Common Orthopedic Injuries in the Pediatric ED
Common Orthopedic Injuries in the Pediatric ED
Authors:
Lilliane M. Sarraff, MD, Fellow, Department of Emergency Medicine, Drexel University College of Medicine, St. Christopher's Hospital for Children, Philadelphia, PA.
Christopher J. Haines DO, FAAP, FACEP, Assistant Professor of Emergency Medicine and Pediatrics, Drexel University College of Medicine; Director, Department of Emergency Medicine and Medical Director, Critical Care Transport Team, St. Christopher's Hospital for Children, Philadelphia, PA.
Peer Reviewer:
John Santamaria, MD, FACEP, Affiliate Professor of Pediatrics, University of South Florida School of Medicine, Tampa, FL
Pediatric fractures are commonly encountered in the emergency department (ED). Approximately 50% of children will fracture a bone during childhood. The unique injury patterns, especially those involving the physis, require that clinicians have a complete and thorough understanding of appropriate diagnostic and management strategies to maximize a child's potential for an optimal outcome. Part I of this two-part series on common orthopedic injuries in the pediatric ED focuses on injuries to the clavicle and upper extremities. Part II will focus on injuries to the lower extremities.
The Editor
Introduction
Musculoskeletal injuries account for approximately 10%-15% of the 10 million annual visits to U.S. pediatric EDs.1 Skeletal fractures represent the majority of injuries, with rates continuing to increase. It is estimated that approximately half of all children will fracture a bone during childhood.1 Most childhood fractures occur as a result of mild to moderate trauma during play and sports. Although fractures vary considerably with age, sex, and maturation, the peak occurs in early puberty.2 Further, it is important to consider other possible etiologies when a child presents with bony pain, especially without a history of trauma. The differential diagnosis should include the following: physical abuse, malignancy, osteogenesis imperfecta, and rickets.
Anatomy
The major anatomic regions of growing bone include the epiphysis, physis (growth plate), metaphysis, and diaphysis. The metaphysis is the wider part of the end of the long bone, adjacent to the epiphyseal disk. The diaphysis is the shaft of the long bone. The epiphysis is the secondary ossification center located at the end of long bones and is separated from the rest of the bone by the cartilaginous physis. The epiphysis is cartilaginous at birth, with the exception of the distal femur.3 This cartilaginous epiphysis serves as a shock absorber, transmitting forces to the metaphysis. Throughout childhood and adolescence the cartilage skeleton begins to ossify with subsequent increase in force transmission to the physis.4 The physis, or growth plate is located between the distal epiphysis and the proximal metaphysis, and is the primary center of longitudinal long bone growth. The epiphyseal cartilage cells grow toward the metaphysis and form columns of cells that degenerate, undergo hypertrophy, and then calcify to form new bone. The epiphyseal cartilage cells stop duplicating at the end of puberty. As a result, epiphyseal growth develops at the site secondary to replacement by bone. This epiphyseal growth promotes rapid healing of fractures in the pre-pubertal population.
The major anatomic differences between the adult and pediatric skeletal system include the presence of the preosseous cartilage, physis and a stronger osteogenic periosteum. Additional differences between pediatric and adult orthopedic injuries can be attributed to the mineral content of bone and the strength of ligaments. Secondary to lower mineral content, the long bones of children are less dense and more porous than those of adults. This difference in mineral content allows the absorption of more energy prior to fracture and deformation. In addition, ligaments of children are stronger than the immature bones in which they are attached. As a result, injury patterns are the opposite of the adult population with pediatric fractures occurring more commonly than ligamentous injuries.5
Healing Differences
Fracture healing involves the following three stages: inflammatory, reparative, and remodeling. Healing of a fractured bone in children begins immediately after the injury with resultant bleeding, inflammation and swelling. Mesenchymal cells are then activated and start laying down new bone. The stronger periosteum in children enhances more rapid formation of a callus and healing. The most unique property of immature bone is the capacity to remodel over time via a combination of periosteral resorption and new bone formation.4 This remodeling potential allows for a greater degree of longitudinal misalignment and angulation.3 However, there are several factors that can affect fracture remodeling including age, proximity to the joint, and the relationship of the deformity to the joint axis of motion. Specifically, fractures that occur in younger children as well as those that occur in close joint proximity have greater potential for remodeling. On the contrary, displaced intra-articular fractures, diaphyseal fractures, and deformities not in the plane of joint axis of motion, will remodel less effectively and therefore require more precise anatomic reduction.6
Fracture Patterns
Pediatric fracture patterns can be approached methodically. When describing a fracture, the following should be included; anatomic location, configuration of the fracture, relationship of the fracture fragments, as well as the relationship of the fracture fragments to the adjacent tissue.
The configuration of the fracture can be classified into the four unique types of fractures seen in children; plastic deformity, buckle (torus) fractures, greenstick fractures, and the physeal fractures.2,7
Plastic Deformity. A plastic deformity is also known as a bowing deformity. This deformity occurs when longitudinal force exceeds the ability of bone to recoil to normal position. As a result the cortex of the diaphysis bends, without visible fracture secondary to the thick pediatric periosteum. Microscopic fractures occur dissipating energy along the side of tension with resultant bowing and plastic deformity. These fractures commonly occur in the long bones of the lower arm and leg and may be associated with a second fracture. This fracture pattern decreases in incidence with increased bone maturity. Radiographically, a fracture line will not be visible, and the bone will display excessive bowing without actual cortical disruption.1,3,6 (See Figure 1.) In addition, if plastic deformity is suspected, additional comparison views may aid in the diagnosis. These fractures typically are stable, and when the bowing deformation is less than 20°, or occurs in a younger child, the angulation will frequently correct itself through remodeling and will not require orthopedic surgical intervention.3
Figure 1. Plastic Deformity or Bowing Deformity of the Left Ulna
Yamamoto L, Inaba A, DiMauro R. Radiology cases in Pediatric Emergency Medicine. Medical Center For Women And Children, Department of Pediatrics, University of Hawaii John A. Burns School of Medicine 1999; Vol. 6, Case 16. Available at www.hawaii.edu/medicine. Used with permission.

