"My Heart's Pounding and Skipping": Evaluation and Management of Palpitations in the Emergency Department
"My Heart's Pounding and Skipping": Evaluation and Management of Palpitations in the Emergency Department
Authors: Corey D. Harrison, MD, Assistant Professor, University of Massachusetts Medical School, UMass Memorial Medical Center, Worcester, MA; and Nicholas Itzin, MD, Resident Physician, University of Massachusetts Emergency Medicine Residency, UMass Memorial Medical Center, Worcester, MA.
Peer Reviewer: Donald H. Schreiber, MD, FACEP, Associate Professor of Emergency Medicine, Stanford University School of Medicine, Palo Alto, CA.
I have long remembered something a wise old cardiologist told me when I was a naïve medical student. I was greatly excited because I had a patient who was having lots of ventricular ectopy. I was sure that this was a problem that needed extensive evaluation and treatment. I went to the textbook and read about ectopy. I learned about the various drug treatments advocated at the time. I carefully planned my typical medical student presentation for him. The kind, you recall, that considers everything important and has no focus, right? Well, after my erudite presentation, the attending, who happened to be a cardiologist trained in the pre-interventional era, sat back and said, "Son, remember the heart is not a chronometer."
That concept has stuck with me ever since. Our heartbeats are not regular; they are naturally irregular. How irregular, to what degree, and what distinguishes the normal irregularity from the harmful irregularly? The symptom of palpitation, or awareness of one's own heartbeat, is a common symptom and will occasionally bring patients into the emergency department. It is important to the emergency physician to be able to evaluate these patients, identify serious cardiac arrhythmias, and assess who is at risk for complications. This review focuses on the serious disorders that can present with palpitations.
J. Stephan Stapczynski, MD, Editor
Case Examples
A 50-year-old man, with a past medical history of anxiety, presented to the emergency department complaining of palpitations and was brought urgently from triage because he reported recently having episodes of ventricular tachycardia that felt similar to this current sensation. On the cardiac monitor, there was monomorphic wide complex tachycardia at a rate of 120/minute. The blood pressure and level of consciousness were intact. The patient reported his symptoms started while doing yard work. All of his previous episodes were related to exertion. A review of his electronic medical records reveals that this individual was diagnosed very recently with arrythmogenic right ventricular dysplasia, and was scheduled for elective ICD placement. While waiting for the cardiology consultant to call back, the patient had a witnessed loss of consciousness and was synchronously electrically converted to sinus rhythm.
A 16-year-old male was brought in by ambulance after a witnessed collapse with loss of consciousness while at hockey practice. After five seconds of unconsciousness, the patient awoke and was asymptomatic thereafter. Upon questioning, he reported a sense of "fast pounding" in his chest for several seconds before fainting. The family history was significant for the sudden, unexplained death of a maternal uncle in his 20s. The patient had undergone a routine athletic pre-participation physical three months earlier and was cleared for all activities. In the ED, the vital signs and physical examination were unremarkable, but his electrocardiogram revealed an abnormally prolonged corrected QT interval of 0.505 seconds.
A 34-year-old female smoker with no medical history presented complaining of palpitations and shortness of breath. The patient described the sensation as "heart racing" and "skipping beats" that were gradual in onset and had partially resolved after three hours without therapy. The heart rate was 105/min, respiratory rate 28/min, and blood pressure and temperature were normal. The ECG was significant for sinus tachycardia with rare PVCs. On interview, the patient reported drinking more than seven cups of coffee that morning to make up for a night with little sleep. After one hour in the ED, she reported complete resolution of symptoms, and a recheck of vital signs revealed a heart rate of 70/min and respiratory rate of 12/min.
Introduction
The variability of experiences that constitute palpitations, and the expanse of potential etiologies, creates a diagnostic dilemma. The chief complaint of palpitations is neither sensitive nor specific for any diagnosis, including cardiac dysrhythmias. However, as a possible symptom of serious rhythm disturbance, the presentation requires a careful evaluation by emergency physicians (EPs). Therefore, palpitations are a high-priority chief complaint. The lengthy differential diagnosis demands vigilance on the part of physicians to consider all etiologies, including non-cardiac ones. Like dysrhythmias, many non-cardiac causes may also be associated with significant immediate and long-term risk.
