Disease Presentations of the Uvula
July 1, 2014
Reprints
Executive Summary
- Most infections of the uvula are viral.
- Bacterial infections are the most common cause of isolated uvulitis.
- Group A Streptococcus is the most common organism causing bacterial uvulitis.
- In cases of isolated uvular edema, think of the possibility of hereditary angioedema.
- Because thermal or chemical burns of the uvula are often associated with illegal activity, patients may not be forthcoming with this history.
I work in a county hospital ED, and as you already know by that statement, we see an interesting and sometimes unusual patient population. We are also close to the Phoenix airport and main bus station, so we commonly have travelers from all over coming by with their problems and issues, some mundane and other fantastical. We have patients complete a registration form with the name, birthdate, and statement, in their own words, why they are coming today to the ED. We get all sorts of responses, some just a few words, others a long tale of woe. It is sometimes a challenge to figure out why, and why now, even after talking with the patient.
For non-critical patients, those who do not need urgent assessment and treatment, my role as an attending is to discuss the patient with the residents after they have performed the history and physical examination. Now it is my turn to try and make sense of these sometimes confusing complaints. It’s my time to cut through the clutter and impart definition to the patient’s problem. And sometimes I’m stumped. If there is a complaint localized to a usual body part or an issue claimed by the patient that I have never heard of (a potential range that shirks the older I get — I may not know the specific details of the latest insights, but at least I have heard of it before), I have a stalling response to give me time to marshall my thoughts; I respond to the resident that I must have been absent that day in medical school where this was discussed.
After that admittedly lame attempt at humor, the resident and I can then work through the patient’s problem together.
So it once was when patients came in complaining of pain or swelling of that thing that hangs in the back of the throat. I have seen a few cases of uvulitis over the years and read the individual case reports. The authors of this issue have written an excellent review of this unusual problem. After reading this issue, you can say with confidence, I know about this problem.
— J. Stephan Stapczynski, MD, FACEP
Introduction
The uvula, or as our patients describe it, "the little thing that hangs down the back of the throat," is one of the most commonly ignored parts of the body. However, like all organs of the body, even the diminutive uvula can have its own unique problems and disease presentations. The purpose of this article is to review different disease presentations and conditions of the uvula. (See Table 1.)
Table 1: Potential Diseases and Conditions of the Uvula
1. Angioedema
a. Isolated angioedema or Quincke’s disease
b. Hereditary angioedema (HAE)
c. Allergic
d. Ace inhibitor and other drug associated angioedema
e. Myxedematous changes of hypothyroidism
2. Burns
a. Thermal
i. Smoke inhalation injuries
ii. Cocaine or marijuana smoking
iii. Sauna exposure
b. Chemical
3. Infections
a. Viral
b. Bacterial
c. Mycobacterium
d. Trauma
4. Postsurgical Uvula
a. Surgical complications
i. Orotracheal intubation associated
ii. Suctioning or bronchoscopy
b. Cultural uvulectomy
5. Hematologic and Oncologic
a. Hemangiomas
b. Oncologic
6. Congenital Variants
a. Bifurcate uvula
b. Elongated uvula
7. Vascular
a. Superior vena cava syndrome
b. Internal carotid artery ligation
c. Lymphatic duct ligation
d. Kawasaki syndrome
Angioedema: Quincke’s Disease or Isolated Angioedema
An isolated form of angioedema called Quincke’s disease can involve the uvula. Quincke’s disease is induced by several factors, including foods, drugs, and inhalants. It is most commonly attributed to a type 1 hypersensitivity reaction, but may also be due to medication reactions, inhalation reactions, trauma (usually from intubation or endoscopy), hereditary angioedema, or infections.5-9 It should be differentiated from uvulitis, which is primarily considered to be an infectious process. Symptoms vary by individual, with the most common complaint being a sore throat. Other complaints include a feeling of neck fullness, difficulty breathing, and inability to swallow. Patients may also have the typical "hot potato voice" due to the swelling of the pharynx.
Figure 1: Isolated Edema of the Uvula
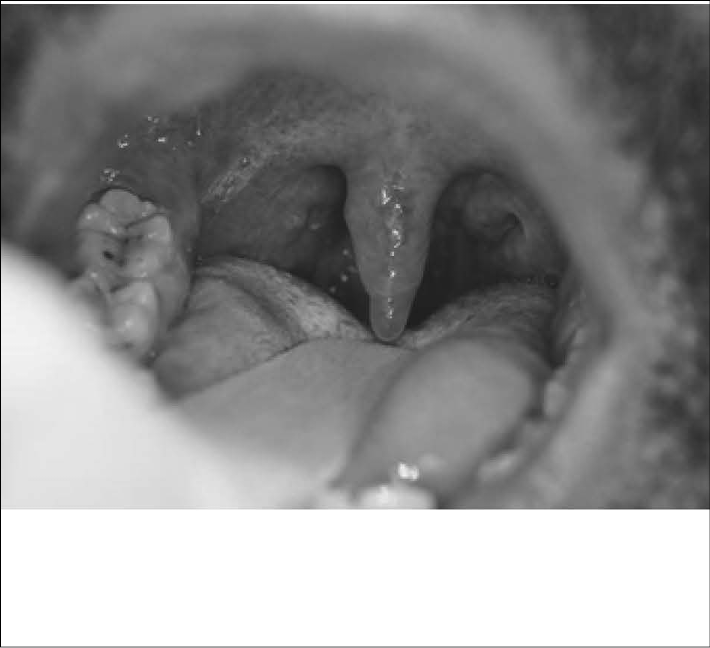
Isolated edema of the uvula in a 30-year-old male who presented to the emergency department complaining of a swollen uvula and a sore throat. The patient denied a fever or recent illness and indicated that his uvula felt "irritated from scratching."