Buckle (Torus) Fractures. A torus fracture occurs at the junction between the porous metaphysis and the denser diaphysis. This fracture type is the result of longitudinal forces on the bone with compressive buckling secondary to the porous nature of pediatric bone. This buckling appears as a bulge in the metaphyseal cortex with concomitant disruption of the normal bone contour. (See Figure 2.) This fracture pattern occurs most commonly in the distal radius but can be seen in any long bone as a result of longitudinal trauma. These fractures are stable and heal in 2-3 weeks with immobilization.1,3,5,6
Figure 2. Left Radius and Ulna Buckle Fractures
Image courtesy of St. Christopher's Hospital for Children Radiology Department, Philadelphia, PA.
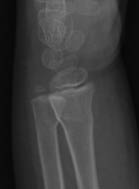
Greenstick Fractures. A greenstick fracture occurs when a bone is angulated beyond the limits of plastic deformity. This pattern is characterized as an incomplete fracture with metaphyseal cortical disruption on the side of tension and an intact bending, or plastic deformity, on side of compression. (See Figure 3.) This fracture type is stable and heals within 3-4 weeks. This type of fracture may have the highest risk of re-fracture, as some authors have published rates of greater than 80%.1,8
Figure 3. Greenstick Fracture
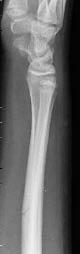
Physeal Fractures. The most significant difference between pediatric and adult fractures is the presence of long-bone growth plates. These growth plates are highly susceptible to fracture, since their cartilaginous composition represents a weak point in the bone.
Physeal injuries have been reported to represent up to 18% of all pediatric fractures. This injury type occurs commonly during times of rapid growth through the weakest part of the physis, the hypertrophic cell zone.5 Fractures in this zone can result in asymmetric bone growth followed by deformity if not treated properly. Growth plate injuries occur most commonly in the following age ranges: 9-12 years for females, and 12-15 years for males.1 The separation of the distal radial physis is the most common growth plate injury.7
Several classification schemes exist to describe physeal injuries including Salter-Harris, Odgen, Peterson, and many others. The Salter-Harris classification system is used most frequently secondary to the ease of application and relevance to the treatment and prognosis of pediatric fractures.
Salter-Harris Classification
This classification system grades physeal fractures as types I through V. Although controversial and joint dependent, generally the higher the Salter-Harris fracture type number, the greater the chance of growth plate arrest and joint incongruity.1 (See Figure 4.)
Figure 4. Salter-Harris Classifications
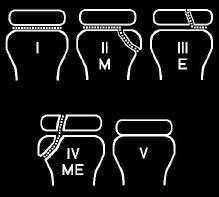
Yamamoto L, Inaba A, DiMauro R. Radiology cases in Pediatric Emergency Medicine. Medical Center for Women and Children, Department of Pediatrics, University of Hawaii John A. Burns School of Medicine 1994; Vol. 1, Case 18. Available at www.hawaii.edu/medicine. Used with permission.
Type I Salter-Harris Fracture. A type I fracture involves the separation of epiphysis from the physis with the reproductive cells of the physis remaining attached to the epiphysis. These injuries can result in both displaced and non-displaced epiphyses. Radiographic abnormalities consistent with type I fractures may be subtle with only soft tissue swelling and / or joint effusion without visible fracture.5 (See Figure 5.) The clinical presentation of a Salter-Harris type I fracture is generally significant point tenderness over the affected growth plate. The treatment of nondisplaced type I fractures consists of immobilization, ice, elevation, and outpatient referral to an orthopedic surgeon for further care; displaced fractures require orthopedic consultation. Fortunately, these fractures rarely result in growth disturbances and prognosis is excellent with proper treatment and referral.1
Figure 5. Salter-Harris Type I Fracture
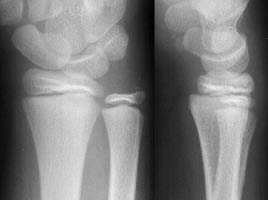
Lateral view shows displaced radial epiphysis; also visible is a small fracture of the ulnar styloid.
Yamamoto L, Inaba A, DiMauro R. Radiology cases in Pediatric Emergency Medicine. Medical Center for Women and Children, Department of Pediatrics, University of Hawaii John A. Burns School of Medicine 1994; Vol. 1, Case 18. Available at www.hawaii.edu/medicine. Used with permission.
Type II Salter-Harris Fracture. Type II fractures are the most common Salter-Harris fracture involving the physis and metaphysis. This fracture type results in a triangular metaphyseal fragment that is commonly referred to as the Thurston-Holland fragment. (See Figure 6.) This fragment of metaphysis remains attached to the epiphysis. The treatment and prognosis are similar to that of a Type I fracture.1,3,5
Figure 6. Salter-Harris Type II Fracture
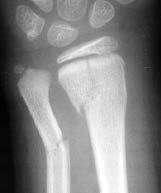
Fracture extends from the metaphysis into the physis, with associated physeal widening; associated green-stick fracture of the distal ulna.
Yamamoto L, Inaba A, DiMauro R. Radiology cases in Pediatric Emergency Medicine. Medical Center for Women and Children, Department of Pediatrics, University of Hawaii John A. Burns School of Medicine. 1994; Vol. 1, Case 18. Available at www.hawaii.edu/medicine. Used with permission.
Type III Salter-Harris Fracture. A type III fracture begins intra-articularly and involves the epiphysis and the physis. (See Figure 7.) The treatment and prognosis of type III fractures are directly related to the achievement of anatomical fragment alignment. Although closed reduction can be achieved in the minority of cases, open reduction is common and minimizes the potential for growth and joint abnormalities. Immediate ED treatment while awaiting orthopedic consultation should include pain control and immobilization.1,3,5
Figure 7. Salter-Harris Type III Fracture
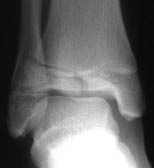
Fracture of the distal tibia involving the articular surface. The fracture extends through the epiphysis and physis.
Yamamoto L, Inaba A, DiMauro R. Radiology cases in Pediatric Emergency Medicine. Medical Center for Women and Children, Department of Pediatrics, University of Hawaii John A. Burns School of Medicine. 1994; Vol. 1, Case 18. Available at www.hawaii.edu/
medicine. Used with permission.
