Psychiatric patients in the ED: Evaluate, document, consult
By Christopher White, MD, JD, Attending Physician, University of Cincinnati Hospital; Lawson Wulsin, MD, Associate Professor of Psychiatry and Family Medicine, University of Cincinnati College of Medicine.
Editor’s note: Patients with psychiatric disorders are a substantial component of the practice of emergency medicine. These patients often have little insight into their problems, may often have impaired communication capabilities, and often will have underlying medical issues that can exacerbate their psychiatric problems. The emergency physician (EP) often is called upon to medically clear these patients, particularly prior to an involuntary psychiatric admission. The process of medical clearance can be fraught with dangers. At times, there is a fine line between diagnosing the altered mental status caused by a mild to moderate delirium originating from a medical condition and a mild psychosis originating from a psychiatric condition.
This issue discusses some of the pitfalls that may arise in the care of the psychiatric patient. The lessons learned may assist EPs and nurses in reducing their malpractice risk, but more importantly, assist them in providing a safe disposition for these patients.
Introduction
Psychiatric patients present unique challenges to the diagnosis and management of conventional medical problems. Up to 50% of primary care patients have either primary or comorbid psychiatric diagnoses.1 Furthermore, studies have shown that an organic cause can be identified for only 25% of the following primary care complaints: fatigue, back pain, dizziness, headaches, dyspnea, angina, abdominal pain, and anxiety.2 These numbers also can apply to today’s emergency departments (EDs), where many people turn for primary care services. These patients often take more time than medical patients without psychiatric disorders. Additionally, failing to consider the psychiatric aspects of care in the ED may result in frequent visits to the ED or other physicians. Plaintiff attorneys are quick to seize upon bad outcomes involving psychiatric patients and may comb through medical records looking for any potential deviations in care. Given the frequency with which psychiatric patients present to the ED, prudent risk management requires a comprehensive review of how psychiatric patients are handled in your ED.
Deviations in care range from entirely missing psychiatric diagnoses by exclusively focusing on somatic complaints to prematurely attributing the patient’s medical complaints to their known psychiatric diagnosis and halting any further diagnosis or treatment. When EPs release patients without any mental health evaluation and these patients go on to attempt suicide, attorneys justifiably ask questions. The entertainment industry often portrays psychiatric patients as dangerous and prone to violence; this occurrence is rare, but it is not zero. Inquiry into suicide risk and danger to others always is appropriate when dealing with patients who have major psychiatric disorders. Finally, treatment of psychiatric patients also can raise novel questions under traditional ED policies, such as those drafted in response to the Emergency Medical Treatment and Labor Act (EMTALA).
Psychotic or Agitated Patients
In contrast to Hollywood’s portrayal of acutely psychotic patients, these patients may roam the streets and coexist, albeit at the fringe of society, and only rarely become violent. In the ED setting, where multiple patients are in various stages of work-up, psychotic patients acting out can be disruptive to the ED. Definitions of psychosis focus on the presence of auditory or visual hallucinations or delusions. In fact, grossly disorganized speech or behavior also suggests an underlying psychotic disorder, even in the absence of hallucinations.3 Not all agitated/psychotic patients suffer from solely psychiatric diagnoses. Delirium, acute intoxication, and some organic brain diseases all can present with agitation. These medical conditions must be excluded before a final psychiatric diagnosis can be attached. Furthermore, delirium alone can represent significant pathology, which if unrecognized or untreated, can cause serious harm to the patient. Thus, any patient who presents agitated or showing signs of psychosis should have a comprehensive medical evaluation before being referred to the mental health services. Unfortunately, the agitated or psychotic patient poses a challenge to interview and examine, thereby further complicating the evaluation.
When one encounters an acutely psychotic and agitated patient, care must be taken to ensure the safety of the patient, yourself, and third parties who could be harmed. The hallmark of all psychotic patients is that they have an impairment in reality testing — a fact that must be remembered when interacting with them and performing the diagnostic evaluation. An agitated patient may demonstrate psychomotor restlessness (e.g., pacing or yelling). The patient may adopt threatening postures or interact with the examiner in a manner that makes the physician feel anxious; these actions often precede violence and, therefore, should be a warning.4 Previous history of violence also is a good predictor of future violence, and this information should be obtained whenever presented with a psychotic or acutely agitated patient. Clinicians should be non-threatening and approach such patients from an angle and with one’s hands in full view. Careful planning, such as preventing the patient from coming between you and the exit, plus making all staff aware of the patient prior to entering the exam area, helps to ensure that resources are available to assist should the patient’s aggressive actions escalate.
Case #1: Psychotic Patient Released
In Brown v. Carolina Emergency Physicians,5 Chris Brown noticed a gradual change in his wife’s behavior as she became more lethargic and depressed. Mr. Brown, who was a member of the National Guard, was scheduled to serve his two-week annual training session in New Mexico. Because of his wife’s condition, he spoke with his commanding officer and requested permission to stay at home. His commanding officer required that he obtain a physician’s note certifying that Mr. Brown was needed at home.
