Is it Normal or Abnormal? Approaching Neonates in the Emergency Department
Authors: Michael R. Osborne, MD, St. Vincent Mercy Medical Center, Department of Emergency Medicine, Toledo, OH; Catherine Marco, MD, FACEP, St. Vincent Mercy Medical Center, Department of Emergency Medicine, Toledo, OH.
Peer Reviewer: James E. Colletti, MD, Assistant Program Director, Mayo Emergency Medicine Residency, Department of Emergency Medicine, Department of Pediatrics, The Mayo Clinic, Rochester, MN.
Newborns—infants younger than 28 days of age—are particularly challenging to emergency medicine physicians. The inability to communicate directly with the patient, the lack of an established pattern of feeding and behavior, and the increased likelihood of congenital disease in this age group make a compulsive history, physical examination, and heightened awareness of the potential for underlying disease a mandate. Despite practitioners’ fear of missing something, the majority of these infants are normal. The most important tool for recognizing a newborn with a problem or potential problem is a strong foundation of knowledge about normal infant rashes, feeding patterns, and expected variations.
The authors review common newborn problems with an emphasis on normal variations and deviations that require a more thorough evaluation.—The Editor
Introduction
Newborn patients, age 0-28 days, comprise a significant fraction of all emergency department (ED) visits. Many emergency physicians are somewhat uncomfortable with this age group, due to a combination of factors that includes altered physiology, inability to obtain historical information from the patient, unreliable and challenging physical examination findings, and numerous other reasons. Common presenting complaints in this age group include jaundice, difficulty breathing, feeding problems, and irritability; the most frequent diagnoses include normal physiology, jaundice, feeding problems, and possible sepsis.1,2 An understanding of normal newborn anatomy, physiology, and behavior can be of great practical value in the safe and effective evaluation and treatment of newborn patients. Understanding the range of acceptable normal variation can help the ED physician in the recognition of more serious underlying pathology. Serious complaints, such as fever, lethargy, sepsis. cardiac disease, and apparent life-threatening events (ATLEs), are discussed in other issues.
Evaluation of the Neonate
Evaluation of the neonate can be particularly challenging. Neonates are unable to provide any history related to their chief complaints. Physical examination findings can be unreliable and variable. While evaluation of the overall appearance can be helpful, a well appearance does not rule out significant illness. Signs such as listlessness, poor feeding, and cyanosis are strongly suggestive of serious illness. However, a well-appearing neonate, even with a social smile, does exclude significant illness, including occult sepsis.
Vital Signs. Assessment of a newborn’s vital signs can provide vital clues to the health of a newborn. Normal body temperature in neonates is less than 38° C. Normal heart rate is 120-180 beats per minute. Normal respiratory rate is 30-60 breaths per minute. Normal blood pressure is 60/40 mmHg or higher. Typical weights are 3-4 kg.
Any fever greater than 100.5° F rectally is abnormal; elevated respiratory rates should suggest underlying respiratory or cardiac disease and elevated blood pressures should be repeated and, if hypertension is confirmed, the infant carefully assessed for underlying cardiac or renal disease.
Sleep Disturbances
As any parent of a newborn is acutely aware, sleeping patterns in the neonatal period are extremely unpredictable. Newborns typically sleep 18-22 hours per day; however, much to the chagrin of exhausted parents, those sleeping hours often do not occur reliably during the night hours. Many newborns lack day/night differentiation, and have sleeping and waking cycles throughout a 24-hour period. Newborn sleeping patterns are so erratic and unpredictable that nearly any sleeping pattern should be accepted as a normal variant. Sleeping patterns typically become more predictable by 2-3 months of age. Sleeping patterns can be influenced by feeding schedules, light, and caregiver preferences.3 Infants predisposed to sleeping disturbances at 12 weeks of age often can be identified by 1 week of age by a high number (greater than 11) of feedings per day, and those infants may demonstrate improved sleeping patterns through behavioral interventions such as maximizing the differences between day and night environments, and delaying nighttime feedings.4
Parents should be advised to place infants on their backs or sides, to reduce the possibility of sudden infant death syndrome (SIDS). Fluffy or overly soft mattresses and blankets should be avoided. Infants should not sleep in the same bed with other children or adults.
Crying/Fussiness
Crying is a normal newborn behavior, so natural and commonplace that the absence of crying is considered abnormal. Crying may be considered a form of communication regarding some unmet need or discomfort. However, crying in the neonatal period often has no discernable reason.
Understanding normal crying patterns is important in the evaluation of newborn fussiness. Crying patterns change with age. The typical newborn may cry for two hours per day, and crying tends to peak at 6 weeks of age.5 Newborns younger than 3 months have the highest frequency of crying, and cry on average of 2-3 hours per day.6-8 This decreases by approximately half by the time the child is 1 year of age. Crying often is at its height during afternoon and evening hours. However, there is considerable variation among infants, and an individual may not fit any discernable pattern yet be completely normal.
Excessive crying is a common complaint among parents of newborns. Crying and irritability are among the most common reasons for seeking medical attention in the first three months of life.9-11 Excessive crying may have detrimental effects on other family members, including sleep deprivation, frustration, feeding difficulties, anger, and child abuse. One interesting study from the United Kingdom estimates an annual cost to the national health system of $104 million related to evaluation and management of crying and sleeping difficulties.12 Excessive crying has numerous definitions in the medical literature; the use of different definitions affects which infants are included.13 Some commonly used definitions include persistent crying for more than three hours per day, inconsolability, level of parental concern, seeking of medical attention, and others.
Colic. Some use the term "colic" to refer to excessive crying in the first three months of life, attributed to unproven intestinal distress. Colic has been defined as paroxysms of crying for three hours per day or more for at least three days per week during a three-week period.14 However, there is considerable variation about the use of the term colic, its definition, and prevalence of the diagnosis. Because of the lack of evidence supporting colic as a specific defined diagnosis, many prefer more general descriptive terms (e.g., excessive crying, persistent crying, or paroxysmal fussing).15
Because of the tremendous variability in infant behavior, parental concerns regarding excessive crying should be taken seriously and investigated. However, physicians should be aware that often no specific organic etiology can be found.16-18 Numerous etiologies for excessive crying have been described, including occult infection, trauma (including child abuse), vaccinations,19 toxicities, congenital anomalies, hair tourniquet around a finger or toe, corneal abrasion, drug withdrawal, and a variety of acute medical and surgical conditions.11,20 Other diagnoses that should be considered include inguinal hernias, testicular torsion, and urinary tract infection.
