Low-Carbohydrate Diets and Weight Loss
Part I of a series on diet and weight loss
By Dónal P. O’Mathúna
The incidence of obesity continues to rise in the United States and most of the developing world. Effective strategies for long-term weight reduction elude most, yet less than a quarter of those trying to lose weight adhere to the two well-established requirements: reduce caloric intake and increase exercise. Instead, Americans spend about $33 billion each year on weight-loss products and services.1 The Atkins diet is one of the most popular current approaches, with an estimated 20 million people worldwide embracing this low-carbohydrate diet.2 Dr. Robert C. Atkins’ book was on the New York Times bestsellers’ list for several years, though the same basic principles are used in other popular diets (the Zone, Carbohydrate Addict’s, and Sugar Busters diets).3 With so many people shunning carbohydrates and loading up on protein and fat, practitioners must be aware of recent studies so they can advise their patients.
Background
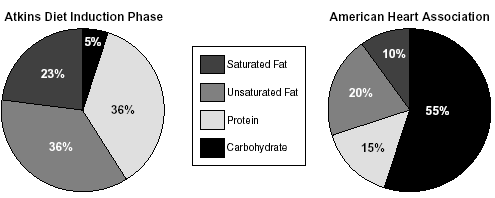
The Atkins diet advocates avoiding carbohydrates, initially recommending they constitute only 5% of one’s daily intake. People can eat unrestricted amounts of high-protein, high-fat foods, like meat, eggs, fish, cheese, olives, and nuts. After the initial two-week induction period, small amounts of complex carbohydrates are allowed (primarily vegetables and fruits), but breads, pastas, and starchy foods should be considered a thing of the past. The goal is to keep carbohydrate intake below 20 g/d.3
The Atkins diet flies in the face of the conventional low-fat approach to dieting. Dr. Atkins points out that while Americans have decreased their proportion of dietary fat from 40% to about 32%, obesity has become a pandemic.4 Atkins concludes that fat is not to blame. However, while the proportion has decreased, the actual per capita fat consumption has increased by 10 lbs/yr since 1975, and the consumption of simple carbohydrates (like sugar, syrup, and processed flour and rice) has increased per capita by 20 lbs/yr.5 A diet that adds even more fat seems questionable, especially in light of calls to reduce fat intake to promote cardiovascular health.
Mechanism of Action
A number of metabolic processes are believed to contribute to weight loss on low-carbohydrate diets.2 When carbohydrate consumption is severely restricted, glycogen stores are depleted along with associated bound water. Early weight loss may thus be due to fluid loss. Depletion of glycogen leads to ketotic acidosis, which may suppress appetite. Atkins claims that weight is lost because a high-protein, high-fat diet is thermogenic and requires increased energy expenditure. Evidence to support this is lacking, but even if significant thermogenesis occurs it is unlikely to cause more than very minimal weight loss. Protein’s greater satiating effect may also help people feel full quicker and for longer, thus making overeating and snacking less likely. In this way, the Atkins diet can be a low-calorie diet, though this is often not measured in studies because people are free to consume as much protein as they desire.
Clinical Studies
A systematic review of studies involving low-carbohydrate diets conducted prior to 2003 uncovered 94 trials.3 Of these, only 13 examined diets with the carbohydrate level recommended by Dr. Atkins (< 20 g/d). None of these trials lasted longer than 90 days and few included control groups. Weight loss was found to be associated with restricted caloric intake and study duration, but not with restricted carbohydrate intake.
During 2003 and 2004, four randomized controlled trials (RCTs) of the Atkins diet were published. The first assigned 53 obese women (mean BMI = 33.6 kg/m2) to either the Atkins diet or a calorie-restricted diet meeting the American Heart Association recommendations (see Figure).6 After six months, those on the Atkins diet lost more weight (8.5 vs. 3.9 kg; P < 0.001) and more body fat (4.8 vs. 2.0 kg; P < 0.01) compared to those on the low-fat diet. Mean levels of blood pressure, lipids, fasting glucose, and insulin improved in both groups over the course of the study, with no statistical differences between the groups at three or six months.
Figure
Comparison of Atkins diet induction phase and American Heart
Association recommendations
Another study randomly assigned 63 obese men and women (mean BMI = 34 kg/m2) to the Atkins diet or a conventional diet (high-carbohydrate, low-fat, low-calorie).7 Drop-out rate was high (41%) and not statistically different between the two diets. Those on the Atkins diet had significantly more weight loss at three months (6.8% vs. 2.7% body weight; P = 0.001) and six months (7.0% vs. 3.2% body weight; P = 0.02), but not after 12 months. Healthy changes in blood pressure and insulin sensitivity occurred in both groups and were not significantly different. Ketone levels were significantly elevated for those on the Atkins diet for only the first three months. No correlation was found between weight loss and ketosis.
Serum lipoprotein changes were more complicated. Total cholesterol and LDL levels initially increased for those on the Atkins diet, but had returned to baseline after 12 months. The levels initially decreased for those on the conventional diet, but were not significantly lower after 12 months. In contrast, total triglycerides and HDL-cholesterol levels remained unchanged on the conventional diet, while the Atkins diet led to significant lowering of total triglycerides and elevation of HDL levels (P < 0.05).
