Strangulation Injuries
Strangulation Injuries
Author:
J. Stephan Stapczynski, MD, FACEP, Chair, Department of Emergency Medicine, Maricopa Medical Center, Phoenix, AZ.
Peer Reviewer:
Ann M. Dietrich, MD, FAAP, FACEP, Professor of Pediatrics, The Ohio State University College of Medicine, Public Health Risk Manager, Section of Emergency Medicine, Columbus, OH.
Case Scenarios
Near Hanging From Jail. You are on duty in the ED when the paramedics bring in a patient from the county jail who had tried to hang himself. When the patient arrives, you are told by the accompanying guard that the patient was found with a tightly twisted bedsheet around his neck and looped over the bedpost of the metal bunkbed. The patient's feet were on the floor, but his buttocks were suspended off the floor. The patient was described as unconsciousness, cyanotic, and not breathing. When taken out of the bedsheet and laid on the ground, he started breathing spontaneously but remained unconscious. To your examination, he does not respond to pain, and you see marks on his neck as shown in Figure 1.
Figure 1: Suicidal Incomplete Hanging
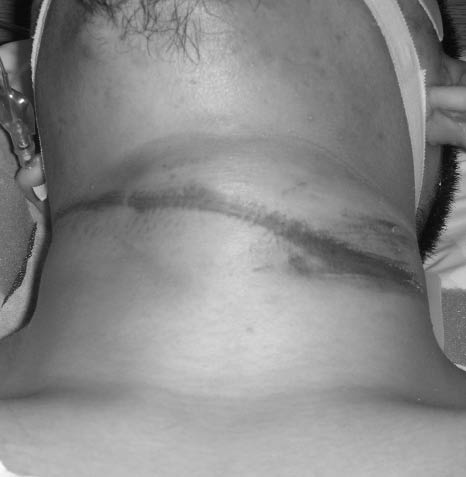
Linear ecchymoses across the neck
DV with Manual Strangulation. The triage nurse comes to you about a patient she is evaluating. The patient was brought in by police because of a domestic violence assault. The patient was choked by her boyfriend and passed out. The patient now says her voice is hoarse and she has pain with swallowing.
Adolescent Choking Game. A 13-year-old boy arrives via EMS in cardiopulmonary arrest. When you ask the paramedics for the history, you are told that the child was found in his bedroom, slumped in a corner with a belt around his neck. He was last seen about an hour prior to that when he went upstairs to his room to do homework.
Introduction
What do these three patients have in common? All three had pressure applied to their necks that resulted in a loss of consciousness. What caused the loss of consciousness, and how should these different cases be assessed in the emergency department?
Strangulation is a well-recognized event in forensic science with many studies in the literature devoted to that field.1-5 It has been estimated that strangulation accounts for 2.5% of traumatic deaths worldwide6 and up to 10% of violent deaths in the United States.7 In general, much of the forensic analysis on strangulation injuries was done on homicide victims and emphasized that serious damage to the vital structures in the neck was common. Comparatively, strangulation as a specific injury did not receive as much attention in the clinical literature until the 1980s with the publication of two review articles.8,9 Only a limited number of publications have specifically focused on patients who survive to emergency department arrival.10,11 As a result, textbook chapters and clinical teaching tend to over-stress those rare but serious injuries and provide little guidance on how to evaluate the majority of patients who present to the emergency department. Many of the initial studies included a majority of victims with hanging as the strangulation mechanism. As discussed below, there are important differences between manual strangulation and hanging, so the results of analysis from hanging victims cannot be consistently applied to victims of manual strangulation.
Definition and Differentiation
The common feature in all three cases is that the functioning cells of the body particularly the brain were deprived of oxygen for a period of time; this is the definition of asphyxia.12 The textbook chapters and medical journal literature concerning asphyxia can be confusing because of the different terms used to describe the specific mechanisms. To provide some clarity to this confusion, an article from the forensic literature this year proposes that asphyxia can be divided into four main categories: suffocation, strangulation, mechanical asphyxia, and drowning.12 (See Table 1.)
Table 1: Classification of Asphyxiation
Suffocation
- Smothering
- Choking
- Confined space entrapment
Strangulation
- Manual
- Ligature
- Hanging
Mechanical
- Positional
- Compressive or traumatic
Drowning
- Death due to immersion in liquid
Suffocation describes the process that impedes or halts respiration. Suffocation subdivides into smothering, choking, and confined spaces/entrapment/vitiated atmosphere. Smothering occurs when there is mechanical obstruction of the flow of air from the environment into the mouth and/or nostrils. Smothering typically requires the use of a soft, flexible object, like a cloth or a pillow that can be molded over the irregular contours of the face, occluding the nostrils and mouth. Choking describes the process whereby the trachea is occluded, either partially or completely, by a foreign body. Most cases of choking are accidental, with only rare cases being intentional suicide.13 Confined space entrapment occurs when there is inadequate oxygen in the enclosed space due to consumption or displacement by other gases.
Strangulation describes the process whereby an external force is applied to the neck that results in a depressed or completed loss of consciousness. The external force can be the use of the bare hands (manual), ligature (a cord-like object), and gravity (near-hanging). The term "garrote" or "garroting" is occasionally used to describe ligature strangulation, but to be precise, the garrote was a specific form of judicial execution formerly used in Spain whereby the ligature was slowly tightened by the twisting of a rod inserted through the loop of the ligature. Accidental strangulation from cords and clothing have been described with Venetian blind cords14, playground slide tie rope15, cotton cloth16, and scarfs (termed the "Isadora Duncan syndrome" after the circumstances surrounding her accidental death).17
In hanging, the external pressure applied to the neck is supplied by the patient's body weight. With incomplete or near-hanging, a portion of the patient's body remains in contact with the undersurface or floor, whereas in complete hanging, the victim is fully suspended.9 In judicial hanging, there is a gravitational free fall or drop before the rope is abruptly tightened, applying pressure to the neck. In most self-inflicted hangings, there is not usually a drop and the pressure applied to the neck is more gradual, as many suicidal hangings are incomplete. Also, with suicidal complete hangings, there is a higher incidence of thyroid cartilage and hyoid bone fractures as compared to incomplete hangings.18
An estimation of the force applied to the neck during the strangulation episode is generally not possible or probably useful.2 In general, the forces applied by manual strangulation are less than those provided by hanging. Accidental strangulation that involves a ligature being caught in running machinery or from a moving vehicle can apply sudden and violent force to the neck; such victims can sustain serious injury and often are dead at the scene.
