer Prevention Study II Nutrition Cohort. Cancer Epidemiol Biomarkers Prev. 2005;14:2898-2904.
6. Diet Supplement Fact Sheet: Calcium. Vitamin D. Office of Dietary Supplements. National Institute of Health.
7. Abbas S, et al. Dietary vitamin D and calcium intake and premenopausal breast cancer risk in a German case-control study. Nutr Cancer. 2007;59:54-61.
8. Almquist M, et al. Serum calcium and breast cancer risk: results from a prospective cohort study of 7,847 women. Cancer Causes Control. 2007;18:595-602.
9. Bertone-Johnson ER. Prospective studies of dietary vitamin D and breast cancer: more questions raised than answered. Nutr Rev. 2007;65:459-466.
10. Robsahm TE, et al. Vitamin D3 from sunlight may improve the prognosis of breast-, colon-, prostate cancer (Norway). Cancer Causes Control. 2004;15: 149-158.
11. John EM, et al. Vitamin D and breast cancer risk: the NHANES I Epidemiologic follow-up study, 1971-1975 to 1992. National Health and Nutrition Examination Survey. Cancer Epidemiol Biomarkers Prev. 1999;8:399-406.
12. Bertone-Johnson ER, et al. Plasma 25-hydroxyvitamin D and 1,25-dihydroxyvitamin D and risk of breast cancer. Cancer Epidemiol Biomarkers Prev. 2005;14: 1991-1997.
13. Garland CF, et al. Vitamin D and prevention of breast cancer: pooled analysis. J Steroid Biochem Mol Biol. 2007;103:708-711.
14. Lowe LC, et al. Plasma 25-hydroxy vitamin D concentrations, vitamin D receptor genotype and breast cancer risk in a UK Caucasian population. Eur J Cancer. 2005;41:1164-1169.
15. Knight JA, et al. Vitamin D and reduced risk of breast cancer: a population-based case-control study. Cancer Epidemiol Biomarkers Prev. 2007; 16:422-429.
16. Shin MH, et al. Intake of dairy products, calcium, and vitamin D and risk of breast cancer. J Nat Cancer Inst. 2002;42:243-251.
17. Robien K, et al. Vitamin D intake and breast cancer risk in postmenopausal women: the Iowa Women's Health Study. Cancer Causes Control. 2007;18:775-782.
An estimated 182,460 new cases of invasive breast cancer, and approximately 40,930 breast cancer deaths (40,480 women, 450 men), are expected to occur among women in the United States during 2008.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