Palpitations are defined as an abnormal awareness of one's own heartbeat, sometimes described as extra forceful and/or irregular. Up to 16% of all medical patients report palpitations.1 In a prospective study of the etiology of palpitations in general medical settings, 43% were attributed to a cardiac cause, 31% psychiatric, 10% extra-cardiac medical, and 16% remained undiagnosed after one year.2 The most frequent cardiac causes were atrial fibrillation/flutter, supraventricular tachycardia (SVT), and ventricular ectopic beats (PVCs). Panic attacks or panic disorders with anxiety were more frequently observed than any single cardiac diagnosis. The subgroup of patients presenting to the ED had a significantly higher percentage of cardiac diagnoses (47%) than those presenting to other sites. One-year mortality (1.6%) compared favorably with an earlier retrospective study,3 which suggested that palpitations alone are not an independent risk factor for increased cardiac morbidity or overall mortality. Among pediatric patients, cardiac pathology is less often (6%) implicated as the cause of palpitations.4 However, in a study of pediatric patients with documented dysrhythmias, 28% had at an earlier time noted palpitations, and a significant time interval usually took place between symptom onset and diagnosis.5
In the ED, the focus is on the appropriate triage of the presenting population such that resuscitation measures and resource use is directed toward those most likely to suffer morbidity or death. Nearly 700,000 Americans die from cardiovascular disease each year, and approximately half of these patients will die suddenly.6,7 A majority of those sudden cardiac deaths are precipitated by acute ventricular dysrhythmias due to coronary artery disease, which underscores the importance of screening presentations for that potential. In addition, palpitations in the presence of other specific symptoms can be diagnostic for panic attacks and disorder, which carries a greater than 90% association with other psychiatric diagnoses including, most significantly, depression and suicide.8,9
Basis for Symptom Perception
Palpitations present as variable sensations described as heart racing, beating irregularly, pounding, flip-flopping, or skipping one or more beats. The symptom onset and termination may be insidious, and the palpitations may be intermittent or constant. Associated symptoms can be variable and are usually non-specific for any single diagnosis.
From a cardiac standpoint, symptom perception can be addressed as a sense of change in rate, rhythm, and/or stroke volume. Report of a rapidly beating heart may be differentiated from the increased sensitivity to heartbeat perception, often by direct questioning. Increased sensitivity to perception has been distinctly associated with anxiety disorders and hypochondriasis.10 During evaluation, a patient's clear description of rapid rate should provoke the qualification of regularity.11 (See Table 2.) Visceral sensation is, by nature, imprecise, and at abnormally fast or slow heart rates it may become more difficult for patients to accurately describe their symptoms. For these reasons, a patient's description of palpitations as regular or irregular is not always diagnostically useful. Additionally, benign ectopic contractions can cause a sense of irregularity in an otherwise regular rhythm.
 |
Assuming an accurate interpretation of visceral sensations, adequate ventricular contractile function is physiologically necessary to sense palpitations,11 which suggests a mechanically or afferently modulated basis for perception. Potential explanations include the impact of ventricular muscle against the thoracic wall or the presence of pulse-pressure waves in the vasculature. Historical studies have demonstrated decreases in systolic arterial pressure and mean cardiac index as high as 29% and 38%, respectively, during episodes of iatrogenic supraventricular tachycardia (SVT).12 The decrease in perfusion pressure, elevation in pulmonary artery pressure, and a decreased relative diastolic interval, potentially explains the often-associated report of lightheadedness, weakness, dyspnea, and chest pain. Patients occasionally report a sense of palpitations in their neck that may be explained by jugular venous distension and pulsations against closed tricuspid valves in the presence of atrial-ventricular dissociation.13
The acute evaluation of patients with palpitations centers on distinguishing true, pathologic cardiac rhythm disturbances from sinus tachycardia or non-cardiac etiologies. Because the mechanism of non-cardiac palpitations is not clear, the absence of identifiable electrical or mechanical cardiac abnormalities creates an opportunity for missed diagnosis, especially when a psychiatric disorder is suspected. Individuals whose sensations represent normal heartbeats are more likely to carry previously established psychiatric diagnoses, and those ultimately found to have a dysrhythmia are less likely to carry those affiliations.10,14 Separate studies have established that the persistent presence of palpitations over months to years is associated with a tendency to amplify normal bodily sensory information combined with a relative increase in minor daily stressors.15 The risk of erroneously attributing a patient's symptoms to anxiety or stress is enhanced by the fact that many patients are evaluated after their palpitations have spontaneously resolved. In a retrospective study of patients with proven paroxysmal SVT, 67% were found to meet criteria for panic disorder.16 A presumably erroneous attribution of symptoms to panic, anxiety, or stress was made in half of those individuals.
Differential Diagnosis
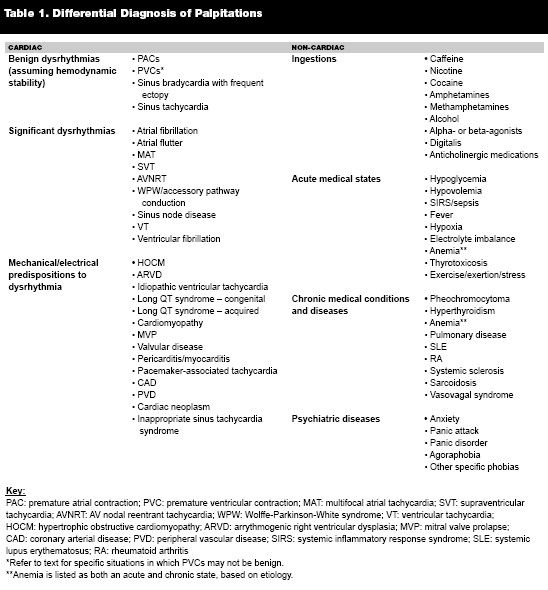
Predictably, the clinical differential for palpitations is broad and complex. (See Table 1.) That complexity may be restrained by appropriate attention to patient characteristics and scenario. The ED presentation should be differentiated by suspicion for cardiac versus non-cardiac etiology. This designation can be reached by a combination of vital signs, historical risk profiles, physical examination, and the electrocardiogram (ECG). Apart from management of vital sign instability or serious associated symptoms, the most important role for the EP is appropriate, discerning use of specialty consults, referrals, and diagnostic testing.
