2004 Salary Survey Results: Quality role is evolving from number cruncher to leader
Salaries and respect are increasing, but only if you take the right steps
The quality professional’s role continues to evolve, with many professionals stepping into leadership and business roles, according to the latest Hospital Peer Review salary survey.
"The strategic importance of quality managers in this pay for performance environment is increasing," says Patrice L. Spath, BA, RHIT, a health care quality specialist with Forest Grove, OR-based Brown-Spath & Associates, referring to the linking of core measure outcomes with Medicare reimbursement.
The 2004 Hospital Peer Review Salary Survey was mailed to readers in the June 2004 issue.
This year’s results show that 44% of quality professionals reported an annual gross income in the $50,000 to $69,000 range, with 9% reporting income more than $100,000.
Slightly more than half of the respondents reported a salary increase of 1% to 3%, 29% reported an increase of 4% to 6%, while 11% received an increase of more than 7%.
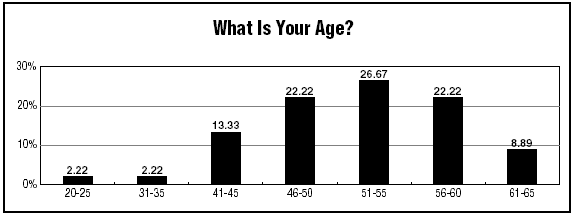
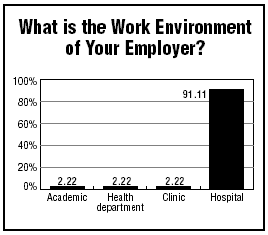
There has never been a time in which the quality of health care services has mattered so much to hospital CEOs, Spath adds.
"But need alone can’t guarantee that quality managers will be seen as trusted business advisors. Quality managers must be more than number crunchers," she says.
Quality management essentially is a consultative function, Spath explains.
"In many respects, the quality executive is no different from a management consultant. He or she has a great deal of responsibility and very little authority," she points out.
To be heard and be effective in the role, the quality manager must gain the respect of senior administrative and medical staff leaders and managers, and establish camaraderie with these individuals, Spath advises.
"Credibility and reliability are only two aspects of the trust relationship that must exist between the quality department and the rest of the organization," she points out.
"Quality professionals often rely solely on these two factors, thus missing many of the other factors that go into creating trusting relationships," Spath continues.
Many times, quality leaders make the mistake of overemphasizing their technical skills and credentials, when people are more interested in results, she explains.
"We need to learn how to measure and articulate the value of quality management activities — talk results, not expertise!" Spath says.
More quality directors are becoming vice presidents than in the past, due to an increased number of individuals getting master’s degrees and because of the breadth that quality now has in an organization, says Janet A. Brown, RN, BSN, BA, CPHQ, FNAHQ, president of JB Quality Solutions Inc., based in Pasadena, CA.
"There are certainly more salaries over $100,000. I think that’s amazing, because there was a time when people thought quality was going by the wayside, particularly in the early 1980s with the implementation of the Medicare Prospective Payment System and the early 1990s with the onset of managed care," she points out.
More organizations are recognizing that quality is a worthwhile investment of money and resources, Brown says.
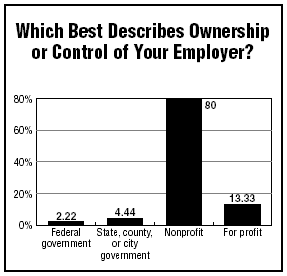
"I think there is a whole philosophy that quality is valuable now, that it’s not just an extra expense," she adds.
Most of the survey respondents appear to be at the middle-management level, Spath notes.
"When quality managers become trusted business advisors, not just technically skilled data analysts, it is quite likely we’ll see more of them assuming senior leadership positions in their organization," she predicts.
The role of the quality professional continues to change, Brown says. "Many are becoming patient safety officers, for example. In the past, the safety emphasis was linked to environment of care. The push for patient safety has moved this role more into the quality arena."
This is largely a result of the Institute of Medi-cine’s 1999 report To Err Is Human: Building a Safer Health System, which found that more people die from medical mistakes each year than from highway accidents, breast cancer, or AIDS, and its 2001 report Crossing the Quality Chasm: A New Health System for the 21st Century, Brown adds.