Hereditary Angioedema (HAE)
In the absence of medications, allergic reactions, trauma, or infection, one may consider hereditary angioedema (HAE) as a cause for uvular edema. The uvula in this case is rarely erythematous, but rather it bears a similar appearance to that of a white grape.9 Bradykinin is a vasodilator thought to be responsible for the characteristic HAE symptoms of localized swelling, inflammation, and pain. The C1-esterase-inhibitor is a key regulator of the factor XII/kallikrein proteolytic cascade that leads to bradykinin production. When the C1 esterase inhibitor is absent or dysfunctional, a bradykinin cascade is triggered, leading to vasodilation and edema of the tissue. Most concerning is concurrent involvement of the larynx and airway compromise. Screening for the enzyme deficiency can be done by ordering a C3 and C4 level. A normal C3 and low C4 would suggest the condition.10 Unfortunately, hereditary and ACE-inhibitor-induced angioedema do not respond to corticosteroids, antihistamines, or epinephrine. Instead, interventions to decrease bradykinin activity are indicated.10,11 Some physicians have successfully used fresh frozen plasma (FFP) to reverse the effects (see Table 2). FFP contains kininase II, which breaks down bradykinin, rendering it ineffective. It also contains a C1 esterase inhibitor, making it effective for hereditary angioedema.10,12 Most symptoms appear to resolve within a matter of hours; however, there are only case reports currently available. No studies to date have been performed to assess a large group’s response to FFP.
Table 2: Pharmaceuticals Used to Treat Uvular Diseases
| Hereditary Angioedema | ||
FFP |
2 units IV (adult) |
Anecdotal cases reports, response takes hours, not currently recommended as first-line therapy |
C1 inhibitor human (Berinert®) |
20 units/kg infused slowly |
Used for acute attacks, response within 30-120 min |
Icatibant (Firazyr®) |
30 mg SC in the abdomen |
Bradykinin receptor antagonist, response within 30-120 min |
Ecallatide (Kalabitor®) |
30 mg (3 mL), SC in three 10 mg (1 mL) injections in thigh, abdomen and upper arm |
Kallikrein inhibitor, response within 30-120 min Anaphylaxis observed in 4% |
| Thermal Burns and Adjunct to Infectious Uvulitis | ||
| Dexamethasone | 0.1 mg/kg IV (max dose 12 mg) q6-12 hours |
Continue until swelling stabilizes |
| Bacterial Uvulitis | ||
| Ceftriaxone | 1 g IV (adult) |
|
There are currently at least two medications available that act on the bradykinin cascade, ecallantide and icatibant. Ecallantide is a kallikrein inhibitor, which reduces the conversion of kininogen to bradykinin, thereby reducing the amount of swelling and pain. Icatibant is a bradykinin receptor antagonist that was approved by the FDA in 2011 for use in severe asthma attacks as well as for treatment of hereditary angioedema. It is a competitive antagonist selective for the bradykinin B2 receptor and has an affinity similar to bradykinin. Icatibant inhibits bradykinin from binding the B2 receptor and, consequently, treats the clinical symptoms of an acute, episodic attack of HAE. The bradykinin cascade is stopped, thereby preventing systemic vasodilation and edema.10,12-14 In a study by Bas et al, 30 mg of icatibant was given subcutaneously to eight patients with angioedema. The average time to initial improvement of symptoms was 50.6 minutes, with complete resolution of symptoms within 4.4 hours.14 In addition, Schmidt et al presented a case of a patient who was given steroids, diphenhydramine (Benadryl), and epinephrine. The patient’s symptoms did not respond. As a last resort, they gave the patient 30 mg of icatibant. Symptoms resolved rapidly, which avoided placement of an advanced airway.15 Randomized, controlled trials have proven icatibant’s efficacy for hereditary angioedema. As the pathways are similar for ACE inhibitor angioedema, it is hoped that icatibant will be likewise effective.13
Allergic
Allergic reactions or type 1 hypersensitivity reactions can cause uvulitis. Due to an IgE-mediated response, the reaction causes a sudden release of mast cells and vasodilation, causing urticaria, angioedema, or anaphylaxis.5,6,8 A typical patient may present with systemic hives, edema, and difficulty breathing. Wheezes may or may not be present, although the patient may have inspiratory stridor. Treatment involves corticosteroids, antihistamines, H1 and H2 blockers, and epinephrine.7 The patient should be monitored for a minimum of 6 hours after these therapeutic interventions to evaluate for a latent reaction phase.