History should be sought, including history of crying, feeding, sleeping, birth history, fever, cough, change in bowel habits, number of wet diapers, illness, and recent vaccinations. Physical examination should be performed while the infant is completely undressed, and should include general appearance, vital signs, and weight. A complete physical examination often reveals the source of crying.21 Particular attention should be paid to ruling out any evidence of trauma or acute medical illness. Interactions between infant and caregiver should be assessed. Ancillary tests should be considered when appropriate, including fluorescein staining of the eyes, urinalysis, skeletal radiographs, and computed tomography of the brain. Sepsis workup should be considered if fever is present or if sepsis otherwise is suspected. If history and physical examination do not reveal a source of distress or illness, several approaches may be recommended, including increasing physical contact, increasing feeding frequency during time periods prone to excessive crying, environmental changes (e.g., car rides, swings, or stroller walks), frequent burping, diaper changing, or changing formula preparations for bottle-fed infants. Parents should be referred back to their pediatrician for follow-up.
Dermatologic Complaints
Dermatologic complaints rather unique to the newborn population presenting to the ED include birthmarks, diaper rashes, and seborrheic and atopic dermatitis.22,23 The majority of these diagnoses are made in the newborn period. By the time the child is older and presents to the ED, the parents usually have consulted with a pediatrician, are aware of the diagnosis, and know specifically what complications are associated with the condition.
Brown birth marks include café-au-lait ("coffee with milk") brown spots and pigmented nevi. Café-au-lait spots usually are macular (flat) and appear to be light tan in color. They are sharply demarcated. Irregularly edged lesions are more likely to be malignant. Five or more lesions on one individual can be a marker for Von Recklinghouse Disease or neurofibromatosis, or McCune-Albright syndrome (polyostotic fibrous dysplasia).
Dark brown lesions usually are congenital melanocytic nevi and occur in 1-2% of the general population. Small lesions are of little concern. Large lesions are more likely to become malignant. Because of the potential for larger lesions to develop into melanoma, the parents should be referred to a dermatologist.
A special pigmented lesion present in a large number of infants of Asian descent, East African, American Indian, or Eskimo heritage is the Mongolian spot. It is seen in about 40% of Hispanics and up to 9% of Caucasians. The lesions are blue-gray spots of melanocytes, usually located over the sacrum, and may be multiple in number. Mongolian spots typically are present at birth and usually resolve by 4 years of age. Frequently, these lesions may be misinterpreted as a hematoma from suspected child abuse. A careful history taken should differentiate these spots from child abuse. These lesions usually have no clinical significance.
Vascular birthmarks are even more common than brown birthmarks (other than Mongolian spots). The flat version, or nevus flammeus, often is called a "stork bite" if on the back of the neck, or "angel kisses" or "temper spot" if on the forehead and upper eyelids. They have no medical significance and usually fade within a few months. A sharply demarcated, persistent, and often highly visible version of the nevus flammeus is the port wine stain. If this is found over the first branch of the trigeminal nerve (forehead), it may be an indication of Sturge-Webber syndrome.
Capillary hemangiomas are a form of vascular malformation. They start either at birth or shortly thereafter, usually grow until about the age of 1 year, then usually involute over the succeeding years. Fifty percent resolve by 5 years of age, and 90% by 9 years of age. Unless the location of the hemangioma causes a secondary problem, the best approach is to wait for resolution. Most hemangiomas are only cutaneous, but some patients also have internal hemangiomas in the lung, liver, gastrointestinal tract or central nervous system. In certain situations, these can be fatal — usually related to heart failure. The possibility of internal hemangiomas should be considered and investigated in any child with signs or symptoms of heart failure or hepatosplenomegaly and several of these lesions.
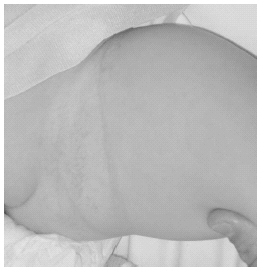
Diaper rashes come in two common forms — mechanical and secondarily infected skin (most commonly by yeast). Typical diaper dermatitis is a mechanical irritation of the skin by the wet soiled diaper. The skin folds generally are spared, as this is not where the diaper rubs. (See Figure 1.) It is more likely on the convex surfaces of the thigh, the mons, or the scrotum, and is typically erythematous and macerated. Hydrocortisone 1% ointment twice a day covered with a paste of zinc oxide paste with each medication dose and each diaper change for no more than one week should improve this condition rapidly. Frequent diaper changes or wearing no diaper at all also is recommended.
|
In the infant with diaper dermatitis, a secondary skin infection with Candida albicans is common. Candidiasis can be differentiated from mechanical irritation by two signs. First, the intriginous skin fold is red and macerated; and second, satellite lesions are present. Surrounding the zone of maceration in candidiasis are erythematous maculopapular lesions, areas of yeast infection not directly contiguous with the major excoriated area. Candidiasis responds well to topical antifungals, such as nystatin ointment, clotrimazole, or miconazole cream. The ointment is less irritating, as it is not alcohol-based. Zinc oxide paste is placed over the medication with each dose and with each diaper change.
Infantile seborrhea (cradle cap) commonly is seen in the neonatal period. Yellow, scaly, scalp plaques are characteristic of the diagnosis. Some parents are hesitant to remove the yellow waxy plaques, which can predispose to seborrhea. The child also may develop a facial rash, and the rash may extend to the entire body. Treatment consists of applying baby shampoo or baby oil to the lesions and leaving on for 30 minutes to soften the plaque, followed by shampooing vigorously enough to remove the plaque. Hydrocortisone 1% twice a day also may be used until the lesions are gone.
Eczema (atopic dermatitis) also commonly is seen in the neonatal period. Eczema tends to be recurrent, whereas seborrhea typically is not, if adequately treated. Infantile atopic eczema typically occurs on the flexor surfaces of the extremities, e.g., in skin folds of the elbows and behind the knees. Eczema tends to be more pruritic and typically develops after 3 months of age. The treatment of choice for atopic eczema is topical steroids, such as hydrocortisone 1% cream, twice a day (except on the face). Emollients, such as petroleum jelly or a hypoallergenic cream (such as Eucerin cream), can be placed over the hydrocortisone at night. Diphenhydramine may be administered at night for older infants, but typically is not recommended in the neonatal period. Avoiding irritating fabrics, heat exposure, and frequent bathing also may provide symptomatic relief.
