Patient flow product taps hidden capacity
Up to 20% increase in bed capacity possible
Capacity limits and bed shortages lead to difficult decisions for hospital administrators, including whether to cancel surgeries, build new facilities, add staff, or continue to divert patients to other hospitals.
Yet, according to Stockamp & Associates Inc., a Portland, OR-based national provider of performance improvement solutions in health care, a crucial option often remains unexplored: tapping into hidden capacity by streamlining how patients move through a hospital’s acute care system. (See flowchart, below.)
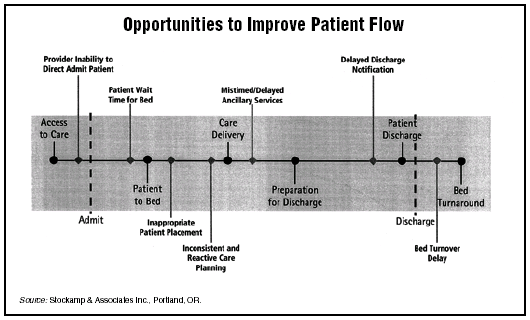
Initial evaluations by the company indicate that often hospitals could increase their capacity by up to 20% by effectively identifying and addressing root causes of inefficiency. This, says the company, presents significant revenue opportunities, reduced cost per case, and increased coordination in the delivery of care.
A new product specifically developed to address this issue, called Patient Progression, has confirmed the company’s hypothesis in early pilot programs.
"We discovered this through a review of the literature and pilot work with our clients," says Ann Kirby, MPA, MSN, a director at Stockamp & Associates Inc.
"That has held true as we have gone out to other clients. The bottom line in what we find typically is our clients can realize up to 2% to 4% of net revenues by better utilizing their capacity. The kicker is there needs to be demand in the market to fill the [additional] beds, but most of our clients are not concerned about that in growing markets."
Kirby has more than 20 years’ experience in the health care industry, including working as a staff nurse for nine years in academic medical centers before moving into hospital management and once was a Stockamp & Associates client.
She has led consulting teams in the assessment, redesign, and implementation of revenue cycle workflow and customer service processes, and oversees the design and delivery of Stockamp’s clinical service lines.
A common philosophy
The Patient Progression methodology focuses on creating new measures of effectiveness for these key factors:
- demand;
- bed management/turnaround performance;
- discharge planning delays;
- the ability to accurately predict discharges;
- performance against established standards of care.
It is a mix of an in-depth review of a hospital’s current operations and systems, the creation of detailed operational benchmarks, and the implementation of data management and reporting systems, according to Stockamp.
Although it is new, it is based on the same approach used to develop earlier products, Kirby explains.
"We address people, process, and tools to drive culture change. In this case, the change is around how patients flow through the hospital. For example, we might look at the role of house supervisor. We have almost universally found they are not empowered and receive poor communication from the rest of the staff," she says.
Unfortunately, a lot of things typically are broken in the patient flow area, Kirby continues.
"There is usually no good way for people who know what is going on with the patient to bring that information to a central area, and this is very important," she adds.
"You must know what is going on with all the beds in the hospital — for example, which patients in beds will be discharged in one hour. The people who really know that information must all be connected to the same process so that the information gets to the same place."
Kirby says her firm uses a combination of its own proprietary tools and some tools the clients already are using.
"We might, for example, introduce an automated work driver," she says.
"This helps the discharge planner. It has the work laid out for them in the morning, does a lot of what they do automatically, and prompts and prioritizes and helps them keep tabs on what’s done," Kirby explains.
"We try and get at things that are good predictors," adds Ken Saitow, Stockamp’s IT manager. "Some things we come up with will really put your finger on the pulse [of patient flow]."
If a hospital does not have metrics for some or all of the potential breakdown points in the patient flow process, it is not optimizing its current resources, according to Kirby.
She recalls when working with one client, asking that client to predict which beds would be available the next day. "They were only right 20% of the time. You can imagine what that does to their decision-making ability. Two beds vs. 10 beds is a significant difference, yet I haven’t found any client who’s measuring that."