Other Causes
There are other non-infectious causes of uvular edema. Myxedematous infiltration in hypothyroidism is well documented in the literature. A variety of pharmaceuticals, both illegal and legal, can lead to uvulitis. Alcoceba et al performed a prospective study identifying characteristics of individuals developing uvular edema. Of these, several were related to drug reactions, namely nonsteroidal anti-inflammatory drugs (NSAIDS), angiotensin-converting-enzyme inhibitors (ACE inhibitors), cocaine and marijuana use, as well as glucosamine sulfate, ipratropium bromide, and the juice from Ecballium elaterium (home remedy for sinusitis).5,8 It is difficult to identify the difference between a medication reaction and an allergic reaction. Thus, initial management should include diphenhydramine, steroids, and, possibly, epinephrine. If ACE inhibitors are involved, the edema is usually due to the same bradykinin cascade as seen in hereditary angioedema and may not be responsive to the aforementioned treatment.
Burns: Thermal
Cannabis sativa contains a chemical, hashish, which burns much hotter than tobacco products. This is particularly irritating to the oropharynx, leading to swelling and erythema of the entire pharyngeal cavity, especially the uvula.16,17 Symptoms occur within hours after heavy smoke exposure and may last up to 24 hours.17,18 Boyce et al presented a clinical case of a patient who presented with difficulty breathing after smoking marijuana. The physical exam showed an edematous uvula. The patient was treated with antihistamines and corticosteroids and discharged home. The presumed etiology was either an inhalation burn or an allergic reaction to the cannabis.19
Figure 2: Edema and Inflammation of the Uvula
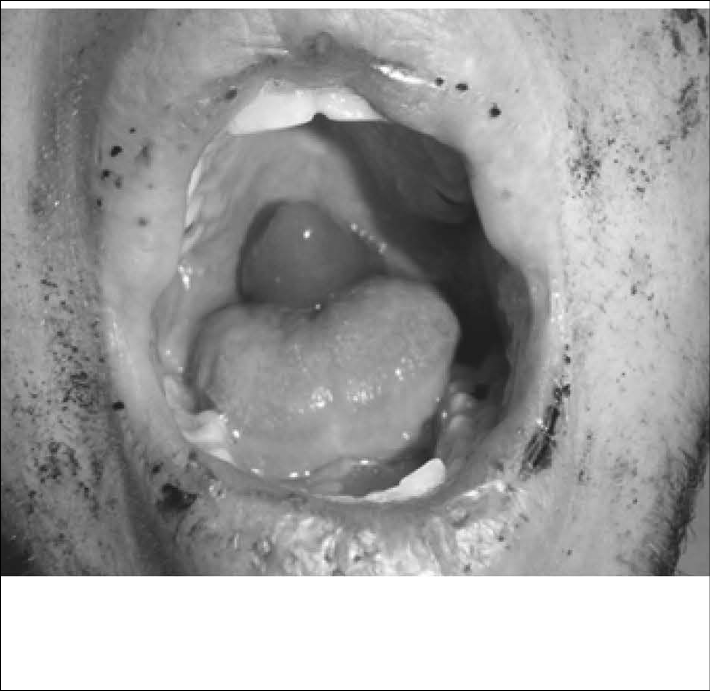
A 26-year-old male who presented for evaluation following an assault. He demonstrated marked edema and inflammation of the uvula, and he admitted to smoking marijuana with a crack pipe.
Cocaine or crack also burns at a higher temperature than typical tobacco products and can cause inflammation as well. In fact, breathing in any air that is extremely hot can cause uvulitis. There have even been reported cases following sauna exposures.9 Treatment involves administration of steroids, in particular dexamethasone, as its anti-inflammatory potency is 25 times greater than hydrocortisone and it has a half life of 36 to 72 hours.17 Dexamethasone can be given continuously with 0.1 mg/kg given every 6-12 hours, but not exceeding 12 mg in any dose.17
Burns: Chemical
Chemical burns to the uvula can occur following ingestion of toxic substances during accidental or purposeful ingestions. Multiple toxic acid or base (alkaline) agents can injure the oral mucosa to include the uvula. Acids typically cause a coagulation necrosis by denaturing proteins. The resulting eschar or coagulum can limit the penetration of the acid. However, bases tend to produce liquefaction necrosis and cause a more severe injury. Denaturing of proteins and saponification of fats occur without forming an eschar to limit tissue penetration.
Infections: Viral
Viral infections of the oropharynx tend to occur more commonly than bacterial ones do. However, there is not a plethora of research involved in identifying the individual viruses that can cause pharyngeal irritation. Human herpesvirus 6 (HHV6) is the virus that causes exanthem subitum (ES), a viral illness characterized by a high fever for approximately four days followed by a diffuse rash. In the early 1990s, uvulo-palatoglossal junction ulcers (UPJ) were identified as an early marker for the disease. The uvulo-palatoglossal junction is located where the palatoglossal folds approximate with the base of the uvula. K.B. Chua et al performed a study in Malaysia identifying UPJ ulcers as a pathognomonic finding in HHV6. They recruited a total of 46 children, 20 of whom had UPJ ulcers. Of the 19 patients who followed up, 17 of them had subsequently progressed to the full-blown symptoms of ES.20 Many other viral agents including Coxsackie A may be associated with a sore throat and often involve the uvula.