 |
Palpitations of cardiac origin are most safely considered symptomatic of potentially unstable dysrhythmias until proven otherwise. The results of numerous adult studies have been unable to differentiate between atrial fibrillation and SVT as the most frequently responsible significant dysrhythmia.2,17 The most common dysrhythmia in pediatric patients is SVT.5,18 Although markedly less common, wide complex tachycardias should always be considered and ruled out, especially in circumstances of congenital or acquired conditions such as long QT syndrome, arrythmogenic right ventricular dysplasia, cardiomyopathy of any cause, and ventricular myocardial scarring from previous infarction. The presence of an accessory conduction pathway should be seriously considered in cases of SVT as well as wide-complex tachycardia. Management of individual dysrhythmias and any associated symptoms or vital sign instability should be expedient and, when available, in consultation with cardiology and critical care specialists.
Premature contractions of ectopic origin are the most common cardiac cause of palpitations.2 Hypokalemia, hypomagnesemia, hypoxia, catecholamine excess from stress or exertion, and sinus bradycardia increase the likelihood for ectopy. A history of coronary or peripheral19 arterial disease, myocardial infarction, valvular disease, cardiac neoplasm,20 autoimmune rheumatic diseases21 (specifically lupus and systemic sclerosis), or sarcoidosis suggests the presence of a myocardial ectopic focus. A history of mitral valve prolapse (MVP) is of particular concern, as this condition has been repeatedly linked to a host of dysrhythmias ranging from benign ectopy to ventricular fibrillation.22
Premature atrial contractions (PACs) may be isolated and benign, or may be the inciting event in atrial fibrillation or SVT. PVCs have been identified on up to 1% of all ECGs, and have been noted on 40-75% of healthy patients on ambulatory monitoring over 24-48 hours.23 Despite their high prevalence, certain cases should provoke the attention of EPs. In the setting of moderate-severe left ventricular dysfunction, with ejection fractions less than 40%, frequent PVCs have been associated with an increased risk of sudden death.24,25
Specific patterns of ventricular ectopy, loosely termed "complex" PVCs, might signify a higher risk of dangerous ventricular dysrhythmia.26 The most notable examples of complex PVCs are multiple consecutive beats, bigeminy, trigeminy, and the R-on-T phenomenon, whereby a strategically placed PVC could incite polymorphic wide complex tachycardia. While follow-up studies have disputed the idea of complex PVCs as a harbinger of ventricular fibrillation (VF) or ventricular tachycardia (VT),24 their presence, especially in individuals with left ventricular systolic dysfunction, should be considered a high-risk characteristic. While normally not requiring intervention, treatment with lidocaine, beta-blockade, or amiodarone may be indicated in patients with acute coronary syndrome.27 Ventricular ectopy is otherwise not associated with adverse outcomes,28 and suppressive therapy is not indicated.
Sinus tachycardia (ST) may present as palpitations. Evaluation of asymptomatic patients for self-limited episodes and associated circumstances many times implicates ST, which is often confirmed by outpatient monitoring.11,27 Many non-cardiac diseases and drugs cause ST, including ingestion/use of caffeine (especially large ingestions),29 cocaine, and other sympathomimetics, including ecstasy.30 Additionally, ST may be a manifestation of anemia, systemic inflammatory response, shock, fever, infection, hypoglycemia, thyrotoxicosis,31 catecholamine-producing neoplasms,32 and histamine-release due to various mechanisms (including mastocytosis,33 scombroid poisoning,34 and anaphylaxis35). In these cases, ST is an appropriate physiologic response and generally part of a more specific constellation of signs and symptoms. Careful analysis of the history of present illness, patient status, and any associated symptoms or abnormalities should direct the evaluation. Additionally, ST may result from an inappropriate physiologic response, such as postural orthostasis,36 or inappropriate sinus tachycardia, an extremely rare hypersensitivity to beta-adrenergic stimulation.37
A history of exercise or exertion has particular influence on the differential diagnosis. While ST is the normal physiologic response, exercise-induced ventricular dysrhythmias have been observed in both adults and children as a result of structural abnormalities such as hypertrophic obstructive cardiomyopathy (HOCM)38 or arrythmogenic right ventricular dysplasia (ARVD),39 electrical abnormalities such as congenital prolonged QT syndrome,27,40 or without any discernable abnormality.41 Furthermore, the presence of increased ventricular ectopy after exercise termination has been linked with increased mortality.42 Symptoms during exercise and the post-exertional period have also been linked to paroxysmal atrial fibrillation.43
More than 25% of individuals will experience at least one panic attack in their lifetime, and palpitations are the most frequently reported symptom.44 Panic attack or panic disorder with anxiety is the final diagnoses for a large number of those presenting, meaning many patients will not demonstrate a biological or electrical constellation of signs and symptoms. A host of individual and inter-related psychiatric acute-state and long-term conditions have been implicated. Unfortunately, a specific psychiatric diagnosis is usually impossible to assign in the ED. In concert with an appropriate medical evaluation, which often requires months, appropriate definitive mental health referral can be arranged. Basic psychiatric screening and nonspecific referral, however, should always be undertaken in the ED and is most relevant for individuals with potential for depression and suicidality.