Stockamp used this formula:
Number of predicted discharges divided by number of actual discharges.
"Now this client is in the 70% accurate prediction range after we have implemented Patient Progression process and tool changes with them," Kirby says.
This may be the single most important factor involved in improving patient flow — perhaps even more important than having good reporting tools or even good metrics, she notes.
"If you do not measure the right things on an ongoing basis, you can lose whatever progress you have made." It is lasting change, Kirby says, that is most critical.
Making the change last
Stockamp uses a number of strategies to ensure change that is both effective and lasting. For example, increased capacity is achieved by involving all the key stakeholders in a hospital setting, from housekeeping and case managers to nurses and physicians, to improve the use of existing beds.
"One of the interventions we use is the discharge coordination meeting," Kirby notes.
"In the morning, we bring together the case manager, the bedside nurse, the nurse manager, and a physician [if available] or a nurse practitioner. Between all of those people, we have a really full picture of what’s going on with the patients. But we also talk with them about what should be happening, she says.
"For example, if a patient is here for knee surgery and our goal is to send her home in X days, what needs to happen? Maybe there needs to be patient education for the transition to happen in a quality manner. We also target in advance beds that will be opening up; by communicating to someone in the central bed hub area, you get a picture of the whole house," Kirby says.
"Quite often, we don’t see clients working across the house, but in silos," Saitow adds.
Kirby concurs. "Sometimes, they collect numbers but just don’t use them across the system. They may know, for example, that they admit 20% of the ED patients, which is 30 beds a day, but that information is not used by others in bed placements."
Sometimes, the metrics are missing or the information is fragmented, Kirby says. To overcome this common weakness, "we have developed a reporting database."
Saitow calls it a dashboard. "Clients can look at it on a weekly basis to understand the trends of certain indicators. As unit coordination meetings and others take place, staff can focus on the performance of metrics to know if emphasis is needed in one area or another," he explains.
"This a management tool that, as far as we can tell, is generally lacking" in hospitals, Kirby says.
Working alongside staff
Equally important to ongoing success: Her team works alongside staff to help them attain efficient bed use on nursing floors, critical care units, and emergency departments (EDs), she notes.
"Typically, consultants will run assessments and leave you with their recommendations. Our approach is to stay with you during the whole period of time and help you implement the change; we are concerned about ongoing return on investment," Kirby continues.
"We do not ask the client to take 12 [full-time employees to implement the program]," Saitow adds. "We work side by side with them as they do their jobs. We begin with a no-charge assessment, to get to understand their processes and to understand the level of opportunity and to let us tailor our solution to their environment."
As an illustration, Stockamp has in place with one client a clinician who works on its project. "Last week, she worked with all the utilization review staff," Kirby says. "She looked at their set of criteria for clinical indicators and level of care required. Side by side, she helped them use the tool to problem solve, to make sure they would know how to do the work when we are gone."
Helping staff understand their roles
Another critical part of creating lasting change is for staff to truly understand their roles, Kirby notes. "For example, when something is not meeting criteria, they need to raise a red flag," she says. "They, along with the physicians, must serve as drivers of care."
But it is the recognition of the need to look at things differently that is "the final point that drives culture change," Saitow says.
"In order to make any of these things work, you need it, or it will go away after a period of time. We work shoulder to shoulder with the clients to internalize and look at this business problem differently than they ever have before. They will get recurring benefits only if the culture is changed," he adds.
The resulting new efficiency not only helps hospitals reduce ED diverts and discharge delays and enhances communication between care providers, but it also leads to improved patient and physician satisfaction as well as heightened morale and accountability among staff, according to Stockamp.
Kirby notes that the firm soon will be able to report on some real-world results with one of its pilot clients. "A lot of things we thought would happen with this product line are true."
Need More Information?
For more information, contact:
• Ann Kirby, MPA, MSN, Director, Stockamp & Associates Inc., Portland, OR. Telephone: (503) 303-1200. Web site: www.stockamp.com.
Capacity limits and bed shortages lead to difficult decisions for hospital administrators, including whether to cancel surgeries, build new facilities, add staff, or continue to divert patients to other hospitals.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