Type IV Salter-Harris Fracture.Type IV fractures originate in the articular space and travel through the epiphysis, physis, and the metaphysis. (See Figure 8.) Similar to type III fractures, there may be significant growth disturbance without precise anatomic alignment. As a result, the preferred method of repair includes open surgical reduction with internal fixation.1,3,5
Figure 8. Salter-Harris Type IV Fracture
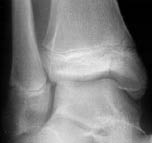
Fracture of the medial malleolus extending from the inferior articular surface of the tibial epiphysis through the physis and metaphysis.
Yamamoto L, Inaba A, DiMauro R. Radiology cases in Pediatric Emergency Medicine. Medical Center for Women and Children, Department of Pediatrics, University of Hawaii John A. Burns School of Medicine. 1994; Vol. 1, Case 18. Available at www.hawaii.edu/
medicine. Used with permission.
Type V Salter-Harris Fracture. In type V fractures, compressive forces are transmitted through the epiphysis into the physis. This force results in a crush injury with disruption of the germinal matrix, hypertrophic region, and vascular supply. This type of fracture occurs most commonly in joints that move in one plane (knee and ankle) and is frequently misdiagnosed as a type I fracture.9 These fractures can be difficult to diagnose secondary to normal appearing radiographs with minimal epiphyseal displacement or joint effusion. The clinical history and the mechanism of injury (axial load) in combination with normal appearing radiographs should alert the clinician to the potential for a type V fracture. (See Figure 9.) The prognosis for this injury is poor secondary to the risk of premature growth cessation and subsequent limb shortening. Treatment should include pain management, immobilization, and orthopedic consultation.
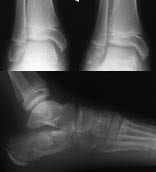
Figure 9. Salter-Harris Type V Fracture
Salter-Harris Type V fracture of the distal tibia was suspected after a fall from second-floor balcony.
Yamamoto L, Inaba A, DiMauro R. Radiology cases in Pediatric Emergency Medicine. Medical Center for Women and Children, Department of Pediatrics, University of Hawaii John A. Burns School of Medicine 1994; Vol. 1, Case 18. Available at www.hawaii.edu/medicine. Used with permission.
Complete Fractures. Complete fractures propagate through the entire bone.7 These fractures are sub-classified by fracture line appearance: transverse, spiral, oblique, and comminuted. A transverse fracture line occurs at a right angle to the long axis of the bone. Spiral fractures have fracture lines that are oblique, encircling a portion of the shaft of the bone. Oblique fractures have fracture lines that are 30° to 40° perpendicular to the long axis of the bone. A comminuted fracture site reveals multiple fragments.9
Clavicle Fractures
Introduction / Etiology. The clavicle is the most common location of a pediatric fracture. This fracture is seen at all ages and represents 10%-15% of all pediatric fractures.10 Newborn clavicle fractures occur as a result of birth trauma, whereas the mechanism of injury for children and adolescents typically includes a fall on an outstretched arm, shoulder, or direct blow.11 In infants and young children, clavicle fractures are usually greenstick type going unnoticed until callus formation. In older children, there is a greater tendency for complete displacement.7 The most common fracture location is the mid-shaft of the clavicle, which represents approximately 80% of all fractures. Although the clavicle is the first bone to ossify, (at five weeks of gestation) the physis is the last to close (at approximately 25 years of age).10 Therefore, as a result of the clavicle's active physis and strong vascular supply, there is potential for rapid healing and remodeling.
Anatomy. The clavicle serves as the connection between the upper extremity and the trunk. It articulates laterally with the acromion of the scapula (acromioclavicular joint) and medially with the sternum (sternoclavicular joint). The clavicle serves two purposes including upper extremity stability as well as protection of underlying neurovascular structures.10-12
The Allman classification divides the clavicle into thirds and is used to describe fracture location. Group I fractures are the most common involving the middle third of the clavicle where the bone is weakest. In addition to representing the weakest area of the clavicle, the middle third has minimal muscular and ligamentous support, which leads to predisposition to fracture. Group II fractures are the second most common location (15%-25%) involving the lateral or distal third of the clavicle. Group III fractures are the least common (5%) involving the medial, proximal third of the clavicle.11,14
Evaluation. Children with clavicle fractures may present to the ED with a variety of signs and symptoms. In a recent published study, symptoms of clavicle fracture were variable with up to 18% percent of patients presenting with normal physical exams.12,14 Commonly, children with clavicle fractures present to the ED with their arm adducted close to the body with the opposite extremity supporting the weight of the affected side.11,12,14 In addition, as a result of the fracture, the tension on the sternocleidomastoid muscle may cause head tilt toward the affected side with rotation of the chin to the contralateral side. Physical exam findings may be significant for point tenderness/crepitus with palpation, ecchymosis, or edema. Further, with completely displaced fractures, the physical exam may be significant for a shoulder that appears to be displaced inferiorly and medially. Although the incidence of complications is low, a careful exam should include neurovascular status, lung auscultation as well as close skin inspection to assess for an open fracture.
Radiographs. Children with suspected clavicle fractures should be imaged utilizing standard radiographs including an anteroposterior view and cranial/caudal tilt views. The cranial/caudal tilt views minimize rib and scapula overlap while assisting with visualization of fractures that are anteriorly and posteriorly displaced.10-12 (See Figure 10.) In rare cases, computed tomography (CT) may be needed for complex comminuted as well as distal/proximal clavicle fractures. In addition, CT imaging will allow better visualization of fractures involving the articular space.11
Figure 10. Right Mid-shaft Clavicle Fracture AP and
45° Views
Images courtesy of St. Christopher's Hospital for Children Radiology Department, Philadelphia, PA.
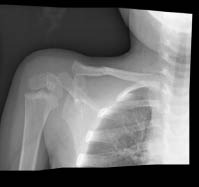
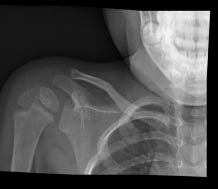
Treatment
The treatment goals include the restoration of normal anatomy, limitation of pain, and promotion of rapid recovery. In comparison to adults, most pediatric clavicle fractures heal rapidly without complication. The treatment of choice for clavicle fractures is immobilization, which should be utilized to provide comfort and pain control. The most common immobilization methods include a sling or figure-of-eight dressing. Although both methods have shown no difference in outcome, slings are more commonly used secondary to comfort and ease of use.12 The duration of immobilization varies based on child specific pain/comfort levels but is usually recommended for 1-4 weeks.
