Poor health care quality is a national problem
Poor health care quality is a national problem
Study shows only 50%-60% get recommended care
A recent analysis of data collected by the RAND Corp, a Santa Monica, CA-based health policy think tank, indicates that people in all parts of the nation are at risk for receiving poor health care.
A previous report from RAND’s Community Quality Index (CQI) study focused on the quality of care delivered nationally, but provided no information about whether the problems observed were consistent across communities or based on exceptionally poor performance in a few communities, researchers reported in the May 4 edition of the journal Health Affairs.1
The new analysis from the study by RAND Health, the corporation’s research division, is the first comprehensive community-based assessment of health care quality in the United States.
"What we now know is that it really doesn’t matter where you live — only about 50% of the time are you getting the recommended care," says lead study author Eve A. Kerr, MD, MPH of the Veterans Affairs Ann Arbor Health Care System and the University of Michigan. "The lack of community level variation in overall quality should serve as a wake-up call to all communities to examine their own quality of care and determine how they can do a better job."
The study examined how effectively health care is delivered in 12 metropolitan areas: Boston; Cleveland; Greenville, SC; Indianapolis; Lansing, MI; Little Rock, AR; Miami; Newark, NJ; Orange County, CA; Phoenix; Seattle; and Syracuse, NY.
To define and measure quality, the research team selected 30 clinical areas that represent the leading causes of death and disability, as well as the major reasons people seek health care. Then they developed a set of quality indicators within each clinical area based on a review of national guidelines and the medical literature.
Although the economic and health resource profiles of these communities are very different, there were few consistent differences in the quality of care received by people in the communities, the final analysis indicates.
The study found that on average:
- People in the 12 communities studied received only 50%-60% of recommended health care.
- There were very few significant variations in the quality of preventive, acute, and chronic care across communities nationwide.
- No single community consistently had the highest or lowest performance for all selected chronic conditions.
- Quality of health care varied substantially across conditions. In almost all communities, the poorest care was for diabetes.
The 12 communities in the CQI are representative of metropolitan areas with populations of 200,000 or more. The study was based on interviews with nearly 7,000 adults in these communities and a review of all of their medical records. It assessed 439 clinical indicators of quality for 30 acute and chronic conditions such as urinary tract infections, diabetes, asthma, high blood pressure, and heart disease — along with preventive care. (See table, below.)
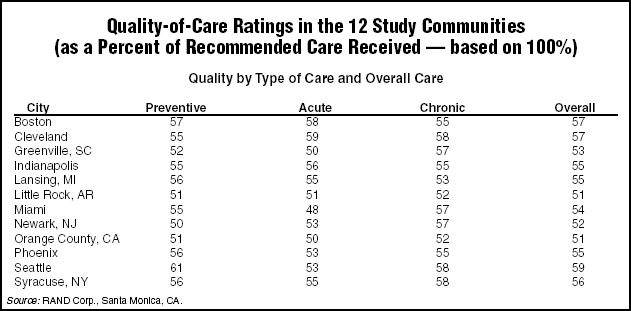
The new analysis demonstrates that poor quality exists throughout the United States health care system and is not relegated to certain pockets of the country, researchers said.
Elizabeth A. McGlynn, PhD, associate director of RAND Health and a co-author of the study, noted that, while low levels of quality were previously reported for the nation, many people might have concluded that quality was better in their own community than in the nation as a whole.
"Even if you are minutes away from the best hospital in your community, you are still at risk for poor care," she said. "We hope this study stimulates a dialogue among patients, doctors, employers, hospitals, and insurers in these 12 communities, and in other communities we did not study, about the best local solutions to these serious deficits."
Researchers noted that some people might be surprised that performance was not better in areas with outstanding medical institutions. The analysis examined average care for adults from an entire metropolitan area, rather than care received from a specific facility, health care system, or doctor.
Although no one community fared significantly better than the others on the quality of preventive, acute, and chronic care, there were some differences. The findings revealed:
- All the communities demonstrated important deficits in the provision of basic care. People living in Little Rock received 51% of indicated care, compared with 59% among those living in Seattle.
- Residents in all communities were more likely to receive services to prevent chronic disease through screening (for example, measuring blood pressure) and immunizations than they were to receive other dimensions of preventive care, such as services to prevent sexually transmitted diseases and HIV, or substance abuse counseling.
- Quality of care for hypertension was among the best for the chronic conditions — residents in Cleveland received about 70% of indicated care.
- Quality of care for cardiac conditions (coronary artery disease, congestive heart failure and atrial fibrillation) was generally lower than care for hypertension, ranging from 52% in Indianapolis and Newark to 70% in Cleveland and Syracuse.
- Care for depression ranged from 47% in Newark to 63% in Seattle.
What can be done?
Although each community must grapple with how to improve the quality of care locally, the researchers note, the analysis clearly indicates that considerable room exists for improvement in health care delivery at the community level.
The researchers suggest that not all of the solutions should come from within the medical system alone. For example:
- Large employers could provide leadership to improve chronic disease care in outpatient settings as they have done to reduce medical errors in hospitals.
- Health care systems, with or without financial incentives, could initiate quality improvement initiatives in collaboration with the community to improve the provision of preventive care.
- Community-based education and outreach efforts could activate patients to demand improved quality across many dimensions and to identify their own care requirements.
"There are many laudable community coalitions and initiatives throughout the country," the authors state in the Health Affairs report. "But, few have meaningful baseline or post-intervention data on the processes and outcomes of health care to be able to answer whether or not their initiatives improve quality of care."
More information on the CQI study, the new analysis, and the methods used to evaluate care delivery are available on the RAND Corp. web site at www.rand.org/
Collaborating on the study were Steven M. Asch, MD, MPH, (RAND, Veterans Affairs Greater Los Angeles Health Care System, University of California Los Angeles); John Adams, PhD, (RAND); and Joan Keesey, BA, (RAND).
The Robert Wood Johnson Foundation funded the study. The Veterans Affairs Health Services Research and Development program supported Drs. Asch and Kerr.
Reference
1. Kerr E, McGlynn E, Adams J, et al. Profiling the quality of care in twelve communities: Results from the CQI study. Health Affairs 2004; 23:247-256.
Source
- Eve Kerr, MD, MPH, and Elizabeth McGlynn, PhD, RAND Health, 1700 Main St., P.O. Box 2138, Santa Monica, CA 90407-2138.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