Patient Assessment
The interview and physical examination of patients in the ED should occur simultaneously with arrangements for appropriate cardiac rhythm monitoring and intravenous access. As information becomes available from the encounter, it might be necessary to scrutinize the ECG or focus the physical examination for specifics. Depending on patient stability and electrical findings, therapeutic intervention might take precedence over a thorough interview, which can be done after stability is assured.
A complete historical assessment includes detailed circumstances and specifics of the presentation, with the aim of identifying factors that increase the likelihood of serious pathology. Independent of objective data, which might not be abnormal in the event of a resolved episode, symptom characteristics have historically been used to guide the initial evaluation. Interpersonal variability in the perception and description of palpitations often limits the value of subjective expression. Nevertheless, attempts have been made to classify certain symptom descriptors and patterns with regard to corresponding dysrhythmias. (See Table 3.)11,27 Twelve-lead electrocardiography and continuous telemetry are generally more specific and necessary corollaries.
 |
A sensation of "flip-flopping" or "skipping beats" is thought to be clinically indicative of premature ectopic contractions. PVCs are many times associated with a pause and forceful ventricular contraction resulting from prolonged diastolic filling, which may explain the sensation. The presence of PVCs on monitoring, especially if correlated with the experience of palpitations, should prompt a review for high-risk characteristics and the need for treatment. Conversely, treatment is rarely indicated for PACs.
Rapid fluttering or beating in the chest might signify either atrial or ventricular tachydysrhythmia, or sinus tachycardia of any etiology. If noted to be irregularwhich can be elicited by having the patient tap or clap out the sensed rhythmsuspicion for atrial fibrillation with rapid ventricular response is increased. A similar experience could result from variable atrial-ventricular conduction patterns or frequent ectopy. Regularity suggests ST, SVT, or VT, but is a sensation of limited value without ECG findings.
A sense of "pounding in the neck," with or without chest palpitations, should provoke concern for atrial-ventricular dissociation with simultaneous contraction against closed atrial-ventricular valves. Resultant regurgitation to the systemic veins leads to a transmission of symptoms to the neck. Prolonged jugular reflux causing bulging in the neck has been termed the "frog sign." Electrophysiologic studies have demonstrated a symptomatic association with AV nodal reentrant tachycardia.13 VT can also result in an irregular AV dissociation with intermittent neck symptoms. For patients with an accessory pathway, there is thought to be an interval between chamber depolarization, and therefore an absence of reflux. As a result, the complaint of neck palpitations should occur less frequently among these individuals.
Modes of onset and termination are probably less helpful for palpitations than for evaluating other symptoms. It has been thought that an abrupt onset is more consistent with dysrhythmias; however, paroxysmal SVT and VT can be preceded by a progressive sense of palpitations, and ST has been observed to start suddenly. Likewise, an acute dysrhythmia is often associated with a period of ST after resolution, complicating the perception of symptom cessation.
Patient and event circumstances will direct the evaluation more effectively than symptom description. A complete, specific review of illicit and prescribed drugs, caffeine, and nicotine use is important for the consideration of toxidromes and assessment of cardiac risk. The review of systems may reveal coincident features that suggest systemic diseases such as infection, systemic inflammatory response, hyperthyroidism, pheochromocytoma, and vascular disease. As previously mentioned, a patient report of symptom onset during or shortly after exercise is concerning, and that report alone justifies a cardiology specialist consult and/or monitored observation. In later life, any precipitant of acute myocardial ischemia should be considered a risk factor for the development of fatal dysrhythmias.25 At any age, congenital cardiac and electrophysiologic abnormalities may associate exertional palpitations with dysrhythmias and sudden death, so an accurate family history, including any unexplained deaths at young ages, is important.45
The most common cause for sudden death in young people and athletes in this country is HOCM. A positive or negative family history of HOCM is often difficult to interpret clinically because of heterogeneous expression.38 Abnormalities of the right ventricle, such as arrhythmogenic right ventricular dysplasia (ARVD), are temporally progressive in manifestation. Young people may present with exertional dysrhythmia and no echocardiographic abnormality, and adults may go undiagnosed for decades before presenting with exercise-related VT.39 Congenitally acquired long-QT syndrome links episodes of polymorphic VT with catecholamine excess and tachycardia that may develop from exertion or emotional stress. However, acquired long-QT syndrome is thought to link slower heart rates with VT, and therefore therapy with beta-blockers or calcium channel antagonists for the misdiagnosed former disorder could actually precipitate the latter.27
Palpitations associated with pre-syncope and syncope are particularly ominous regardless of circumstance, and even more so for individuals with known cardiomyopathy. The American College of Emergency Physicians standards for the evaluation of syncope highlight signs and symptoms of heart failure as evidence of high risk.46 Consciousness is thought to be indicative of retained cardiac output in the face of dysrhythmia. Patients presenting with concomitant dysrhythmia and syncope should be attended closely. The EP can assume that there is either poor ventricular function limiting stroke volume or that depolarizing rates have exceeded levels that could be autonomically managed, or both.
