2009 Salary Survey Results: Infection preventionists hold the battered line amid devastated economy, H1N1 flu pandemic
2009 Salary survey Results
Infection preventionists hold the battered line amid devastated economy, H1N1 flu pandemic
Freeze out: A third of IPs receive no raises in 2009
After an economic wildfire that swept through health care and laid waste to entire industries in other sectors, infection preventionsts may be a little singed around the edges — but they're still standing.
The majority even got some kind of raise, underscoring their longstanding job security and value to health care facilities in age of patient safety and increasing liability for health care-associated infections, according to the 2009 salary survey by Hospital Infection Control & Prevention.
Sure, we're drawing the glass half full here, in part in contrast to corporate America, much of which has been sitting on empty, its employees clinging to jobs and having long forgotten raises. But the great "Decession" took its toll on health care as well, often considered a recession-proof harbor in any economic storm. As a result, 32% of infection preventionists reported no raises for the period, up from the 20% that reported no wage growth in 2007 and 14% in 2006.
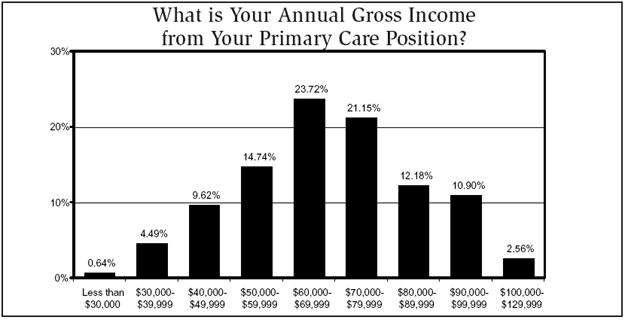
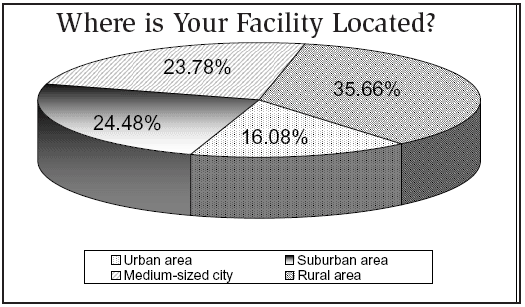
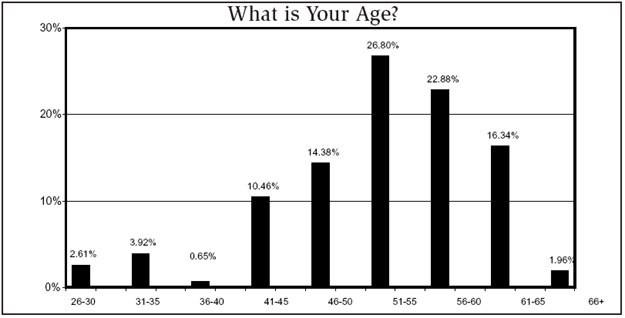
The 2009 survey found a median salary for IPs in the $60,000 to $69,999 range, the same as the previous year. The median age range of the 157 respondents was 51 to 55 years old, with most working in small to midsize hospitals of 300 beds or less. In salary percentage breakdowns, 10% were making $40,000 to $49,999; 15% were paid $50,000 to $59,999; and 24% had salaries in the $60,000 to $69,999 range. Another 21% were in the 70,000 to $79,999 range.
A glass half empty
It's not hard to take a "half-empty" view of a glass that may even have a few hairline cracks upon closer inspection. And why not? As the federal government scrambled to offset a complete economic collapse, the hospital sector began to take a beating. According to the American Hospital Association, the economic crisis struck hospitals hard and is still manifest in the following trends:
- The proportion of emergency department patients without insurance is increasing.
- A higher proportion of patients are unable to pay for care and many hospitals are seeing more patients covered by Medicaid and other public programs for low-income populations.
- Fewer patients are seeking inpatient and elective services raising concerns that individuals are putting off needed care.
- Community need for subsidized services such as clinics, screenings and outreach is increasing even as charitable contributions are down for many hospitals.