"Since that time, we have seen more of a link between the quality professional and safety," she says.
Patient safety is a role that organizational leaders can grasp easily, Brown stresses. "This is a quality function that administration can get their hands around quickly, because it’s a risk management issue and a bottom-line issue as well," she explains.
Still, there is no question that you will need to sharpen your skills to advance in today’s quality field, Brown notes.
She suggests using the content outline of the Certified Professional in Healthcare Quality (CPHQ) exam as a guideline.
"Those tasks are concrete and are the things quality professionals must be prepared to do," Brown explains. This includes quality management, quality improvement, case/care/disease/ utilization management, and risk management activities.
Having an organizationwide role is key, such
as being involved in strategic planning, and developing the balanced scorecard for performance measures, she says.
The role of the quality professional should include the processes of organizationwide implementation, measurement, and reporting of performance measures that directly link to strategic goals, Brown adds.
"The skills of the quality professional as leader also include coordination of the quality data organizationwide, not limited just to the medical staff level or departmental level and just collecting data," she says.
"We’ve got to understand enough about statistics to know which statistical tools and graphs and data displays to use, and what kind of reports are needed at all levels. We’ve got to know who are the best statisticians and information technology professionals in the organization and how to get to them on a daily basis, if needed," Brown notes.
"However, I can only hope that quality professionals who agree to take on these roles are requesting a commensurate increase in salary. If you have the authority to do the job, you have to have the salary commensurate with that," she says. "I don’t know whether that’s happening or not."
Above all, quality professionals must be able to work effectively with other leaders in the organization, Brown stresses. "They need to have a comfortable relationship with everyone in leadership and be able to pick up the phone without feeling intimidated," she says. "You need to know your leadership role and use it."
More than half (62%) of quality professionals are working more than 45 hours a week, with 11% reporting spending more than 55 hours a week
at work. Just 13% work fewer than 40 hours, and another 24% work between 41 and 45 hours a week.
"The more roles you take on, the longer the hours you are going to be working. There is no way around it," Brown continues. Although long hours go with the territory, you need to master the art of delegation, she says. "You end up knowing every problem in the organization, so people will come to the quality professionals for answers or problem solving. Therefore, you have to be a great delegator."
Whenever you take on a new role, you have to determine what the roll out is going to be, such
as identifying the processes that will have to be done and who has the expertise to do them, says Brown.
"If you need more staffing, more time, more computers or other resources, or access to other people like information technology staff or statisticians, that’s the leader’s responsibility to ascertain and request," she says.
You’ll need to determine who in the organization has the skills to meet the new demand and what training may be necessary, Brown explains.
"What can you as a leader train others to do?" she asks.
Communication is the key to thriving in a leadership role, and the leader of any quality team has to meet with them regularly, Brown says. In thinking of the quality umbrella departments, this includes those performing in quality, utilization, risk management, infection control, social services, patient representatives, and data analysts, she says.
Walk around management is easier if you have geography in your favor; but if your team is not centrally located, you’ll need to find a way to communicate, which could mean e-mail, telephones, pagers, and/or meetings, Brown explains.
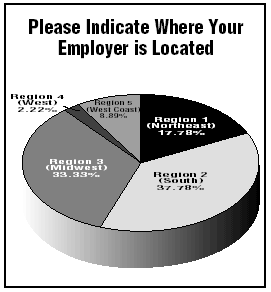
"You have to have that kind of responsiveness to each other," she says. Brown suggests having purposeful informal meetings to pass on tasks and allow staff to vent their concerns.
"In order to delegate effectively, you need to communicate and assure them that you are equally committed to the task, and be prepared for feedback," she says.
"Ensuring good process flow requires good communication, and the leader has to find ways to make that happen."
The No. 1 goal is to think of yourself as a leader, Brown urges. "You need to see yourself and have others see you as the organizational expert on quality," she says.
"But I think that leader has to design the process model so that all those with skills and desire to perform can flourish. If the leader is too overwhelmed, he or she can’t be responsive to other people, or the tasks and objectives are not met," she says. "The organization’s performance goals are met when the team works well and feels valued."
The quality professionals role continues to evolve, with many professionals stepping into leadership and business roles, according to the latest Hospital Peer Review salary survey.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