ED discharge instruction should include range of motion exercises and strengthening activities that may be started as tolerated. In addition, parents should receive education regarding the development of a callus after fracture. The callus will typically develop approximately 10 days after the initial injury and may remain for up to 6 months.12,14,15 Children with clavicle fractures should generally be referred to orthopedics for long-term follow-up and assistance with recommendations for full return to activity or sports.
It is common for young infants to present to the ED with swelling in the region of the clavicle. This presentation is typical of a clavicle fracture that was sustained at birth and noticed by parents in the first 10 days of life after callus formation. These infants require no further treatment with the exception of reassurance and education regarding the progression of the callous. Neonatal clavicle fractures typically heal rapidly and have an excellent prognosis.11,14,15
Surgical Indications
Pediatric clavicle fractures rarely require surgical management with most pediatric orthopedic surgeons preferring conservative management compared to open reduction.7 However, recent published studies have suggested that surgical management may be indicated and improves outcomes in select pediatric patients.16,17 Although more studies are needed, the current accepted indications for surgical management include open fractures, fracture associated with neurovascular injury, greater than one hundred percent displacement with skin tenting, or multiple fractures associated with a compromised chest wall.
Elbow Fractures
Introduction. Elbow fractures represent 15% of all pediatric fractures with supracondylar fractures occurring most commonly (50%-70%) followed by lateral condyle fractures.18 The unique anatomy of the elbow in conjunction with a potential for significant complications, requires prompt, accurate diagnosis and treatment.
Figure 11. Diagram of Elbow Ossification Centers
Yamamoto L, Inaba A, DiMauro R. Radiology cases in Pediatric Emergency Medicine. Medical Center for Women and Children, Department of Pediatrics, University of Hawaii John A. Burns School of Medicine 1994; Vol. 1, Case 11. Available at www.hawaii.edu/medicine. Used with permission.
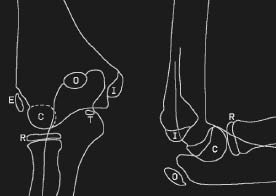
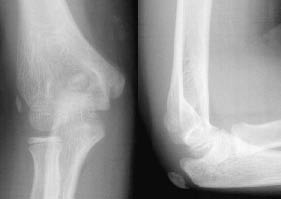
Anatomy. The pediatric elbow consists predominantly of cartilage, with secondary ossification centers of the elbow becoming calcified during childhood. During adolescence, these secondary ossification centers fuse to their respective long bones.19 The ossification growth centers in children appear in a predictable fashion based on the child's age and gender. The mnemonic CRITOE is used as an aid to assist clinicians in regard to time of ossification. (See Figure 11.) Knowledge of this sequence of ossification is paramount in distinguishing a fracture from a normal finding in the elbow. The capitellum "C" is the first ossification center to appear, and is usually formed by 1-2 years of age. The radial head "R" is the next to appear at 2-5 years of age, which is then followed by the medial or internal epicondyle "I" at 5-7 years. The trochlea "T" appears at 7-10 years of age, while the two final ossification centers; olecranon "O" and the lateral or external epicondyle "E" appear between 9-11 years of age. The ages of each center's appearance may be approximated by using odd numbers; capitellum (1 year), radial head (3 years), medial/internal epicondyle (5 years), trochlea (7 years), olecranon (9 years), and lateral/external epicondyle (11 years).14,20,21 The ossification sequence occurs slightly earlier in females when compared to males secondary to the onset of puberty. Although knowing the sequence and timing of ossification center fusing is helpful, there will likely be times when a comparison view is helpful to determine if a fracture is present.
Supracondylar Humerus Fractures
Epidemiology. Supracondylar humerus fractures are more common in males with the peak incidence occurring at 5-7 years of age. The vast majority of these fractures occur in the first decade of life secondary to falls. Factors contributing to the incidence include both ligamentous laxity and weakness in the bony architecture of the elbow.21-24 There are two major classifications of supracondylar fractures that are based upon mechanism of injury. Extension-type fractures represent 95% of all supracondylar fractures; the mechanism of injury is commonly a fall on an outstretched extremity. This mechanism causes the ulna and the triceps to exert an unopposed force on the distal humerus resulting in posterior displacement (lateral or medial) of the fracture.14 Less commonly, a flexion-type supracondylar fracture may result from a direct blow to the posterior aspect of the elbow during flexion with anterolateral displacement of the condylar complex.18,20,21
Evaluation of the Pediatric Patient. Examination of children with elbow fractures may be difficult secondary to pain and anxiety. The physical examination should begin with inspection for any swelling, asymmetry, or misalignment. As these fractures can be associated with significant neurovascular injury, assessment should occur upon arrival to the ED and serially. Children with supracondylar fractures typically present with their arm in a pronated position with a refusal to move the extremity while displaced fractures generally present with significant elbow swelling and localized tenderness with or without obvious deformity. Contrary to the displaced supracondylar fracture, non-displaced fractures may present in a more subtle fashion, with minimal findings except refusal to move the affected arm.12,18,21
Neurovascular Injury. Supra-condylar humerus fractures have a high potential for neurovascular compromise and residual deformity. A thorough exam to assess neurovascular status should include palpation of distal pulses, skin color, temperature, capillary refill, and sensory and motor aspects of the median, ulnar, and radial nerves. Approximately 10%-15% of supracondylar fractures will have an associated neurologic injury. Specifically, the median nerve is most commonly injured followed by the radial and ulnar nerves.18,21 The likelihood of neurovascular injury is directly related to the degree of fracture displacement.18,21,25 Knowledge of anatomy, injury mechanism, and the direction of fracture displacement should be utilized as tools to determine which neurovascular structures may have been injured. The median nerve crosses the elbow with the brachial artery and may be damaged with a posterolateral displacement due to an anteromedial displacement of the proximal fragment.21 Damage to the median nerve results in weakness of flexor muscles of the hand and loss of two-point sensation in the index and middle fingers. Injury to the anterior interosseous nerve, a branch of the median nerve, is the most common nerve injury associated with pediatric supracondylar fractures. A partial injury to this nerve results in a weakness of the flexor pollicis longus or the flexor digitorum profundus to the index finger. This nerve can be examined by asking the patient to make an "okay" sign with their hand. In contrast, the radial nerve is usually damaged with posteriormedial humeral displacement. The patient can be asked to perform a "thumbs up" sign to assess the function of the radial nerve.20,21 The ulnar nerve crosses the elbow posteriorly to the medial epicondyle and is most commonly damaged during a flexion type supracondylar fracture with resultant anterior displacement.14,22
Vascular insufficiency/injury occurs in approximately 10% of children with supracondylar fractures. Vascular examination includes distal evaluation of capillary refill as well as brachial and radial pulses by palpation or ultrasound. The brachial artery is injured in approximately 7%-12% of supracondylar fractures.14 Vascular injury occurs most commonly with posterolateral humeral displacement and is associated with an absent or weak radial pulse. In published studies, authors have concluded that although pulses are an important aspect of the assessment of a child with a supracondylar fracture, it is the absence of brisk capillary refill that best indicates the likelihood of long-term vascular injury.12,14,18,20,21
Supracondylar fractures are at high risk for the development of compartment syndrome, which mandates a timely diagnosis. Patients with suspected compartment syndrome should be assessed for the five "Ps" (pain, pallor, pulselessness, paralysis, and paresthesias).3,12,14 The most reliable sign of compartment syndrome associated with supracondylar fractures is pain with passive range of motion of the distal fingers.18 In addition to the initial assessment, serial exams should be performed, as compartment syndrome of the volar forearm can develop 12-24 hours after the injury. Finally, missed or delayed diagnosis of compartment syndrome may lead to significant complications including muscle necrosis/fibrosis, deformity and loss of function.