Mechanical asphyxia encompasses positional, compressive, and traumatic asphyxia. Positional or postural asphyxia usually occurs in infants or small children, when the child's neck is caught in crib or fence slats. In traumatic or compressive asphyxia, there is mechanical limitation of the expansion of the lungs by external forces. An example includes victims crushed by a crowd, as might occur when a large group tries to exit a crowded room through a small door, crushing those in front against the building structure or underneath the weight of those behind them.
Drowning is death due to immersion in liquid. It is generally agreed that asphyxia plays an important pathophysiological role, but it is likely that other neurologic and cardiovascular reflexes also play a part in the fatal outcome. Thus, drowning is a more complex event than simple asphyxia.
Pathophysiology
When pressure is placed on the neck, the victim first experiences pain, followed by anxiety as the victim becomes distressed from a subjective sensation of difficulty breathing. With enough force to impair respiration, the victim will typically lose consciousness within 10-15 seconds.19 Obviously, the loss of consciousness is not solely due to apnea. It is likely that arterial obstruction, venous obstruction, and autonomic nervous system reflexes all play a role in the rapid loss of consciousness with strangulation.
The neck is vulnerable to external injury because it does not have bony protection and within its relatively small diameter course the airway, vascular supply to the brain, the spinal cord and other vital nerves, and the cervical vertebral column. External force can injure many of these important structures.
The airway is anchored at its superior end by the thyroid cartilage and the hyoid bone. Fractures of both structures occur from manual strangulation, ligature strangulation, and hanging suicides.20,21 Older individuals may have an ankylosed hyoid bone or an ossified thyroid cartilage, which renders them more brittle and susceptible to fracture from strangulation. Laboratory studies on fresh human larynges indicate that the thyroid and cricoid cartilage can be broken with static loads of 16 and 21 kg, respectively.22 With fractures, hemorrhage and edema can develop to affect the airway. Transient occlusion of the upper airway at the level of the thyro-hyoid membrane is estimated to occur with a 10-kg force.23 But even without fracture, contusion to the larynx can result in hemorrhage and edema with similar consequences. However, as opposed to victims who are dead at the scene, fractures of the thyroid cartilage or hyoid bone are uncommon in victims of accidental strangulation who arrive to the emergency department with signs of life and are even rarer in survivors of manual strangulation or hanging. Fortunately, direct injury to the trachea is rare with strangulation.24
The carotid arteries, because of their relatively superficial position in the neck, can be affected by external pressure. With an anterior force, the carotid artery can be compressed against the transverse process of the fourth to sixth cervical vertebrae. Flow through the artery can be impaired by either mechanical obstruction or the induction of spasm, which narrows the vascular lumen. The force required to obstruct flow through the carotid arteries and produce loss of consciousness is estimated to be equal to a static load between 2.5 and 10 kg, depending on the direction of force.23 Forces applied to the vessel wall may cause hemorrhage within the media or intimal disruption. Such traction injuries have been reported in up to 5% of suicidal hangings25, but such injury is uncommon after non-lethal hanging and strangulation. The intimal damage may induce thrombosis, which typically produces symptoms and signs over the subsequent 12-24 hours.19,26-28 Obstruction in one internal carotid artery can produce dense contralateral hemiparesis, whereas bilateral occlusion can produce loss of consciousness. In addition, the traumatic thrombosis in the internal carotid artery can break off and embolize to the distal cerebrovascular circulation. As thus described, the major morbidity from intimal injury to the neck from strangulation or hanging is from thromboembolism, and the standard treatment is with anticoagulation, generally with heparin.29 Fibrinolytics, either systemic or local catheter directed, have been used to treat non-traumatic carotid thrombosis30 and have been suggested for use in traumatic causes.19
The vertebral arteries are well protected from external forces as they course though the transverse foramen of the cervical vertebrae. To compress the vertebral arteries, a horizontal encircling force equal to a 30- to 40-kg load is required.23 However, with extreme rotation or flexion, flow through there arteries can also be compromised and less external force is required to occlude flow.
The low-pressure jugular venous system is superficial in the anterior neck, and flow through these veins is easily affected by external pressure. Occlusion of venous outflow from the brain produces stagnant hypoxia and impairment in consciousness. The force required to obstruct flow though the internal jugular vein is estimated to be equal to a 2 kg static load.23 For manual strangulation and suicidal near-hanging victims, venous obstruction is a significant factor that produces loss of consciousness.
Pressure on the carotid sinus sympathetic ganglion (carotid body) in the neck is well known to produce bradycardia and cardiac arrest by the so-named "carotid sinus reflex." The role this reflex plays in the pathophysiology of strangulation is believed to be uncommon, as force must be applied to a specific and localized area,2 and while bradycardia can occur within seconds, the force must be maintained for a minimum of 3-4 minutes to induce cardiac arrest.27 The role such reflex plays in cardiac arrest and death after strangulation and near-hanging is disputed. It is suggested that older individuals with atherosclerosis and carotid artery disease are more susceptible to this reflex, and this may contribute to the occurrence of cardiac arrest after strangulation and near-hanging in the elderly.9
Spinal fractures are rare in most strangulation victims, either manual or incomplete-hanging. Analysis of judicial hangings indicates that a free-fall drop of at least the victim's height is required to produce cervical vertebral fractures. In these cases, the most common injury is distraction of the upper cervical vertebrae, usually the second from the third, and occasionally the third from the fourth.31
Pulmonary edema is a common complication seen in comatose victims who survive to hospitalization. The cause of the pulmonary edema can either be due to anoxic injury to the central nervous system (neurogenic pulmonary edema) or from the large negative intrathoracic pressures seen when the victim struggles to breathe in against an occluded airway (obstructive pulmonary edema). With airway obstruction and aggressive attempts at inspiration, the intrapleural pressure can fall to as low as -100 cm H2O, compared to a range of -2 to -5 cm H2O seen with quiet respiration. The excessive negative intrathoracic pressure increases venous return and pulmonary blood volume while also lowering interstitial pressure. This results in an increased hydrostatic gradient with movement of fluid from the pulmonary capillaries into the tissues. The incidence of obstructive pulmonary edema is about 10% in adults who require active airway intervention for acute airway obstruction.32 Because neurogenic pulmonary edema is almost always seen with severe if not lethal brain injury, the presence of pulmonary edema in a strangulation or hanging victim who is experiencing a good neurological recovery is likely due to obstruction as opposed to neurologic injury.