Mr. Brown took his wife to Greenville Memorial Hospital’s ED to obtain the required physician’s statement. Dr. Benjamin Crumpler, the EP on duty, examined Mrs. Brown and diagnosed her with acute delusional psychosis. Based on his observations, he recommended that Mrs. Brown be admitted to the hospital, but neither Mr. nor Mrs. Brown wanted her to be admitted. Because it was Friday, Mr. Brown assured Dr. Crumpler that he would care for his wife at home during the weekend and return to the ED if needed. Dr. Crumpler then obtained collateral information from a family friend regarding the couple. Satisfied by this conversation and Mr. Brown’s assurances, he arranged for the required National Guard physician’s note, provided referral to a mental health center the following Monday, and prescribed hydroxyzine for Mrs. Brown.6
Although the following day Mrs. Brown seemed better, by Sunday she was strangely energetic, racing around the family’s home singing religious hymns. Mr. Brown physically restrained her and carried her to the bedroom after she suddenly fell asleep in the midst of the struggle. When she awoke some 30 minutes later, she was very agitated. After a verbal confrontation with her husband, she became very angry and repeatedly hit him with a rod. Following another physical struggle, she again suddenly went limp and appeared to be asleep. Mr. Brown left the room, went to the kitchen, and called 911. While he was on the phone, Mrs. Brown beat the couple’s 16-month-old son to death.
At Mrs. Brown’s criminal trial, psychiatric experts testified that she suffered from paranoid schizophrenia and thus, was unable to distinguish between moral and legal right and moral and legal wrong when she killed her son. The State stipulated that Mrs. Brown was not guilty by reason of insanity. The family then filed a civil action against the hospital and Dr. Crumpler seeking damages. The Browns claimed that Dr. Crumpler’s negligent failure to properly diagnose, treat, and hospitalize Mrs. Brown proximately caused the death of their son. The trial court granted summary judgment for the defendant hospital and physicians.
On appeal, the South Carolina Court of Appeals reversed and held that Dr. Crumpler’s inadequate treatment of Mrs. Brown’s psychosis in the ED was the proximate cause of her fatal assault on the couple’s youngest son a few days later.7 The court was convinced by the plaintiff’s expert witnesses who opined that Mrs. Brown’s condition "warranted either a psychological evaluation to be performed by a licensed psychologist or a psychiatric consultation to be performed by a licensed psychiatrist."8 The experts agreed that given Mrs. Brown’s psychotic state as identified by Dr. Crumpler, hospitalization was the proper course of action. Failing to do this, Dr. Crumpler negligently failed to prescribe appropriate antipsychotic medication. The antihistamine, although perhaps mitigating some symptoms, did nothing to treat the underlying problem. Finally, the referral to a community counseling center was not an appropriate initial step in treating Mrs. Brown’s psychosis.
Discussion
One problem in this case arose when Dr. Crumpler diagnosed a psychotic disorder but did not initiate any treatment for this potentially dangerous condition. Obligation to initiate treatment or transfer to an appropriate institution depends on the assessment of the severity of the condition. In this sense, psychosis is the psychological equivalent of acute physical pain. Once recognized, patients with psychosis or who are high suicide risks legitimately deserve hospitalization unless a sound alternative plan is established. By any standard of practice, Dr. Crumpler’s plan was not sufficient to initiate treatment of psychosis. A better alternative for the patient (and for Dr. Crumpler) would have been to prescribe a low dose of an antipsychotic medication, such as haloperidol (Haldol) or olanzapine (Zyprexa).
For agitation in the absence of psychosis, short-acting benzodiazepines, such as lorazepam (Ativan), may be sufficient. Lorazepam often is used because it has good absorption when given in the intramuscular (IM) form, unlike many other benzodiazepines. However, careful use of benzodiazepines is warranted in some patient populations, such as the elderly, children, and the mentally retarded due to concern about excessive sedation or concern regarding possible disinhibition. Antihistamines can be used acutely for their sedating properties and often are employed in the control of agitated children. Diphenhydramine (Benadryl) is used in the IM form in these situations and is dosed on the patient’s weight, but should not exceed 5 mg/kg/day.
Although haloperidol was the antipsychotic of choice for IM delivery for many years, there is a definite risk of dystonic reactions for patients with psychosis, which can be significant and even life-threatening if laryngospasm occurs. For this reason, the pharmaceutical companies that manufacture the newer atypical antipsychotics have developed several alternative delivery routes. Ziprasidone (Geodon) and olanzapine both have injectable preparations. Risperidone (Risperdal) has an oral solution and a rapidly disintegrating tablet that melts instantly when placed on the tongue. These newer agents are used routinely in the psychiatric ED setting and should be available in the traditional ED.
Multidisciplinary Team Approach
Most mental health management involves reliance on a multidisciplinary team approach to the patient. Members of the team include social workers, psychologists, nurses, and case managers, in addition to the physician. Both social workers and psychologists can perform initial assessments and also may provide counseling or long-term therapy for patients.
Social workers facilitate locating community resources; psychologists often are employed for diagnostic testing. In the ED setting, staffing issues often require that initial assessments be delegated to these midlevel providers. However, all members of the team are specifically trained to assist in the provision of mental health services and play valuable roles despite approaching the patient from divergent backgrounds. When midlevel providers play a role in the diagnostic evaluation of a psychiatric patient, it remains the ultimate liability of the physician to ensure that the appropriate assessment and treatment plan is completed.
