'Mandatory or not,' errors are going unreported
'Mandatory or not,' errors are going unreported
Ambiguity big reason for underreporting
A story that ran in the Sept. 12 issue of the Philadelphia Inquirer — "Hospitals' mistakes are going unreported" — might have shocked readers with its description of unreported errors in New Jersey and Pennsylvania despite the states' mandatory reporting requirements. But it came as no surprise to those in the health care or regulatory industry.
"For me it's not a surprise," says Debora Simmons, RN, MSN, CCRN, CCNS, formerly senior clinical quality improvement analyst for the Institute of Healthcare Excellence at M.D. Anderson Cancer Center in Houston.
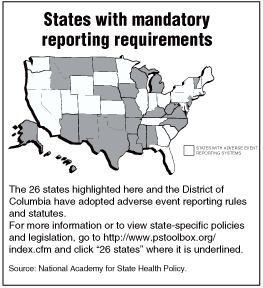
William Hyman, PhD, professor of biomedical engineering at Texas A&M University, agrees. "Mandatory or not," errors are going unreported, he says, despite the fact that 26 states now have state reporting requirements.
Deterrents to reporting
The reasons for under- or unreporting are plenty and, according to the experts Hospital Peer Review spoke with, the most common is simply not understanding what should be reported. A "really important piece" of encouraging disclosure is "making sure everyone is clear on what needs reporting," says Diane Rydrych, MA, assistant director of the division of health policy at the Minnesota Department of Health.
Though the law might seem black and white, she says, "there are lot of gray areas, and we have to do a lot of work on definition and making it clear to people what's reportable and what's not. There's a lot of confusion."
Minnesota requires health care facilities to report on any of the 28 National Quality Forum (NQF) serious adverse events. Seems clear enough, but Rydrych points out there are multiple nuances within this. For instance, with an object left in a patient after surgery. At what point the surgery ends is one of the definitional areas she says needs clarification. Or what about instances in which the object is intentionally left in because to get it out would put the patient at greater risk than leaving it be?
She prefers a nonpunitive approach to encourage reporting and says that in Minnesota, reporting requirements resulted from a "collaborative" effort with hospitals at the table, specifically the Minnesota Alliance for Patient Safety, which was founded by the Department of Health, hospital associations, and medical associations.
"They worked together with other stakeholders to get the law passed in Minnesota so it didn't have that adversarial or punitive tone from the beginning," she says. " I think that that has really helped in Minnesota with compliance."
Others do see merit in stronger enforcement. "I think there's an inherent flaw in asking hospitals to report with no meaningful enforcement... They're clearly not doing it," Hyman says.
"People don't like the big stick approach, but I think the only way you're going to get it is serious enforcement," he adds. He questions if states are doing enough with the information. "What's the level of analysis? What's the response from the state? What are they making publicly available? And is it of use to anybody?"
Simmons says it all comes down to human nature. "It's not our human nature to want to say you made a mistake in any circumstance, even if it's nonpunitive, even if I feel like I'm not going to get any repercussions from it. We don't like saying we made mistakes, especially if you're a highly esteemed professional," she says.
Rydrych doesn't believe the majority are knowingly not reporting and says it comes back to a lack of understanding. "Someone can make what they feel is a legitimate decision that it's not a reportable event and that's where we have to make sure we're educating them on what their responsibilities are. It's hard for me to imagine people are deliberately not reporting things they know are reportable," she says. "Maybe it's naive, but I really don't believe that's going on in any widespread fashion."
Trying to make it work
Robert Wachter, MD, professor and associate chairman of the department of medicine at the University of California, San Francisco, thinks linking reporting to the NQF serious adverse event list is the way to go to promote compliance, citing California, Minnesota, and Indiana practices.
"I've never been a fan of Pennsylvania's reporting initiative that basically said report everything and has generated, at last count, 600,000 or 700,000 reports. I think that's silly. That's way too much data," he says.
The NQF list provides "a nice start of a manageable number of pretty serious things," he says. When California began requiring that facilities report on those events, "it really transformed our internal processes," he says.
"I'm convinced that maneuver markedly improved safety, but it didn't do it because the state is doing anything so spectacular with regard to reports," he says. "It did it because we now know when one of those things happened, we had to create an internal process to learn about it, analyze it quickly, come out with an action plan, see that to fruition, and share the results of what we learned." It's a much more systematic approach, he adds.
Double checking
In Minnesota, Rydrych says getting reporting facilities on board to help sort out definitional issues has helped compliance. The state also requires all professional boards, such as boards of medical practices and boards of nursing, to report any event they've heard of as a sort of "cross check."
The Department of Health reviews death records monthly to see if any events show up. "That's only a partial cross check," she says, "because not all of the events are associated with death." One problematic area, she sees, is linking one hospital-associated event with problems at other facilities or nursing homes. For instance, if a patient falls in one facility but later dies in another, no good mechanism exists to check that, so death records in those cases have helped. But she thinks the recent law change to include not only death but serious disabilities that stem from falls will help.
Her advice for quality and safety managers is to view reporting as "an opportunity to learn and an opportunity to learn how you can improve your system."
"If you have a reporting system in place, figuring out what really specifically you do have to report and what you don't have to report, getting those grey areas sorted out, is really important."
When you're not sure if you should report something, she suggests calling your department of health or hospital association. When health care facilities call her with a questionable case, she'll discuss it with them and if needed she'll refer to the hospital association and discuss it further with them. In more challenging cases, the event goes before a larger group, comprised of mostly the larger urban hospitals, for further review.
"I think an outsider would be really surprised" by the amount of work that goes into these discussions, she says. "It's ultimately the department of health that decides," she adds, but says she gets a lot of feedback from outside experts.
She acknowledges the difficulties in 100% compliance with any mandatory reporting efforts. "It's not perfect," she says. "I talk a lot with other states that have similar laws, and the underreporting question is something that everyone struggles with."
AHRQ efforts to centralize reporting
The Agency for Healthcare Research and Quality (AHRQ) is responsible for administering the provisions of the Patient Safety and Quality Improvement Act of 2005, which authorized the creation of patient safety organizations (PSOs) to collect voluntary reporting data from health care facilities to counteract the two big impediments to reporting: confidentiality and isolated data with no ability to aggregate and compare. The Department of Health and Human Services issued interim guidance in early October to implement the act and to allow organizations to apply to act as a PSO. Final guidance is expected at the end of the year.
"It's exactly where we needed to go," Simmons says of the PSO initiative. "The fact that it's taken us 10 years to get there is really sad."
Hyman sees one issue with the PSO roll out: duplication. If you're in state that requires reporting and if you also decided to report to a PSO, you're reporting to many agencies — the state, the PSO, the FDA, your risk management committee, The Joint Commission, CMS, etc. — and often you're reporting similar things to more than one place, he says. If only there was one online checklist, he adds wistfully and only half joking.
(Editor's note: For more information about AHRQ's PSO roll out, go to www.pso.ahrq.gov/.)
A story that ran in the Sept. 12 issue of the Philadelphia Inquirer "Hospitals' mistakes are going unreported" might have shocked readers with its description of unreported errors in New Jersey and Pennsylvania despite the states' mandatory reporting requirements.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