Radiographic Findings. Standard radiographs with a suspected supracondylar fracture should include an anteriorposterior view in extension as well as a lateral view in 90°of flexion. Additional oblique radiographs of the elbow should be obtained if there is a high degree of suspicion for a medial or lateral condyle fracture. In addition to the findings of an obvious fracture, it is important to utilize radiographic signs of an occult elbow fracture.9,14,15,18,21,26 Each of these signs will be described in detail below.
Fat Pads. Fat pads are a nonspecific marker for a joint effusion. There are two fat pads that overlie the anterior and posterior aspects of the elbow joint capsule. In the normal child, the anterior fat pad of the elbow lies over the coranoid fossa.14,15,18,25,26 Radiographically, it can be seen as a thin radiolucent line at the anterior border of the distal humerus. However, when the elbow joint capsule becomes distended by effusion secondary to a fracture, the anterior fat pad becomes more displaced anteriorly and superiorly forming a triangle shape that resembles a sail of a ship (sail sign).9,18,25,26 The posterior fat pad normally lies over the more concave, and deeper olecranon fossa. As a result of this difference in location, it should never be visualized on normal radiographs. The presence of a posterior fat pad, regardless of size, (even a thin radiolucent line) on a true lateral view radiograph is pathognomic for an intra-articular fracture of the elbow.9,14,18,25,26 (See Figure 12.)
Figure 12. Fat Pads
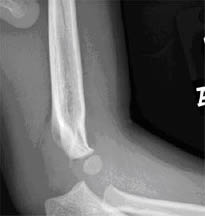
Mild soft tissue swelling as well as anterior and posterior "sail" signs consistent with joint effusion.
Image courtesy of St. Christopher's Hospital for Children Radiology Department, Philadelphia, PA.
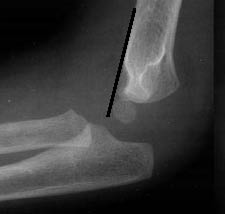
Anterior Humeral Line. The anterior humeral line is drawn along the anterior surface of the distal humerus and should only be utilized with a true lateral radiographic view of the elbow. To identify a true lateral, the medial posterior cortical contour and the lateral posterior cortical contours should be distinctly different. In a child without a fracture, this line should intersect the middle third of the capitellum. Additionally, in young children, the anterior humeral line may pass through the anterior third of the capitellum secondary to the small size of the ossification center.27,28 In the presence of a posteriorly displaced supracondylar fracture, the anterior humeral line will pass through the anterior third of the capitellum, or completely anterior to the capitellum without intersecting the anterior surface. (See Figure 13.) A displaced capitellum secondary to a physis fracture may also result in an abnormal anterior humeral line.25,26
Figure 13. Posteriorly Displaced Supracondylar Fracture
The capitellum is posterior to the anterior humeral line.
Yamamoto L, Inaba A, DiMauro R. Radiology cases in Pediatric Emergency Medicine. Medical Center for Women and Children, Department of Pediatrics, University of Hawaii John A. Burns School of Medicine 1995; Vol. 2, Case 18. Available at www.hawaii.edu/medicine. Used with permission.
Radiocapitellar Line. The radiocapitellar line can be visualized on both the anteriorposterior and lateral radiographic views of the elbow. In a child without injury, this line is drawn along the central axis of the radius, intersecting the middle third of the capitellum in both views. Failure of the radiocapitellar line to transect the capitellum represents radial head dislocation and/or a fracture through the radial neck region.14,18,25 (See Figure 14.)
Figure 14. Abnormal Radiocapitellar Line
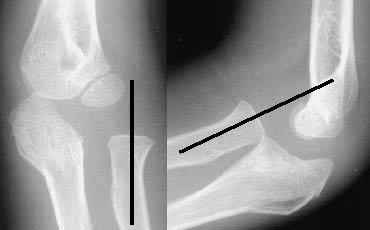
AP and lateral views of the elbow, representing a dislocated radial head.
Yamamoto L, Inaba A, DiMauro R. Radiology cases in Pediatric Emergency Medicine. Medical Center for Women and Children, Department of Pediatrics, University of Hawaii John A. Burns School of Medicine 1995; Vol. 2, Case 18. Available at www.hawaii.edu/medicine. Used with permission.
Figure of Eight. The figure of eight, or hourglass configuration, of the distal humerus should be visualized in a true lateral view of the elbow. Disruption of the figure-of-eight indicates an occult supracondylar fracture.14,15,25 (See Figure 15.)