Case #2: Is Psychological Evaluation Malpractice?
Hodges v. State of Tennessee9 raises the somewhat intellectual question of whether one can avoid professional malpractice claims under the doctrine of sovereign immunity by using psychologists to perform ED evaluations instead of psychiatrists.
Anthony Hodges was transported to the ED at the Regional Medical Center in Memphis following his attempted suicide. In the ED, he was evaluated and treated by Dr. James Buechele, a psychologist employed by the state of Tennessee to perform psychiatric evaluations. The patient was released from the ED and fewer than 12 hours later committed suicide. Mr. Hodges’ widow filed a lawsuit against the state claiming that Dr. Buechele committed negligence in failing to treat or hospitalize Mr. Hodges.
The State of Tennessee successfully argued at the trial level that the Tennessee constitution limits governmental liability and thus, barred Mrs. Hodges lawsuit under the doctrine of sovereign immunity. On appeal, it was noted that the legislature recently had amended the statute that abrogated immunity for "professional malpractice" by changing the wording to "legal or medical malpractice" claims.10 Based on this change, the State argued that when psychologists perform ED evaluations, they are not practicing medicine and thus, cannot be subjected to medical malpractice liability. The appeals court rejected this argument and held that the State cannot avoid liability for psychiatric evaluations in the ED by using psychologists in lieu of psychiatrists. Although a psychologist, Dr. Buechele acted in a medical capacity when he evaluated Mr. Hodges, utilized the same American Psychiatric Association guidelines as psychiatrists, and performed the same function as a psychiatrist while working in the ED.11 Accordingly, the imposition of liability on the State of Tennessee for his negligence was justifiable.
Discussion
This case illustrates that the physician cannot escape ultimate responsibility by using midlevel providers. As some of the later cases also make clear, the EPs can be held liable despite their reliance on a mental health consult when the consult provider is not a physician. In lawsuits, physicians are targeted for their perceived wealth, but also because there exists the notion that the treating physician is the captain of the ship. The recent advent of prescription drug privileges for psychologists in several states will continue to test the outer limits of midlevel mental health workers’ liability and the overlap between their evolving roles and that of treating physicians. This case did not specifically mention the ED provider because it raised a fairly narrow question.
The ED physician is responsible for the assessment of the psychiatric patient and the determination of whether a consult is needed. He or she remains ultimately liable for the care of the patient in the ED regardless of who or what type of service is consulted. Ultimately, the consultant should be viewed as making recommendations, which the treating ED physician is free to adopt or reject — especially true when the consultant is not a physician but rather a midlevel provider. It is not appropriate nor medicolegally prudent to pretend a psychiatric patient no longer exists on the ED board simply because a psychiatric consult has been called any more than you would leave a chest pain patient once you notify cardiology. The specialist obviously will focus on the specific question or problem posed in their area of expertise, whereas the ED physician should ensure that all consultants work together to address the patient’s needs. Therefore, this case had more to do with the level of supervision provided to a nonphysician psychiatric consultant than the issue of whether it is malpractice to release a suicidal patient.
Conditions Attributed to Psychiatric Disorders
The patient with panic disorder presents with a panic attack that turns out to be a true myocardial infarction (MI). The depressed pregnant woman with a cocaine habit has undiagnosed hypocalcaemia and rickets. The differential diagnosis of medical conditions in patients with known psychiatric disorders can be challenging. The key strategy for not being misled by psychiatric diagnoses rests with a sound psychiatric history and its temporal ties to the current physical symptoms. If, by reviewing the prior records, these symptoms are new or out of the ordinary for this patient, then added attention should be paid. Often, cases of multiple sclerosis, other cerebral insults, and systemic illnesses are first diagnosed on the psychiatric floor. These diagnoses typically follow a patient’s multiple admissions and occur when a clinician realizes that a complete organic work-up has not been completed.
Case #3: MI Called Conversion Disorder
In Brown v. Christian Health Ministries,12 Ms. Brown was brought to the ED complaining of multiple vague symptoms. She had a recent history of stroke and heart disease. Dr. Catherine Loe (the EP on duty) examined Ms. Brown, ordered a heart monitor, multiple laboratory studies, and a CT scan of Mrs. Brown’s head. During this time, Ms. Brown’s personal physician also came to the ED and examined her. Both physicians, independent of one another, diagnosed the patient with a conversion disorder. A conversion disorder occurs when a patient’s psychological or emotional problems manifest as physical symptoms. The hospital did not have any psychiatric facilities, so arrangements were made to transfer the patient to a psychiatric hospital.