Milia is another form of facial dermatitis commonly encountered in newborns. These are tiny, plugged hair follicles, also known as small epidermal inclusions cysts. Lesions are very small (1 mm or less in size), white papules. Milia are benign, and local hygiene with baby soap and a washcloth is usually all that is necessary for treatment.
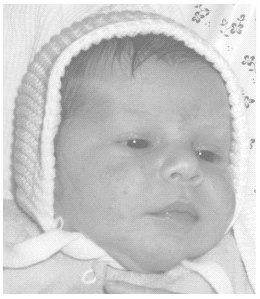
Neonatal acne occurs commonly in the first two weeks of life, related to maternal hormone shifts following delivery. (See Figure 2.) Neonatal acne typically resolves spontaneously following the normalization of the infants hormonal regulation, and no treatment is necessary. Over-the-counter acne preparations and overly aggressive cleansing should be avoided.
|
Molluscum contagiosum also may appear as white papules on the face or neck. The lesions of molluscum, a viral exanthem, have an umbilicated or depressed center.
Conjunctivitis
The most common cause of neonatal conjunctivitis is chemical irritation, which usually occurs in the first two days of life as a result of ocular prophylaxis. Silver nitrate is 2-12 times more likely to cause irritation than erythromycin or tetracycline. Maternal-fetal transmission of specific etiologic agents at delivery also may lead to conjunctivitis. The majority of these etiologic agents are sexually transmitted diseases. To prevent maternal-fetal transmission, silver nitrate 1% (AgNO3) commonly was used. However, because of local irritation and resultant chemical conjunctivitis, erythromycin 0.5% ointment (1 dose) now routinely is recommended. A second option is to use tetracycline 1% ointment in a single dose.
Gonorrhea conjunctivitis is a serious form of bacterial conjunctivitis, and typically results in hyperpurulent discharge occurring at days 2-4 of life. Patients with gonorrheal conjunctivitis typically should be admitted for antibiotics, eye irrigation, and management of potential complications, including corneal ulcerations, scarring, synechiae formation, and resultant sight impairment. All infants with suspected gonorrhea require a complete septic evaluation to exclude systemic disease. If there is evidence of systemic illness (disseminated disease), ceftriaxone 25-50 mg/kg IV is given daily for seven days.24 If the infant only has local eye disease, a single dose of ceftriaxone 25-50 mg/kg IM or IV may be given. The neonate is concomitantly empirically treated for Chlamydia trachomatis. The mother and her sex partner also are treated.
C. trachomatis usually presents on days 3-10 of life and may be diagnosed by antigen detection. Treatment with oral erythromycin syrup (50 mg/kg/day in four divided doses for 14 days) is recommended. No topical treatment is needed. Alternately, azithromycin syrup (20 mg/kg po daily for three days) has been shown to be effective.25 The mother and her sex partner also need to be treated.
Herpes simplex type 1 and type 2 also can be transmitted in utero or as the child passes through the birth canal, and usually presents on days 2-16 of life. All neonates with signs of eye involvement, or who have suspicious mucus membranes or skin findings, should have a flourescein exam, which typically demonstrates dendrites on the cornea if herpes is present. A complete septic evaluation should be obtained, and initiation of intravenous acyclovir is warranted. Topical ophthalmologic therapy is also used, Vidarabine ointment five times a day is used for up to 21 days. The ointment usually is better tolerated than drops. If the infant does not respond adequately, trifluridine (1 drop an hour 9 times a day for 21 days) can be used. Many cases (30-50%) will recur within two years.
After the first two weeks after birth, suppurative conjunctivitis from Staphylococcus aureus, Streptococcus pneumoniae, or Haemophilus influenzae may be more common. Empiric therapy with topical bacitracin-polymyxin B, trimethoprim (TMP), or erythromycin ointment should be instituted.
Respiratory Complaints
The normal respiratory rate for newborns is 30-60 breaths per minute, and from 1-6 months, 30-50 breaths per minute is considered normal. The first signs of pneumonia usually are tachypnea and tachycardia. As the disease progresses, the child may develop retractions and nasal flaring. Since the typical ill infant invests additional energy into the work of breathing, poor feeding may result. Agitation and irritability also may be seen. Because of smaller caliber airways in younger infants, difficulty in breathing may be exacerbated. A small amount of edema from inflammation can reduce the diameter of the opening of the airway dramatically in young infants.
Organisms causing respiratory infections in the newborn period differ from typical organisms seen in the older child. Maternal antibodies help protect the newborn in the first 30 days of life; as a result, S. pneumoniae and H. influenza are much less likely causative organisms. During the neonatal period, the organisms colonizing the respiratory tract are likely to have been transmitted during the birthing process. Listeria, which colonizes the female genital tract, not only is a causative agent in 7% of the cases of meningitis in infants under 1 month of age, but can also cause pneumonia. Group B streptococcus, Escherichia coli, S. aureus, Pseudomonas aeroginosa, C. trachomatis, and Treponema pallidum are other bacterial causes of pneumonia up to 1 month of age. Admission and empiric treatment with ampicillin and gentamicin or cefotaxime, is indicated. C. pneumonia is treated with erythromycin. Erythromycin in infants up to 6 weeks of age has been associated with increased incidence of hypertrophic pyloric stenosis. Any association with azithromycin and hypertrophic pyloric stenosis has not yet been defined.
In the 1-3-month age group, the child has not been vaccinated fully and maternal antibodies have waned. Organisms responsible for pneumonia is this age group include S. pneumoniae, Chlamydia, Bordetella pertussis (whooping cough), and S. aureus. If the child is suspected to have a bacterial etiology for the pneumonia, cefotaxime or ceftriaxone therapy may be initiated. Children with "blue" or apneic spells, oxygen requirement, poor oral intake, or poor follow-up should be admitted to the hospital. Erythromycin or azithromycin alone may be used for chlamydial or pertussis infections.