In contrast to ulcer formation, human papillomavirus 6 (HPV-6) and human papillomavirus 11 (HPV-11) can lead to papillomas of the oral cavity. Though typically occurring on the tongue or palate, they can also cause lesions on the uvula. The papillomas form fibrous lesions that can lead to uvular elongation and a sense of choking in the patient. These can be removed surgically and rarely lead to cancer of the oropharynx.21
Infections: Bacterial
Infections of the uvula often accompany tonsillitis and, in the past, were seen relatively commonly with epiglottitis. Uvula infections can also occur as isolated infections. Infections are perhaps the most concerning cause of uvular edema. Bacterial infections are the most common, namely due to group A streptococcus, although it can also be caused by Streptococcus pneumoniae, and, in some individuals, Haemophilis influenzae.8,22 In the case of H. influenzae, it is not the uvular edema that is the primary concern so much as it is the epiglottitis, which can concurrently develop, resulting in airway compromise. In adults this is rarely the case; however, in the pre-vaccine era it was not uncommon in children. Currently, it can still be seen in those who have not been vaccinated.8,9,22 Patients typically present with a sore throat and fever. However, symptoms may be even more severe, including presentation of an individual with a hot potato voice, respiratory distress, drooling, and dysphagia. Current recommendations for any patient with both fever and uvular edema are to obtain lateral soft tissue films of the neck.8,9,22 If signs of epiglottitis are evident, namely the typical "thumb print sign," further investigation with laryngoscopy and consultation with an ear, nose, and throat specialist (ENT) and surgery are advised.9 While waiting for the consultant, a complete blood count (CBC), blood cultures, and oropharyngeal cultures should be obtained, and the patient should be started on ceftriaxone and dexamethasone.9 As a precaution, if the patient is not tolerating oral secretions and appears in respiratory distress, then the patient should be kept calm and allowed to remain in any position that is most comfortable for him or her. In this case, obtaining an oropharyngeal culture should be deferred until the patient is taken to the operating room for intubation, although antibiotics should be started as soon as possible.
Figure 3: Tonsillitis with Uvula Swelling and Inflammation
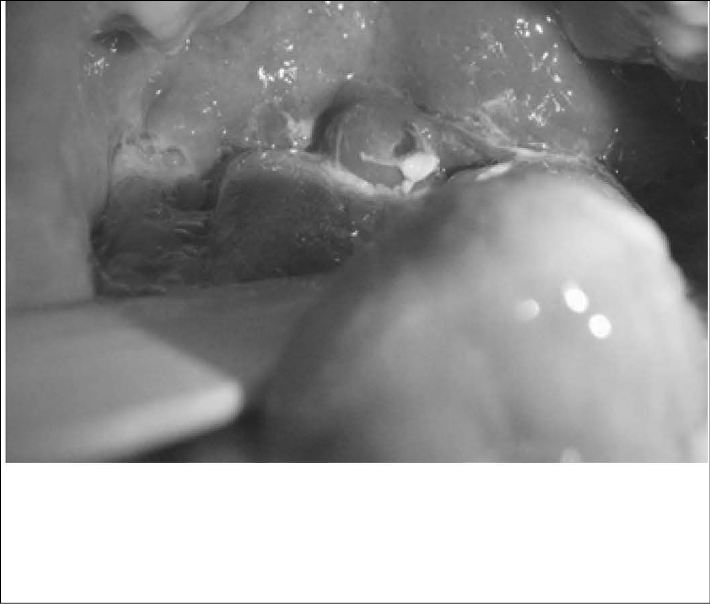
Tonsillitis along with uvula swelling and inflammation of unknown etiology in an 18-year-old male who presented for evaluation of severe throat pain. The rapid streptococcal test was negative.
Diphtheria is a historical disease in the developed world that also involves the uvula. However, in underdeveloped countries the disease can still be found and is associated with the bacterium Corynebacterium diphtheriae (a pleomorphic Gram-positive rod). Diphtheria predominantly involves the nasopharyngeal mucosa and presents as a dirty gray membrane covering the tonsils, tonsillar pillars, soft palate, and uvula. Bleeding with attempts at removal of the membrane and a "bull-neck" appearance secondary to cervical adenopathy are commonly described. The case mortality rate for diphtheria is up to 12%.