Ms. Brown was transferred four hours after her arrival at the ED and arrived at the accepting hospital after an hour-long ambulance ride. Approximately two hours after arriving at the psychiatric facility, she developed hemoptysis. The psychiatric facility began to arrange transfer to a local hospital for treatment. Her vital signs continued to deteriorate, and she subsequently died. Following a post-mortem exam, the cause of death was determined to be primarily an MI, with coronary atherosclerosis and a cerebral lacunar infarct contributing.13
Ms. Brown’s relatives brought suit against the treating hospitals claiming an EMTALA violation by not providing an adequate medical screening exam. In reviewing the medical record, the court found that the ED exams and studies did not explain Ms. Brown’s symptoms. Additionally, her vital signs were stable and did not deteriorate until two hours after transfer. Finally, the court had an affidavit indicating that the patient was stable for transfer and that the patient’s sister had consented to the transfer. The court cited numerous authorities for the proposition that EMTALA is not a federal malpractice standard and that as long as Ms. Brown received the same screening exam as other patients, no violation exists. "Faulty screening, in a particular case, as opposed to disparate screening or refusing to screen at all, does not contravene the statute."14 Accordingly, the District Court granted summary judgment for the defendants, Dr. Loe, and ED staff.
Discussion
Although couched in terms of EMTALA litigation, there certainly was a corresponding state malpractice claim. However, the fact pattern was particularly illustrative of what can happen when a patient complaining of vague symptoms and with a known psychiatric history presents to an overworked ED. Many psychiatric patients with comorbid medical conditions may have a mental illness that affects their adherence or follow-up. Many of these patients also may not have received significant screening or preventative health exams; therefore, care should be taken to ensure that a psychiatric patient’s known, as well as potential, medical history is reviewed. Accordingly, this case reaffirms the principle that good medical practice is the best defense against medical malpractice. Sufficient cardiac screening in this case may have ruled out an acute MI at the time of the initial ED examination, absolving Dr. Loe of responsibility for the later MI in a different setting. It is unclear from the court documents if the patient actually complained of cardiac symptoms. However, this case also reminds us of the toll that psychiatric disorders take on the cardiovascular system,15 and the need for particularly careful cardiac evaluations of pat-ients with acute exacerbations of psychiatric disorders.
In particular, the recurrent nature of most anxiety and depressive disorders eventually may dysregulate the stress response symptom and the autonomic nervous system, raising resting heart rate, decreasing heart rate variability, altering glucose regulation via excessive cortisol secretion, increasing platelet aggregation, and promoting plaque formation in the coronary arteries. In patients with pre-existing coronary disease, the intense autonomic discharge of a panic attack may overwhelm the marginal resilience of the diseased heart and contribute to ischemia. Documenting sufficient physical evaluation in patients with symptoms that may be explained by their psychiatric disorders is not only legally sound, it is clinically prudent.16
Involuntary Admission and Psych Holds
Although the laws vary from state to state, the general principle that patients can be committed involuntarily to the hospital is universal. The statutory schemes usually involve a variation on the following theme: The patient in question has a mental illness (often drugs and alcohol are excluded) and because of this mental illness, poses a serious risk of harm to himself or others or is grossly unable to care for himself.17 The statutes specify the specific procedure that must be followed, but it usually involves a qualified individual providing an initial report that often is based on either direct observations or a witness’s statement. Once this statement is submitted to probate court, it triggers a "psychiatric hold," which means that the patient can be detained for a specified period of time, usually 24 hours, until a designated individual (usually a psychiatrist) can perform a more complete diagnostic assessment to determine whether the pa-tient meets the state’s specified involuntary hospitalization criteria. If the physician then feels that the patient does not meet one of the statutory requirements, and the patient is unwilling to sign in voluntarily, the patient must be released from the hospital regardless of whether he/she has a mental illness that would benefit from inpatient treatment. Current laws are based on some historical atrocities committed in the asylums of yesteryear, and they strongly favor patients’ rights, sometimes to the significant impediment of treatment. For example, patients who meet involuntary admission criteria still are free to refuse all but emergent treatments. Thus, to involuntarily administer medication to these hospitalized patients, one must make another trip to the courthouse.
Suicidal Patients in the ED
In the United States alone, 25,000-50,000 people commit suicide each year with 20 times that number attempting it.18 Successfully identifying suicidal patients and getting them the help they need is obviously a public health priority. However, it is even more important to remind physicians of these sad statistics — more than 75% of suicidal patients will have seen a physician in the last three months and almost half within the weeks immediately before their action.19 The majority of successful suicides are completed with firearms; therefore, inquiries into the patient’s access to firearms must be documented.20
A patient should be considered suicidal if he is seen in the ED following an attempted suicide, complains spontaneously to staff of suicidal feelings, responds affirmatively when questioned about suicide during the interview, or demonstrates any suicidal behavior. It can be very difficult to distinguish between suicidal behavior and actions merely intended to communicate how unhappy the patient feels (i.e., chronic cutting or other self-injurious behavior). However, in the ED setting, remember that not all suicidal behavior is overt. Regardless of whether the patient claims it was an accident, all drug overdoses/ingestions, single-vehicle accidents, and self-inflicted trauma cases warrant a thorough evaluation for whether the patient is suicidal.21
Specifically asking about suicidal feelings will not increase an individual’s risk or cause the thought to exist if not already present. The assessment of an individual patient’s safety should focus on his risk factors for suicide as well as the existence of any mitigating/protective factors.