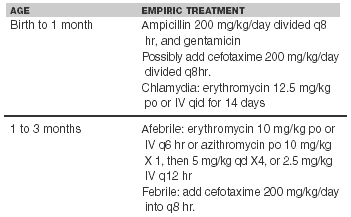
RSV (respiratory syncytial virus) and parainfluenza virus are the major viral etiologies of pneumonitis and bronchiolitis in this age group. These viral etiologies are more frequent in winter months and have been associated with both stridor and wheezing. In the 1-3-month-old age group with a nonfebrile community-acquired pneumonia, a macrolide such as azithromycin provides adequate antibiotic coverage.29,30 (See Table 1.)
|
Some physicians believe that with a diffuse appearing chest x-ray infiltrate and no fever azithromycin is the drug of choice; however, if the chest x-ray shows a lobar infiltrate more suggestive of S. pneumonia, then amoxicillin or cefotaxime is appropriate. In one study looking at community-acquired pneumonia treated with azithromycin in children as young as 1 month of age, the groups were divided prospectively into lobar type infiltrates and diffuse infiltrates. The azithromycin arm of the study did better than the erythromycin plus amoxicillin group for both typical lobar and vs. just erythromycin in the group with atypical diffuse infiltrates. By day 7, in those with classic pneumonia, 81% of the azithromycin group had normalized chest x-rays, vs. 61% of the erythromycin plus amoxicillin therapy group. For those with atypical pneumonia, by the 14th day 100% of the azithromycin treated group had a normal chest x-ray vs. 81% of the erythromycin group. These children were treated on an outpatient basis.29
Stridor in the newborn (younger than 1 month of age) is highly unusual and typically is associated with a congenital abnormality. Laryngomalacia is the most common diagnosis following consultation with a subspecialist and appropriate diagnostic testing. This is a structural problem caused by immature cartilage not adequately supporting the opening of the airway. Severe cases typically are diagnosed during the newborn’s initial hospital stay at birth. The most severe cases require surgical intervention to maintain the airway. The use of bronchodilators actually can worsen the symptoms of a child with laryngomalacia, as the muscular layer that holds the airway open can be relaxed by the bronchodilator, furthering the collapse. Other structural anomalies causing stridor in this age group include vocal cord paralysis, vascular ring, laryngeal web, or choanal atresia. Any child with stridor in the newborn period should be admitted for a thorough diagnostic evaluation to determine the etiology of the problem.
Bronchiolitis is a viral lower respiratory tract inflammation in infants, usually younger than 2 years of age. It is more common in winter months. Etiologies may include RSV, parainfluenza virus, adenovirus, and influenza virus. Wheezing and coarse rales may be present. Symptoms often come on slowly with a cough and upper respiratory infection symptoms. Grunting is an ominous sign of the infant trying to maintain an open airway with physiologic positive end-expiratory pressure. In older children, bronchiolitis may be difficult to differentiate from a true asthma exacerbation, though asthmatics usually have a history of allergic rhinitis, atopic dermatitis (eczema), or a family history of asthma.
The use of bronchodilators in bronchiolitis is controversial. Multiple trials spanning several years have demonstrated differing results. Most have not shown any benefit with the use of albuterol.31-37,40,42 Racemic epinephrine treatments have been more likely to show improvement.32,33,38 Part of the problem with the beta-agonist studies probably has been that nebulizing normal saline actually improves the respiratory scores as much as using the beta-agonist. A single study in 2003 tried the use of normal saline with epinephrine vs. 3% saline with epinephrine in hospitalized children with bronchiolitis and showed shorter hospital stays with the group given 3% saline and epinephrine.39 The use of steroids in bronchiolitis also is controversial.34,41,43
RSV is a major cause of bronchiolitis in the winter months. RSV bronchiolitis has been associated with apnea and death in children younger than 2 months of age, premature infants, and those with a history of apnea.44-46 The single strongest risk factor for developing apnea with RSV bronchiolitis in at least one study was age younger than 2 months. Other risk factors associated with apnea are bronchopulmonary dysplasia, congenital heart disease, cystic fibrosis or other respiratory diseases, or immunosuppression. The environmental exposures to passive smoke and daycare also increase the risk of severe RSV disease. Admission of all infants with RSV bronchiolitis would be warranted if younger than 2 months of age or with premature birth, complaint or history of apnea, with underlying cardiac or pulmonary disease, or with immunosuppression. Similarly, admit hypoxic or hypercarbic children; those who cannot be orally rehydrated or feed well; those with comorbid conditions; or those with parents or guardians who may be unable to provide adequate home care or follow-up care.
Feeding Issues
Feeding is a significant concern for both parents and physicians. Weight is a rapidly available test and a good measure of appropriate feeding. Small weight gains or losses may not be appreciated unless the same scale is used for serial weights. Newborns typically lose 5-10% of their birth weight in the first three days of life, primarily due to water loss. Birth weight is usually reattained by 10 days of age. After this time period, normal newborns would be expected to gain 20-30 g/day, and to double birth weight by 5 months of age.47
Feeding patterns are highly variable in the first month of life. Parents unnecessarily may be concerned about adequate nutritional intake based on excessive crying, fussiness, or perceived inadequate intake. Adequate feeding is best judged by appropriate weight gain. The strict adherence to breast milk or formula-only diet in the first 3-4 months of life should be emphasized.
Breastfeeding Issues. Breast milk is recommended by the American Academy of Family Physicians (AAFP), the U.S. Public Health Service (USPHS), and the American Academy of Pediatrics (AAP) as the ideal nutritional source for infants.48-50 Breastfeeding is associated with ideal nutrition, fewer feeding difficulties, and the less tangible benefits of strong maternal-infant bonding.51 Breastfeeding also is associated with a reduced incidence of otitis media, diarrheal illness, a variety of other infections, and decreased risk of childhood diseases such as diabetes mellitus, ulcerative colitis, and others.52,53
Adequate intake by breast-fed infants can be difficult to ascertain, due to the unknown volume of breast milk taken by the infant. Concerns about adequate nutrition are common, yet inadequate nutrition among strictly breast-fed infants is rare.53 Occasionally, infant factors can be associated with decreased intake, such as sleepiness, fussiness, difficulty with suckling, or infant illness. Adequate nutrition can be ascertained by appropriate weight gain, adequate number of wet diapers, post-prandial infant satisfaction (e.g., sleeping and reduced crying), assessment of maternal-infant bonding, and establishment of appropriate breastfeeding regimens. Frequency of feedings may be higher among breast-fed infants; many infants feed 8-10 times in a 24-hour period.
