AHA is leading a hospital rebellion against OSHA’s tuberculosis mandate
AHA is leading a hospital rebellion against OSHA’s tuberculosis mandate
APIC: New Year’s Eve OSHA surprise disingenuous’
Charging that the Occupational Safety and Health Administration (OSHA) violated laws for regulatory review and comment, the American Hospital Association (AHA) is rallying opposition to recently mandated tuberculosis requirements that include annual respirator fit-testing.
"[We] encourage hospitals to ask OSHA to rescind the standard," says Rosalyn Schulman, senior associate director for policy at the AHA in Chicago. "We will be fighting it. At the same time, we will be letting hospitals know what the [requirements] are and what may occur if the standard is not rescinded. Ultimately, our main priority is getting this standard rescinded."
In dropping its hard-fought bid for a separate standard on tuberculosis, OSHA announced Dec. 31, 2003, that it will apply its existing general industry respiratory protection standards to health care facilities to protect workers from TB.1,2 For infection control professionals that means that annual respirator fit-testing for health care workers — a procedure many ICPs have protested is labor-intensive and unnecessary — will be required beginning in July 2004. OSHA announced the move as a fait accompli, saying no comment period would be allowed because the TB requirements were being added to an existing general respiratory standard. That 1998 standard had a comment period before it was enacted, and there was a comment period during the protracted battle for the doomed TB standard.
The AHA argued that the Occupational Safety and Health Act, which empowers OSHA to regulate workplaces, requires a determination — based on substantial evidence — that there is a significant health risk under existing conditions. The question of evidence, or lack thereof, appeared to be answered by OSHA withdrawing its proposal for a separate TB standard. "OSHA subsequently agreed that such evidence did not exist and that the agency’s proposed standard is unlikely to reduce the remaining health risk from TB," the AHA stated in a letter to OSHA. ". . . Our concern is that OSHA has now used selected information taken from this process to justify imposing something different than the proposed rule for which the data were originally gathered."
Legal action discussed
The decision to impose the new mandate cannot be issued as a final rule without the opportunity to review or provide public comment, the AHA argued. "This decision is a substantially different action than merely withdrawing the proposed TB standard," the AHA letter stated. "We strongly disagree with OSHA’s assertion that it has met the requirement to permit public comment during the comment period provided for the proposed TB standard. The decision to publish this mandate as a final rule violates OSHA law."
OSHA offered no rationale for instituting a new and costly respiratory protection standard against a disease that it acknowledged is declining and for which effective protective measures already exist, the AHA argued in the letter. (See TB chart below.) An OSHA spokesman would say only that the agency has received the AHA’s letter and will respond directly to the AHA.
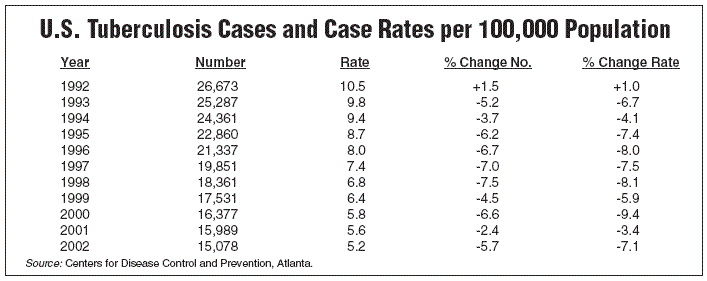
"TB has declined dramatically, including in health care settings," Schulman says. "With OSHA saying that hospitals are in substantial compliance with CDC [Center’s for Disease Control and Prevention] guidelines on tuberculosis, and having made a decision to withdraw the TB standard, it’s just counterintuitive. It doesn’t make sense to now apply among the strictest respiratory standards to TB."
The AHA, which represents some 5,000 hospitals nationwide, has discussed the possibility of legal action to block the requirement, she confirms. "We have had some discussions about that, but it is not far enough along that I can really comment on it. What we would like them to do is rescind the standard and then open it up for some discussion on the issue."
A fair question
OSHA critics find a troubling disconnect in the agency’s action. In withdrawing the TB standard, OSHA stated compellingly why its own regulation was not needed: "Hospitals, which are the settings where workers are likely to have the highest risk of exposure to TB bacteria, have come into substantial compliance with federal guidelines for preventing the transmission of TB," OSHA stated. "Overall reductions in TB mean that all workers are much less likely now to encounter infectious TB patients in the course of their jobs. [An] OSHA standard is unlikely to result in a meaningful reduction of disease transmission caused by contact with the most significant remaining source of occupational risk: exposure to individuals with undiagnosed and unsuspected TB."1
That reads like a page ripped out of an ICP’s testimony against the proposed TB standard, but then in the same issue of the Federal Register OSHA announced that while it was withdrawing the TB regulation it would include some of its requirements under the general respiratory standard.2 This move was heralded in an OSHA press release as "extending the same high level of respiratory protection to workers exposed to tuberculosis that is provided to workers throughout general industry. This enhancement results from OSHA’s decision to withdraw its 1997 proposal on tuberculosis."
