Special Feature: The Electrocardiographic Diagnosis of LV Aneurysm
The Electrocardiographic Diagnosis of LV Aneurysm
By William J. Brady, MD
Left ventricular (LV) aneurysm is defined as a localized area of infarcted myocardium that bulges outward during the entire cardiac cycle. LV aneurysm most frequently is seen after extensive anterior wall myocardial infarction (MI), but also may be encountered following inferior and posterior wall MIs. In most instances, the LV aneurysm is manifested electrocardiographically by some degree of ST segment elevation (STE); approximately 60% of patients with completed MI who manifest persistent ST segment abnormality will demonstrate ventricular aneurysm.
Among ED patients with STE, LV aneurysm is an uncommon cause of the ST segment abnormality, accounting for only 3-4% of all patients with STE.1,2 While STE secondary to aneurysm is rare, this pattern of STE is an important cause of error in diagnosis and management of ED chest pain patients with ST segment abnormality.3,4
Patients who tend to develop LV aneurysm include those individuals with a previous large MI, particularly in those instances with resultant LV ejection fractions less than 50%. A marked gender difference is encountered in these patients, with a male-to-female ratio of 4:1.5 At coronary angiography, LV aneurysm is seen in approximately 8% of post-MI patients. The incidence of LV aneurysm following MI ranges from 3% to 15%, as determined at autopsy.6 The vast majority of LV aneurysms result from MI, yet other etiologies are encountered, including blunt chest injury with myocardial contusion, Chagas disease, and cardiac sarcoidosis. Approximately three-quarters of LV aneurysms involve the anterior wall, and are attributable to MI due to obstruction of the left anterior descending artery.7
Regarding electrocardiographic pathophysiology, the ST segment abnormalities result from either an injury current originating from viable yet ischemic myocytes in the aneurysm, or from mechanical wall stress caused by traction on the adjacent, normal myocardium.8 Pathologically, the aneurysm is characterized by transmural fibrosis—clearly delineated from, and markedly thinner than, the adjacent myocardium.9 Associated post-mortem findings include significant multi-vessel coronary artery disease, scarred papillary muscle, pulmonary edema, pericardial thickening, and mural thrombi.
The diagnosis of LV aneurysm best is made via an analysis of the history (past MI) and physical examination (evidence of congestive heart failure) findings, as well as the results of cardiac imaging studies beyond the electrocardiogram (ECG). The patient may be asymptomatic, however, with a markedly abnormal ECG. Echocardiography and coronary angiography are excellent modalities that can demonstrate the anatomic and functional features of LV aneurysm. Echocardiography has a sensitivity and specificity of 93% and 94%, respectively, for detecting LV aneurysm, representing the most frequently and easily applied test for this anatomic abnormality. Coronary angiography, however, remains the gold standard for diagnosis.
Electrocardiographic Features of LV Aneurysm
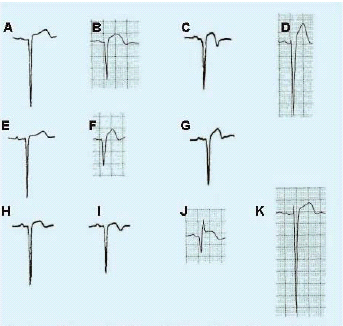
The electrocardiographic features of LV aneurysm include the following: 1) STE, most often less than 3-4 mm; 2) diminished or inverted T waves; 3) QS or Qr complexes preceding the STE in the right-to-mid precordial leads; and 4) lack of dynamic change of these findings over time on ECG. (See Figure.) Inferior aneurysms usually have QR waves and are very difficult to distinguish from acute MI of the inferior wall. LV aneurysm is characterized electrocardiographically by persistent STE seen days to weeks after MI. STE resulting from LV aneurysm may assume varying morphologies, ranging from benign, minimally deviated, concave elevations to more ominous, pronounced, convex ST segment elevation. (See Figure.) Fortunately, the vast majority of LV aneurysm patients will demonstrate a concave morphology of the elevated ST segment.2 It also has been shown that the magnitude of the STE does not correlate with thesize of the aneurysm.10
|
Because LV aneurysm frequently is anterior or anterolateral in location, electrocardiographic STE typically is seen in leads I, aVL, and V1-V6. STE resulting from LV aneurysm of the inferior wall is noted in leads II, III, and aVF (the inferior leads); the magnitude of the STE in this distribution is less pronounced than that seen in the anterior wall aneurysm pattern. Posterior wall aneurysm is more difficult to detect electrocardiographically from the perspective of the traditional 12-lead ECG; if used, the posterior leads V8 and V9 may demonstrate STE.