Maternal factors may be responsible for inadequate milk supply in some cases. If milk supply is considered potentially inadequate, maternal factors should be investigated, including fatigue, sore nipples, improperly fitted nursing brassiere, and inadequate caloric or fluid intake. Mastitis should be considered and treated with antibiotics, if present. Appropriate breastfeeding technique can be assessed by observation in the ED. In general, mothers who encounter difficulties with breastfeeding should be encouraged to continue breastfeeding and correct impediments to adequate milk supply and breastfeeding techniques, rather than switching to formula feedings. Access to breastfeeding consultants may be particularly helpful, especially for first-time mothers who are new to breastfeeding.
Formula Feeding. Formula-fed infants often require fewer feedings per day than breast-fed infants. A typical infant might require 6-10 feedings per day, consisting of 2-5 ounces per feeding. Three common types of formula exist, including cow’s milk-based formulas (e.g., Similac, Enfamil, Gerber, etc.), soy protein-based formulas (e.g., Isomil, Prosobee, etc.), and casein-hydrolysate-based formulas (e.g., Nutramigen, Alimentum, Progestimil, etc.). Typically, a cow’s milk-based formula is offered as first-line nutrition. If poorly tolerated, a soy-based formula or protein hydrolysate formula may be used. Iron-supplemented formulas are recommended by the AAP. Whole cow’s milk should not be used in the first year of life. Overfeeding bottle-fed infants can result in excessive crying and regurgitation. Observation of feeding and review of feeding schedule and amounts can be helpful in diagnosing overfeeding and instructing parents about appropriate schedules and volumes.
Underfeeding may be manifested by excessive crying, poor weight gain, poor sleeping habits, reduced number of wet diapers, and constipation. Overfeeding may be manifested by regurgitation, vomiting, excessive weight gain, abdominal distention, and flatulence.
In rare circumstances, significant congenital anomalies may present with feeding difficulties, including esophageal obstruction, congenital heart disease, or metabolic abnormalities. Infants with previously normal feeding patterns who develop a sudden decrease in intake should be evaluated for acute infection, cardiac disease, or other significant medical conditions.
Regurgitation. Regurgitation is a common reason for ED visits among neonates. Neonates have reduced lower esophageal sphincter pressure, and this may result in regurgitation, a result of gastrointestinal reflux. Regurgitation is nearly universal in the first six months, and decreases in frequency by age 12 months. Regurgitation can be a result of normal reflux, or may result from gastro-esophageal reflux disease.54 The infant should be assessed for appropriate weight gain. Feeding patterns should be established and overfeeding should be ruled out or addressed. Education about the importance of post-feeding burping in the upright position may be helpful to parents. Observation of feeding and regurgitation in the ED may be helpful in differentiating regurgitation from vomiting.
Vomiting, resulting from forceful contractions of the diaphragm and abdominal musculature, differs from the passive phenomenon of regurgitation. True vomiting is more worrisome, and infants should be assessed thoroughly through a complete history, physical examination, and diagnostic studies, as dictated by clinical suspicion. The physical examination should focus on the head shape and fontanelle (large head, split sutures, and full fontanelle suggest hydrocephalus); careful evaluation of the child’s heart (include femoral pulses and four extremity blood pressure to exclude a critical coarctation of the aorta); gentle examination of the abdomen for masses ("olive" of pyloric stenosis, hepatomegaly with metabolic diseases); and a thorough evaluation of the diaper area (examine testicles, check for hernias, and make sure anus is in correct position). In an infant with increasingly forceful nonbilious emesis, continual hunger, and a normal physical examination (or an "olive"), pyloric stenosis should be considered. A child with bilious emesis requires a thorough evaluation for obstructive diseases such as malrotation or volvulus. Other etiologies of vomiting should be considered, including child abuse, infections, urinary tract disease, and hepatobiliary disease. Infants should be assessed and treated for dehydration, and any child with an atypical history, exam, or who fails to thrive typically should be admitted for further evaluation and management.
Constipation
Constipation is a common complaint. Often, true constipation does not exist; the infant merely does not exhibit the frequency of bowel movements that is expected by the parents. Infants, particularly those who are breast fed, may not have bowel movements every day. It is normal for infants to draw their legs up to strain to have a bowel movement. Frequency is not the basis of the diagnosis of constipation, but rather the nature of the stool and difficulty of passing it.55 For example, straining lasting more than 10 minutes and associated with a hard bowel movement is consistent with constipation.
The key question is, when did the constipation start? Typically, the first meconium stool is passed within 24 hours of delivery; if this did not occur, a heightened awareness of possible structural defects should be considered. If a child is constipated, a gentle, digital rectal examination is warranted. Prior to a digital rectal examination, it is critical to be certain that the anus is in normal position and normal size. If the anus is in an atypical position, a surgical evaluation is appropriate. Congenital processes that may be associated with constipation include: meconium ileus (more common in children with cystic fibrosis), intestinal atresia or stenosis, or Hirshsprung’s congenital aganglionic megacolon. An infant with mechanical obstruction may have a distended abdomen with significant pain.
Infant botulism is a possible etiology of constipation. It usually is found in children younger than 1 year in age, who have been given honey by a caregiver. Presenting symptoms include lethargy and weakness. A careful history regarding honey often will lead to the diagnosis. Diagnosis is confirmed by isolating the organism or the toxin from the stool and electromyography (EMG) consistent with botulism. It is imperative to make the diagnosis prior to respiratory failure, which may ensue if untreated.58
Often, the cause of hard bowel movements is relative dehydration. For infants older than age 3 months, using baby juice (for example, pear or apple juice) twice a day may correct this. If this does not work, prune juice (½-1 ounce) may help. Older infants may improve by increasing amounts of fruits and vegetables in the diet. A glycerine suppository may be used as a temporary measure to ease passage of a particularly hard bowel movement.
Diarrhea
Loose stools are common in infants. Breast-fed babies have particularly soft, pasty bowel movements. About the 4th-6th day of life in breast-fed infants, the stool may contain mucus, and may appear loose and yellow-green. This lasts a few days, and then the stool changes to the typical soft, pasty bowel movement of breast-fed babies. When the change is made to cow’s milk, the infant may have an episode of transitional constipation.
