E-mails to Improve Compliance to a Protocol
E-mails to Improve Compliance to a Protocol
Abstract & Commentary
Synopsis: Compliance with a protocol for managing catheter-related bacteremia was improved from 56% to 75% simply by sending a reminder by e-mail.
Source: Rijnders BJ, et al. Use of semiautomatic treatment advice to improve compliance with Infectious Diseases Society of America guidelines for treatment of intravascular catheter-related infection: A before-after study. Clin Infect Dis. 2003;37:980-983.
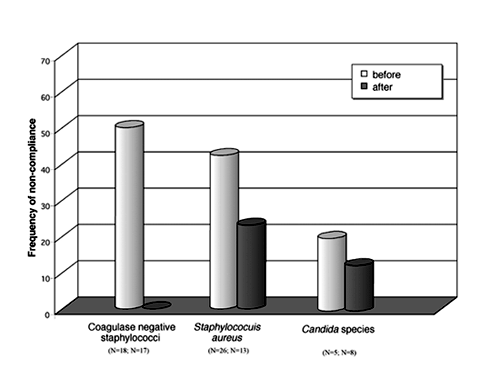
Designing protocols is one thing; keeping to the recommendations is quite another. This is shown clearly in this study of episodes of catheter-related bacteremia (CRB). The protocol was based on recommendations of the Infectious Diseases Society of America1 and provided advice on the antibiotic, dosage, and duration for a particular infection (see Table). The behavior of physicians familiar with the protocol in question was monitored for 8 months to assess their compliance in managing 52 episodes of CRB. It was not impressive, with noncompliance being recorded at 20%, 40%, and 50% for Candida infections, Staphylococcus aureus infections, and coagulase-negative staphylococcal infections, respectively (see Figure). A second phase lasting 7 months was then initiated in which the attending physician received standardized advice by e-mail accompanied by a printout that was placed on the physician’s desk. Compliance improved dramatically when dealing with CRB due to coagulase-negative staphylococci and moderately when dealing with other infections. Rijnders and associates conclude that their simple intervention was successful in bringing compliance up to 85%.
|
Table |
|||
| Criteria Used to Judge Whether Treatment of CRB was Adequate | |||
| Pathogen & Susceptibility | Recommended Antibiotic | Acceptable Dosage | Acceptable Duration |
| Coagulase-negative staphylococci | |||
| Methicillin susceptible | Flucloxacillin | 1-2 g/d | 5-10 d |
| Methicillin resistant | Vancomycin | Serum levels | 5-10 d |
| Staphylococcus aureus | |||
| Methicillin susceptible | Flucloxacillin | 1-2 g/d | 12-16 d |
| Methicillin resistant | Vancomycin | Serum levels | 12-16d |
| Candida species | Fluconazole | 400 mg/d | 14-16 d |
|
Comment by J. Peter Donnelly, PhD
The provision of a simple reminder obviously assisted these particular physicians in managing CRBs, which is encouraging as the system was neither costly nor labor-intensive, consuming less than 10 minutes of laboratory time. Moreover, Rijnders et al estimated that they only needed to send a reminder once a day in their 1700-bed hospital, which is hardly likely to place an intolerable burden on laboratory time. Importantly, their hospital uses an electronic medical record system so the physician encounters the recommendation as part of the routine tasks. The antibiotic formulary is also available online, making access to antibiotic information readily accessible. Interestingly, Rijnders et al did more than just send an e-mail; they also placed the reminder on the physician’s desk to ensure he or she got the message. This double security does rather suggest the electronic system is not foolproof. This is not surprising since the physician nominally in charge may not be the one who is caring for the patient on a day-to-day basis. The system will therefore only be as good as the level of communication within and between departments. This aspect deserves specific study since it is seldom clear why communications break down as they frequently do. The ready availability of PDAs also seems to offer more possibilities for exchanging information between people and systems.
There are grounds for caution with this attractive and simple approach. First, human beings are prone to suffer from information fatigue and overload. This might be avoided by ensuring that the delivery of electronic advice about a specific problem in a specific patient is incorporated into the process of managing the patient. For instance, if the electronic dossier is consulted before doing daily ward rounds, the advice should be available then so that it can be implemented. There is little point in sending the advice out after this time since it might cause confusion if treatment has already been agreed and has to be changed again later on in the day and may even be left until the day after. The approach is also not a substitute for consultation with infectious disease physicians or clinical microbiologists but complementary. However, with this in mind, the study does show a novel way of ensuring compliance to protocols that everyone has agreed to implement. This cannot be a bad thing and might be extended to other settings where protocols form an appropriate part of the care.
Dr. Donnelly is Clinical Microbiologist University Hospital Nijmegen, The Netherlands Section Editor, Microbiology
Reference
1. Mermel LA, et al. Clin Infect Dis. 2001;32:1249-1272.
Compliance with a protocol for managing catheter-related bacteremia was improved from 56% to 75% simply by sending a reminder by e-mail.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.