ST segment depression, when observed in the setting of ST segment elevation elsewhere on the ECG, may represent reciprocal change and strongly suggest the presence of STE acute MI. ST segment depression, however, may also be seen in lead aVL in the patient with inferior wall LV aneurysm; caution is therefore advised.
Patients with LV aneurysm also frequently will have significant Q waves in the same distribution. In fact, it has been demonstrated that patients with larger LV aneurysms have a wider distribution of Q waves.10 The loss of R wave deflection in standard leads also may correlate with the presence of LV aneurysm.11 Initially, the QRS complex duration usually is normal in the setting of electrocardiographic LV aneurysm, assuming that intraventricular conduction is normal; however, the QRS complex width may increase with the age of the aneurysm.10
Lastly, the ratio of maximum T-wave amplitude to the QRS complex amplitude is important, with lower values occurring in association with LV aneurysm. Smith and colleagues have reported that this ratio (T-wave amplitude/QRS complex amplitude), when less than 0.36, is associated highly with LV aneurysm-related STE.12 In the patient with STE acute MI, the T-wave frequently is quite prominent—termed the hyper-acute T-wave of acute MI. In acute MI, the ratio of the T-wave to the QRS complex, therefore, usually is a larger value, occasionally approaching 1.0.
Dr. Brady, Associate Professor of Emergency Medicine and Internal Medicine, Vice Chair, Emergency Medicine, University of Virginia, Charlottesville, is on the Editorial Board of Emergency Medicine Alert.
References
1. Brady WJ, et al. Electrocardiographic ST segment elevation in emergency department chest pain center patients: Etiology responsible for the ST segment abnormality. Am J Emerg Med 2001;9:25-28.
2. Brady WJ, et al. Electrocardiographic ST segment elevation: The diagnosis of AMI by morphologic analysis of the ST segment. Acad Emerg Med 2001;8:961-967.
3. Brady WJ, et al. Errors in emergency physician interpretation of ST segment elevation in ED chest pain patients. Acad Emerg Med 2000;7:1256-1260.
4. Brady WJ, et al. Electrocardiographic ST segment elevation: Correct identification of AMI and non-AMI syndromes by emergency physicians. Acad Emerg Med 2001;8:349-360.
5. Dubnow MH, et al. Postinfarction ventricular aneurysm. A clinicomorphologic and electrocardiographic study of 80 cases. Am Heart J 1965;70:753-760.
6. Faxon DP, et al. Prognostic significance of angiographically documented LV aneurysm from the Coronary Artery Surgery Study (CASS). Am J Cardiol 1982; 50:157-164.
7. Elliott MA, et al. Acute myocardial infarction. In: Braunwald B, ed. Heart Disease. Philadelphia: W.B. Saunders Co.; 1997:1.
8. Goldberger AL. Myocardial Infarction: Electrocardiograhic Differential Diagnoses, 4th ed. St Louis: Mosby; 1991:1.
9. Alexander RW, et al. Diagnosis and Management of patients with Acute Myocardial Infarction. In: Alexander RW, et al., eds. Hurst’s The Heart. McGraw-Hill: New York; 1998:1.
10. Cokkinos DV, et al. LV aneurysm: Analysis of electrocardiographic features and postresection changes. Am Heart J 1971;82:149-157.
11. Rosenberg B, et al. Electrocardiogram in ventricular aneurysm. Am Heart J 1949;37:267-277.
12. Smith SW, et al. Ratio of T amplitude to QRS amplitude best distinguishes acute anterior MI from anterior left ventricular. Abstract. Acad Emerg Med 2003; 10:516-517.
Left ventricular (LV) aneurysm is defined as a localized area of infarcted myocardium that bulges outward during the entire cardiac cycle. Among ED patients with ST segment elevation, LV aneurysm is an uncommon cause of the ST segment abnormality, accounting for only 3-4% of all patients with STE.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.