A stepwise approach to outsourcing revenue cycle
A stepwise approach to outsourcing revenue cycle
By Elizabeth Guyton
Cap Gemini Ernst & Young
Atlanta
Health care organizations are discovering, as many industries have already learned, that thriving — even surviving — in a competitive marketplace means concentrating their talent and experience on what they do best, and offloading noncore services and administrative functions to vendors who can do them better, faster, and cheaper.
In principle, business process outsourcing is little different from sending out the hospital laundry. The difference is that outsourcing revenue-generating, mission-critical processes requires a much higher skill level, and a high level of collaboration and trust between customer and vendor. Such a partnership entails some risk and requires careful vendor selection.
Outsourcing revenue cycle processes is intended to improve cash flow and process effectiveness by introducing leading practices and eliminating activities that don’t add value. In processing accounts receivable, outsourcing can help to collect receivables sooner and reduce write-offs of bad debt.
By standardizing workflow and data collection, a knowledgeable vendor can help reduce errors in claims processing and improve efficiencies throughout the revenue cycle. Improving the timeliness and accuracy of initial claims, and shortening the turnaround time of any denials that still occur can further enhance cash flow.
Clinical integration processes can be improved, too. Knowledgeable personnel using state-of-the-art methodologies can improve the specificity, completeness, and consistency of all clinical documentation, including bills and insurance claims.
Outsourcers can consolidate the business office and support functions of multiple hospitals, departments, or acquired physician practices into a shared services model that provides more effective services at lower cost.
Outsourcing point-of-service functions can reduce the time patients spend in admitting and registration, and provide self-service capabilities, both of which dramatically improve patient satisfaction. Best of all, outsourcing the revenue cycle can accomplish all these benefits for substantially less money than health organizations spend today for support services that don’t perform as well.
An outsourcing vendor should be prepared to transform business processes as it takes on each new responsibility, and not merely take over existing processes and accomplish them with existing methods. For better results, an outsourcing vendor must possess the talent, expertise, comprehensive methodologies, and technological support to transform processes across the entire revenue cycle into leading practices.
This transformative approach is key to sustainable, high-value improvements in financial performance. Process transformation makes the difference between saving money through outsourcing and achieving market dominance through financial leadership.
Selecting an outsourcing vendor who can deliver maximum benefit to a health care organization’s bottom line must be a top priority. In general, the vendor of choice should have excellent references and extensive experience in both financial services and health care management. An outsourcing vendor should be able to show a long and consistent track record of helping health care clients improve their revenue cycle performance.
Cost should be considered, but the prospective customer should beware of companies trying to buy themselves into the growing and lucrative health care market. These companies, some with financial expertise in other industries, are willing to offer low prices for the privilege of gaining health care experience — usually at the provider’s expense. Here are some other criteria that should be considered:
• Focus on customer service
Outsourcing vendors who place emphasis on training and retaining a highly skilled staff make excellent business partners. These companies realize that satisfied, well-treated employees are likely to provide good customer service. Training costs can be applied to improving the knowledge and skill levels of employees who aren’t taking their expertise to better opportunities.
This customer-centered attitude reflects well on the health care provider. Patients appreciate helpful, competent assistance from a provider’s business office. Cumbersome admitting procedures, clerical errors, and unsatisfying interactions with "customer service" personnel are a prime cause of customer defections.
• Deep revenue cycle knowledge
It is vital for an outsourcing vendor to understand the processes and issues involved in fulfilling revenue cycle functions for health care providers, who operate from a much different business model from other enterprises. In addition to expertise in general accounts receivable management, a vendor must have deep knowledge of Medicare billing requirements, Blue Cross issues, local medical regulations, and regional billing methods. The vendor must be able to handle transactions with the local managed care payer and the federal government, with expertise in processing complex, detail-oriented forms, such as the UB 92.
• Resource availability
An outsourcing vendor should have sufficient and knowledgeable staff to handle its responsibilities effectively. Special skills that should be available include expertise in billing, collection and follow-up, accounts receivable analysis, and IT support.
• Appropriate management and client service infrastructure
Effective project management improves the collaboration between vendor and client. Having the right personnel and technologies dedicated to supporting each engagement facilitates greater improvement in financial performance.
• IT competence
Many health care organizations seek an outsourcing vendor to provide the IT expertise and state-of-the-art technologies they lack. For its part, the vendor must be familiar with the core business applications used by health care clients, notably ADT (admitting, discharge, and transfer) and PFS (patient financial services) systems. The vendor should have the capability to quickly and flexibly generate a wide variety of reports from its core information systems.
These reports are important tools for decision support. The vendor must also have experience with automated billing systems, and competency in workflow management and interface development.
• Overall understanding of provider issues
Expertise in revenue-cycle processes is not enough for an effective outsourcing relationship. Vendors should understand more general health care challenges, such as patient relations issues that can contribute to patient satisfaction and loyalty. Business office personnel also should understand how the integration of detailed, correctly coded clinical records benefits the patient at every point of contact.
Outsourcing is not an all-or-nothing proposition. Although the eventual goal may be to outsource the revenue cycle end-to-end, giving up control of revenue-generating processes has risks. To manage risk, many health care organizations first offload back-office functions such as billing, collection, denial management, and clinical documentation and coding, which require little or no patient interaction. (See figure below.)
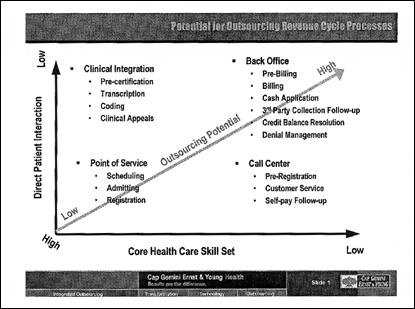
Many organizations achieve dramatic financial improvements at this limited stage of outsourcing. They find that the outsourcing vendor’s methods and personnel deliver significant improvements in cash flow, accounts receivable, and other financial metrics at lower cost.
Next, the provider may contract with the outsourcing vendor to establish a call center to handle direct patient interactions such as pre-registration, self-pay follow-up, and customer service requests. As the relationship matures and better processing methods become available, outsourcing has the potential to encompass the entire revenue cycle and all points of patient service.
An outsourcing vendor that can combine business process expertise with thorough knowledge of health care issues is a provider’s best guide to transforming the revenue cycle from a support service to a competitive advantage.
(Editor’s note: Elizabeth Guyton is a vice president in the health consulting practice of Cap Gemini Ernst & Young and leads the national revenue transformation service line. She has more than 20 years of health care management experience concentrating in the areas of accounts receivable and financial management.)
Health care organizations are discovering, as many industries have already learned, that thriving even surviving in a competitive marketplace means concentrating their talent and experience on what they do best, and offloading noncore services and administrative functions to vendors who can do them better, faster, and cheaper.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
