Guest Column: How to make NuvaRing an option for patients

How to make NuvaRing an option for patients
By Robert Hatcher, MD, MPH
Professor of Gynecology and Obstetrics
Emory University School of Medicine
Atlanta
While some clinicians think women will not be willing to place a foreign body into the vagina and then remove it, other providers have been successful in introducing women to the vaginal contraceptive ring (NuvaRing, Schering-Plough Corp.; Kenilworth, NJ). Exactly how is the method presented to women by those clinicians?
Outliers can be extraordinarily instructive to people trying to gain acceptance for their product. We can learn from ordinary people who achieve extraordinary results. Look at this example: a producer of soft ice cream machines received an order to send two machines to one address. It had never happened before . . . two of these huge machines being sent to a single site. The producer flew from Chicago to Los Angeles where he found a very effective purveyor of fast foods. In this way, Ray Kroc met the owner of the first McDonald's. They decided to work together. And, as they say, the rest is history.
I heard that some clinicians were finding women very receptive to the NuvaRing, while others had never prescribed them and said that their patients really didn't like the idea of placing something into their vagina. I wanted to know what was going on in the offices extensively prescribing the contraceptive. Three years after NuvaRing was approved for U.S. use, I contacted five nurse practitioners and five physicians by telephone. All were happy to talk about this vaginal contraceptive. I asked each clinician four questions:
- Of 100 of your patients using a combined hormonal contraceptive, what percentage will use pills, NuvaRing, and Ortho Evra patches?
- What are you doing to introduce NuvaRing to women?
- To what extent are your patients using NuvaRing for extended periods of time or continuously?
- What seems to be the feature women like best about this method?
Look at frequency
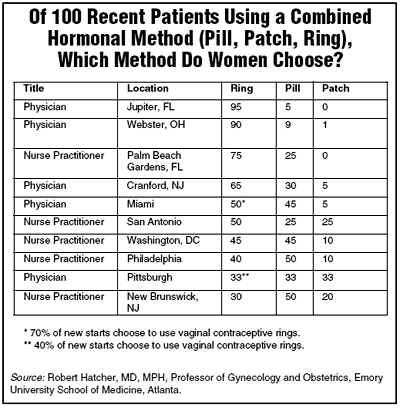
The below table outlines the extent of use of NuvaRing in 10 practices. Findings indicate that 30%-95% of all women using a combined hormonal contraceptive were using the vaginal contraceptive ring.
All of the surveyed clinicians were positive in their comments about the method's convenience, acceptability, and low incidence of side effects. All of them report routinely offering to place a NuvaRing for their patient to demonstrate that it is easy to insert and does not cause discomfort. Two clinicians indicated that if acceptable to the patient, they will insert the ring after doing the Pap smear. They virtually make placement of a ring a routine part of the exam in order to demonstrate its ease of insertion.
Women were asked by eight of the 10 clinicians if they would like to remove and then reinsert the ring themselves. The clinician left the room, the patient removed and reinserted the vaginal ring, and then told the clinician if she wanted to try this contraceptive.
One clinician describes the process: "If a woman is interested in the ring, I insist on them putting it in and taking it out. I leave the room, have them remove the ring I have just inserted, and then they put it back in themselves. If they don't like the ring, I have them throw it away. Usually they are smiling when I return to the room, and they leave with the ring in place."
One clinician said Food and Drug Administration approval of extended-regimen oral contraceptives has increased the acceptability of extended and continuous use of all three combined hormonal methods (pills, patches, and rings). The percentage of women choosing to use NuvaRing in a continuous regimen in this set of 10 clinicians ranged from 25% to 97%. One clinician who provides most of the contraceptives for residents at her institution finds that almost all of them use the ring on a continuous basis.
What do women like most about the contraceptive vaginal ring? All of the surveyed clinicians say it is the convenience of inserting the ring and having nothing to do for a month. Other positive features include the low incidence of hormonal side effects and the decreased incidence of previously troublesome cyclic symptoms if the ring is used for an extended time, clinicians note. Removal of the NuvaRing at the time of intercourse is uncommon among the women, the clinicians report.
What does it take?
The Wal-Mart pharmacy near one of the surveyed clinicians might become the first in the country to have to purchase a second refrigerator to store all the NuvaRings prescribed for more than 1,500 patients! This exercise inspires me to look for outliers providing the levonorgestrel intrauterine system, another superb contraceptive, to high percentages of women.
The NuvaRing is a safe, effective, easy-to-use, and convenient contraceptive.1,2 It remains effective for up to 35 days. This permits clinicians to teach women choosing this method to remove their ring and insert a new ring the first day of each month, or any other date of the month they can easily remember. Discuss this ease of use, and demonstrate insertion and removal, to help women achieve success with the vaginal contraceptive ring.
References
- Alexander NJ, Baker E, Kaptein M, et al. Why consider vaginal drug administration? Fertil Steril 2004; 82:1-12.
- Roumen F, Apter D, Mulders TM, et al. Efficacy, tolerability, and acceptability of a novel contraceptive vaginal ring releasing etonogestrel and ethinyl estradiol. Hum Reprod 2001; 16:468-475.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