True diarrhea is defined as greater than 10 grams of stool per kg in 24 hours. Not all loose stool is diarrhea. Causes of acute diarrhea include infectious etiologies (bacterial and viral); dietary etiologies, such as foods high in fructose or sorbitol; dietary intolerance such as to soy or milk, fruits, beans, etc.; and medication-induced, often related to antibiotics.59
Chronic diarrhea is defined as diarrhea lasting more than two weeks. Milk or soy allergy is possible, as is lactose intolerance. Other causes include short intestine, malrotation of the gut, IgA deficiency or combined immunodeficiency, celiac disease, bile salt malabsorption, Hirshsprung enterocolitis, and infection (as in acute diarrhea). Bacterial overgrowth and Clostridium difficile infection are possible after antibiotics. Diagnostic tests should include stool culture and examination for white blood cells. If antibiotics recently have been prescribed, C. difficile toxin should be ordered. A rapid assay for rotavirus (Rotazyme) can help with the diagnosis of viral gastroenteritis and help the parents understand that no antibiotic is indicated; however, it should be noted that rapid testing may be associated with false-positive reactions.
Most diarrhea may be tolerated, and the family should be encouraged to supplement with an oral electrolyte solution for 1-2 days. If the child appears ill, infectious causes should be investigated. Bacterial diarrhea usually is associated with increased stool white blood cells. If suspected, a stool culture and specimen to look for white cells is indicated. Signs of dehydration should be sought, including sunken fontanelle and eyes, dry mucus membranes, poor skin turgor, and delayed capillary refill. All children with evidence of dehydration should have active rehydration started in the ED. Rehydration should be instituted with intravenous fluid, 10-20 cc/kg, followed by reassessment of hydration status. If the child can tolerate oral rehydration (usually older than 3-6 months of age), this is preferred and is associated with less time in the ED. A parent or care-giver is assigned to give 5 cc of the electrolyte solution every five minutes for one hour.60 If this is tolerated, the amount may be increased to 10 cc every five minutes. If the child vomits, fluids should be withheld for 30 minutes. Vomiting three times may be considered failure of oral rehydration, and intravenous rehydration is warranted. Because neonates have lower reserves for hydration and nutritional status, a lower threshold for intravenous hydration and hospital admission and a search for underlying congenital abnormalities should be maintained for infants in the first 30 days of life.
Hospital admission should be considered for any child with dehydration younger than 2 months of age if the child remains unable to tolerate oral intake, if significant etiologies are suspected, or if caregivers are unable to provide adequate home care or follow-up care.
Umbilical Cord Concerns
Care of the umbilical cord is an important concern among parents of newborns. For first-time parents, it is an unfamiliar task and may be disconcerting. The umbilical cord may be predisposed to infection due to exposed, moist, necrotic tissue.61 Current recommendations include keeping the cord stump as dry as possible, including folding down the upper edge of the diaper. Opinions vary regarding the use of antiseptics for cord care. Although antiseptic cord care has been demonstrated to reduce infection and sepsis in underdeveloped countries, its role in developed countries is less clear. Institutions vary in their protocols for umbilical cord care. Various authors recommend chlorhexidine, salicylic sugar powder, povidone-iodine, hexachlorophene, triple dye, isopropyl alcohol, bacitracin, or local cleaning alone.62-64 One recent study demonstrated shorter time to cord separation, with no increase in infection rate, by using alcohol compared to triple dye.64 Another recent study demonstrated reduced infection and colonization when a triple dye/alcohol combination was used, compared to dry cord care.65
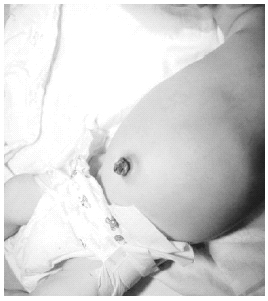
Omphalitis is a relatively rare but significant complication that may result from inadequate umbilical cord care. (See Figure 3.) It should be distinguished from the normal discharge that may be seen prior to stump detachment. Omphalitis may be manifest as foul-smelling, purulent discharge from the umbilical cord area, and may be associated with surrounding erythema. Systemic symptoms such as fever, lethargy, and irritability also may be seen. Omphalitis should be treated with systemic antibiotics and local cord care, and patients typically should be admitted for inpatient management.
|
Jaundice
Newborn jaundice is very common, and occurs clinically in 60% of neonates.67 Jaundice is typical in a newborn as the infant’s liver takes over the metabolism of bilirubin. Hyperbilirubinemia can be expected to peak at 3-5 days of age and improve by the 7th day in bottle-fed infants. Breast-fed infants may be jaundiced for 10-14 days. Preterm infants are more likely to become jaundiced and their brains are more prone to the deleterious effects of hyperbilirubinemia, so therapy is instituted at lower levels. Kernicterus is the dreaded complication if the hyperbilirubinemia is untreated.68 Individual infants may tolerate an elevated bilirubin differently, and toxicity may be seen at different levels among individuals. If there is evidence of neurologic involvement, even with a level that would not normally mandate treatment, phototherapy should be instituted on the basis of symptoms alone. Specifically, if the patient exhibits lethargy, vomiting, poor feeding, apnea, tachypnea, temperature instability, or excessive weight loss, phototherapy may be started. Other causes of jaundice should be ruled out, including sepsis, galactosemia, and G6PD deficiency.
Jaundice appearing after the first week is more ominous and may be associated with bacterial infections and sepsis.69,70 Because infants presenting with jaundice after the first week of life are at increased risk for occult bacteremia and sepsis, a septic workup should be undertaken. Urinary tract infection (UTI) is an important entity in the differential diagnosis of jaundice.71-73 UTIs are present in 7.5% of newly jaundiced afebrile, asymptomatic newborns presenting after the first week of life. Pyuria (5 white blood cells per high-powered field) may not be present reliably in newborns with UTIs. One study demonstrated that only 28% of infants younger than 16 weeks with documented UTI had pyuria, and 13% of all those with pyelonephritis by nuclear scan did not have pyuria.74
Phototherapy is indicated to produce a decline of the total serum bilirubin level of 1-2 mg/dL within 4-6 hrs. If the level does not decline appropriately, or the level does not remain low, failure of the phototherapy is apparent, and exchange transfusion may be warranted. Age of the infant and prematurity are important considerations regarding whether to institute phototherapy or exchange transfusion. The AAP, Provisional Committee for Quality Improvement, and Subcommittee on Hyperbilirubinemia published a consensus opinion on indications for management of hyperbilirubinemia. (See Table 2.)75
Conclusion
Newborns are a special group of patients with many unique aspects to their physiology. The accurate evaluation and management of a child in this age group requires a thorough understanding of normal physiology, normal variants, and developmental expectations, as well as the ability to recognize the sometimes subtle presentations of congenital abnormalities. In addition, the newborn does not handle infectious processes in the same manner as an older child and requires a complete septic evaluation for any febrile illness. Understanding normal variations and deviations is critical to the safe and effective evaluation and treatment of newborn patients.
