For better worker health, bring those silos down
Collaborative model recommended
The term silos is used quite often in discussions about health care quality improvement, but perhaps not quite as frequently when it comes to occupational health. Changing that trend could lead to significant improvement in employee health, asserts Robin F. Foust, PAHM, president of Zoe Consulting Inc., a Catawba, SC-based occupational health consulting firm. What exactly are the silos in occupational health? "In an employer setting, they can include case management, disease management, disability management, the benefits department, and even the treating physician," she says.
The reason these silos can work against optimal treatment, Foust notes, is that none of the participants sees the big picture in terms of an individual patient’s health problems. "The various professionals all do their own thing from their particular focus and area of expertise," she explains. "There are people who are more expert than others in certain areas, like case management and disability management, but there seem to be opportunities lost if you do not coordinate with them and talk to each other about what is best for the patient. If you did coordinate, you’d get a better history, and therefore a better understanding of where the case has been going."
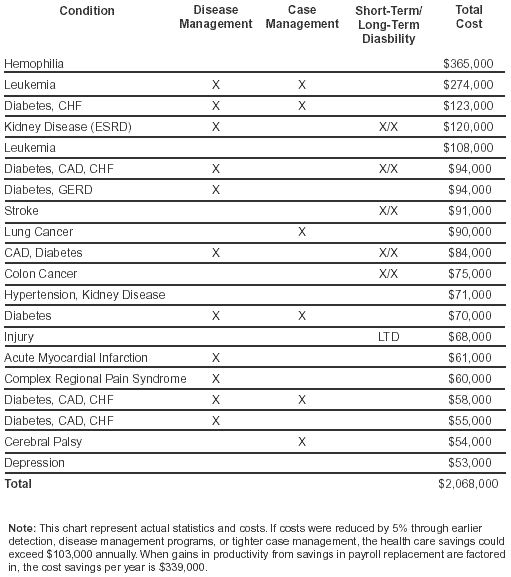
Based on data her company compiled, only between 20% and 40% of patients are being treated using a collaborative model. (See table.) "That means that 60%-80% of all sick or injured employees are being managed in a more silo-based approach," Foust asserts.
|
There are a number of different approaches to eliminating the silos in occupational health, she notes. "One of the most effective approaches I found was with an employer/client who actually brought the different organizations together where the case was openly discussed and data was shared," Foust says. "After the meeting, they all said, Why haven’t we done this before?’ It’s almost like they were just so focused in their own areas of expertise it never occurred to them; it just takes some enlightenment."
In the disease management world, she notes, people are collecting multiple assessments and monitoring them, "But they don’t necessarily share that data with the occ-health manager or the disability manager. They’re not really using those data, except for reporting purposes."
The ideal approach being hypothesized, says Foust, is the concierge or patient advocacy model, where there is one person coordinating all aspects of care with a centralized database. "However, I don’t think that will happen that soon," Foust laments. The next best approach, she says, would be to have within the system contact information for each of the key people at these various departments, and a notes section in your software for building other fields for their input on each case. This way, even if a case has already gotten farther than it perhaps should have, optimal health can be picked up at any given point.
"Let’s say you have a diabetic patient who ended up having an amputation," Foust says. "There’s a lot of history involved, and even if they were not in the diabetes management program before, you can encourage them to get into it now to prevent more complications and disability in the future. In other words, when patients are transferred from one area to another, sharing their history will help you realize what was provided previously, which can better inform your future treatment recommendations."
Driving the process
From an occupational health standpoint, the occ-health manager is the likely person to drive the coordination of care, and, if appropriate, to transfer a patient from one department to another, says Foust. "For example, a lot of disease management programs have lower back pain modules. If an employee has a lower back injury at work, the occ-health manager would work with them on a return-to-work program that could involve collaboration with the disease management program. So if there is long-term management of the injury involved, they can make sure they stay in that program."
Another big challenge in the collaboration model, she notes, is determining which silo the employee should enter. "It could be occ-health, it could be disease management; that’s why you need a central person to make that determination. They may be eligible for all of the available services."
Another important area to consider is the Health Insurance Portability and Accountability Act (HIPAA) — but that should not present an insurmountable problem, says Foust. "There are ways to make sure that the process is HIPAA-compliant; they just need to be taken into consideration as you bring the silos down," she says. "No one should share personal health information without following the proper procedures."
The bottom line, Foust concludes, is that by eliminating these silos, occupational health professionals "can ultimately achieve better outcomes for the patient and for the employer who is responsible for outcomes resulting from patient care."
[For more information, contact Robin F. Foust, PAHM, Zoe Consulting Inc., P.O. Box 258, Catawba, SC 29704. Telephone (803) 371-0774 (mobile); (803) 324-8626 (office); (803) 329-7819 (fax). E-mail: [email protected].]
The term silos is used quite often in discussions about health care quality improvement, but perhaps not quite as frequently when it comes to occupational health. Changing that trend could lead to significant improvement in employee health, asserts Robin F. Foust, PAHM, president of Zoe Consulting Inc., a Catawba, SC-based occupational health consulting firm.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.