Clinical Presentations
The clinical presentations can vary according to the method of strangulation. Common features upon emergency department presentation include evidence of pressure against the skin (hyperemia and/or ecchymosis), increased venous pressure in the face (facial or conjunctival petechiae), change in laryngeal function (voice change or difficulty breathing), and evidence of cerebral hypoxia (a report of loss of consciousness).6,10,11,33 One study from the United Kingdom found that victims of non-fatal suicide attempts via hanging have a significantly higher suicidal intent scale score and a lower use of alcohol as part of the self-harm act when compared to self-poisoning controls.34 Hanging victims are more likely to arrive in the emergency department with a depressed level of consciousness than are victims of manual strangulation. This is presumably due to the more intensive and prolonged compressive force applied to the neck due to hanging than is typically seen with manual pressure. Facial and conjunctival petechiae are common and are evidence of prolonged elevated venous pressure from the strangulation. It has been estimated that the jugular vein needs to be occluded for at least 15-30 seconds for the development of facial petechiae.
The majority of strangulation victims present with these local signs of cervical injury and/or evidence of cerebral hypoxia. Injury to other organ systems from strangulation is uncommon and primarily described in isolated case reports. As previously noted, pulmonary edema has been reported following strangulation, usually from hanging. Case reports of diaphragmatic injury35, multiple organ failure36, and thyroid storm37 after strangulation have appeared in the medical literature.
Clinical Associations with Strangulation
Three events often involve strangulation as part of that activity: domestic or intimate partner violence, the "choking" game, and auto-erotic asphyxiation.
Strangulation is well described with domestic or intimate partner violence episodes.38,39 The occurrence of strangulation has been reported in 47-68% of women who were being assessed for intimate partner violence.38,40 The occurrence of strangulation was identified as an independent risk factor for subsequent intimate partner attempted or completed homicide in women; women who reported strangulation as part of a domestic violence episode had a six to seven times greater likelihood of attempted or completed homicide during a seven-year follow-up compared to abused controls.41 Smothering or strangulation has been identified in 25% of women killed by an intimate partner.42
Studies of women who were strangled by their intimate partners have found several important issues for emergency physicians. The patient, when initially evaluated by emergency department personnel, may not always report the strangulation episode. As is common with cases of domestic violence, the victim may be hesitant to fully describe what happened or will minimize the severity of the attack. Specific questions often are required to elucidate the strangulation mechanism. Visual evidence of force applied to the neck during intimate partner violence strangulation is often absent on initial police and medical evaluation.10,43 The lack of physical findings may lead authorities to discount the patient's report.43 In addition, the laws concerning strangulation as a specific assaultive mechanism vary by state and, consequently, strangulation may not be considered as serious as a punch.44
The "choking game" is an activity that has been most commonly described among adolescents, but may be played by children as young as 6.44-47 The purpose of this activity is to induce a euphoric state or "high" by temporarily strangling the neck, reducing cerebral blood flow, and creating cerebral hypoxia. Once the initial lightheaded sensation is felt, the stranglehold is released, allowing return of blood flow, often with a second "rush." Various ligatures, such as rope, bed sheets, belts, shoelaces, cloth towels, or dog collars, are reported.44-48 In addition, manual strangulation with the individual's own hands or the hand of another can be used. If the victim engages in this activity while alone, loss of consciousness followed by death may occur before the stranglehold can be released.49 As compared to drug use among adolescents for the purposes of getting "high," analysis of victims of this asphyxial game are more likely to be athletic, have good academic standing, and believe the choking game is a safe alternative to drug use for the purposes of achieving a euphoric high.
As street drugs of abuse can possess many different slang names, the choking game is also known by other terms; names such as Suffocation, Roulette, Rising Sun, California High, Flatliner, Space Cowboy, Passout, Tingling, Funky Chicken, American Dream, Space Monkey, Blackout, and Gasp have been reported by clinical, forensic, and legal authorities. The following clinical features are described as useful in detecting children and adolescents who engage in this activity: a combination of these findings vascular injection or petechiae of the conjunctiva, marks on the neck, a report of loss of consciousness or altered mental status, or severe headache especially if they occur after the child has spent time alone. Emergency physicians are encouraged to have an awareness of this game and to have a low threshold for inquiry regarding its possibility. It also is important to stress when talking to children and parents that this activity be identified and discussed as "strangulation activity" that can produce coma and death, as opposed to the less dangerous sounding phrase "playing the choking game."50 Identification of a child who engages in this activity may not only prevent future episodes or death in that individual, but may prevent the patient from engaging in this activity with others.47,51
Auto-erotic asphyxiation is the use of strangulation by either ligature or hanging to enhance sexual activity.9 The individual is usually alone and uses a device or prop for sexual stimulation. The intent is that the induced cerebral hypoxia will make the sexual pleasure more intense and the stranglehold will be released before permanent cerebral injury. Children have been reported to engage in auto-erotic asphyxiation activity.52 If the individual dies, it is termed an auto-erotic death. Auto-erotic deaths are more common in males than females and, while rare in children, have been reported in individuals as young as 9.53 The correct identification of an auto-erotic asphyxiation death from other causes (accidental, homicidal, or suicidal) is dependent on proper scene investigation.
Physical Assessment
Like other traumatic injuries, the assessment of a strangulation victim starts with the ABCs airway, breathing, circulation. While cervical vertebra bony and ligamentous injury is rare in strangulation victims arriving to the emergency department, cervical spine stabilization initially should be done and maintained until such injury is appropriately excluded.9,25 It is uncommon that airway injuries from strangulation or near-hanging inhibit or interfere with needed standard endotracheal intubation in the emergency department.25,54 Conversely, care reports of accidental strangulation where the ligature was caught in moving machinery and severe, sudden force was applied to the neck have documented distortion of the laryngeal structures resulting in difficulty with intubation.17 Although unproven in cases of hanging and strangulation, it is often recommended that comatose patients who are hemodynamically stable be treated with intravenous opioids (fentanyl) and lidocaine prior to laryngoscopy to blunt the cardiovascular (hypertension and tachycardia) and cerebral (increased intracranial pressure) responses to intubation.
