Which Patients with S aureus Bacteremia Are at Risk for Serious Disease?
Which Patients with S aureus Bacteremia Are at Risk for Serious Disease?
Abstract & Commentary
Synopsis: By determining whether 4 key risk factors are present, clinicians might be able to identify those patients with S aureus bacteremia who are at increased risk of serious, "complicated" infection.
Source: Fowler VG Jr., et al. Clinical identifiers of complicated Staphylococcus aureus bacteremia. Arch Intern Med. 2003; 163:2066-2072.
This study, performed by Fowler and associates at Duke University Medical Center, attempted to identify whether certain easily discernible demographic, clinical, and laboratory features could predict which patients with Staphylococcus aureus bacteremia are at risk of developing some of the most serious complications of the infection. Endocarditis, osteomyelitis and septic arthritis, and visceral or brain abscess are some of the dreaded complications of this infection.
All patients hospitalized with S aureus bacteremia over a 5-year period were studied. Excluded were those with polymicrobial bacteremia (blood cultures yielding more than 1 pathogen), patients younger than 18 years of age, and patients with peripheral white blood cell counts < 1,000/µL. Fowler et al collected data during the patients’ hospitalization and for a 12-week follow-up period, specifically noting the presence of "complications": 1) death attributed to staphylococcal infection; 2) hematogenously seeded infection (such as osteomyelitis); 3) local extension of infection beyond the primary focus (such as septic thrombophlebitis or abscess); 4) embolic stroke; and 5) recurrent staphylococcal infection during the follow-up period. Uncomplicated bacteremia was defined by absence of complicated or recurrent infection.
Follow-up blood cultures were drawn 48-96 hours after the initial set of positive blood cultures in most patients (79%, or 571 of the 724 enrolled in the study). Community-acquired bacteremia was present in 17%.
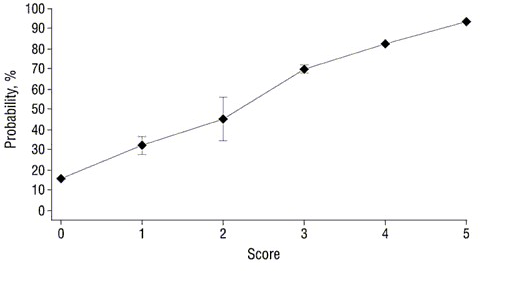
Using a host of such variables as demographic characteristics, clinical findings, and treatment modalities, Fowler et al developed logistic regression models to predict the presence of complicated S aureus bacteremia. Of the 40 variables that were examined, positive follow-up blood culture (odds ratio [OR], 4.94), community-acquired bacteremia (OR, 3.08), and fever persisting at least 72 hours after the initial blood culture (OR, 2.00) were the most significant predictors. Cutaneous markers of systemic infection (eg, petechiae, infarcts, and vasculitis), residence on a surgical service, advanced age, presence of a new or diastolic murmur, and the presence of a prosthetic device were also significantly associated with complicated infection but to a lesser degree. Refinement of the statistical model again identified 4 of these factors as the most predictive: positive follow-up blood culture, community-acquired infection, persistent fever, and cutaneous markers suggesting acute systemic infection. Awarding points to each risk factor—2 points for a positive follow-up blood culture and 1 point for each of the others—resulted in a linear relationship showing increasing probability of complicated infection (see Figure). Importantly, even in the absence of any of the 4 risk factors, complicated infection was predicted in 16% of the patients.
|
Association between S aureus Bacteremia
Score and
|
Comment by Jerry D. Smilack, MD
Even in the antibiotic era, S aureus bacteremia is a serious infection and frequent cause of mortality. The challenge facing clinicians is distinguishing between patients who are at risk of serious morbidity or even death and those who will respond uneventfully to antimicrobial therapy.
Several years ago, associating S aureus bacteremia with the presence of a removable focus of infection (eg, an intravascular catheter or drainable cutaneous abscess) was suggested as a basis for short-course antimicrobial therapy since the risk of complications was felt to be low. More recently, use of echocardiography (especially transesophageal echocardiography) has been advocated as a means of identifying those with occult endocarditis.
Fowler et al now offer us another schema for identifying those at high risk, suggesting that patients with none of 4 easily ascertainable risk factors "may be suitable for shorter courses of antibiotic therapy and/or less complex testing," presumably echocardiography. They caution, however, that even in the absence of these risk factors, 1 in 6 patients with S aureus bacteremia will have a serious complication from that infection.
Several points of caution must be raised. First, the most important risk factor predictive of complicated infection was a positive follow-up blood culture. However, 21% of the entire patient population in this study failed to have follow-up blood cultures drawn. Was this because the patients responded rapidly to therapy and their treating physicians did not feel that follow-up cultures would be helpful? Could cultures have been obtained with greater frequency in the sicker patients, perhaps those with prolonged fever or other complications? Since Fowler et al did not state what criteria were used to determine when or if follow-up cultures were obtained, it seems possible that bias could have entered into the predictive model. Second, is the ability to predict those at risk going to make a clinical difference? Can physicians treat those with none of the 4 risk factors differently from those with 1 or 2 (or even all 4) risk factors, since even 16% of those free of risk factors could be predicted to have complications?
Nevertheless, this study offers a fresh look into the question of which patients are at increased risk of complications from S aureus bacteremia. If similar, more controlled studies confirm its findings, we will have gained a useful tool in confronting a very vexing clinical problem.
Dr. Smilack is Infectious Disease Consultant Mayo Clinic Scottsdale Scottsdale, AZ.
By determining whether 4 key risk factors are present, clinicians might be able to identify those patients with S aureus bacteremia who are at increased risk of serious, complicated infection.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.