Mycobacterium
An additional consideration in immunocompromised patients is the presence of Mycobacterium tuberculosis. Although oral cavity M. tuberculosis typically occurs in the tongue and mandible, some cases have been reported with primary sites involving the uvula. Signs of infection can range from a single ulcer to a yellow discharge to a nodular mass. The workup should include a chest X-ray, purified protein derivative (PPD) test, and a culture and stain for acid fast bacilli. After confirming the diagnosis, treatment should be started with a six-month course of rifampin, ethambutol, isoniazid, pyrazinamide, and streptomycin.23-25
Fungal
Candida, in addition to causing thrush in infants, can also be isolated to the uvula. The presentation may be an erythematous uvula in the absence of other findings or white plaques isolated to the uvula. The investigation should include neck films to evaluate for epiglottitis and possibly uvular cultures. Treatment is nystatin, which leads to a resolution of symptoms within a few days.26
Figure 4: Lesions on Palate and Uvula Consistent with Herpangina
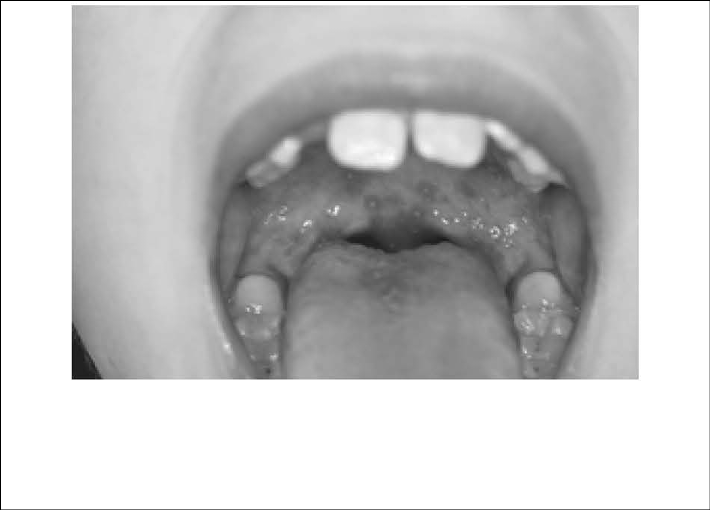
Eight-year-old female presenting with the chief complaint of fever, cough, rhinorrhea, and a sore throat. The lesions demonstrated on the palate and uvula were consistent with herpangina, which is typically caused by the Coxsackie A virus.
Trauma: Post-surgical Uvula
Tonsillectomy is one of the oldest and most commonly performed surgeries in the pediatric population. Originally performed in an attempt to prevent recurrent pharyngitis, it is now used in cases for obstructive sleep apnea.27 Occasionally these pediatric patients will present to the ED after having their tonsils and adenoids removed. To the untrained eye, the posterior pharynx may look severely infected. However, the normal healing process involves the formation an eschar over the incised area, usually extending across the entire posterior pharynx and appearing yellow, white, and occasionally black in some places. This usually sloughs off in 5 days. Bleeding from this area may occur. Patients are advised to initially try icing; however, if there is a large amount of bleeding, the patient should return to the emergency department. Overnight observation is typically warranted to ensure hemostasis, and about half of these patients need to be taken the OR for revision. Tweedie et al performed a retrospective review of post-operative complications. Those at highest risk of post-operative complications were patients with Down syndrome, cardiac disease, obesity, cerebral palsy, craniofacial anomalies, mucopolysaccharidoses, and hemoglobinopathy.28 The most common complaint was respiratory distress, especially in the aforementioned patients. Other complaints include fever, odynophagia, and uvular edema.27 Of the 1735 patients, only seven returned to the operating room for hemorrhage.28 Gallagher et al performed a study involving surgical techniques in 4776 children. Post-operative bleeding was more common in older children compared to younger kids.27
Surgical Complications
One complication of adenoidectomy is uvular necrosis. Most often this is iatrogenic, due to intubation. However, isolated cases have also been reported in patients undergoing endoscopy.29-33 It is thought that ischemia occurs due to impingement of the uvula against the hard palate or posterior oropharynx either by the scope or by the orotracheal tube during the procedure. The uvula then swells and may become necrotic or even ulcerate. It often appears elongated, with the tip of the uvula turning white.34 Patients complain of a sore throat persisting past the usual duration for post-operative throat pain, as well as a sensation of a foreign body in their mouth.29 After 5-14 days, the patient should report relief of symptoms, often with the tip slouching off.30-33
Figure 5: Eschar of the Uvula
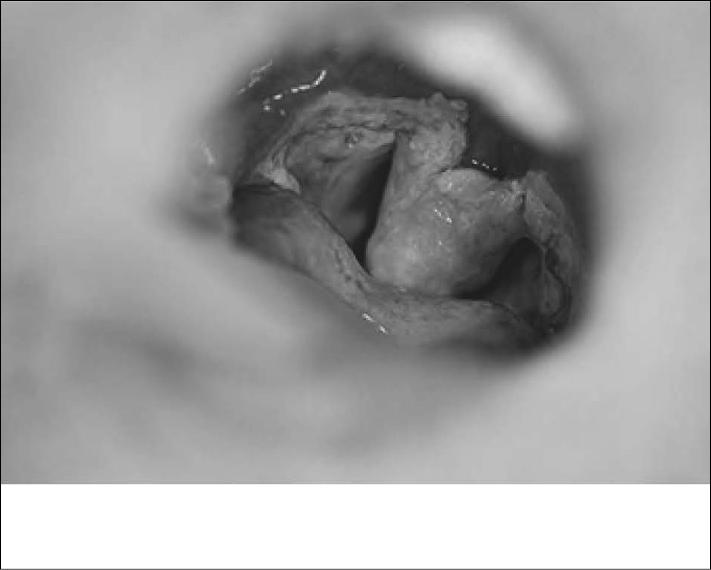
Eschar of the uvula in a 17-year-old girl four days following tonsillectomy and adenoidectomy.
Aside from oropharyngeal intubation and endoscopy, isolated cases of uvular necrosis have also been reported in patients after undergoing aggressive oropharyngeal suctioning,29,32 bronchoscopy,34 or even after use of a laryngeal mask airway.35 Regardless of the cause of uvular necrosis, conservative management is recommended, usually with observation, pain control, steroids, and in some cases epinephrine.29-31,35 If conservative management is ineffective, surgical removal of the uvula is advised.