Therapeutic hypothermia has become an accepted modality for improving neurologic outcome in victims of out-of-hospital cardiac arrest who are successfully resuscitated but do not quickly regain consciousness.55,56 It would be anticipated that therapeutic hypothermia would also be beneficial in hanging and strangulation victims who have sustained anoxic brain injury and do not quickly recover consciousness. While there are no randomized trials in near-hanging victims57, based on theoretical considerations and limited clinical experience, it seems reasonable to consider therapeutic hypothermia in all comatose victims of near-hanging.58,59
With strangulation, the initial presenting symptoms and physical signs may be deceptively minimal. It takes time for hemorrhage and edema to develop after compressive injuries, and the full clinical manifestations may not occur for 36 hours after the event.
The following specific clinical manifestations are possible in strangulation victims:
Voice changes are reported in up to 50% of manual strangulation victims and may range from a raspy or hoarse voice to complete inability to talk.10
Swallowing abnormality is not a common symptom on initial emergency department assessment, but is reported during the subsequent two weeks in 44% of women who survive a domestic violence strangulation episode.10 Swallowing may be painful (odynophagia) or difficult (dysphagia).
Breathing difficulties are common, seen in up to 85% of women during the initial two weeks after a strangulation event.10 The dyspnea can be psychogenic in origin and may be due to anxiety, fear, depression, or hyperventilation. Difficulty breathing can also be due to laryngeal edema or hemorrhage, although those injuries are less common in surviving victims.
Pain in the throat or neck is common after strangulation. The patient may be able to localize it to a specific area of injury, or it may be diffuse and poorly localized.
Mental status changes can be due to the occurrence of cerebral hypoxia or from concomitant intracranial injury or ingestion of drugs or ethanol.
Neurologic symptoms are frequently reported in victims of strangulation and include changes in vision, tinnitus, eyelid droop, facial droop, or unilateral weakness. While common, many of these reported symptoms may not be detectable or confirmed by neurologic testing.
Injury to the soft tissues in the neck may manifest with edema, hyperemia, ecchymoses, abrasions, or scratches. Abrasions and scratches may be defensive in nature, as the victim has tried to remove the assailant's from his or her neck.60 The hyperemia may be transient and not visible by the time of assessment. Ecchymoses and swelling may take time to develop and may not be visible on initial assessment. Ligature marks can be hidden within the natural skin folds of the neck and potentially missed on cursory examination, especially if the cervical collar is not removed and good lighting is not used. Chin abrasions have been reported to occur from the defensive actions of the victims as they flex their cervical spines forward and bring their chins down in an effort to protect their necks from the manual strangulation of the assailant.
Petechiae can occur at or above the area of compression and are most frequently reported on the face and conjunctiva.61,62 More extensive cutaneous and mucosal bleeding, such as a subconjunctival hemorrhage, is generally seen only after a particularly vigorous struggle between the victim and the assailant.
Laryngeal injuries can manifest with focal tenderness of the laryngeal cartilage or subcutaneous emphysema over or around the laryngeal cartilage.
Pulmonary findings can be due to aspiration pneumonitis if the victim vomits and then inhales during the strangulation event. As noted above, pulmonary edema can occur, but this is generally only seen in hanging victims who remain comatose after emergency department arrival.
Neurologic findings can include ptosis, facial droop, and unilateral weakness. In many patients, the findings are transient and believed to be incited by focal cerebral ischemia produced by the strangulation process that resolves with time. In rare cases, damage to the internal carotid artery may induce thrombosis with a delayed neurologic presentation.19,26,27
A structured checklist can guide the assessment and documentation.7 (See Table 2.) Regardless of the phrase or term used by the patient, it is recommended that medical personnel use the term "strangle" or "strangulation" to describe and document the event.
Table 2: Structured Assessment and Documentation for Strangulation Victims
Method or Manner
- Hands (manual strangulation)
- Elbow and forearm (sleeper or "choke hold")
- Knee
- Ligature
- Other
Number of Episodes
- Single
- Multiple
- Repeated with different methods
Other Circumstances
- Was the victim also smothered?
- Was the victim also shaken?
- Was the victim knocked or pounded into a wall or the ground?
- Was the victim also hit or physically assaulted?
- Was the victim also sexually assaulted?
Symptoms
- Did the victim lose consciousness?
- Neck pain
- Neck swelling
- Difficulty breathing
- Voice changes: hoarse, raspy, unable to speak
- Sore throat
- Difficulty swallowing
- Pain with swallowing
- Headache
- Other symptoms: urinary and/or fecal incontinence
Signs
- Redness or ecchymoses on the neck
- Neck swelling
- Neck tenderness
- Laryngeal and subcutaneous crepitus
- Facial or conjunctival petechiae
- Ptosis, facial droop, unilateral weakness
Imaging and Laryngoscopy
The imaging modalities used to assess for internal injuries after strangulation include plain radiographic, computed tomography (CT), computed tomographic angiography (CTA), magnetic resonance imaging (MRI), Doppler ultrasound of the carotid arteries, and fiberoptic visualization of the laryngeal structures (fiberoptic laryngoscopy). Each of these modalities has utility for detecting specific injuries. (See Table 3.)
