Special Feature: Techniques for Removing Nasal Foreign Bodies
Special Feature
Techniques for Removing Nasal Foreign Bodies
By Theodore C. Chan, MD, FACEP
Patients with foreign bodies in the nose commonly present to the emergency department (ED). These foreign bodies include a wide range of small objects limited only by the imagination, and include inanimate materials (e.g., toy parts, rocks, beads, paper, chalk, sponges, and batteries), vegetable matter (e.g., corn, peas, and nuts), and animate objects (e.g., worms, cockroaches, and other insects). Objects can be found in any portion of the nasal cavity, though most commonly on the floor below the inferior turbinate or immediately anterior to the middle turbinate.1 (See Figure 1.)
Figure 1. Common locations of foreign bodies,
and removal using a hooked probe
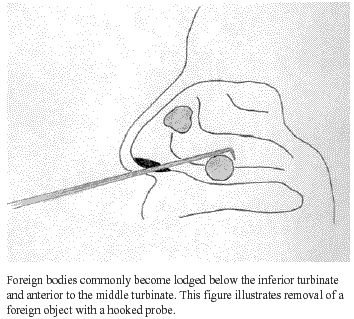 |
Patients typically are school-age children or younger, or developmentally delayed adults who insert objects into their noses out of curiosity and play. Adults and children alike may insert items in an attempt to relieve nasal irritation or epistaxis. On occasion, patients may not report any history of insertion or symptoms related to the foreign body. Incidental or occult objects have been reported in patients for prolonged periods of time.2
Patients commonly present with pain or discomfort associated with the foreign body, though this has been reported to occur in fewer than half of cases.3 In addition, unilateral, malodorous nasal discharge may be present and may be the only clue to the presence of a foreign body in occult cases. Other clinical manifestations are related to complications, including unilateral nasal obstruction, respiratory symptoms, epistaxis from trauma, and infection, including sinusitis. Rare complications include the development of rhinolith concretions from calcium and magnesium deposits, as well as erosion into contiguous structures such as the sinuses and soft palate.
Removal can be quite simple or present a significant challenge, depending on the type, size, location, and friability of the foreign body, as well as the age of the patient and his or her ability to cooperate with examination and removal.3,4 A variety of techniques and instruments have been used to remove foreign bodies from the nasal passages.
The emergency physician can remove most objects with little or no sedation (depending on the patient). Two large case series have reported successful removal rates of greater than 90% in the ED.5,6
More difficult cases generally should be referred to an ear-nose-throat (ENT) specialist for removal with an operating microscope. One key exception to this rule is the patient with a small button battery foreign body. In these cases, moisture within the orifice creates an electrolyte bath for the battery with the potential for creating an electrical current, hydroxide formation, and subsequent tissue electrolysis. In addition, leakage can cause liquefactive necrosis and significant organ injury.7,8 In these cases, immediate removal is necessary.
Another special circumstance occurs with myiasis, or the presence of animate objects (such as screw worms and larvae). This condition occurs more commonly in warm, tropical climates and areas with poor hygiene. In many cases, removal can be accomplished after first killing the offending insect (such as with chloroform solution), followed by more standard removal techniques including curettage, direct instrumentation, suction, and irrigation.
Removal Techniques
Direct Instrumentation. The most common removal technique for nasal foreign bodies is direct instrumentation by grasping the object anteriorly and removing it. Grasping instruments include alligator forceps, long bayonette forceps, and mosquito and hemostat clamps. This technique particularly is useful for solid, anteriorly placed objects. The object should be well-visualized prior to removal. Use of topical vasoconstrictors or anesthetics may aid both in visualization and removal. In addition, with smaller objects, an alligator forceps can be inserted through the otoscope head (by sliding the magnification window to the side) or through the nasal speculum, and removal performed under direct visualization. (See Figure 2.)