Cultural Uvulectomy
Since ancient times, the uvula has been thought to contribute to a range of maladies, including cough, upper respiratory infections, and reflux.39 Some cultures traditionally remove the uvula in infancy while others may wait for persistent disease manifestations attributed to the uvula.40-42 Prual et al reported that by the age of 5 years, almost 20% of children in Niamey, capital of Niger, had undergone removal of the uvula.41 Some African cultures believe that removal of the uvula facilitates breast feeding and speech development. Removal is done by traditional medicine, sometimes using a special knife or by tying a horse hair tied around the tissue. Complications include throat pain, aspiration into the airway of the cut uvula, hemorrhage, and infections such as neck abscesses and tetanus.41,42 Obstructive sleep apnea and snoring caused by palatal stenosis resulting from traditional uvulectomy during childhood has been reported.43
Hemangiomas
Cavernous hemangiomas involve rapid proliferation of blood vessels during early childhood, followed by slow involution. They are usually soft and painless and rarely resolve completely. Most develop in the head and neck region, usually sparing the oral mucosa. However, adult hemangiomas occur more frequently in the oral mucosa in areas of trauma, namely the tongue or lips, although rare cases have been reported with involvement of the uvula. Most hemangiomas do not necessitate surgery. Management includes treatment with steroids, sclerotherapy, cryotherapy, or surgical removal. Two separate laser techniques are used: CO2 laser therapy and neodymium:yttrium-aluminum garnet (Nd-YAG).36 In an isolated case reported by Thong et al, a middle-aged man presented with a chief complaint of sleep apnea. On examination, the individual had a large, bluish-colored uvula. Nasal endoscope showed extension to the nasal portion of the soft palate. Removal of the uvula using CO2 laser therapy resolved the patient’s symptoms.36
Figure 6: Idiopathic Necrosis of the Uvula
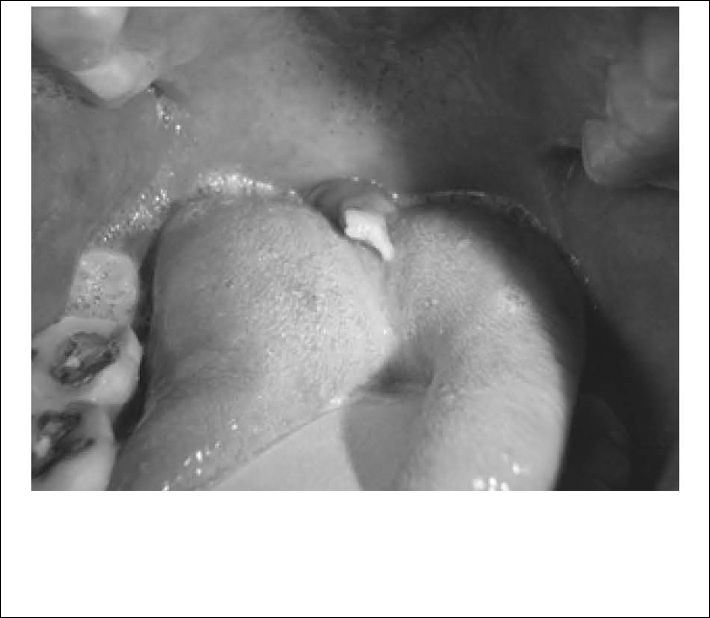
Idiopathic necrosis of the uvula in a 31-year-old male who presented for evaluation of physical changes noted to his uvula. The patient denied any trauma or infections.
Oncologic
Cancer of the uvula is rare. The most common type is papillomas secondary to a viral infection, namely HPV-6 and HPV-11. This typically causes a fibrous protrusion on the uvula, which may result in elongation and a choking/gagging sensation. Surgical incision leads to resolution of symptoms.21
Carcinomas of the oropharynx typically involve the tongue and oral mucosa. Rarely, they involve the uvula, although they are considered a very aggressive tumor when they do. Restrepo et al performed a retrospective study evaluating the frequency and characteristics of uvular carcinomas, as well as patient outcome. They found that most patients presented with T1 or T2 size lesions. Despite primarily being only T1 or T2, many tumors were able to metastasize, as the tumor may have been more developed, but was restricted visibly by the size of the uvula. Metastasis is via the lymphatic system, although lymphadenopathy may be absent, unilateral, or bilateral. In lesions greater than 1 cm, cervical lymph node metastasis was present 92.9% of the time. The treatment of choice for uvular carcinoma is uvula removal with bilateral cervical lymph node dissection. Patients diagnosed with stage I and II of the disease have a good chance of surviving without any disease complications. However, of the individuals diagnosed in stage III and IV, 78.5% ended up dying of further disease complications.37
Goldman et al described a case of neuroendocrine carcinoma. Although carcinoid tumors rarely involve the head and neck, they are sometimes found in the larynx. In this case, the patient presented with a feeling of something being stuck in the back of his throat. On exam, the patient had a 2 cm lesion on the uvula, as well as bilateral cervical adenopathy. A biopsy of the uvular lesion showed a poorly differentiated carcinoma of unknown type, but subsequent neck dissection did not show any lymph node involvement.38
Congenital Variants
Not all abnormal-appearing uvulas are a sign of pathology. There are some normal variants that occur, including the bifurcate uvula and elongated uvula. The bifurcate uvula occurs when the uvula undergoes partial fusion, resulting in a single trunk and two tips. In and of itself, it has no impact on development or speech in the individual and is merely an interesting deviation. However, when the uvula is split completely in half, this may be indicative of incomplete palatal fusion.1