Table: Suicide Risk Factors
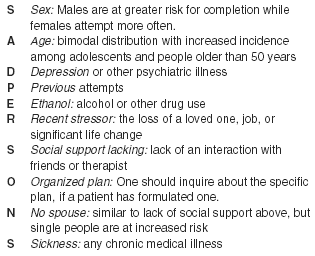
The acronym SAD PERSONS (see table above) should remind clinicians of the risk factors for suicide that should be assessed in any suicidal patient.22 The following factors may be considered somewhat protective in patients: Family members or friends are with the patient and able to monitor the patient closely (getting help if needed), an established relationship with a therapist or psychiatrist, and the attempt was in response to an acute stressor that has resolved subsequently.23 This risk-balancing inquiry is not an exact science that simply allows the examiner to add and subtract to arrive at a conclusion. Rather, one must make a Gestalt determination after reviewing all of the information, including collateral information from friends and family members. The following cases, regardless of findings of ultimate liability, represent tragic fact patterns against which to discuss some possible interventions that might have made a significant difference for all involved.
Case #4: No Liability for Suicide After ED Release
Although courts have imposed liability on EPs when a psychiatric patient commits suicide shortly after discharge, some courts have taken a different view. In Garcia v. Lifemark Hospitals of Florida,24 Ramon Garcia was evaluated in the ED following an overdose on numerous medications. Mr. Garcia recently had undergone a surgical fusion procedure, and Dr. Fernandez, the EP on duty, diagnosed Mr. Garcia as suffering from an accidental overdose. Apparently, the patient had ingested several over-the-counter medications. The EP ordered a gastric lavage, monitored the patient, and then subsequently discharged him home. Despite the history of overdose, Dr. Fernandez did not request a psychiatric consultation nor recommend any form of mental health follow-up.
Two days following his discharge, Mr. Garcia crashed his car into the concrete dividing wall near an exit ramp. After being extricated at the scene, he was transported to the same ED for evaluation, where a different EP evaluated him. In the middle of his work-up, Mr. Garcia asked to be released from the hospital. Dr. Pablo Alonso, the EP on duty that night, released Mr. Garcia after having him complete the against medical advice (AMA) paperwork. Following completion of the paperwork, the patient was discharged without any form of mental health assessment or follow-up. Shortly after returning home that evening, Mr. Garcia committed suicide.
The court stated that "[w]here a patient has surrendered himself to the custody, care, and treatment of a psychiatric hospital and its staff, liability may be predicated upon the hospital’s failure to take protective measures to prevent the patient from injuring himself."25 Mr. Garcia’s family members argued that the ED physicians had a legal duty to properly diagnose and treat all of his ailments, including his suicidal tendencies. The court disagreed and stated that given the fast-paced and often chaotic environment of EDs, a close physician-patient relationship is difficult. Accordingly, the ED physician’s job should be to treat the emergent condition that brought the patient to the hospital. The court also used a hypothetical example that indicated it was unlikely to impose any liability on ED physicians with respect to missed psychiatric diagnoses when it stated, "if a person goes to an ophthalmologist because he has an eye infection, one could hardly contend that there is a duty for the doctor to diagnose and treat the patient for hemorrhoids. Likewise, it is even more difficult to argue that this doctor has a duty to diagnose and treat that patient for obsessive-compulsive disorder. Imposing such a duty takes us down the path of clairvoyance."26 The court based its holding on the notion that psychiatry is different from other disciplines of medicine. It stated that the "outward manifestations of infectious diseases lend themselves to accurate and reliable diagnoses . . . [however] the internal workings of the human mind remain largely mysterious."27
Case #5: No Liability for Suicide After Transfer
Continuing with the theme of liability for suicide of patients following evaluation in the ED, the case of Jinkins v. Evangelical Hospitals Corp.28 stands for the principle that there are limits to an ED’s liability for a suicide completed after disposition. George Jinkins resided with his wife and several other family members in Chicago. Mr. Jinkins began to drink quite heavily, wear dirty clothes, and give away his possessions to strangers. This behavior occurred during a three- to four-month period until Mrs. Jinkins and the children finally moved out. One evening, neighbors found him laying face down in a muddy puddle. His pants were down by his ankles, and his underwear was stained as he was bleeding from his rectal area. A neighbor and Mr. Jinkins’ mother took him to Christ Hospital that evening for an evaluation and treatment.
Dr. Daniel Sachs was the emergency medicine resident on duty that evening who evaluated Mr. Jinkins. He noted that Mr. Jinkins had a blood alcohol level of 0.203 mg/dL, and his urine toxicology screen was positive for marijuana. The family and friends present reported that Mr. Jinkins had been walking intentionally in front of cars and making comments about death. Additionally, Mr. Jinkins’ mother said that he had been paranoid and would stand over her when she cooked to make sure the food was not poisoned. Dr. Sachs diagnosed him with acute psychosis with suicidal behavior; his treatment plan was to have him evaluated for a psychiatric admission. The social worker on duty completed an initial involuntary hold petition on Mr. Jinkins and arranged for his transfer to a psychiatric hospital, apparently for insurance reasons.