If SVT is present, systemic symptoms are less likely associated with mechanical failure and more likely associated with advanced rates. Extremely high rates are suggestive of accessory AV pathway conduction (due to absence of AV nodal delay), which requires immediate and long-term management. A notable exception is syncope at the onset of SVT, which could reflect acute-phase autonomic vasodilation. This possibility should not deter the EP from focusing on more life-threatening possibilities.12 If palpitations with or without syncope are found to be related to ventricular dysrhythmia, prompt intervention and specialty evaluation are indicated.
Diagnosis can be suggested by physical examination alone, especially in the instance of systemic non-cardiac illness and toxidromes. Fluctuations in levels of consciousness and orientation should arouse suspicion for blood glucose abnormality, systemic inflammatory response, intoxication, or profound cardiac disease. A head-to-toe assessment is indicated to rule out causes of appropriate ST, such as focal infection. Cardiac auscultation should reveal rate and rhythm abnormalities, and identify murmurs related to various pathologies such as MVP. Lung auscultation might reveal a single focus of infection or diffuse findings consistent with pulmonary edema. The presence of wheezing suggests that the patient may have recently used inhaled bronchodilators, which stimulate cardiac activity. Vascular abnormalities such as peripheral edema and jugular venous distention are important indicators of heart failure. Simultaneous palpation of pulse and observation of monitored rhythm might reveal electro-mechanical dissociation that suggests AVNRT or VT. Skin examination will reveal findings related to perfusion deficits, superficial infections, histamine-related pathology, or prior vascular procedures. Suicidal and homicidal ideations must be screened. Above all, constant and repeated attention must be paid to heart rate, blood pressure, oxygenation, and level of consciousness.
Laboratory Studies, Imaging, and Electrocardiography
Laboratory analysis and imaging in the ED should be directed by an appropriately constructed differential diagnosis. Many ED laboratory results, with the exception of electrolyte, drug, or glucose levels, generally will not rule out acute disease. However, based on each patient's individual risk factors, laboratory results may be necessary for the initiation of further work-up and accuracy of disposition. Biomarkers for cardiac ischemia, congestive heart failure, and end-organ ischemia are useful in appropriate patients. Such usefulness is dependent on suspicion for specific disease, and no single test, other than an ECG, is indicated for every patient with palpitations.
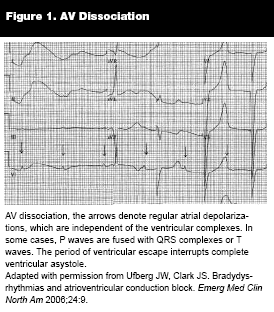
Twelve-lead ECG and prolonged rhythm strips are necessary for diagnosis or exclusion of cardiac dysrhythmia. The approach to ECG interpretation should be reproducibly systematic, beginning with rate and rhythm assessment. Bradycardia weakly suggests the patient's palpitations may be due to ectopy. In all cases of bradycardia, special attention should be paid to rule out AV nodal block or dissociation with escape rhythms. (See Figure 1.)47-49 Severe bradycardia may unpredictably alternate with rapid ventricular rate in cases of sinus node disease. (See Figure 2.)49 Tachy-dysrhythmias are traditionally categorized by QRS duration, which nonspecifically suggests whether the rhythm is supraventricular (narrow complex) or ventricular (wide complex).
 |
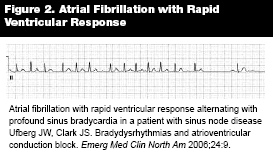 |
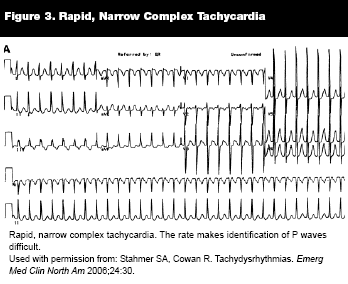
Assessment of SVT is dependent on the nature of P waves for differentiation between fibrillation/flutter and re-entrant mechanisms. A rapid rate often makes elucidation of P waves difficult (see Figure 3),47,50 if not impossible. In some cases, unless suspicion for conduction through an accessory pathway exists, pharmacologic slowing of rate or blockage of the AV node is helpful for rhythm identification. Wide-complex rhythms are generally indicative of VT or SVT with aberrancy (including accessory pathway conduction). Often, these two entities are difficult to distinguish from one another. The appearance of this rhythm, however, is ominous, and the patient's vital signs and evidence of peripheral perfusion should be watched closely.