Table 3: Imaging Modalities Useful in Strangulation Injuries
|
Modality |
Advantages |
Disadvantages |
|
Plain radiography (bone technique) |
Readily available in the ED Visualization of cervical vertebral fractures |
Cervical vertebral fractures rare in strangulation injuries |
|
Plain radiography (soft-tissue technique) |
Readily available in the ED Visualization of laryngeal injuries (subcutaneous emphysema, tracheal deviation from edema and hemorrhage) Visualization of hyoid bone fractures |
Low sensitivity for detecting these uncommon secondary signs of deep soft-tissue or laryngeal injuries in survivors |
|
Computed tomography (CT) |
Routinely available in most U.S. EDs Higher sensitivity for soft-tissue injuries |
Intravenous contrast needed for highest sensitivity |
|
Computed tomographic angiography (CTA) |
Routinely available in most U.S. EDs Visualization of carotid artery injury and thrombosis |
Need for intravenous contrast |
|
Magnetic resonance imaging (MRI) |
Highest sensitivity for deep soft-tissue injury |
Less availability in U.S. EDs |
|
Doppler ultrasound |
Visualization of intimal injury to carotid arteries and/or intraluminal thrombosis Can be brought to the bedside of unstable patients |
Less availability in U.S. EDs Lower resolution and presumably less sensitive for carotid artery injury and intraluminal thrombosis |
|
Fiberoptic laryngoscopy |
Visualization of vocal cords and adjacent structures |
Not readily available in the emergency department |
Plain radiography, with either bone or soft-tissue technique, is readily available in the emergency department. Fractures of the cervical vertebrae are extremely rare in strangulation injuries unless there has been a hanging with a free-fall drop of the body, so routine plain radiographs of the cervical spine are generally of low yield. Significant injuries to the laryngeal structures may produce secondary signs visible on cervical radiographs using soft-tissue technique subcutaneous emphysema, tracheal deviation from edema or hemorrhage, and associated hyoid fractures. This technique is insensitive for more subtle injuries and, given the availability of computed tomography, soft-tissue cervical spine radiographs have little routine use.
Computed tomography (CT) is more sensitive for bony injuries, subcutaneous emphysema, soft-tissue edema, and internal hemorrhage. (See Figure 2.) Importantly, CT is widely available in emergency departments. For optimal visualization of these soft-tissue injuries, intravenous contrast is recommended.
Figure 2: Suicidal Incomplete Hanging
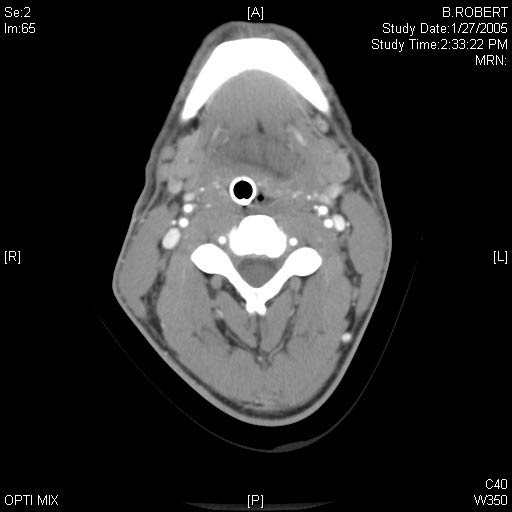
CT scan shows significant pharyngeal edema, most marked in the palatine fossa.
Computed tomography angiography (CTA) is useful to detect injury to the carotid arteries.19 As noted above, the initial injury is usually an intimal tear that then promotes local thrombosis. The clot can obstruct the carotid artery lumen and/or break off pieces that embolize the distal cerebrovascular circulation. The current "gold standard" for blunt carotid injury is four-vessel selective cervical angiography.29 The ability of CTA to detect (sensitivity) and exclude (specificity) injury to the internal carotid artery from blunt trauma has been the subject of several articles in the medical literature, with reported sensitivities as low as 47%.63 With improved CT imaging techniques and enhanced recognition, the more recent studies have found that the sensitivity of CTA for blunt carotid injury varies from 82% (when compared to selective angiography)64 to 100% (when compared to clinical outcome).65 These differences suggest that some blunt injuries to the internal carotid artery may not produce clinical consequences, and detection of these asymptomatic events is perhaps without benefit. Because blunt carotid injury is uncommon after strangulation, there is not enough experience to present an evidence-based approach for the use of CTA. The author of this article recommends that four-vessel cranial-cervical CTA be done for patients who remain unconsciousness after emergency department arrival or exhibit unilateral neurologic signs.
Magnetic resonance imaging (MRI) is considered the best imaging modality for victims of strangulation because it can assess the deep soft tissues, larynx, and vessels better than other techniques. Articles reporting on the use MRI to evaluate victims of strangulation are relatively new in the medical literature.66-68 Some of the initial case reports were on non-survivors of manual strangulation and often found fractures of the larynx and hyoid bone injuries uncommon in survivors. A small study of 14 survivors of manual strangulation found hemorrhage into the subcutaneous tissues, muscle (platysma), lymph nodes and salivary glands with MRI, but the life-threatening potential for these injuries remained undefined.68
An article from 2009 examined 56 survivors of strangulation injuries with MRI (without contrast) to determine if there were findings that correlated with life-threatening potential.69 Based upon their experience with both survivors and non-survivors of strangulation, two board-certified forensic pathologists using clinical information judged that 15 victims had life-threatening injury while 41 victims did not. In all 56 victims, the most common injuries noted were subcutaneous hemorrhage and edema (55%), followed by intramuscular hemorrhage and edema (29%), intracutaneous hemorrhage (29%), and swelling of the platysma (29%). The last three findings were the best for distinguishing between victims with life-threatening and non-life-threatening injuries, but the sensitivity was low, with only 53% of these individual findings present in those with life-threatening injury.
Because no single MRI finding was adequate to discriminate between the two groups, the authors developed a score based on the extent of injury within the neck.69 The neck was divided into three zones, from superficial to deep. Zone A included the skin and subcutaneous fat. Zone B included the cervical muscles, vessels, lymph nodes, and salivary glands. Zone C included the larynx and surrounding tissues. A score of 0 to 3 was assigned according to the number of zones with MRI findings; a score of 0 indicated that no MRI findings could be identified in any of the three zones, while a score of 3 indicated that all three zones were involved. A score of greater than or equal to 2 provided the best combination of sensitivity (67%) and specificity (73%) for detecting life-threatening injury.
Loss of consciousness was the clinical finding that produced the greatest correlation with MRI findings. Dysphagia and sore throat had a moderate correlation, while hoarseness had no correlation with MRI findings.
Interestingly, injuries to zone B (where the blood vessels run) had the greatest correlation with life-threatening strangulation as opposed to the expected deeper zone C (where the larynx and airway resides).69 The authors suggest that this finding supports the theory that death following strangulation is due more to obstruction to the cerebral circulation than to airway obstruction. The authors therefore termed zone B the "danger zone" for life-threatening injury after strangulation.
