ECG Review: ‘Scoopies’ on ECG
By Ken Grauer, MD
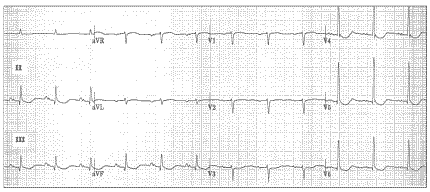
Figure. 12-lead ECG obtained from an older man on multiple medications.
Clinical Scenario: The ECG in the Figure was obtained from an older man on multiple medications. The patient was known to have longstanding cardiopulmonary disease and chronic renal failure, and he presented to the emergency department for an acute exacerbation of his underlying condition. He has chronic angina, but reports no recent change in his chest pain pattern. In view of this history, how would you interpret his 12-lead ECG? Which cardiac drug do you most strongly suspect he is taking?
Interpretation: The rhythm is sinus at a rate of just over 75 beats/minute. The PR, QRS, and QT intervals are all normal. Mean QRS axis is +70°. Left atrial enlargement (LAE) is suggested by the P-mitrale (notching) pattern seen in the inferior leads. QRS amplitude falls shy of criteria for left ventricular hypertrophy (LVH). Perhaps the most remarkable finding on this ECG is the scooped appearance (without QT prolongation) of the ST segment in multiple leads.
There are many potential causes of ST segment depression on a 12-lead ECG. Among the most important causes of ST depression to routinely consider whenever one notes this finding are: 1) "strain" (from ventricular hypertrophy); 2) ischemia (which could be chronic or acute); 3) rate-related (if tachycardia is present); 4) digoxin effect; and 5) hypokalemia/hypomagnesemia. In many cases, more than one of these factors will be operative, creating a combination effect on ST-T wave appearance. Clues to the specific etiology of the ST-T wave abnormality are sometimes forthcoming from morphologic appearance. Thus, symmetric T wave inversion is more suggestive of ischemia, whereas asymmetric ST segment depression is more suggestive of "strain." Morphologic appearance is subject to variation, however, and overlap of patterns is not uncommon. As a result, either symmetric or asymmetric ST-T wave depression may at times be due to the simultaneous presence of both ischemia and strain in the same patient. Clinical correlation and comparison with prior tracings are essential for accurate interpretation.
Patients who are taking the drug digoxin are likely to manifest one of three ECG patterns: 1) asymmetric ST segment depression that is very similar in appearance to that seen with "strain" from LVH; 2) a scooped appearance to the ST segment in multiple leads; or 3) no effect at all on ST-T wave appearance. The interesting clinical point is that the presence or absence of "dig effect" on the ST-T wave (patterns 1 or 2) is unrelated to the serum digoxin level, and that as many as one third of patients who are taking this drug manifest no ECG changes at all (pattern 3). Diffuse ST segment "scooping" of the type shown in the Figure strongly suggests that digoxin was among the medications that this patient was taking.
Dr. Grauer, Professor and Assistant Director, Family Practice Residency Program, University of Florida, Gainesville, is on the Editorial Board of Emergency Medicine Alert.
The ECG in the Figure was obtained from an older man on multiple medications. Which cardiac drug do you most strongly suspect he is taking?
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