 |
Wolffe-Parkinson-White syndrome is a specific condition marked by the presence of an accessory conduction pathway between the atria and ventricles. The ECG criteria for accessory pathway identification include PR interval less than 0.12 seconds, QRS interval greater than 0.1 seconds, and slurred upstroke morphology at the QRS complex (delta waves).47,48,50 Additional factors suggestive of this pathology include heart rate above 200/min (in adults) and irregular wide complex tachycardia.27,51 In the presence of antegrade accessory-pathway conduction, the use of medications that block the AV node such as adenosine may result in a decompensation to VF.27
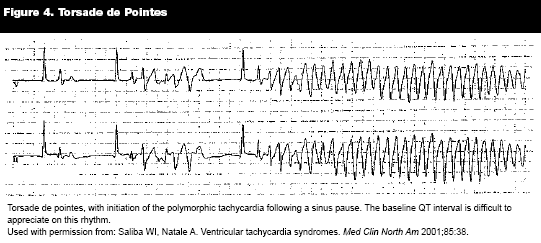
The QRS, QT, and T wave axis, intervals, and morphology should be scrutinized to diagnose primary cardiac pathology. This can range from acute ischemia to congenital structural heart disease. (See Table 4.)17 QT segment measurement and rate-adjusted calculation is required to rule out long-QT syndrome, which may be pre-emptive to polymorphic VT. (See Figure 4.)44,47,52 Corrected QT is determined by the calculation QTc = QT/RR1/2. The upper limit of normal is controversial, but an interval greater than 0.5 seconds is reliably abnormal. A non-diagnostic ECG does not preclude cardiac consultation, referral, or monitoring when indicated by patient history, comorbidities, or characteristics of the complaint.
 |
 |
Management and Disposition
Unstable patients in the ED should be managed without delay according to ACLS guidelines,53 with careful attention paid to maintaining a patent airway and systemic perfusion, with external chest compressions when necessary. Instability or serious symptoms related to dysrhythmia demand electrical pacing for bradycardia and electrical rhythm conversion for tachycardia or VF. Cardioversion of SVT or VT should be synchronized electrically, and such patients should be pre-medicated with sedatives and analgesia when the situation allows. Synchronization decreases the chance of shock coincident with cardiac repolarization, which may precipitate VF.53 Higher frequency tachycardia might make synchronization impossible, and if so, non-synchronous conversion is indicated. Pulseless VT and VF require immediate non-synchronous cardioversion.
Stable patients with proven dysrhythmias are also treated according to ACLS guidelines, with close attention to avoid iatrogenic worsening of accessory pathway conduction or ventricular mechanical failure. Any precipitating factors such as electrolyte imbalance or hypoglycemia should be sought out and managed.
Disposition of ED patients is, like the work-up, largely dependent on the cause of the patient's palpitations. In the event of any dysrhythmia, including complex PVCs, timely evaluation by a cardiologist is indicated. Chronic ectopic-focus suppression with medications generally should not be undertaken independently by the EP. If complex PVCs are present, initiation of suppression is worthwhile only in consultation. For patients suspected to have acute coronary syndrome, however, rate control measures are imperative in the initial stabilization and management. Previously healthy patients with no family or personal history of heart disease or unexplained syncope, with normal ECGs, and with no evidence of non-cardiac pathology (including drug use or side effects) may be considered low risk. These patients should be screened for depression and suicidal ideation. An assessment of major life events should be made. Patients undergoing life changes who may have a predisposition to amplify meaningless bodily sensations are at risk for chronic symptoms and frequent medical resource utilization.15 Appropriate primary care and psychiatric follow-up with judicious use of ambulatory cardiac monitoring are indicated. (See Table 5.)
 |
Patients who are asymptomatic in the ED without ECG abnormality other than intermittent isolated ectopy, yet have risk factors for dysrhythmia, require further evaluation. This can be done on an outpatient basis in cooperation with the patient's primary physician. Ambulatory event monitors have been shown to be the most cost-effective means of outpatient dysrhythmia analysis.54 The value of instructing the patient to increase dietary potassium (orange juice or bananas) and/or magnesium (green leafy vegetables) is unknown. In the event of persistent, disabling symptoms despite reassuring ambulatory monitoring, cardiology referral for elective outpatient electrophysiologic evaluation may be indicated.11
Cardiology consultation in the ED and/or hospital admission with continuous cardiac monitoring is indicated for patients with proven or ongoing dysrhythmia, any cardiovascular instability, significant risk for coronary artery disease, or cardiomyopathy.55 Palpitations found to be secondary to extra-cardiac medical disease, including ingestion, panic, or anxiety disorders, are managed according to the diagnosis. As a significant proportion (more than 16%) of patients ultimately do not receive a diagnosis, the EP should be prepared to manage and reassure these individuals with appropriate attention to follow-up arrangements.2
Case Conclusions
The causes of palpitations and the types of patients who present are variable. In some cases, such as when a patient has a known diagnosis of cardiac abnormality with predisposition to dysrhythmia, the primary responsibility of the emergency physician is to achieve and ensure hemodynamic stability. Alternatively, the patient might unknowingly carry a potentially fatal disorder that is just at the time becoming manifest, such as congenital repolarization abnormality (prolonged QT). Most cases will offer less obvious diagnoses. An attentive, directed evaluation would reveal immediately life-threatening conditions, and an understanding of the patient and his or her circumstances helps refine the investigation. For many presentations, a narrow differential diagnosis may be all that can be achieved after serious conditions have been ruled out. In the third case, for example, caffeine ingestion is a potential source for the symptom, but one cannot rule out PVCs or ST of any etiology. Patient education and reliable, comprehensive referral and follow-up are important in all cases.