This MRI study has several limitations. The "gold standard" for life-threatening injury was determined by subjective judgment, albeit by experienced forensic pathologists who were not aware of the MRI findings during their deliberation. The number of patients is small, and there were no serious injuries found that have been described in strangulation victims laryngeal fracture, hyoid bone fracture, or carotid artery disruption. The absence of these findings in the study may not be such a shortcoming in that, while rare, identification of any one of these indicates a potential life threat regardless of other MRI findings.
There is not enough experience with MRI to present an evidence-based decision tool for its use in strangulation victims. Based upon the case reports and the study discussed above, the author of this article recommends that MRI be done in patients who are awake but report a loss of consciousness during the strangulation episode or have facial or conjunctival petechiae indicating that significant force was applied to the neck for a period of time greater than 15-30 seconds. For patients who remain unconscious, the physician will have a choice between CTA and MRI. In most settings, CTA will be more readily available from the emergency department.
Doppler ultrasound is useful to evaluate carotid artery flow. Intraluminal thrombosis is readily detected and sometimes intimal injury too. The use of Doppler ultrasound has been described in care reports of traumatic carotid artery thrombosis from hanging.27 One advantage of Doppler ultrasound is that the technique is portable and the device can be brought to the bedside of unstable patients. Also, the lack of radiation and no need for intravenous contrast enables the serial use of ultrasound as needed if the patient's clinical condition changes. The spatial resolution of Doppler ultrasound is on the range of 1 to 2 mm, which can be up to an order of magnitude less than for CT angiographic images. This lower resolution can lower the sensitivity for intimal injury and intraluminal thrombosis from blunt trauma to around 80-90% when compared to selective angiography. This presumably lower sensitivity for traumatic carotid injury has not been compared with CT angiography in strangulation victims to determine if the difference would be clinically relevant.
Fiberoptic laryngoscopy is useful to evaluate the vocal cords and adjacent structures for edema and hemorrhage.6,7,9,10 In a patient who is hoarse or reports difficulty talking, this technique can identify such injuries. However, fiberoptic laryngoscopy cannot evaluate injury to the deep neck tissues (muscles and vessels) that correlates with a potential life-threat. Thus, while commonly described as a potential modality to evaluate strangulation victims, the clinical utility of fiberoptic laryngoscopy to distinguish victims with life-threatening injuries from those without remains unproven.
The choice and sequence of imaging chosen by the physician is dependent on the patient's clinical condition and availability of the specific modalities. As noted in the discussion above, there is inadequate experience to develop a comprehensive evidence-based approach to imaging for strangulation victims. Based on the review of the literature noted above, the author of this article offers his recommendations. (See Table 4.)
Table 4: Imaging Recommendations for Strangulation Victims in the Emergency Department
|
Clinical Scenario |
Recommended Imaging Modality |
Alternative Imaging Modality |
|
Manual strangulation with no loss of consciousness and no physical evidence of force to the neck |
None |
None |
|
Manual strangulation with no loss of consciousness but with voice changes |
MRI with contrast |
Fiberoptic laryngoscopy |
|
Manual strangulation with loss of consciousness and/or physical evidence of force to the neck |
MRI without contrast |
CT with intravenous contrast |
|
Incomplete near-hanging with intact consciousness and bilateral neurologic function |
MRI without contrast |
CT with intravenous contrast |
|
Accidental strangulation with ligature caught in moving machinery but with intact consciousness and bilateral neurologic function |
MRI without contrast |
CT with intravenous contrast |
|
Any form of strangulation with persistent unconsciousness |
4-vessel cranial-cervical CT angiogram |
MRI without contrast |
|
Any form of strangulation with intact consciousness but with unilateral neurologic findings |
4-vessel cranial-cervical CT angiogram |
Doppler ultrasound of the carotid arteries or 4-vessel selective angiography |
Disposition and Follow-up
In general, the ED disposition of strangulation victims is primarily determined by their clinical condition and evidence of injury to their deep neck structures. At one extreme are patients who remain comatose, have a persistently altered mental status, or require ventilatory and/or cardiovascular support. These patients should be admitted to an intensive care unit for close monitoring and treatment. While rare, patients with laryngeal fracture detected by the presence of perilaryngeal emphysema or visible on MRI, hyoid bone fracture, or carotid artery injury should also be admitted to the intensive care unit, even if they are awake, have adequate spontaneous ventilation, and have no neurologic deficits. At the other extreme are patients with no loss of consciousness, minimal or no physical evidence of soft-tissue injury to the neck, a completely normal neurologic examination, a safe residence to go to, and responsible adults who can watch for the late development of complications. Such patients can be discharged.
In the middle are those with a report of loss of consciousness, have evidence of vascular obstruction with facial or conjunctival petechiae, or have symptoms or signs of soft-tissue injury to the neck. While they may be breathing normally, soft-tissue swelling and/or bleeding is likely to get worse. Such patients should be admitted for at least 12-24 hours for close monitoring.70 An alternative is the use of an ED-based 24-hour observation unit. Also, victims who are intoxicated from ethanol or drugs should be observed until the effect of those agents has dissipated.
The outcome of strangulation and hanging injuries arriving to the emergency department is determined by the presence of cardiopulmonary arrest (as indicated by a requirement for cardiopulmonary resuscitation at the scene and/or invasive airway management) and degree of anoxic brain injury (as correlated with a low scene and emergency department Glasgow Coma Score and cerebral edema on initial CT scan).71-73
Return to Case Scenarios
The patient with near-hanging from jail was intubated in the emergency department and admitted to the ICU. Over the next 36 hours, the patient recovered consciousness and was extubated on the second day. The second patient underwent CT scan of the neck with intravenous contrast that found edema of the platysma muscle. The patient was admitted for overnight observation and did well. While in the emergency department, the domestic violence advocate evaluated the patient, and the domestic violence report was completed and filed with the police. The third patient was admitted to the pediatric ICU. Discussion with the extended family identified a cousin who described playing the choking game with the patient for the purposes of getting "weird." Unfortunately, the patient sustained severe anoxic brain injury and died after care was withdrawn.
References
1. Cartwright AJ. Degrees of violence and blood spattering associated with manual and ligature strangulation: A retrospective study. Med Sci Law 1995;35:294-302.
2. Hawley DA, McClane GE, Strack GB. A review of 300 attempted strangulation cases Part III: Injuries in fatal cases. J Emerg Med 2001;21:317-22.