Additionally, the uvula can also grow longer, sometimes reaching the level of the vocal cords. This can cause irritation, cough, vomiting, dysphagia, and sleep apnea. If asymptomatic, no treatment is necessary. However, if symptoms persist, a uvulectomy may be performed.2 Although generally considered a benign disorder, uvular elongation can be fatal. Nachman et al present a case in which an infant died of asphyxiation due to an elongated uvula becoming lodged between the vocal cords. Another concern for uvular elongation is that there may be a correlation in patients having an increased risk of developing uvulitis.5
Vascular
Vascular alterations such as superior vena cava syndrome, ligature of the internal jugular vein, and obstruction of lymphatic flow after ligature of the thoracic duct have been reported to cause uvular swelling.5 Additionally, uvula swelling can occur as part of the presentation of a vasculitis such as Kawasaki syndrome.44
Conclusion
The posterior pharynx is often visualized to evaluate for pharyngitis, coxsackie viruses, or for petechiae. The uvula itself is commonly overlooked, except in cases in which it looks vastly abnormal. Some may be regular anatomical variants, while others may be indicators of a life-threatening illness. All patients presenting with isolated uvulitis should have a thorough history and physical exam, in particular noting any recent drug use (legal or illegal), surgical procedures, or recent fevers/illness. If the patient presents with fever and an erythematous uvula, a lateral soft-tissue film should be obtained to evaluate for epiglottitis, and antibiotics should be started. If an ACE inhibitor is involved or there is a concern for hereditary angioedema, the patient should be examined with a fiberoptic endoscope to evaluate for concurrent laryngeal edema. The physician should also inquire about recreational drug use, as there have been many reports of isolated angioedema due to cannabis and crack inhalation injuries.
References
- Friedman O, Wang T, Milczuk H. Chapter 186: Cleft Lip and Palate. In: Flint, Cummings. Otolaryngology Head & Neck Surgery, 5th edition, 2010.
- Marom T, Roth Y, Cinamon U. Elongated uvula. Ear Nose Throat J 2010;89(7):E38.
- Woodson G. Chapter 56: Laryngeal and Pharyngeal Function. In: Flint, Cummings. Otolaryngology Head & Neck Surgery, 5th edition, 2010.
- Finkelstein Y, Meshorer A, Talmi YP, Zohar Y, Brenner J, Gal R. The riddle of the uvula. Otolaryngol Head Neck Surg 1992;107(3):444-450.
- Alcoceba E, Gonzalez M, Gaig P, Figuerola E, Auguet T, Olona M. Edema of the uvula: Etiology, risk factors, diagnosis, and treatment. J Investig Allergol Clin Immunol 2010;20(1):80-83.
- McNamara RM. Clinical characteristics of acute uvulitis. Am J Emerg Med 1994;12(1):51-52.
- Mohseni M, Lopez MD. Images in emergency medicine. Uvular angioedema (Quincke’s disease). Ann Emerg Med 2008;51(1):8, 12.
- Huang CJ. Isolated uvular angioedema in a teenage boy. The Internet Journal of Emergency Medicine. 2007;3(2). Last accessed 26 January 2013.
- Le Blanc C, Jenkins C, Godsoe S. Acute uvulitis in the ED. Canadian Journal of Diagnosis 2008. Last accessed 26 January 2013.
- Banerji A. Hereditary angioedema: Classification, pathogenesis, and diagnosis. Allergy Asthma Proc 2011;32(6):403-407.
- Vasekar M, Craig TJ. ACE inhibitor-induced angioedema. Curr Allergy Asthma Rep 2012;12(1):72-78.
- Stewart M, McGlone R. Fresh frozen plasma in the treatment of ACE inhibitor-induced angioedema. BMJ Case Rep 2012; Aug 24.
- Illing EJ, Kelly S, Hobson JC, Charters S. Icatibant and ACE inhibitor angioedema. BMJ Case Rep 2012; Aug 30.
- Bas M, Greve J, Stelter K, Bier H, Stark T, Hoffmann TK, Kojda G. Therapeutic efficacy of icatibant in angioedema induced by angiotensin-converting enzyme inhibitors: A case series. Ann Emerg Med 2010;56(3):278-282.
- Schmidt PW, Hirschl MM, Trautinger F. Treatment of angiotensin-converting enzyme inhibitor-related angioedema with the bradykinin B2 receptor antagonist icatibant. J Am Acad Dermatol 2010;63(5):913-914.
- Tennant FS Jr, Prendergast TJ. Medical manifestations associated with hashish. JAMA 1971;216(12):1965-1969.
- Mallat A, Roberson J, Brock-Utne JG. Preoperative marijuana inhalation — an airway concern. Can J Anaesth 1996;43(7):691-693.