References
1. Kroenke K, Arrington ME, Mangelsdorff AD. The prevalence of symptoms in medical outpatients and the adequacy of therapy. Arch Intern Med 1990; 150:1685-1689.
2. Weber BE, Kapoor WN. Evaluation and outcomes of patients with palpitations. Am J Med 1996;100:138-148.
3. Knudson MP. The natural history of palpitations in a family practice. J Fam Pract 1987;24:357-360.
4. Massin MM, Bourguignont A, Coremans C, et al. Chest pain in pediatric patients presenting to an emergency room or to a cardiac clinic. Clin Pediatr 2004;43:231-238.
5. Massin MM, Benatar A, Rondia G. Epidemiology and outcome of tachyarrhythmias in tertiary pediatric cardiac centers. Cardiology 2008;111: 191-196.
6. National Center for Health Statistics. Health, United States. 2007. With Chartbook on Trends in the Health of Americans. Hyattsville, MD:2007. http://www.cdc.gov/nchs/hus.htm. Accessed 5/1/2008.
7. Zipes DP, Camm AJ, Borggrefe M, et al; American College of Cardiology/American Heart Association Task Force; European Society of Cardiology Committee for Practice Guidelines; European Heart Rhythm Association; Heart Rhythm Society. ACC/AHA/ESC 2006 Guidelines for Management of Patients With Ventricular Arrhythmias and the Prevention of Sudden Cardiac Death: A report of the American College of Cardiology/American Heart Association Task Force and the European Society of Cardiology Committee for Practice Guidelines (writing committee to develop Guidelines for Management of Patients With Ventricular Arrhythmias and the Prevention of Sudden Cardiac Death): Developed in collaboration with the European Heart Rhythm Association and the Heart Rhythm Society. Circulation 2006;114:e385-484.
8. Rund DA, Bialecki PI, Saveanu RV, et al. Anxiety disorders and panic attack. In: Wolfson AB, et al., eds. Harwood Nuss' Clinical Practice of Emergency Medicine, 4th ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2005:639-643.
9. American Psychiatric Association, 1994. Diagnostic and Statistical Manual of Mental Disorders, 4th ed. Washington, DC: APA.
10. Ehlers A, Mayou RA, Sprigings DC, et al. Psychological and perceptual factors associated with arrhythmias and benign palpitations. Psychsomatic Med 2000;62:693-702.
11. Brugada P, Gursoy S, Brugada J, et al. Investigation of palpitations. Lancet 1993;341:1254-1258.
12. Goldreyer BN, Kastor JA, Kershbaum KL. The hemodynamic effects of induced supraventricular tachycardia in man. Circulation 1976;54:783-789.
13. Gursoy S, Steurer G, Brugada J, et al. The hemodynamic mechanism of neck palpitations. N Engl J Med 1992;327:772-774.
14. Barsky AJ. Palpitations, arrhythmias, and awareness of cardiac activity. Ann Int Med 2001;134(2)supp:832-837.
15. Barsky AJ, Ahern DK, Bailey ED, et al. Predictors of persistent palpitations and continued medical utilization. J Fam Prac 1996;42:465-472.
16. Lessmeier TJ, Gamperling D, Johnson-Liddon V, et al. Unrecognized paroxysmal supraventricular tachycardia: Potential for misdiagnosis as panic disorder. Arch Int Med 1997;157:537-543.
17. Zimetbaum P, Josephson ME. Evaluation of patients with palpitations. N Engl J Med 1998;338:1369-1373.
18. Vickers Saarel EV, Stefanelli CB, Fischbach PS, et al. Transtelephonic electrocardiographic monitors for evaluation of children and adolescents with suspected arrhythmias. Pediatrics 2004;113:248-251.
19. Chen JY, Tsai WC, Lee YL, et al. Association of premature ventricular complexes with central aortic pressure indices and pulse wave velocity. Am Heart J 2008;155:500.e1-6.
20. Fernandes F, Soufen HN, Ianni BM, et al. Primary neoplasms of the heart. Clinical and histological presentation of 50 cases. Arq Bras Cardiol 2001; 76:231-237.
21. Seferovi PM, Risti AD, Maksimovi R, et al. Cardiac arrhythmias and conduction disturbances in autoimmune rheumatic diseases. Rheumatology (Oxford) 2006;45 Suppl 4:iv39-42.
22. Duren DR, Becker AE, Dunning AJ. Long term follow-up of idiopathic mitral valve prolapse in 300 patients: A prospective study. J Am Coll Cardiol 1988;11:42-47.
23. Ng GA. Treating patients with ventricular ectopic beats. Heart 2006;92: 1707-1712.
24. Cannom DS, Prystowsky EN. Management of ventricular arrhythmias. Detection, drugs, and devices. JAMA 1999;281:172-179.