The Madden Center was selected by Christ Hospital as the psychiatric facility to which Mr. Jinkins would be transferred. However, this hospital had a policy of not accepting patients until their blood alcohol was below the legal limit. Accordingly, Mr. Jinkins was held in the Christ Hospital ED overnight, during which time he became agitated and received 10 mg haloperidol. He subsequently tried to escape from the hospital and was found outside a half-hour later. When his blood alcohol level had decreased, he was transferred by ambulance in full leather restraints from Christ’s ED to the Madden Center.
At the Madden Center, Dr. Choong Lee, a board-certified psychiatrist, examined Mr. Jinkins as part of the routine intake procedure. A licensed professional counselor at the Madden Center also examined Mr. Jinkins. Mr. Jinkins was calm and coherent and displayed no paranoid symptoms. Furthermore, he denied being suicidal or depressed. Dr. Lee reviewed the Christ Hospital paperwork and was aware of the positive toxicology screen. By this time, Mr. Jinkins’ wife had arrived and disputed the facts contained in the involuntary hold petition. Additionally, she insisted he was not suicidal and asked to be allowed to take him home. Dr. Lee diagnosed Mr. Jinkins as suffering from an alcohol-related disorder. Based on his clinical exam and Mr. Jinkins’ wife’s representations, Dr. Lee referred him to a community health center for outpatient treatment despite his continued denial of help. Mr. Jinkins left the Madden Center shortly thereafter with his wife and his mother. After arriving back at his home that morning, Mr. Jinkins shot himself in the head. Despite attempts to resuscitate him at Christ Hospital’s ED, Mr. Jinkins died.
As Mr. Jinkins’ administrator, his widow brought suit against Dr. Sachs and Christ Hospital, claiming that their negligence in treating her husband resulted in his death from suicide. Specifically, she alleged that their transfer to the outlying psychiatric hospital, which subsequently released him, was the proximate cause of his death. The trial court did not buy the argument and granted summary judgment for the defendant physicians and hospital. On appeal, the court held that the plaintiff’s expert failed to establish that the transfer was improper or proximately caused Mr. Jinkins’ death. The incontrovertible evidence was that the defendants felt Mr. Jinkins suffered from a psychiatric illness and posed a risk to himself from suicidal behavior. Accordingly, Dr. Sachs and Christ Hospital took steps to ensure that he was evaluated by a psychiatric facility. No one involved with Mr. Jinkins’ care at Christ Hospital anticipated that he would be released upon evaluation at the Madden Center. Thus, the Madden Center’s independent evaluation and Dr. Lee’s decision to release Mr. Jinkins constituted an intervening act and thus, absolved the defendants from liability for their care of Mr. Jinkins.
Discussion
The above cases were chosen specifically to illustrate some of the outer limits of physician liability stemming from patients who are released from the ED and subsequently commit suicide. However, some specific comments are warranted in an attempt to analyze the fact patterns and hopefully offer some anticipatory guidance to ED practitioners who may very well find themselves dealing with similar situations. With respect to Case #4, no prudent EP should rely on this case to justify his or her avoiding the assessment of suicide risk in a patient with substantial risk factors for suicide. The combination of three facts (the recent "accidental overdose," the single-car accident, and the bid to leave AMA) is substantial clinical evidence of dangerousness, enough to require inquiry and documentation of assessment for suicidality and dangerousness. The standard of care among EPs who are not mental health specialists dictates that at least a basic evaluation of suicidality be performed and documented in patients whose trauma suggests the possibility of self-harm. Although somewhat flattering to psychiatrists and other mental health professionals abilities, the court’s dicta that psychological assessments, like the workings of the mind, are too complex to expect that busy EPs will get it right should be viewed as insulting and extremely misguided. Surely, accurate psychiatric diagnosis and management is complex and time consuming, but a basic inquiry into a patient’s dangerousness to self or others is fairly straightforward and well within the standard of care of all physicians. The notion that suicide assessment is well within the standard of care of EPs is well supported by case law finding physicians liable for failing to protect the patients themselves or identifiable third parties.
Case #5 reassures us that documenting a satisfactory suicide evaluation and disposition provides sufficient protection against accusations of negligence or malpractice. It’s not enough to do the evaluation. Protect yourself with your pen. The ED staff correctly assessed the patient’s risks (as evidenced by his successful suicide) and arranged for a mental health assessment, resulting in the proper course of action, namely involuntary hospitalization. Unfortunately, the ultimate outcome was that the patient was released prematurely and went on to complete suicide. The take-home point is to involve mental health professionals whenever there is a question of risk and to document fully your reasons for whatever course of action you adopt. Al-though no system will be perfect, these two measures will go a long way to minimizing your medicolegal risk.
EMTALA
Under EMTALA, hospitals must provide appropriate medical screening exams to anyone who presents to the ED to determine whether an emergent medical condition exists, and the ED must act to stabilize any emergency medical conditions prior to discharging or transferring the patient to another facility. After countless lawsuits, the courts have made it clear that EMTALA was not intended to be a federal malpractice statute. Rather, its purpose was to "get patients into the system who might otherwise go untreated and be left without a remedy because traditional medical malpractice law affords no claim for failure to treat."29 The following case represents an interesting fact pattern giving rise to an EMTALA-related litigation. Although the final judgment was for the defendant health care providers, this should not be reassuring. Lawsuits, such as this one, represent a second bite at the apple; defendants also may be guilty of medical malpractice.