As a result of such trends, infection preventionists and their colleagues in other health care fields saw support staff, travel budgets — and anything else not nailed to the floor — swept away. The Association for Professionals in Infection Control and Epidemiology reported many IPs were having budgets slashed and critical functions such as surveillance undercut. In an online survey reported at the 2009 APIC conference 41% of respondents reported cuts in budgets for infection prevention. According to the APIC survey, nearly 40% had layoffs or reduced hours, and a third experienced hiring freezes.
 APIC is planning to repeat the survey, but the anecdotal evidence is that IPs are holding the line. "We have not heard of any additional staffing freezes, layoffs, and cutbacks beyond what we reported in that survey," says Kathy Warye, CEO of APIC. "This is just informed instinct — not data — but my sense is that institutions are kind of holding the line."
APIC is planning to repeat the survey, but the anecdotal evidence is that IPs are holding the line. "We have not heard of any additional staffing freezes, layoffs, and cutbacks beyond what we reported in that survey," says Kathy Warye, CEO of APIC. "This is just informed instinct — not data — but my sense is that institutions are kind of holding the line."
There are hopeful signs amid the debris, she tells HIC. "I have been hearing that health care institutions are performing better financially overall because patients with elective surgery and that sort of thing are starting to come back," Warye says. "As the economy has gotten a little bit better, health care organizations have seen some benefit from that. Their revenue sources, from what I understand, are starting to tic up just a bit, so hopefully we will not see any more additional cutbacks and freezes as the overall health care picture continues to improve."
Still, the H1N1 influenza A pandemic is exacting a heavy price in resources to departments already pared down to the bone by the economic situation. The other concerns is that these economic-driven cuts may become the "new normal" even as the economy rebounds, with health care administrators reluctant to restore funding and remove department constraints. "We are not hearing — and again this is anecdotal — that those resources are being restored," Warye says. "I think hospitals are just like every other business — once you cut something the tendency is to hold the line there. It is only with a very sound argument over time that resources begin to trickle back."
Joint Commission's critical role
A key ally in this fight will be The Joint Commission, which has increasingly emphasized the importance of infection prevention in its quality improvement initiatives. Indeed, the Joint Commission focused on improving hand hygiene problems as the first project of its Center for Transforming Healthcare. The new center is The Joint Commission's key foray into national health care reform, which must include a quality component — including preventing health care-associated infections (HAIs) — if it is to become an effective and affordable reality, says Mark Chassin, MD, MPP, MPH, president of The Joint Commission. "We know that for every HAI that is prevented, we will save money and we save the patient that suffering." Asked about budget woes and cutbacks widely reported by infection preventionists, Chassin said the Joint Commission has not lowered its expectations of hospitals due to the economic situation. "The Joint Commission standards and national patient safety goals — in other words, requirements for health care organizations that underpin safety and quality — don't change with economic fluctuations," he told HIC. "If we find that there is a problem with infection prevention and control, we will work with the organization to solve it whether it is a staffing problem, a training problem, or an implementation problem. We are not seeing in our own survey results any substantial increase in problems due to reduced staffing in these critical programs. But our surveyors look for that, as well as lack of compliance with requirements for other reasons."
In addition, a recently published paper on Joint Commission leadership standards specifically cited infection prevention, noting that "a hospital's performance is demonstrated through its performance with respect to other important hospitalwide systems, such as those for information management, infection control, and medication management."1
The challenge for APIC and individual IPs is to leverage such perceptions of increasing importance into the reality of restored and expanded resources.
"We are working very closely with the Joint Commission to increase their awareness and sensitivity to the resources issues," Warye says. "We need to continue with this drumbeat of evidence and messaging around infection prevention and control, and put more tools in our members' hands to make the 'business case.'"
APIC is currently developing a new tool to address IP staffing and resources. "It's not going to be a situation where we say you should have 'x' number of infection preventionists to 'x' number of beds because we know that hospitals are far more complicated than that," she says. "We are looking at a whole combination of human, technological and other resources so that an IP can come up with the best-case scenario of how to allocate those within her specific institution."
Reference
- Schyve, Paul. Leadership in healthcare organizations: A guide to Joint Commission leadership standards. Governance Institute, 2009: Available at: http://www.jointcommission.org.

Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