3. Sharma BR, Harish D, Sharma A, et al. Injuries to neck structures in deaths due to constriction of neck, with a special reference to hanging. J Forensic Leg Med 2008;15:298-305.
4. Sauvageau A, Godin A, Desnoyers S, et al. Six-year retrospective study of suicidal hangings: Determination of the pattern of limb lesions induced by body responses to asphyxia by hanging. J Forensic Sci 2009;54:1089-92.
5. Godin A, Kremer C, Sauvageau A. Fracture of the cricoid as a potential pointer to homicide: A 6-year retrospective study of neck structures fractures in hanging victims. Am J Forensic Med Pathol 2010 Feb 25. [Epub ahead of print]
6. Wahlen BM, Thierbach AR. Near-hanging. Eur J Emerg Med 2002;9:348-50
7. Funk M, Schuppel J. Strangulation injuries. Wisc Med J 2003;102:41-5.
8. Stanley RB Jr, Hanson DG. Manual strangulation injuries of the larynx. Arch Otolaryngol 1983;109:344-7.
9. Iserson KV. Strangulation. A review of ligature, manual, and postural neck compression injuries. Ann Emerg Med 1984;13:179-85.
10. McClane GE, Strack GB, Hawley D. A review of 300 attempted strangulation cases Part II: Clinical evaluation of the surviving victim. J Emerg Med 2001;21:311-5.
11. Plattner T, Bolliger S, Zollinger U. Forensic assessment of survived strangulation. Forensic Sci Int 2005;153:202-7.
12. Sauvageau A, Boghossian E. Classification of asphyxia: The need for standardization. J Forensic Sci 2010 Jun 17. [Epub ahead of print]
13. Sauvageau A, Yesovitch R. Choking on toilet paper: an unusual case of suicide and a review of the literature on suicide by smothering, strangulation, and choking. Am J Forensic Med Pathol 2006;27:173-4.
14. Masand M. Accidental strangulation with a Venetian blind cord a near miss. BMJ 2010;340:c3458.
15. Sep D, Thies KC. Strangulation injuries in children. Resuscitation 2007;74:386-91.
16. Chattopadhyay S, Pal I. Survival following accidental ligature strangulation: A case report. J Forensic Leg Med 2008;15:53-5.
17. Gowens PA, Davenport RJ, Kerr J, et al. Survival from accidental strangulation from a scarf resulting in laryngeal rupture and carotid artery stenosis: The "Isadora Duncan syndrome." A case report and review of literature. Emerg Med J 2003;20:391-3.
18. Morild I. Fractures of neck structures in suicidal hanging. Med Sci Law 1996;36:80-4.
19. Kiani SH, Simes DC. Delayed bilateral internal carotid artery thrombosis following accidental strangulation. Br J Anaesth 2000;84:521-4.
20. Fineron PW, Turnbull JA, Busuttil A. Fracture of the hyoid bone in survivors of attempted manual strangulation. J Clin Forensic Med 1995;2:195-7.
21. Maxeiner H, Bockholdt B. Homicidal and suicidal ligature strangulation a comparison of the post-mortem findings. Forensic Sci Int 2003;137:60-6.
22. Travis LW, Olson NR, Melvin JW, et al. Static and dynamic impact trauma of the human larynx. Trans Sect Otolaryngol Am Acad Ophthalmol Otolaryngol 1975;80(4 Pt 1):382-90.
23. Khokhlov VD. Pressure on the neck calculated for any point along the ligature. Forensic Sci Int 2001;123:178-81.
24. Singh B, Kumar S, Kumar V. Blunt laryngotracheal injury following accidental strangulation. Injury 2003;34:937-9.
25. Kaki A, Crosby ET, Lui AC. Airway and respiratory management following non-lethal hanging. Can J Anaesth 1997;44:445-50.
26. Malek AM, Higashida RT, Halbach VV, et al. Patient presentation, angiographic features, and treatment of strangulation-induced bilateral dissection of the cervical internal carotid artery. Report of three cases. J Neurosurg 2000;92:481-7.
27. Clarot F, Vaz E, Papin F, Proust B. Fatal and non-fatal bilateral delayed carotid artery dissection after manual strangulation. Forensic Sci Int 2005;149:143-50
28. Chokyu I, Tsumoto T, Miyamoto T, et al. Taumatic bilateral common carotid artery dissection due to strangulation. A case report. Interv Neuroradiol 2006;12:149-54.
29. Cothren CC, Moore EE. Blunt cerebrovascular injuries. Clinics (Sao Paulo). 2005;60:489-96.
30. Maiza D, Theron J, Martel B, et al. [Acute carotid occlusion: Thrombolytic treatment] J Mal Vasc 1996;21 Suppl A:83-9.
31. Hellier C, Connolly R. Cause of death in judicial hanging: A review and case study. Med Sci Law 2009;49:18-26.
32. Lang SA, Duncan PG, Shephard DA, et al. Pulmonary oedema associated with airway obstruction. Can J Anaesth 1990;37:210-8.
33. Howell MA, Guly HR. Near hanging presenting to an accident and emergency department. J Accid Emerg Med 1996;13:135-6.
34. Hawton K, Bergen H, Casey D, et al. General hospital presentations of non-fatal hanging over a 28-year period: Case-control study. Br J Psychiatry 2008;193:503-4.
35. van de Ven K, Vanclooster P, de Gheldere C, et al. Strangulation: A late presentation of right-sided diaphragmatic rupture. Acta Chir Belg 1995;95:226-8.
36. Taniguchi T, Saito S, Mizukoshi Y, et al. Multiple organ failure after strangulation injury. Intensive Care Med 2002;28:1193.
37. Ramírez JI, Petrone P, Kuncir EJ, et al. Thyroid storm induced by strangulation. South Med J 2004;97:608-10.
38. Wilbur L, Higley M, Hatfield J, et al. Survey results of women who have been strangled while in an abusive relationship. J Emerg Med 2001;21:297-302.
39. Taliaferro E, Mills T, Walker S. Walking and talking victims of strangulation. Is there a new epidemic? A commentary. J Emerg Med 2001;21:293-5.
40. Block CR, Engel B, Naureckas SM, et al. The Chicago women's health risk study: Lessions in collaboration. Violence Against Women 1999;5:1158-1177.