References
1. McCollough M, Shareiff GQ. Common complaints in the first 30 days of life. Emerg Med Clin North Am 2002;20:27-48.
2. Millar, KR, Glorr GE, Wellington N, et al. Early neonatal presentations to the pediatric emergency department. Pediatr Emerg Care 2000;16:145-150.
3. Clemons RM. Issues in newborn care. Prim Care 2000;27:251-262.
4. Nikolopoulou M, St. James-Roberts I. Preventing sleeping problems in infants who are at risk of developing them. Arch Dis Child 2003; 88:108-111.
5. Reust CE. Diagnostic workup before diagnosing colic. Arch Fam Med 2000;9:282-283.
6. Long T. Excessive infantile crying: A review of the literature. J Child Health Care 2001;5:111-116.
7. Baildam EM, Hillier VF, Ward BS, et al. Duration and pattern of crying in the first year of life. Dev Med Child Neurol 1995;37:345.
8. Barr RG. The normal crying curve: What do we really know? Dev Med Child Neurol 1990;32:356.
9. Forsyth BW, Leventhal JM, McCarthy PL. Mothers’ perceptions of problems of feeding and crying behaviours. Am J Dis Child 1985;139:269-272.
10. St. James-Roberts I. Persistent infant crying. Arch Dis Childhood 1991;66:653-655.
11. Trocinski DR, Pearigen PD. The crying infant. Emerg Med Clin North Am 1998;16:895-910.
12. Morris S, St. James-Roberts I, Sleep J, et al. Economic evaluation of strategies for managing crying and sleeping problems. Arch Dis Child 2001;84:15-19.
13. Reijneveld SA, Brugman E, Hirasing RA. Excessive infant crying: The impact of varying definitions. Pediatrics 2001;108:893-897.
14. Wessel MA, Cobb JC, Jackson EB, et al. Paroxysmal fussing in infancy, sometimes called "colic." Pediatrics 1954;14:421-435.
15. Oberklaid F. Persistent crying in infancy: A persistent clinical conundrum. J Paediatr Child Health 2000;36:297-298.
16. Gormally S, Barr RG. Of clinical pies and clinical clues: Proposal for a clinical approach to complaints of early crying and colic. Amb Child Health 1997;3:137-153.
17. Poole S. The infant with acute, unexplained excessive crying. Pediatrics 1991;88:450-455.
18. Barr RG. Pediatrics 1998;102:1282-1286.
19. Blumberg DA, Lewis K, Mink CM, et al. Severe reactions associated with DPT vaccine: Detailed study of children with seizures, hypotonic-hyporesponsive episodes, high fevers, and persistent crying. Pediatrics 1993;91:1158.
20. Khan NS, Baka AG. Crying, fussy infant. In: Harwood-Nuss et al, eds. The Clinical Practice of Emergency Medicine Philadelphia: Lippincott Williams and Wilkins: 2001:1158-1160.
21. Poole SR. The infant with acute, unexplained, excessive crying. Pediatrics 1991;88:448.
22. Mallory SB. Neonatal skin disorders. Pediatr Clin North Am 1991; 38:745-761.
23. Edwards L. Dermatology in Emergency Care, 1st ed. London: Churchill Livingstone; 1997:281-288.
24. Gilbert D, Moellering R, Sande M, eds. Conjunctivitis. In: The Sanford Guide to Antimicrobial Therapy, 33rd ed. Hyde Park, VT: Antimicrobial Therapy, Inc.; 2003:8.
25. Hammerschlag, MR, Gelling M, Roblin PM, et al. Treatment of neonatal chlamydial conjunctivitis with azithromycin. Pediatr Infect Dis J 1998;17:1049-1050.
26. Gilbert D, Moellering R, Sande M, eds. Pneumonia. In: The Sanford Guide to Antimicrobial Therapy, 33rd ed. Hyde Park, VT: Antimicrobial Therapy, Inc.; 2003:25.
27. British Thoracic Society Standards of Care Committee, British Thoracic Society Guidelines for the Management of Community Acquired Pneumonia in Childhood. Thorax 2002;57:i1-24.
28. McIntosh K. Community acquired pneumonia in children. N Engl J Med 2002;346:429-437.
29. Kogan R, Martinez MA, Rubilar L, et al. Comparative randomized trial of azithromycin versus erythromycin and amoxicillin for treatment of community-acquired pneumonia in children. Pediatr Pulmonol 2003;35:91-98.
30. Roord J, Wolf BRM, Gossens M, et al. Prospective open randomized study comparing efficacies and safeties of a three-day course of azithromycin and a 10-day course of erythromycin in children with community-acquired acute lower respiratory tract infections. Antimicrob Agents Chemother 1996;40:2765-2768.
31. Dobson JV, Stephens-Groff SM, McMahon SR, et al. The use of albuterol in hospitalized infants with bronchiolitis. Pediatrics 1998; 101:361-368.
32. Patel H, Platt RW, Pekeles GS, et al. A randomized, controlled trial of the effectiveness of nebulized therapy with epinephrine compared with albuterol and saline in infants hospitalized for acute viral bronchiolitis. J Pediatr 2002;141:818-824.
33. Wainwright C, Altamirano L, Cheney M, et al. A multicenter, randomized, double-blind, controlled trial of nebulized epinephrine in infants with acute bronchiolitis. N Engl J Med 2003;349:27-35.
34. Berger I, Argaman Z, Schwartz SB, et al. Efficacy of corticosteroids in acute bronchiolitis: Short-term and long-term follow-up. Pediatr Pulmonol 1998;26:162-166.
35. Klassen TP, Rowe PC, Sutcliffe T, et al. Randomized trial of salbutamol in acute bronchiolitis. J Pediatr 1991;118:807-811.
36. Can D, Inan G, Yendur G, et al. Salbutamol or mist in acute bronchiolitis. Acta Paediatrics Jpn 1998;40:252-255.
37. Kellner JD, Ohlsson A, Gadomski AM, et al. Efficacy of bronchodilator therapy in bronchiolitis. A meta-analysis. Arch Pediatr Adol Med 1996;150:1166-1172.
38. Hariprakash S, Alexander J, Carroll W, et al. Randomized controlled trial of nebulized adrenaline in acute bronchiolitis. Pediatr Allergy Immunology 2003;14:134-139.