Figure 15. Figure of Eight
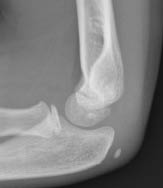
L: Normal figure of eight sign. R: Distorted figure of eight sign, consistent with supracondylar fracture.
Yamamoto L, Inaba A, DiMauro R. Radiology cases in Pediatric Emergency Medicine. Medical Center for Women and Children, Department of Pediatrics, University of Hawaii John A. Burns School
of Medicine 1995; Vol. 2, Case 18. Available at www.hawaii.edu/medicine. Used with permission.
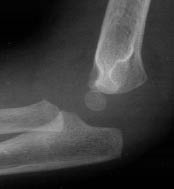
Classification. The Gartland classification system is used for extension-type supracondylar fractures. A type I fracture is non-displaced and will have limited radiographic evidence with a posterior fat pad sign as the only positive finding. Type II fractures are angulated and displaced with the posterior cortex of the humerus intact. The distal fragment maintains a connection to the humerus and appears to be hinged posteriorly to the humeral shaft. (See Figure 16.) Type III fractures have a complete displacement of the distal fragment with loss of connection to the more proximal humerus. (See Figure 17.) In both Type II and III fractures the anterior humeral line will fall anterior and not intersect the capitellum.12,18
Figure 16. Type II Supracondylar Humerus Fracture
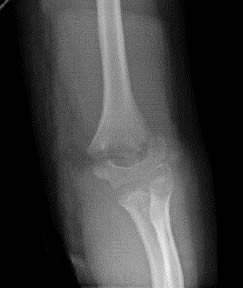
AP/lateral views
Images courtesy of St. Christopher's Hospital for Children Radiology Department, Philadelphia, PA.
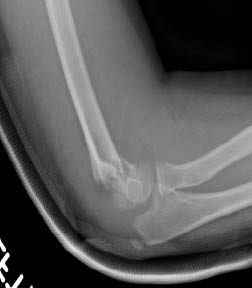
Figure 17. Supracondylar Humerus Fracture
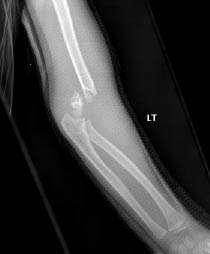
Type III fracture
Image courtesy of St. Christopher's Hospital for Children Radiology Department, Philadelphia, PA.
Management. Immediate ED therapy should include pain management, immobilization, arm elevation, and orthopedic consultation. Management of extension-type fractures is based on the Gartland classification. Type I fractures should be splinted with a posterior long-arm splint with ninety degrees of elbow flexion with forearm in neutral position. These patients may be discharged home if their neurovascular status is intact and adequate follow-up is arranged (in less than one week).14,15,25,29 Type II and III fractures are displaced fractures requiring orthopedic consultation and subsequent reduction to decrease the risk for cosmetic deformity and poor functional outcome.30-32 In regard to management of type II supracondylar fractures, older published literature supported hyperflexion casting after closed reduction as an alternative to operative management. However, in comparison to hyperflexion casting, more recent literature suggests that type II supracondylar fractures without neurovascular compromise, may have more favorable outcomes with closed reduction and delayed percutaneous pinning.20,25,28,30
Complications. Volkmann's ischemic contracture is a complication of undiagnosed or under diagnosed compartment syndrome secondary to supracondylar fracture. This uncommon complication is characterized by fixed elbow flexion, forearm pronation, wrist flexion, and joint extension of the metacarpal-phalangeal joint. Frequent neurovascular monitoring and timely use of fasciotomies, may prevent this complication. Additional long-term complications of supracondylar fractures include cubitus varus or "gunstock" deformity. This occurs when a supracondylar fracture heals with a varus deformity resulting in a cosmetic deformity without loss of function.14,15,18,25
Lateral Condyle Fractures
Lateral condyle fractures are the second most common (10%-20%) elbow fracture. The mechanism of injury and age distribution are similar to that of supracondylar fractures.14,15,18 This fracture type is an oblique fracture of the lateral portion of the joint surface. It occurs as the result of varus or valgus stress secondary to the radial head impacting the capitulum of the humerus during a fall.14,15,24 This fracture may be difficult to diagnose and will frequently have the appearance of a Salter-Harris II fracture. Despite this appearance, the majority of lateral condyle fractures are highly unstable Salter-Harris IV fractures.24
Evaluation. Children with these fractures complain of swelling, localized tenderness, and decreased range of motion of the elbow. When compared to supracondylar fractures, patients with this fracture type have more lateral ecchymosis as a result of tearing of the lateral intermuscular septum.12,14 The physical evaluation should include a thorough neurovascular examination. However, in comparison to supracondylar fractures, the risk of neurovascular compromise is much lower.14,18,20,24
Imaging. As with all elbow radiographs, true anteroposterior and lateral views should be obtained. If the clinical suspicion for lateral condyle fracture is high, oblique views should be considered and may aid in the diagnosis. In displaced fractures, radiographic confirmation is made by an abnormal capitellum-radial head relationship. This abnormality will be visualized by lateral displacement of the condyle and capitellum in reference to the radial head. In addition, the most common radiographic finding is the presence of a posteriorly displaced metaphyseal fragment known as a Thurston-Holland fragment.14,15,18 (See Figure 18.)
Figure 18. Lateral Condyle Fracture
Oblique view of the elbow with a lateral condyle fracture. An associated fracture of the capitellum is also present.
Image courtesy of St. Christopher's Hospital for Children Radiology Department, Philadelphia, PA.