The research team in charge of the third RCT published separate reports after six8 and 12 months.9 Of 132 severely obese subjects (mean BMI = 43 kg/m2), 79 returned for six-month evaluations, and 87 were examined after 12 months. The low-carbohydrate diet restricted carbohydrate intake to 30 g/d with fruits and vegetables as recommended carbohydrate sources. After six months, weight loss was significantly greater for those on the low-carbohydrate diet compared to the conventional low-fat diet (5.8 vs. 1.9 kg; P = 0.002). At 12 months, however, the weight losses were no longer statistically different. Total triglyceride levels were significantly lower with the low-carbohydrate diet after six and 12 months. Cholesterol levels were not significantly different after six months, but after 12 months the HDL values were lower with both diets, with significantly greater reductions with the conventional diet (P = 0.028).
The most recent RCT involved 120 healthy subjects (mean BMI = 34 kg/m2) randomly assigned to either the Atkins diet or a conventional reduced-calorie diet.1 All participants were provided with a support group and exercise recommendations, and those on the Atkins diet also took the Atkins-recommended dietary supplements. One-third of the participants did not complete the study. After 24 weeks, weight-loss was greater on the Atkins diet (12.9% vs. 6.7% body weight; P < 0.001). The Atkins diet also led to significantly greater reduction in triglyceride levels (P = 0.004) and elevation of HDL levels (P = 0.001).
Adverse Effects
Concerns about the Atkins diet have centered around the high fat content and low plant and fiber content. Much of the additional protein comes from animal meats that are high in cholesterol. One study reported that the Atkins diet increased intake of cholesterol from 215 mg to 461 mg and then to 285 mg (at baseline, three months, and six months, respectively).6 These were significantly higher than those on the conventional diet: 273 mg, 169 mg, and 182 mg, respectively.
Studies have thus far reported improvements in some cardiovascular risk factors. The elevated HDL levels are sometimes cited as evidence of the Atkins diet being heart-healthy. However, elevated HDL levels can result from needing to remove additional cholesterol in the diet, and reduced HDL level can result from less cholesterol in the system. As Dean Ornish, a critic of the Atkins diet, put it, "Eating a stick of butter will raise HDL-C in those who are able to do so, but that does not mean that butter is good for the heart."5
The long-term effects of sticking with the Atkins diet are not well understood. Short-term adverse effects are less serious, but relatively common. One study funded by the Atkins Center found that among those using the Atkins diet for six months, 70% were constipated, 65% had halitosis, 54% had headaches, and 10% had hair loss.10 Reduced fruit, vegetable, and whole-grain consumption may explain these adverse effects.
Conclusion
Controlled studies of the Atkins diet support its greater effectiveness than a low-fat, reduced-calorie diet over six months, but not over 12 months. Such findings can be explained by the depletion of stored glycogen resulting in fluid loss, and the satiety effect of protein and ketosis. The resulting rapid weight loss, and the diet’s novelty, can be highly motivating. However, the big question is whether people can tolerate the high- protein diet over long periods—and whether it is safe, long term.
The improved lipid profiles found in RCTs are surprising given the large proportion of fat being consumed. However, even minor weight loss can markedly improve lipid profiles and glucose tolerance.2 In addition, the Atkins diet includes nutritional supplements that contain multivitamins and essential oils (flaxseed, borage seed, and fish oils; each 1,200 mg daily).1 Studies have not taken into account their use and impact on lipid profiles. Of great concern also is the long-term cardiovascular impact of consuming the high-fat, low-fiber diet.
Recommendation
Current evidence supports the use of low-carbohydrate diets like Atkins for short-term weight loss. Some risk factors for cardiovascular disease may also improve, but precisely how requires further research. Beyond six months, low-carbohydrate diets are no more effective than conventional, low-fat, reduced-calorie diets. Frequent constipation and headaches may lower compliance, resulting in one more "failed diet" that may discourage people from making necessary lifestyle and dietary changes. The long-term nutritional quality of low-carbohydrate diets, and their impact on long-term cardiovascular risk factors, remains a major concern.
Dr. O’Mathúna is a lecturer in Health Care Ethics at the School of Nursing, Dublin City University, Ireland.
References
1. Yancy WS, et al. A low-carbohydrate, ketogenic diet versus a low-fat diet to treat obesity and hyperlipidemia. Ann Intern Med 2004;140:769-777.
2. Astrup A, et al A. Atkins and other low-carbohydrate diets: Hoax or an effective tool for weight loss? Lancet 2004;364:897-899.
3. Bravata DM, et al. Efficacy and safety of low-carbohydrate diets: A systematic review. JAMA 2003;289: 1837-1850.
4. Stephenson J. Low-carb, low-fat diet gurus face off. JAMA 2003;289:1767-1768, 1773.
5. Ornish D. Was Dr. Atkins right? J Am Diet Assoc 2004;104:537-542.
6. Brehm BJ, et al. A randomized trial comparing a very low carbohydrate diet and a calorie-restricted low fat diet on body weight and cardiovascular risk factors in healthy women. J Clin Endocrinol Metab 2003;88: 1617-1623.
7. Foster GD, et al. A randomized trial of a low-carbohydrate diet for obesity. N Engl J Med 2003;348: 2082-2090.
8. Samaha FF, et al. A low-carbohydrate as compared with a low-fat diet in severe obesity. N Engl J Med 2003; 348:2074-2081.
9. Stern L, et al. The effects of low-carbohydrate versus conventional weight loss diets in severely obese adults: One-year follow-up of a randomized trial. Ann Intern Med 2004;140:778-785.
10. Westman EC, et al. Effect of 6-month adherence to a very low carbohydrate diet program. Am J Med 2002; 113:30-36.
O'Mathuna DP. Low-carbohydrate diets and weight loss. Altern Med Alert 2004;7(12):133-136.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