- Guarisco JL, Cheney ML, LeJeune FE Jr, Reed HT. Isolated uvulitis secondary to marijuana use. Laryngoscope 1988;98(12):
1309-1312. - Boyce SH, Quigley MA. Uvulitis and partial upper airway obstruction following cannabis inhalation. Emerg Med (Fremantle) 2002;14(1):
106-108. - Chua KB, Lam SK, AbuBakar S, Lim ST, Paranjothy M, Koh MT, Lee WS. The predictive value of uvulo-palatoglossal junctional ulcers as an early clinical sign of exanthem subitum due to human herpesvirus 6. J Clin Virol 2000;17(2):83-90.
- Goodstein LA, Khan A, Pinczewski J, Young VN. Symptomatic squamous papilloma of the uvula: Report of a case and review of the literature. Case Report Otolaryngol 2012;2012:329289. Epub 2012 Apr 17.
- McNamara R, Koobatian T. Simultaneous uvulitis and epiglottitis in adults. Am J Emerg Med 1997;15(2):161-163.
- Baruah B, Goyal A, Shunyu NB, Lynrah ZA, Raphael V. Tuberculosis of nose and palate with vanishing uvula. Indian J Med Microbiol 2011;29(1):63-65.
- Kumar V, Singh AP, Meher R, Raj A. Primary tuberculosis of oral cavity: A rare entity revisited. Indian J Pediatr 2011;78(3):354-356.
- Kakisi OK, Kechagia AS, Kakisis IK, Rafailidis PI, Falagas ME. Tuberculosis of the oral cavity: A systematic review. Eur J Oral Sci 2010;118(2):103-109.
- Krober MS, Weir MR. Acute uvulitis apparently caused by Candida albicans. Pediatr Infect Dis J 1991;10(1):73.
- Gallagher TQ, Wilcox L, McGuire E, Derkay CS. Analyzing factors associated with major complications after adenotonsillectomy in 4776 patients: Comparing three tonsillectomy techniques. Otolaryngol Head Neck Surg 2010;142(6):886-892.
- Tweedie DJ, Bajaj Y, Ifeacho SN, Jonas NE, Jephson CG, Cochrane LA, Hartley BE, Albert DM, Wyatt ME. Peri-operative complications after adenotonsillectomy in a UK pediatric tertiary referral centre. Int J Pediatr Otorhinolaryngol 2012;76(6):809-815.
- Calikapan GT, Karakus F. Uvula necrosis after endotracheal intubation for rhinoplasty. Aesthetic Plast Surg 2008;32(4):710-711.
- Shores NJ, Bloomfeld RS. Images in clinical medicine. Uvular necrosis after endoscopy. N Engl J Med 2009;361(12):e20.
- Evans DP, Lo BM. Uvular necrosis after orotracheal intubation. Am J Emerg Med 2009;27(5):631.
- Tang SJ, Kanwal F, Gralnek IM. Uvular necrosis after upper endoscopy: A case report and review of the literature. Endoscopy 2002;34(7):
585-587. - Commins DJ, Whittet H, Okoli UC, Ewart M. Postintubation uvular necrosis. Anaesthesia 1994;49(5):457-458.
- Sunio LK, Contractor TA, Chacon G. Uvular necrosis as an unusual complication of bronchoscopy via the nasal approach. Respir Care 2011;56(5):695-697.
- Emmett SR, Lloyd SD, Johnston MN. Uvular trauma from a laryngeal mask. Br J Anaesth 2012;109(3):468-469.
- Thong JF, Pang KP, Siow JK. Haemangioma of the uvula causing loud habitual snoring — a rare entity. Med J Malaysia 2008;63(5):408-409.
- Espinosa Restrepo F, Martínez Capoccioni G, Martín Martín C. T1-T2 squamous cell carcinoma of the uvula: A little big enemy. Otolaryngol Head Neck Surg 2012;146(1):81-87.
- Goldman NC, Barnes RE Jr. Atypical carcinoid (moderately differentiated neuroendocrine carcinoma) of the uvula. Ear Nose Throat J 2012;91(2):75-76.
- Nachman R, Krispin A, Nnoli M, Hiss J. Infantile asphyxia due to aberrant uvula — an anatomic misadventure. J Forensic Leg Med 2010;17(7):401-403.
- Hodes R. Cross-cultural medicine and diverse health beliefs. Ethiopians abroad. West J Med 1997;166(1):
29-36. - Prual A, Gamatie Y, Djakounda M, Huguet D. Traditional uvulectomy in Niger: A public health problem? Soc Sci Med 1994;39(8):1077-1082
- Adeyi A, Nimkur TL. The traditionally amputated uvula amongst Nigerians: Still an ongoing practice. ISRN Otolaryngology 2011;125(9):982-986.
- Ravesloot MJ, de Vries N. "A good shepherd, but with obstructive sleep apnoea syndrome": Traditional uvulectomy case series and literature review. J Laryngol Otol 2011;125:982-986.
- Kazi A, Gauthier M, Lebel MH, Farrell CA, Lacroix J. Uvulitis and supraglottitis: Early manifestations of Kawasaki disease. J Pediatr 1992;120(4 Pt 1):564.
Want to earn free Emergency Medicine CME courses? With FreeCME you can earn accredited CME courses for free online. Get started today!
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