Figure 2. Removal of foreign object using alligator forceps
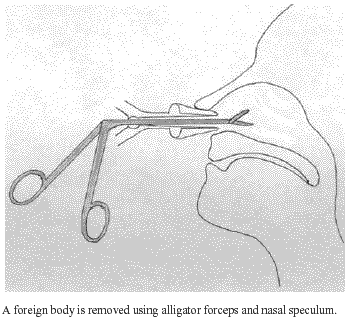 |
Complications from this technique include accidentally pushing the object posteriorly, increasing the risk for obstruction and aspiration. As such, this technique is less useful for large, smooth, round, and posteriorly situated objects. In addition, friable objects may be less amenable, as they could fall apart once grasped.
Hooked Probes. Another method of instrumentation involves the use of hooks (right-angle or curved), curettes, wire loops, or even molded paper clips to remove the foreign body. In this case, the probe tip is passed behind the object, turned such that the hook is now posterior to the object, and then pulled forward —with the object — out of the nares. (See Figure 1.)1,9 Objects must be located anteriorly and be small enough to allow the hook to pass behind it. In addition, friable objects may fall apart on removal. Complications include mucosal damage and bleeding from injury caused by the probe and object.
Balloon Catheters. Similarly, balloon catheters such as a small Foley (5, 6, or 8 F) or Fogarty catheter have been used to removal nasal foreign bodies.10 The deflated catheter is lubricated (2% lidocaine jelly) and inserted through the nasal cavity posteriorly past the foreign body. The balloon then is inflated with 0.5-2 cc of air or water. The catheter is withdrawn, pulling the object out of the nare with the balloon. A greater than 90% success rate has been reported, with no complications using this technique; it may be particularly useful for posteriorly placed objects.11 Potential complications are similar to those of the hooked probes, including tissue damage and epistaxis.
Suction. Suction catheters can be used to directly remove the foreign body. Most commonly, a Frazier tip or Schunkt-neck suction catheter is hooked up to 100-140 mmHg suction and directed at the foreign body for removal. Suction best is utilized for large, round, smooth objects that allow for a solid seal to be formed between the suction device tip and foreign body. Complications include tissue damage from instrumentation in the nasal cavity and inadvertently pushing the object posteriorly.3
Positive Pressure. A number of methods have been described to essentially blow the foreign body out of the nasal cavity. Forced exhalation can be utilized by cooperative patients and adults. In this technique, the patient is asked to take a deep breath in by mouth, then to forcefully exhale with the unaffected nostril occluded with lateral pressure. This forced exhalation of air out of the affected nare causes the object to be dispelled simultaneously. It is important that the unaffected nostril be occluded without causing septal deviation and occlusion of the affected side.
The mouth-to-mouth or "parent’s kiss" technique is a variant of this same idea that can be used on children. In this case, the caregiver or parent holds the supine child in his or her arms, stabilizing the chin and holding the mouth open with one hand and occluding the unaffected nostril with the fingers of the other hand. The caregiver forms a tight seal between his or her mouth and the child’s mouth (as if to give a kiss), and then promptly delivers a rapid, forceful puff of air into the child’s mouth. This action causes glottic closure and rapid expulsion of air out the affected nare, hopefully along with the object. Marked success has been reported with this technique.12,13 A similar technique has been described using a bag-valve-mask device in which the mask forms a seal only with the mouth of the patient. In this case, the bag then is used to deliver the forceful puff of air into the mouth.14
Positive pressure delivered through the unaffected nostril, rather than the mouth, also has been described. In this case, air pressure is delivered through a male-male oxygen tube adapter attached to oxygen at 10-15 L/min and inserted into the unaffected nostril. Air pressure from this device (termed a "Beamsley Blaster") is used to force the object out of the affected nare.15 All these positive pressure techniques are best suited for large, posterior foreign bodies that occlude the nasal passage, making them amenable to forceful exhalation. Theoretical complications include barotrauma, but no significant injuries have been reported thus far with these techniques.
