Grading Valve Regurgitation By Echo/Doppler
Abstract & Commentary
Synopsis: The Task Force on Valvular Regurgitation recommends the integration of several different techniques for evaluating the severity of native valvular regurgitation for echocardiography.
Source: Zoghbi WA, et al. J Am Soc Echocardiogr. 2003;16:777-802.
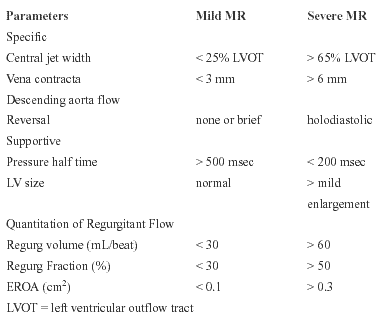
The Task Force on Valvular Regurgitation of the American Society of Echocardiography, in conjunction with the ACC, AHA, and ESC, has published recommendations for evaluating the severity of native valvular regurgitation by echocardiography. Unfortunately, the task force did not come up with a simple foolproof system, and certainly, one cannot rely on any one measurement or assessment technique. Instead, they recommended the integration of several different techniques. They recommend starting with the most specific signs (> 90% specificity) complemented by less specific but supportive signs. If this initial assessment indicates that the regurgitation is clearly mild, then nothing further is done. If not, quantitative measurements are recommended to determine whether the regurgitation is moderate or severe. They acknowledge the use of crossover categories such as mild to moderate and moderate to severe but don’t take a firm stand that this is necessary. Trivial is lumped in with mild and they don’t try to distinguish them. They describe the various assessment and measurement techniques in detail and point out technical issues and pitfalls of each. This is important because when all the techniques are congruent, the assessment of regurgitation severity is easy, but when they are not, considerable expertise and judgment is required to know which assessments are valid for establishing the correct severity. Also, they point out that blood pressure can affect the severity of regurgitation and recommend its measurement with an assessment of valvular regurgitation. (See the condensed versions of their Tables for grading the severity of mitral and aortic regurgitation as either mild or severe; everything else is moderate.) Tricuspid and pulmonic regurgitation are also covered in the recommendations but not shown here.
|
|
Comment by Michael H. Crawford, MD
This is an important step in extracting ourselves from the quagmire surrounding the estimation of valve regurgitation severity grading. I have personally seen several patients turned into cardiac cripples because valvular regurgitation, which would be graded as mild by these criteria, was called moderate to severe by well-meaning physicians. Some of the patients actually went on to have surgery because of symptoms that were not due to their mild valve disease. Although less frequently, I have seen severe regurgitation graded as moderate, which lead to an unnecessary delay in corrective surgery with the risk of irreparable left ventricular damage. Hopefully, these recommendations will push us to a higher standard in grading valvular regurgitation. However, this will only happen if echocardiographers find these recommendations helpful and actually use them. Unfortunately, they are not simple or easy, and most of them require some measurement to be made. Current reimbursement levels in echo don’t cover the costs of this intensive series of measurements in all patients with valvular regurgitation. Zoghbi and colleagues recognize this and suggest that the most time-consuming and technically demanding measurements of regurgitation should be reserved for the cases where the distinction between mild to moderate or severe was involved. The obviously mild cases wouldn’t require these more sophisticated measures. This makes sense and would probably eliminate measurements in two-thirds of patients. There are a few simple points that can be made from the recommendations. First, grading left heart regurgitation as severe requires left ventricular enlargement and also left atrial enlargement with mitral regurgitation, unless the regurgitation is acute. Of course, the left ventricle and left atrium can be enlarged for other reasons (eg, atrial fibrillation), so otherwise mild regurgitation isn’t automatically moderate or severe if the left heart chambers are enlarged. Second, grading mitral regurgitation requires an attempt to measure flow convergence since it is 1 of 3 highly specific measures. Unfortunately, it is not always technically possible, especially if the regurgitation is eccentric. Third, interrogation of more remote vessels, such as pulmonary veins in mitral regurgitation and the descending aorta in aortic regurgitation, is helpful for confirming grading. Finally, if blood pressure is high, the patient’s doctor should be contacted and advised to perform a repeat echo after it has been lowered to desirable range. I have seen left heart regurgitation decrease 1 full grade with therapy of hypertension. The 4 cardiology organizations are to be congratulated for tackling this difficult task; now it is up to the rest of us to implement their recommendations and start making some sense out of the morass we are in with valvulular regurgitation grading.
Dr. Crawford, Professor of Medicine, Associate Chief of Cardiology for Clinical Programs, University of California, San Francisco, is Editor of Clinical Cardiology Alert.
The Task Force on Valvular Regurgitation of the American Society of Echocardiography, in conjunction with the ACC, AHA, and ESC, has published recommendations for evaluating the severity of native valvular regurgitation by echocardiography. Unfortunately, the task force did not come up with a simple foolproof system.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.