25. Huikuri HV, Castellanos A, Myerburg RJ. Sudden death due to cardiac arrhythmias. N Engl J Med 2001;345:1473-1482.
26. Lown B, Wolf M. Approaches to sudden death from coronary heart disease. Circulation 1971;44:130-142.
27. Yealy DM, Delbridge TR. Dysrhythmias. In: Marx J, et al., eds. Rosen's Emergency Medicine: Concepts and Clinical Practice, 6th ed. Philadelphia, PA: Mosby Elsevier; 2006; 1199-1246.
28. Kennedy HL, Whitlock JA, Sprague MK, et al. Long-term follow-up of asymptomatic healthy subjects with frequent and complex ventricular ectopy. N Engl J Med 1985;312:193-197.
29. Myers MG. Caffeine and cardiac arrhythmias. Ann Intern Med 1991;114: 147-150.
30. Liechti ME, Kunz I, Kupferschmidt H. Acute medical problems due to Ecstasy use. Case-series of emergency department visits. Swiss Med Wkly 2005;135:652-657.
31. Kwon KT, Tsai VW. Metabolic emergencies. Emerg Med Clin North Am 2007;25:1041-1060.
32. Werbel SS, Ober KP. Pheochromocytoma. Update on diagnosis, localization, and management. Med Clin North Am 1995;79:131-153.
33. Rohr SM, Rich MW, Silver KH. Shortness of breath, syncope, and cardiac arrest caused by systemic mastocytosis. Ann Emerg Med 2005;45:592-594.
34. McInerney J, Sahgal P, Vogel M, et al. Scombroid poisoning. Ann Emerg Med 1996;28:235-238.
35. Bani D, Nistri S, Mannaioni PF, et al. Cardiac anaphylaxis: Pathophysiology and therapeutic perspectives. Curr Allergy Asthma Rep 2006;6:14-19.
36. Pandian JD, Dalton K, Henderson D, et al. Postural tachycardia syndrome: An underrecognized disorder. Int Med J 2007;37:529-535.
37. Morillo CA, Klein GJ, Thakur RK, et al. Mechanism of 'inappropriate' sinus tachycardia. Role of sympathovagal balance. Circulation 1994;90:873-877.
38. Maron BJ. Sudden death in young athletes. N Engl J Med 2003;349: 1064-1075.
39. Sen-Chowdhry S, Lowe MD, Sporton SC, et al. Arrhythmogenic right ventricular cardiomyopathy: Clinical presentation, diagnosis, and management. Am J Med 2004;117:685-695.
40. Batra AS, Hohn AR. Consultation with the specialist: Palpitations, syncope, and sudden cardiac death in children: Who's at risk? Pediatr Rev 2003;24: 269-275.
41. Tan JH, Scheinman MM. Exercise-induced polymorphic ventricular tachycardia in adults without structural heart disease. Am J Cardiol 2008;101: 1142-1146.
42. Frolkis JP, Pothier CE, Blackstone EH, et al. Frequent ventricular ectopy after exercise as a predictor of death. N Engl J Med 2003;348:781-790.
43. Coumel P. Clinical approach to paroxysmal atrial fibrillation. Clin Cardiol 1990;13:209-212.
44. Ietsugu T, Sukigara M, Furukawa TA. Evaluation of diagnostic criteria for panic attack using item response theory: Findings from the National Comorbidity Survey in USA. J Affect Disord 2007;104:197-201.
45. Giese EA, O'Connor FG, Brennan FH, et al. The athletic preparticipation evaluation: Cardiovascular assessment. Am Fam Physician 2007;75: 1008-1014.
46. Huff JS, Decker WW, Quinn JV, et al; American College of Emergency Physicians. Clinical policy: Critical issues in the evaluation and management of adult patients presenting to the emergency department with syncope. Ann Emerg Med 2007;49:431-444.
47. Goldberger AL. Clinical Electrocardiography: A Simplified Approach, 7th ed. Philadelphia, PA: Mosby Elsevier; 2006.
48. Libby P, et al, eds. Braunwald's Heart Disease. A Textbook of Cardiovascular Medicine, 8th ed. Philadelphia: Saunders Elsevier; 2007.
49. Ufberg JW, Clark JS. Bradydysrhythmias and atrioventricular conduction blocks. Emerg Med Clin North Am 2006;24:1-9.
50. Stahmer SA, Cowen R. Tachydysrhythmias. Emerg Med Clin North Am 2006;24:11-40.
51. Chew HC, Lim SH. Broad complex atrial fibrillation. Am J Emerg Med 2007;25:459-463.
52. Saliba WI, Natale A. Ventricular tachycardia syndromes. Med Clin North Am 2001;85: 267-304.
53. Field JM, Hazinski MF, Gilmore D, eds. Handbook of Emergency Cardiovascular Care: for Healthcare Providers, 3rd ed. Dallas, TX: American Heart Association.
54. Rao A, Lomax S, Ramsdale K, et al. Ambulatory cardiac rhythm monitoring. Br J Hosp Med (Lond) 2007;68:132-138.
55. Chen EH, Hollander JE. When do patients need admission to a telemetry bed? J Emerg Med 2007;33:53-60.
Well, after my erudite presentation, the attending, who happened to be a cardiologist trained in the pre-interventional era, sat back and said, "Son, remember the heart is not a chronometer."Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