Case #6: Missed Psychiatric Drug Toxicity
The case of Jackson v. East Bay Hospital, et al,30 details the tragic story of a patient who died from a psychiatric drug toxicity, despite being evaluated in the ED three times in one week.
On April 2, Robert Jackson visited the Lake County Mental Health Department to see a psychiatrist. He previously had been evaluated and diagnosed with a psychotic disorder, borderline intellectual functioning, and pedophilia by an outside agency. Per its policy, Lake County instructed Mr. Jackson to obtain medical clearance from the Redbud Hospital ED prior to returning for psychiatric treatment.
At Redbud’s ED, a triage nurse took Mr. Jackson’s history (including his current medications and allergies) and then his vital signs. Mr. Jackson was complaining of hallucinations, dizziness, and general unsteadiness. Dr. Schug, the EP on duty, examined Mr. Jackson and ordered several laboratory studies. Based on his review of the chart, he was aware that Mr. Jackson was taking lorazepam and clomipramine (Anafranil). Following this review and based largely on his examination, he diagnosed Mr. Jackson as suffering from acute psychosis.
Redbud did not provide any psychiatric care; the unwritten policy of the ED was whenever a patient presented with a psychiatric complaint, the physicians would examine the patient to determine whether a coexisting medical condition existed. Assuming that the psychiatric diagnosis was the only medical problem, the patient would be referred to a psychiatrist or to a mental health facility for follow-up. Dr. Schug arranged for Lake County to follow up with Mr. Jackson as was intended originally. A Lake County em-ployee evaluated him following his discharge.
On April 4, Mr. Jackson returned to the Redbud ED. A triage nurse re-evaluated him and retook his history, medications, allergies, and vital signs. A different EP, Dr. Miguel Ollada, examined Mr. Jackson who was complaining of a sore throat, chest pain with respiration, and dry heaves. During the interview, it was recorded that Mr. Jackson was talking to himself. As part of his evaluation, Dr. Ollada performed a complete physical exam and ordered a battery of tests (including an electrocardiogram [ECG], urine drug screen, and an arterial blood gases measurement). As expected, the urine drug screen indicated that Mr. Jackson was taking his prescribed tricyclic antidepressant (TCA), clomipramine. Following this work-up, Mr. Jackson was diagnosed with chest contusions, hypertension, and psychosis. Dr. Ollada requested a psychiatric evaluation by Lake County Mental Health, which refused because he had been evaluated recently and found not to be suicidal. Accordingly, Dr. Ollada released Mr. Jackson and instructed him to follow up with Lake County in the morning.
At 3:45 a.m. on April 5, Mr. Jackson returned to the Redbud ED after his wife found him wandering in the middle of the road. A triage nurse repeated the initial assessment and Dr. Ollada, who still was on duty, performed another physical assessment.
Although he found Mr. Jackson to be very agitated, he denied any other physical symptoms and had a regular heartbeat. To sedate Mr. Jackson, he was given haloperidol and diphenhydramine. Dr. Ollada then contacted Lake County and advised them of Mr. Jackson’s condition.
Later that morning, a Lake County Mental Health crisis worker came to the ED and evaluated Mr. Jackson. The worker determined that he met the criteria for inpatient involuntary psychiatric admission. Following Lake County’s recommendation, Dr. Ollada then medically cleared Mr. Jackson for transfer to East Bay Hospital, which functioned almost exclusively as a psychiatric hospital. Dr. Ollada’s medical certification indicated that Mr. Jackson’s condition had stabilized and that a transfer to East Bay did not pose a risk to his condition.
At 9:15 a.m., Redbud transferred Mr. Jackson to East Bay Hospital where he was evaluated by a psychiatrist, Dr. Steele, who performed a psychiatric assessment but not a physical exam. Dr. Steele prescribed more haloperidol for Mr. Jackson. At approximately 2 p.m., the East Bay staff concluded that Mr. Jackson was so unable to control his own movements that he posed a danger to himself and others. During their attempts to control his behavior, Mr. Jackson went into cardiac arrest, and staff began to perform CPR. He was transported by ambulance to Brookside Hospital where he arrived at 2:30 p.m. However, despite resuscitation efforts, he was pronounced dead at 2:37 p.m. An autopsy determined that Mr. Jackson had died from a lethal cardiac arrhythmia caused by a toxic level of clomipramine.
Mr. Jackson’s widow and daughter brought suit against the treating hospitals and physicians claiming EMTALA violations. The district court granted summary judgment for the defendant health care providers, and the family appealed. They also filed a state based malpractice claim, which probably settled. (Editor’s note: If the parties at the trial court level settle the case after the appellate court decision, the final outcome is not made public.)
In upholding the trial court’s grant of summary judgment the appellate court noted that a screening exam does not have to be medically adequate to satisfy the statutory requirement. Mr. Jackson was seen by a triage nurse during each of his visits and was assessed by a physician who performed a physical exam and ordered tests. Accordingly, the court held his screening was similar to other patients presenting to the defendant hospitals, which satisfies the statutory requirement. Additionally, because the hospitals never detected the drug toxicity, under EMTALA they cannot be held liable for failure to stabilize this condition prior to transfer. The statutory requirement only applies to medical conditions actually discovered prior to transfer.