Nasal Wash. A variant of the positive pressure techniques is the nasal wash. With this technique, the patient is seated upright with the neck in neutral position. A bulb syringe filled with approximately 7 mL of sterile normal saline is inserted into the unaffected nostril and advanced several centimeters until a tight seal is formed. The syringe is then forcibly squeezed and the object is propelled with the flow of saline out of the affected nostril. Small case series have reported excellent results (including with friable objects) with no complications.16 However, potential complications include risk of aspiration and reflux of saline and nasal contents into the Eustachian tubes and sinuses.17 Given these potential risks, this technique should not be performed on infants younger than 6 months old or those with airway or neurologic impairment. In addition, this type of irrigation should be avoided with batteries, as well as vegetative matter that might swell and expand.
Adhesives. Cyanoacrylate glue and tissue adhesive can be used to remove difficult foreign bodies from the nose.18 A small amount of the glue is placed on the cut surface of a hollow plastic swab stick or blunt end of a wooden cotton swab and placed directly on the object for 60 seconds. The stick and object then are removed gently from the nostril. This technique is best suited for solid objects that can be "glued" to the stick. Complications include glue adherence to the nasal mucosa and traumatic injury to the nasal cavity.
Dr. Chan, Associate Clinical Professor of Medicine, Emergency Medicine, University of California, San Diego, is on the Editorial Board of Emergency Medicine Alert.
References
1. Kalan A, et al. Foreign bodies in the nasal cavities: A comprehensive review of the aetiology, diagnostic pointers, and therapeutic measures. Postgrad Med J 2000;76:484.
2. Werman HA. Removal of foreign bodies of the nose. Emerg Med Clin North Am 1987;5:253.
3. Brown L, et al. A literature-based approach to the identification and management of pediatric foreign bodies. Pediatr Emerg Med Rep 2002;7:1.
4. Fritz S, et al. Foreign bodies of the external auditory canal. Emerg Med Clin North Am 1987;5:183.
5. Balbani APS, et al. Ear and nose foreign body removal in children. Int J Pediatr Otorhinolaryngol 1998;46:37.
6. Baker MD. Foreign bodies of the ears and nose in childhood. Pediatr Emerg Care 1987;3:67.
7. Capo JM, et al. Alakaline battery foreign bodies of the ear and nose. Arch Otolaryngol Head Neck Surg 1986; 112:562.
8. Kavanagh KT, et al. Miniature battery foreign bodies in the auditory and nasal cavities. JAMA 1986; 255:1470.
9. McMaster WC. Removal of foreign body from the nose. JAMA 1970;213:1905.
10. Kadish HA, et al. Removal of nasal foreign bodies in the pediatric population. Am J Emerg Med 1997;15:54.
11. Nandapalan V, et al. Removal of nasal foreign bodies with a Fogarty biliary balloon catheter. J Laryngol Otol 1994;108:758.
12. Backlin SA. Positive-pressure technique for nasal foreign body removal in children. Ann Emerg Med 1995; 25:554.
13. Guazzo E. Removal of foreign bodies from the nose. N Engl J Med 1985;312:725.
14. Finkelstein J. Oral ambu-bag insufflation to remove unilateral nasal foreign bodies. Am J Emerg Med 1996; 14:1.
15. Navitsky RC, et al. Nasal positive-pressure technique for nasal foreign body removal in children. Am J Emerg Med 2002;20:1.
16. Lichenstein R, et al. Nasal wash technique for nasal foreign body removal. Pediatr Emerg Care 2000;16:59.
17. Handler S. Nasal wash technique for nasal foreign body removal (letter). Pediatr Emerg Care 2000;16:307.
18. Hanson RM, et al. Cyanoacrylate-assisted foreign body removal from the ear and nose in children. J Paediatr Child Health 1994;30:77.
Continue your learning for free with our online CME courses on FreeCME. Create your account today to get started.
Patients with foreign bodies in the nose commonly present to the emergency department. Objects can be found in any portion of the nasal cavity, though most commonly on the floor below the inferior turbinate or immediately anterior to the middle turbinate.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