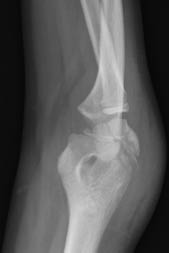
Management / Complications. The ED management of lateral condyle fractures is similar to that of types II and III supracondylar fractures. The majority of these fractures require surgical repair and long-term follow up to prevent complications including nonunion, avascular necrosis, cubitus valgus/varus deformity, ulnar nerve palsy, and physeal arrest.14,15
Forearm Fractures
Introduction. Fractures of the radius and/or ulna represent 10%-45% of pediatric fractures.6,12,14,23 These injuries vary in severity and complexity involving one or both bones of the forearm. Buckle (torus), greenstick, metaphyseal and physeal fractures are the most common types of fractures of the forearm.6,12,14
Forearm fractures are most commonly the result of a fall on an outstretched hand but may occur as a result of direct trauma. The majority of forearm fractures are classified according to location, degree of displacement, and severity of angulation. In general, the treatment for forearm fractures is immobilization and/or closed reduction secondary to the ability of pediatric bone to vigorously remodel.35 Operative management may be required for open fractures, arterial injuries, failed reductions, and patients with skeletal maturity.14,15,23
Evaluation. The examination of children with displaced forearm fractures will include positive findings such as swelling, obvious deformity, and point tenderness.12,14,15 However, a thorough examination should be conducted, as signs and symptoms of fracture may be subtle with a plastic deformity or small buckle fracture. In addition, the exam should include a careful inspection of the skin to rule out an open fracture. Further, it is common for children with minor fractures of the forearm to present to the ED several days after the initial injury with intermittent pain and decreased use of the extremity.
Imaging. A minimum of two radiographic views of the forearm should be obtained, including anteroposterior and lateral views. In addition, elbow and wrist radiographs should be obtained to exclude fractures that have associated joint dislocation.
Nightstick Fracture. This fracture type involves the ulna and usually results from direct trauma to the midshaft. Typically, the trauma occurs as the forearm is held in a protective position during an altercation. This fracture occurs more commonly in the adolescent and adult age group. Treatment involves immobilization in a posterior long-arm splint with 90° of elbow flexion and a neutral hand position.14,15,34
Figure 19. Monteggia Fracture
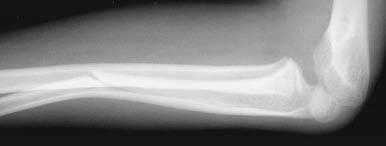
Fracture of the proximal third of ulna with radial head dislocation
Yamamoto L, Inaba A, DiMauro R. Radiology cases in Pediatric Emergency Medicine. Medical Center for Women and Children, Department of Pediatrics, University of Hawaii John A. Burns School of Medicine 1994; Vol. 1, Case 11. Available at www.hawaii.edu/medicine. Used with permission.
Monteggia Fracture. A Monteggia fracture was first described as the combination of a proximal ulnar fracture with anterior dislocation of the radial head. (See Figure 19.) Currently, the Monteggia fracture-dislocation includes several different types of ulnar fractures with radial head dislocation. The classic form of a Monteggia injury is uncommon in children, comprising 2% of all pediatric elbow fractures. Children that have sustained this fracture present with limited mobility of the arm, pain with movement, point tenderness, and significant swelling. This is an important fracture type secondary to the complications that may arise if the diagnosis of the concomitant radial head dislocation is missed. It further emphasizes not only the need for radiographs that image the joint above and below the site of injury, but also the need for clinicians to search for multiple injuries. Complications that may arise with failure to diagnose this fracture type include nerve palsies (radial/median nerves) as well as long-term deformity and loss of function. Specifically, physical findings associated with nerve injury secondary to a Monteggia fracture include weakness and inability to extend the fingers and thumb (injury of the posterior interosseous nerve, a branch of the radial nerve). These fractures require orthopedic consultation for closed reduction and immobilization. However, if closed reduction is not successful, operative intervention is required.14,15,34
Wrist / Distal Forearm Fractures
Introduction. The majority (up to 84%) of radius and ulna fractures involve the wrist and distal forearm. The fracture mechanism is typically a fall on an outstretched hand with subsequent displacement the result of wrist position during the injury. Specifically, a fall with a dorsiflexed wrist will result in a dorsal angulation or displacement. Conversely, a fall with a volar flexed wrist will result in volar angulation or displacement.14,15, 34 Important to mention is that injury to the carpal bones is uncommon in the pediatric population, due to the immaturity of these bones. Common mechanisms that cause bony wrist injuries in adults, result in fractures of the forearm in children.25
Evaluation. Children will complain of swelling, and localized tenderness that is worsened with movement. In addition, patients may have significant deformity, which is dependent upon the degree of fracture angulation. Patients with suspected forearm fractures should undergo a thorough neurovascular and skin exam.
Treatment. Physeal fractures of the distal forearm are classified by the Salter-Harris system. Treatment for physeal fractures was mentioned previously, as well as treatment for buckle (torus) fractures. Greenstick fractures are usually managed with closed reduction and long-arm or sugar-tong casting if the angulation is less than 15°. Parents should be cautioned of the increased risk of re-injury with these fractures.14,15,34
Galeazzi Fractures. A Galeazzi fracture is a fracture of the distal radius with associated disruption of the radioulnar joint. These fractures are rare in children and immediate orthopedic consultation is required for a closed reduction.14,15,34 (See Figure 20.)
Figure 20. Galeazzi Fracture
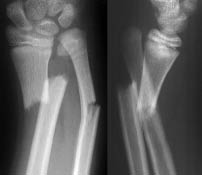
Distal third radius fracture with distal ulnar dislocation.
Yamamoto L, Inaba A, DiMauro R. Radiology cases in Pediatric Emergency Medicine. Medical Center for Women and Children, Department of Pediatrics, University of Hawaii John A. Burns School of Medicine 1994; Vol. 1, Case 16. Available at www.hawaii.edu/medicine. Used with permission.
Colles Fracture. A Colles fracture is a transverse fracture that occurs proximal to the distal radial physis with dorsal displacement of the distal segment and volar angulation.14,15 (See Figure 21.) This fracture is also known as a dinner fork deformity due to the subsequent appearance of the forearm. A neurovascular exam should be done to exclude median nerve injury. In children that are skeletally immature, a 40° displacement is well tolerated because of the ability of pediatric bone to remodel. However, if there is significant rotational deformity, a closed reduction may be needed. Orthopedic consultation may help direct definitive care for angulated fractures.