39. Mandelberg A, Tal G, Witzling M, et al. Nebulized 3% hypertonic saline solution in hospitalized infants with viral bronchiolitis. Chest 2003;123:481-487.
40. Totapally BR, Denercu C, Zureikat G, et al. Tidal breathing flow-volume loops in bronchiolitis in infancy: The effect of albuterol. Crit Care 2002;6:160-165.
41. Roosevelt G, Sheehan K, Grupp-Phelan J, et al. Dexamethasone in bronchiolitis: A randomized, controlled trial. Lancet 1996;348:292-295.
42. Schindler M. Do bronchodilators have an effect on bronchiolitis? Crit Care 2002;6:111-112.
43. Schuh S, Coates AL, Binnie R, et al. Efficacy of oral dexamethasone in outpatients with acute bronchiolitis. J Pediatrics 2002;140:27-32.
44. Church N, Anas NG, Hall CB, et al. Respiratory syncytial virus related apnea in infants. Demographics and outcome. Am J Dis Child 1984;138:247-250.
45. Aujard Y, Fauroux B. Risk factors for severe respiratory syncytial virus infection in infants. Respir Med 2002;96:S9-14.
46. Kneyber MC, Brandenburg AH, de Groot R, et al. Risk factors for respiratory syncytial virus associated apnoea. Eur J Pediatr 1998;157:331-335.
47. Mellis P. Assessment of the child in the emergency department: A practical application of normal child development. In: Tintinalli R, et al, eds. Emergency Medicine: A Comprehensive Study Guide. New York: McGraw-Hill; 2000:753-757.
48. Behrman RE, Kliegman RM, Jenson HB. Nelson Textbok of Pediatrics, 16th ed. Philadelphia: WB Saunders Company; 2001:149-166.
49. Public Health Service. Healthy People 2000: National health promotion and disease prevention objectives. Washington DC: Department of Health and Human Services. DHHS publication No. HRSA-M-CH-91-2, Public Health Service, 1990:379-380.
50. Spencer JP. Practical nutrition for the healthy term infant. Am Fam Phys 1996;54:138-144.
51. Zembo CT. Breastfeeding. Obstet Gyn Clin North Am 2002;29:51-76.
52. Hanson LA, Korotkova M. The role of breastfeeding in prevention of neonatal infection. Semin Neonatol 2002;7:275-281.
53. Wight NE. Management of common breastfeeding issues. Pediatr Clin North Am 2001;48:321-332.
54. Badriul H, Vandelplas Y. Gastro-oesophageal reflux in infancy. J Gastroenterol Hepatol 1999;14:13-19.
55. Behrman RE, Kliegman RM, Jenson HB. Nelson Textbok of Pediatrics, 16th ed. Philadelphia: WB Saunders Company; 2001:510-512.
56. Bhisitkul, DM, Listernick R, Shkolnik R, et al. Clinical application of ultrasonography in the diagnosis of intussusception. J Pediatrics 1992; 121:182-186.
57. Henrikson S, Blane CE, Koujok K, et al. The effect of screening sonography on the positive rate of enema for intussusception. Pediatr Radiol 2003;33:190-193.
58. Cox N, Hinkle R. Infant botulism. Am Fam Physician 2002;65: 1388-1392.
59. Schwartz MW, ed. The 5-Minute Pediatric Consult, 2nd ed. Philadelphia; Lippincott, Williams and Wilkins; 2000:25-26, 280-281.
60. Atherly-John YC, Cunningham SJ, Crain EF. A randomized trial of oral vs intravenous rehydration in a pediatric emergency department. Arch Pediatr Adolesc Med 2002;156:1240-1243.
61. Darmstadt GL, Dinulos JG. Neonatal skin care. Pediatr Clin N Amer 2000;47:757-768.
62. Pezzati M, Biagioli EC, Martelli E, et al. Umbilical cord care: The effect of eight different cord-care regimens on cord separation time and other outcomes. Biol Neonate 2002;81:38-44.
63. Zupan J, Garner P. Topical umbilical cord care at birth. Cochrane Database Syst Rev 2000;2:CD001057.
64. Dore S, Buchan D, Coulas S, et al. Alcohol versus natural drying for newborn cord care. J Obstet Gynecol Neonatal Nurs 1998;27:621-627.
65. Golombek SG, Brill PE, Salice AL. Randomized trial of alcohol versus triple dye for umbilical cord care. Clin Pediatr 2002;41:419-423.
66. Janssen PA, Selwood BL, Dobson ST, et al. To dye or not to dye: A randomized, clinical trial of a triple dye/aocohol regime versus dry cord care. Pediatrics 2003;111:15-20.
67. Kivlahan C, James EJP. The natural history of neonatal jaundice. Pediatrics 1984;74:364 -370.
68. Hansen TW. Kernicterus: An international perspective. Semin Neonatol 2002;7:103-109.
69. Chavalitdhamrong PO, Escobedo MB, Barton LL, et al. Hyperbilirubinemia and bacterial infection in the newborn. Arch Dis Child 1975; 50:650-654.
70. Rooney J, Hill DJ, Danks DM. Jaundice associated with bacterial infection in the newborn. Am J Dis Child 1971;122:39-41.
71. Garcia, FJ, Nager AL. Jaundice as an early diagnostic sign of urinary tract infection in infancy. Pediatrics 2002;109:846-851.
72. Dayan PS, Bennett J, Best R, et al. Test characteristics of the urine Gram stain in infants < 60 days of age with fever. Pediatr Emerg Care 2002;18:12-14.
73. Crain EF, Gershel JC. Urinary tract infections in febrile infants younger than 8 weeks of age. Pediatrics 1990;86:363-367.
74. Landau D, Turner MH, Brennan J, et al. The value of urinalysis in differentiating acute pyelonephritis from lower urinary tract infection in febrile infants. Pediatr Infect Dis J 1994;13:777-781.
75. American Academy of Pediatrics. Practice parameter: Management of hyperbilirubinemia in the healthy term newborn. Provisional Committee for Quality Improvement and Subcommittee on Hyperbilirubinemia. Pediatrics 1994;94:558-565.
Newbornsinfants younger than 28 days of ageare particularly challenging to emergency medicine physicians. The most important tool for recognizing a newborn with a problem or potential problem is a strong foundation of knowledge about normal infant rashes, feeding patterns, and expected variations. The authors review common newborn problems with an emphasis on normal variations and deviations that require a more thorough evaluation.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.