41. Glass N, Laughon K, Campbell J, et al. Non-fatal strangulation is an important risk factor for homicide of women. J Emerg Med 2008;35:329-35.
42. Block CR, Devitt CO, Fonda D, et al. The Chicago women's health study: Risk of serious injury or death in intimate violence: A collaborative research project. Washington DC: Department of Justice. National Institute of Justice; 2000.
43. Strack GB, McClane GE, Hawley D. A review of 300 attempted strangulation cases. Part I: Criminal legal issues. J Emerg Med 2001;21:303-9.
44. Laughon K, Glass N, Worrell C. Review and analysis of laws related to strangulation in 50 states. Eval Rev 2009;33:358-69. Epub 2009 Jun 9.
45. [No authors listed]. Unintentional strangulation deaths from the "choking game" among youths aged 6-19 years United States, 1995-2007. Centers for Disease Control and Prevention (CDC). MMWR Morb Mortal Wkly Rep 2008;57:141-4.
46. [No authors listed]. "Choking game" awareness and participation among 8th graders Oregon, 2008. Centers for Disease Control and Prevention (CDC). MMWR Morb Mortal Wkly Rep 2010;59:1-5. Erratum in: MMWR Morb Mortal Wkly Rep 2010;59:49.
47. Egge MK, Berkowitz CD, Toms C, et al. The choking game: a cause of unintentional strangulation. Pediatr Emerg Care 2010;26:206-8
48. Le D, Macnab AJ. Self strangulation by hanging from cloth towel dispensers in Canadian schools. Inj Prev 2001;7:231-3.
49. Toblin RL, Paulozzi LJ, Gilchrist J, et al. Unintentional strangulation deaths from the "choking game" among youths aged 6-19 years United States, 1995-2007. J Safety Res 2008;39:445-8.
50. Katz KA, Toblin RL. Language matters: Unintentional strangulation, strangulation activity, and the "choking game." Arch Pediatr Adolesc Med 2009;163:93-4.
51. Cowell DD. Autoerotic asphyxiation: Secret pleasure lethal outcome? Pediatrics 2009;124:1319-24.
52. Sabo RA, Hanigan WC, Flessner K, et al. Strangulation injuries in children. Part 1. Clinical analysis. J Trauma 1996;40:68-72.
53. Sauvageau A, Racette S. Autoerotic deaths in the literature from 1954 to 2004: A review. J Forensic Sci 2006;51:140-6.
54. Boots RJ, Joyce C, Mullany DV, et al. Near-hanging as presenting to hospitals in Queensland: Recommendations for practice. Anaesth Intensive Care 2006;34:736-45.
55. Janata A, Holzer M. Hypothermia after cardiac arrest. Prog Cardiovasc Dis 2009;52:168-79.
56. Sagalyn E, Band RA, Gaieski DF, et al. Therapeutic hypothermia after cardiac arrest in clinical practice: Review and compilation of recent experiences. Crit Care Med 2009;37(7 Suppl):S223-6.
57. Borgquist O, Friberg H. Therapeutic hypothermia for comatose survivors after near-hanging a retrospective analysis. Resuscitation 2009;80:210-2.
58. Jehle D, Meyer M, Gemme S. Beneficial response to mild therapeutic hypothermia for comatose survivors of near-hanging. Am J Emerg Med 2010;28:390.e1-3
59. Baldursdottir S, Sigvaldason K, Karason S, et al. Induced hypothermia in comatose survivors of asphyxia: A case series of 14 consecutive cases. Acta Anaesthesiol Scand 2010;54:821-6.
60. Mohanty MK, Rastogi P, Kumar GP, et al. Periligature injuries in hanging. J Clin Forensic Med 2003;10:255-8.
61. Nielson AS, Kang CS. Images in emergency medicine. Chokehold strangulation. Ann Emerg Med 2006;47:327, 343.
62. Lambe A, Püschel K, Anders S. Extensive petechiae in attempted self-strangulation. J Forensic Sci 2009;54:212-5..
63. Miller PR, Fabian TC, Croce MA, et al. Prospective screening for blunt cerebrovascular injuries: Analysis of diagnostic modalities and outcomes. Ann Surg 2002;236:386-93; discussion 393-5.
64. Sliker CW, Shanmuganathan K, Mirvis SE. Diagnosis of blunt cerebrovascular injuries with 16-MDCT: Accuracy of whole-body MDCT compared with neck MDCT angiography. AJR Am J Roentgenol 2008;190:790-9.
65. Langner S, Fleck S, Kirsch M, et al. Whole-body CT trauma imaging with adapted and optimized CT angiography of the craniocervical vessels: Do we need an extra screening examination? AJNR Am J Neuroradiol 2008;29:1902-7.
66. Yen K, Thali MJ, Aghayev E, et al. Strangulation signs: Initial correlation of MRI, MSCT, and forensic neck findings. J Magn Reson Imaging 2005;22:501-10.
67. Matsuyama T, Okuchi K, Seki T, et al. Magnetic resonance images in hanging. Resuscitation 2006;69:343-5.
68. Yen K, Vock P, Christe A, et al. Clinical forensic radiology in strangulation victims: Forensic expertise based on magnetic resonance imaging (MRI) findings. Int J Legal Med 2007;121:115-23.
69. Christe A, Thoeny H, Ross S, et al. Life-threatening versus non-life-threatening manual strangulation: Are there appropriate criteria for MR imaging of the neck? Eur Radiol 2009;19:1882-9.
70. Di Paolo M, Guidi B, Bruschini L, et al. Unexpected delayed death after manual strangulation: Need for careful examination in the emergency room. Monaldi Arch Chest Dis 2009;71:132-4.
71. Penney DJ, Stewart AH, Parr MJ. Prognostic outcome indicators following hanging injuries. Resuscitation 2002;54:27-9.
72. Matsuyama T, Okuchi K, Seki T, et al. Prognostic factors in hanging injuries. Am J Emerg Med 2004;22:207-10.
73. Nichols SD, McCarthy MC, Ekeh AP, et al. Outcome of cervical near-hanging injuries. J Trauma 2009;66:174-8.
You are on duty in the ED when the paramedics bring in a patient from the county jail who had tried to hang himself. When the patient arrives, you are told by the accompanying guard that the patient was found with a tightly twisted bedsheet around his neck and looped over the bedpost of the metal bunkbed.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