Figure 21. Colles Fracture
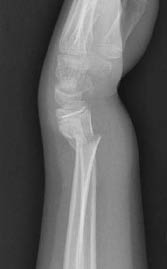
When reduction is required, the distal radius should be restored toward the normal volar tilt.14,25 Immobilization is successful in a sugar tong splint with slight volar angulation at the wrist.14,15,25,34
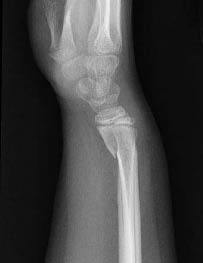
Smith Fracture. A Smith fracture is the reverse of a Colles fracture, with volar displacement and dorsal angulation. (See Figure 22.) This fracture type occurs less commonly than the Colles fracture but has a similar risk of injury to the median nerve. Further, this fracture has a tendency to be less stable, and generally only 10° of angulation is tolerated prior to the need for closed reduction and/or operative repair. For all angulated fractures, consider orthopedic consultation for definitive management.
Figure 22. Smith Fracture
Conclusion
Part I of this two part series on common orthopedic injuries in the pediatric ED focused on upper extremity injuries, their unique pediatric presentations, diagnostic evaluation and treatment options to optimize outcomes. Part II will focus on common injuries in the lower extremities.
References
- Mathison JD, Agrawal D. General principles of fracture management: Fracture patterns and description in children. www.uptodate.com/home/index.html. Accessed June 14, 2010.
- Goulding A. Risk factors for fractures in normally active children and adolescents. Med Sport Sci 2007;51:102-120.
- Della-Giustina K, Della-Giustiina DA. Emergency department evaluation and treatment of pediatric orthopedic injuries. Emerg Med Clin North Am 1999;17:895-922.
- Hart ES, Albright MB, Rebello GN, et al. Broken bones: Common pediatric fractures-Part I. Orthop Nurs 2006;25:251-255.
- Davenport M, Nesbit C. An evidence-based approach to pediatric orthopedic emergencies. Pediatr Emerg Med Pract 2009;6:1-16.
- Gholve, PA. Common Fractures. In: Kielgman RM, et al, eds. Nelsons Textbook of Pediatrics, 18th ed. Philadelphia: Saunders; 2007:682.
- England SP, Sundberg S. Management of common pediatric fractures. Pediatr Clin N Am 1996;43:991-1012.
- Park HW, Yang IH, Joo SY, et al. Refractures of the upper extremity in children. Yonesei Med J 2007;48:255.
- Frick SL. Skeletal Growth, Development, and Healing as Related to Pediatric Trauma. In: Green & Swiontkowski: Skeletal Trauma in Children. 4th ed. Elsevier 2008;1:1-18.
- Shannon EG, Hart ES, Grottkau BE. Clavicle fractures in children: The essentials. Orthop Nurs 2009;28:210-214.
- Pecci M, Kreher JB. Clavicle fractures. Am Fam Phys 2008;77:65-69.
- Hart ES, Grottkau BE, Rebello GN. Broken bones: Common pediatric upper extremity fractures-Part II. Orthop Nurs 2006;25:311-324.
- Soto F, Fiesseler F, Morales J, et al. Presentation, evaluation, and treatment of clavicle fractures in preschool children presenting to an emergency department. Pediatr Emerg Care 2009;
25:744-747. - Carson S, Woolridge DP, Colletti J, et al. Pediatric upper extremity injuries. Pediatr Clin N Am 2006;53:41-67.
- Benjamin HJ, Hang BT. Common acute upper extremity injuries in sports. Clin Ped Emerg Med 2007;8:15-30.
- Wiesel BB, Getz CL. Current concepts in clavicle fractures, malunions and non-unions. Curr Opin Orthop 2006;17:
325-330. - Hill JM, McGuire MH, Crosby LA. Closed treatment of displaced middle-third fractures of the clavicle gives poor results. J Bone Joint Surg Br 1997;7:
537-539. - Shrader MW. Pediatric supracondylar fractures and pediatric physeal elbow fractures. Orthop Clin N Am 2008;39:163-171.
- Smith JR, Kozin S. Identifying and managing physeal injuries in the upper extremity. JAAPA 2009;22:39-45.
- Green NE. Fractures and dislocations about the elbow. In: Green NE, Swiontkowski ME, eds. Skeletal Trauma in Children. 4th ed. Philadelphia: Elsevier; 2008:207-282.
- Baratz M, Micucci C, Sangimino M. Pediatric supracondylar humerus fractures. J Hand Clinic 2006;22:69-75.
- Brubacher JW, Dodds SD. Pediatric supracondylar fractures of the distal humerus. Cur Rev Musculosket Med 2008;1:190-196.
- Skaggs D. Pershad J. Pediatric elbow trauma. Pediatr Emerg Care 1997;13:425-434.
- Spiegel PG et al. Fractures. In: Skinner: Current Diagnosis and Treatment in Orthopedics. 4th ed. Columbus, OH: McGraw-Hill Companies; 2008:11;
635-643. - Menckhoff C, Welter C, Sessums C. Pediatric wrist and elbow injuries: Mechanisms of injury, findings, and treatment. Pediatr Emerg Med Reports 2008;8:93-108.
- Emery KH. Imaging of sports injuries of the upper extremity in children. Clin Sports Med 2006;25:53-568.
- Skaggs DL, Mirzayan R. The posterior fat pad sign in association with occult fracture of the elbow in children. J Bone Joint Surg Am 1999;81:1429-1433.
- Wu J, Perron AD, et al. Orthopedic pitfalls in the ED: Pediatric supracondylar humerus fractures. Am J Emerg Med 2002;20:544-550.
- Carmichael KD, Joyner K. Quality of reduction versus timing of surgical intervention for pediatric supracondylar humerus fractures. Orthopedics 2006;29:628-632.
- Farley FA, Patel P, Craig CL. Pediatric supracondylar humerus fractures: Treatment by type of orthopedic surgeon. J Child Orthop 2008;2:91-95.
- Valiati R, Ibrahim D, Abreu MER. The treatment of condylar fractures: to open or not to open? A critical review of this controversy. Int J Med Sci 2008;5:
313-318. - Kamath AF, Baldwin K, Horneff J. Operative versus non-operative management of pediatric medical epidcondyle fractures: A systematic review. J Child Orthop 2009;3:345-357.
- Keppler P, Salem K, Schwarting B. The effectiveness of physiotherapy after operative treatment of supracondylar humeral fractures in children. J Pediat Orthop 2005;25:314-316.
- Dolan M. Fractures and Dislocations of the Forearm, Wrist, and Hand. In: Green & Swiontkowski: Skeletal Trauma in Children. 4th ed. Elsevier 2008;8:159-205.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