Discussion
This disastrous case provides us with another example of the danger of missing the diagnosis of delirium. A series of physicians overlooked the possibility of delirium and the probability of clomipramine toxicity (perhaps because clomipramine is not commonly used). Though ECG changes and arrhythmias are often a precursor to lethal toxicity by TCAs, the absence of those signs was not sufficient to rule out toxicity as an etiology of this man’s delirium.
Many drugs employed in the management of mental illness are prone to toxicity and therefore, require careful monitoring for both clinical toxidromes and blood levels. The mood stabilizers, such as divalproex sodium (Depakote) and lithium, several of the antiepileptic medications, and TCAs require monitoring. There has been an increased use of TCAs for conditions such as neuropathic or chronic pain. Psychiatric patients, like many elderly patients, may be unreliable in medication adherence or taking the proper amount. Psychiatric patients also may take numerous medications with frequent changes in doses and times, thereby making them more prone to medication errors. Therefore, the physician strongly should consider toxicity in any patient who reveals he is on a psychotherapeutic medication, or has access to one that may result in toxicity, or has a readily discernable blood level. Low-level measurements are useful to subsequently treating mental health professionals because they represent a possible cause for the patient’s presentation and also the solution. Low levels also provide evidence of medication nonadherence, an obstacle that needs to be identified and dealt with by the treating physicians. Finally, "accidental overdoses" of medications actually may be a sign of suicidal behavior; therefore, all patients with toxic levels need further assessment for this risk.
Conclusion
Many patients with mental illness rely on the ED for their primary care needs Given the sheer number of such patients, it is increasingly prudent to ensure that one’s ED has adequate policies and resources in place to deal with this burgeoning population. The physician’s thorough exam, appropriate referral to mental health services, and review of collateral information will serve as strong defenses to the claims of medical malpractice.
Endnotes
1. Taylor RB, David AK, Phillips DM, eds. Family Medicine: Principles and Practice. New York City: Springer-Verlag; 2003, p. 300.
2. Rake RB, ed. Textbook of Family Medicine. 6th ed. Philadelphia: WB Saunders; 2002, p. 1496.
3. For more information on the spectrum of psychotic disorders, see generally Diagnostic and Statistical Manual of Mental Disorders Fourth Edition Text Revision pages 297-345 (2000).
4. Knesper D, Riba M, Schwenk T, eds. Primary Care Psychiatry. Philadelphia: WB Saunders; 1997:45-46.
5. Brown v. Carolina Emergency Physicians, P.A., 560 S.E.2d 624 (2001).
6. Id. at 627.
7. Id. at 631.
8. Id. at 630.
9. Hodges v. State of Tennessee, No. W2001-01026-COA-R3-CV (Feb. 26, 2002).
10. Id. at 2.
11. Id. at 4.
12. Brown v. Christian Health Ministries, No. CIV. A. 97-0643 (Aug. 22, 1997).
13. Id. at 1.
14. Id. at 2 [quoting Correa v. Hospital San Francisco, 69 F.3d 1184 (1st Cir. 1995)].
15. Lesperance F, Frasure-Smith N, Talajic M. Five-year risk of cardiac mortality in relation to initial severity and one-year changes in depression symptoms after myocardial infarction. Circulation 2002;105:1049-1053.
16. Wulsin LR. Is depression a major risk factor for coronary disease? A systematic review of the epidemiologic evidence. Harv Rev Psychiatry 2004;12:79.
17. American College of Legal Medicine. Legal Medicine. 6th ed. New York City: Mosby; 2004, p. 651 (discussing the notion that this power stems from the inherent police power of the state and the doctrine of parens patriae).
18. Shaner R, ed. Psychiatry. 2nd ed. Philadelphia: Lippincott, Williams & Wilkins; 2000, p. 351.
19. Knesper, supra note 4.
20. Mago R, Certa KM, Markov R, et al, Suicide risk assessment: Questions that reveal what you really need to know. Curr Psychiatry 2004;3:13, 15.
21. Knesper, Supra note 4.
22. Seitz FC. Behavioral Medicine Made Ridiculously Simple. Miami: Medmaster; 1997, p. 63.
23. Mago, supra note 20.
24. Garcia v. Lifemark Hospitals of Florida, et al, 754 So. 2d 48 (1999).
25. Id. at 49.
26. Id. at 49.
27. Id. at 49.
28. Jinkins v. Evangelical Hospitals Corporation, 783 N.E.2d 123 (2002).
29. Bryan v. Rectors and Visitors of the University of Virginia, 95 F.3d 349, 351 (4th Cir. 1996).
30. Jackson v. East Bay Hospital, et al., 246 F.3d 1248 (9th Cir. 2001).
This issue discusses some of the pitfalls that may arise in the care of the psychiatric patient. The lessons learned may assist EPs and nurses in reducing their malpractice risk, but more importantly, assist them in providing a safe disposition for these patients.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
