Guest Column: A new season: Extending the 21/7 pill regimen

A new season: Extending the 21/7 pill regimen
By Robert A. Hatcher,
MD, MPH
Professor of Gynecology and
Obstetrics
Emory University School of
Medicine, Atlanta
Chairman, Contraceptive
Technology Update Advisory Board
Since 1960, women have been instructed to take 21 hormonally active pills followed by seven placebo pills (or seven days of taking no pill at all). Throughout the remainder of this commentary, this pattern will be referred to as 21/7, 21/7, 21/7. The one exception to this pattern is the pill marketed as Mircette (Organon, West Orange, NJ). After 21 hormonally active pills, a woman on Mircette takes no hormones for two days followed by five days of an estrogen-only pill with 10 mcg of ethinyl estradiol.
No pill has been marketed that has instructed a woman to take more than 21 consecutive pills that are hormonally active. The new pill, Seasonale (Barr Laboratories, Pomona, NY), under review by the Food and Drug Administration (FDA) at press time, will instruct women to take 84 consecutive pills, each with 30 mcg of ethinyl estradiol and 0.15 mg of levonorgestrel, followed by seven placebo pills. Four of these 91-day cycles will last 91 x 4, or 364 days (one day short of a year). Four times a year a woman will have a period, hence the name: Seasonale.
There are two types of combined oral contraceptive pills: monophasic pills, which provide exactly the same hormones every day, and phasic pills, where the strength of the hormones changes during the 21 days a hormonally active pill is taken.
Over the past 43 years, it has not escaped the attention of women and their clinicians that pills could be taken for more than 21 days. Usually, a monophasic pill has been chosen since the fluctuating level of hormones in triphasic pills, if taken for more than 21 days, can cause spotting or breakthrough bleeding. Continuous use of monophasic pills for more than 21 days started with women being treated for endometriosis.1
Break out of the box
The availability of an FDA-approved product designed to be taken 84/7, 84/7, 84/7 will validate the taking of pills continuously and markedly increase the continuous use of pills, much as the FDA approval of Preven (Gynetics, Belle Mead, NJ) and Plan B (Women’s Capital Corp., Washington, DC) increased use of combined pills as emergency contraceptive pills. The accompanying table outlines the different ways in which combined pills may be taken. (See Table 1, below.)
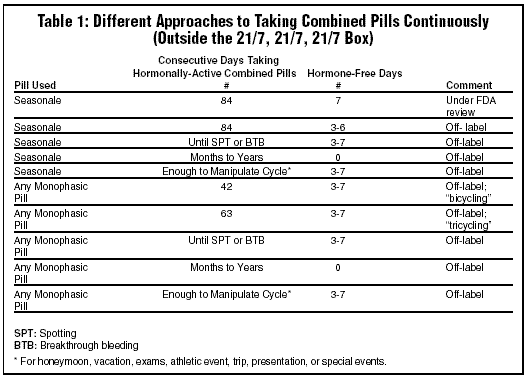
There still will be other variations. While any of the many monophasic-combined pills can be (and now are) used for more than 21 days, an FDA-approved product may quickly become the most commonly used pill to lengthen the number of days taking hormonally active pills.
In order to prescribe combined pills using FDA-approved instructions, we have been placed in a 21/7, 21/7, 21/7 "box" since 1960. Thinking outside this box has happened, but the availability of a pill labeled 84/7, 84/7, 84/7 is going to be important. The many ways of prescribing pills "outside the box" or outside of the "21/7, 21/7, 21/7 box" could be summarized this way: It means taking combined pills for any number of days beyond the usual 21 days. And it includes any number of hormone-free days from 0 to 7, but not more than seven hormone-free days.
Eye the pros and cons
What are the advantages of taking pills continuously?
- Convenience.
If a dedicated product is approved, there will be fewer packages of pills to obtain, open, and start on the correct day. With a continuous regimen, there are fewer days of bleeding and decreased expenditures for menstrual hygiene products.2
- Compliance.
The regimen is somewhat less complicated, and strict compliance may be somewhat less important.
- Increased ovulation
suppression.
Missed pills may be less likely to lead to ovulation and risk of pregnancy.3 This may be particularly beneficial for women with complicated lives.
- Benefit by certain
illnesses.
Women with endometriosis, porphyria, toxic shock, seizures or asthma, occurring exclusively premenstrually or exclusively during menses, may see relief.2,4,5
- Minimization of cyclic
symptoms.
Women who regularly experience one or more cyclic symptoms in the course of their menstrual cycles may benefit from the elimination of some or all cycles.2,4-6 (See Table 2, below.)
| Table
2. Cyclic Symptoms that May Improve in Women Taking Oral Contraceptives
Continuously
During Menstrual Phase
At Midcycle
During Premenstrual Phase
|
- Increased noncontraceptive
benefits.
Women on combined pills have been shown to have increased bone mass.7 Taking pills continuously may increase this noncontraceptive benefit.
Increasing a woman’s total exposure over time to combined pills may increase other documented noncontraceptive benefits of pills, such as the decreased risk for ovarian and endometrial cancer and improvement in acne.
What are the disadvantages of taking pills continuously?
- Unnatural.
Some women will not find the amenorrhea and irregularity of taking pills in one of the regimens described in Table 1 acceptable.
- Expense during pill
use.
Use of any of the currently available monophasic pills continuously necessitates purchasing more cycles of pills. The retail and public sector/HMO price of Seasonale remains to be seen.
- Expense if discontinued.
The purchasing of enough pills at a time for one-fourth of a year (Seasonale, under FDA review at press time) will cost much more than a single cycle of pills providing 21 combined pills. Should a woman discontinue the pills before completing a package, she may have spent $50 to $75 on unused pills.
- Additional counseling.
Since there are so many different regimens and so many different approaches to managing spotting, prescribing pills continuously will require careful counseling.
Review these advantages and disadvantages, and consider the patient for whom an extended regimen might be appropriate, including women who find such pill-taking easier to remember, those with busy lifestyles, and women seeking relief from cyclic symptoms. Taking pills continuously offers women and their clinicians an important new contraceptive option.
References
1. Kistner RW. Current status of the hormonal treatment of endometriosis. Clin Obstet Gynecol 1966; 9:271-292.
2. Miller L, Notter KM. Menstrual reduction with extended use of combination oral contraceptive pills: Randomized control trial. Obstet Gynecol 2001; 98:771-778.
3. Spona J, Elstein M, Feichtinger W, et al. Shorter pill-free interval in combined oral contraceptives decreases follicular development. Contraception 1996; 54:71-77.
4. Kaunitz AM. Menstruation: choosing whether . . . and when. Contraception 2000; 62:277-284.
5. Kwiecien M, Edelman A, Nichols MD, et al. Bleeding patterns and patient acceptability of standard or continuous dosing regimens of a low-dose oral contraceptive: A randomized trial. Contraception 2003; 67:9-13.
6. Sulak PJ, Scow RD, Preece C, et al. Hormone withdrawal systems in oral contraceptive users. Obstet Gynecol 2000; 95:261-266.
7. Berenson A, Radecki CM, Grady JJ, et al. A prospective, controlled study of the effects of hormone contraception on bone mineral density. Obstet Gynecol 2001; 98:576-582.
No birth control pill has been marketed that has instructed a woman to take more than 21 consecutive pills that are hormonally active. The new pill, Seasonale, under review by the Food and Drug Administration at press time, will instruct women to take 84 consecutive pills.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