The combination of the two actions raises a fair question: Why enhance TB protection for a worker group deemed "much less likely now to encounter infectious TB patients?" The Association for Professionals in Infection Control and Epidemiology (APIC) fired off a letter to OSHA telling the agency that its action was "disingenuous." APIC is urging infection control professionals to join a letter writing campaign to block the action. The APIC example letter ICPs are being provided to work from charges that "OSHA made this decision without allowing time for public comment. A good-faith effort would have involved issuing a specific proposal to apply the general industry respiratory protection standard to patients with possible TB infection."
Dear OSHA
"With the grass-roots letter effort, we are trying to let [OSHA] know the thoughts and opinions of the people who are doing this every day," says Patti Grant, RN, MS, CIC, an APIC member and infection control director at RHD Memorial Medical Center in Dallas. "At the bare minimum, there should be a comment period."
ICPs are responding to the call. "I will use that [letter] and encourage my colleagues to use it, too," says Jeanette Daniel, RN, CIC, infection control coordinator at Henrico Doctors’ Hospital in Richmond, VA. "I’ve shared the AHA letter with a lot of people, too."
In its formal letter to OSHA, APIC expressed concern that the agency "clearly ignored the fact that there is no scientific justification for this practice [annual fit-testing]. This information was presented at the time of those [TB and respiratory] rulemakings. In addition, regardless of the fact that information was gathered, it is disingenuous to later use only selected information as a justification for imposing something different than the rules for which they were originally gathered."
Another aspect of the agency’s action that has provoked a strong response was the timing of the announcement: New Year’s Eve. It does not take a conspiracy theorist to see the holiday timing as a way to head off initial resistance and criticism about an issue that has been highly controversial for almost a decade.
"I don’t recall any precedent quite like this," says Judene Bartley, MPH, MS, infection control consultant to the AHA. "It was really such an unexpected event that occurred literally on New Year’s Eve. It caught many of us by surprise that they would not only, on the one hand, withdraw the standard and, on the other, apply this general industry standard, which was designed with a very different scope."
The dynamics of exposure and transmission for biologic agents contrast dramatically with airborne chemical contaminants or particulate matter such as asbestos, the AHA argued.
"Biological organisms are transmitted differently than smoke and fumes and other agents for which the general industry standard was developed," Bartley says. "[Industrial agents] have actual thresholds and measurable percentages. We don’t have that for biological agents and that is not addressed in this current standard."
APIC’s letter to OSHA echoed those sentiments, noting that "health care facilities are not like marine terminals, long shoring and construction sites, that can pre-assess the potential for exposure and determine levels of contaminants."
Still, with severe acute respiratory syndrome and the threat of emerging infections, doesn’t it make sense to adopt the full regimen of OSHA requirements for particulate respirators? Bartley doesn’t buy that argument, noting that the vast majority of "airborne" pathogens are really transmitted by large droplet [i.e., influenza] and do not warrant use of N95 respirators.
Cost at what benefit?
OSHA estimated the total cost of compliance to be close to $12 million nationally, with more than 90% comprised of fit-testing and training expenditures for the N95 particulate respirators commonly used for TB protection. Still, the agency said the costs represent only 0.005% of the revenues of the affected establishments in the hospital sector. That figure seems a little more imposing when individual ICPs look at the impact on their systems.
For example, Daniel says her six-hospital system estimated previously it would cost $200,000 to refit test everybody to purchase new respirators. "We did that based on the number of employees we had and the number that would have to be fitted just to change a product, which would essentially be the same thing as refit testing everybody every year."
APIC argued in its letter that the OSHA’s estimates "grossly underestimate" the true costs. Fit-testing is extremely time-consuming, labor-intensive, and difficult to limit to small groups of workers. "Since TB patients can be any age and often have other underlying disorders requiring hospital care, the feasibility of limiting fit-testing to a nominal number of workers is neither practical nor in the best interest of patient care," APIC stated.
"Given the numbers of people that are hired, not just to do [fit-testing] initially but to do it annually, this is a major outlay of [resources] at a time when there are so many other constraints," Bartley says. "What benefits are we getting for that additional cost? There is no study that shows the efficacy of [annual] fit-testing in terms of providing a maximum benefit for the worker. These are the kind of issues we would like to see OSHA air in a more public forum, not under a mandate of the current [respiratory] standard."
References
- Department of Labor. Occupational Safety and Health Administration. Occupational exposure to tuberculosis, proposed rule; Termination of rulemaking respiratory protection for M. tuberculosis; final rule; revocation. Fed Reg 68:75767-75775 (Dec. 31, 2003).
- Department of Labor. Occupational Safety and Health Administration. Respiratory protection for M. Tuberculosis. Final rules. Fed Reg 68:75,776-75,780 (Dec. 31, 2003).
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
