Pediatric Migraine: Recognizing and Managing Big Headaches in Small Patients
Author: Raymond D. Pitetti, MD, Assistant Professor, Division of Pediatric Emergency Medicine, Department of Pediatrics, Children’s Hospital of Pittsburgh and the University of Pittsburgh School of Medicine, Pittsburgh, PA.
Peer Reviewer: Ronald M. Perkin, MD, MA, Professor and Chairman of Pediatrics, Brody School of Medicine, East Carolina University, Greenville, NC.
Children often present to the emergency department (ED) complaining of headaches. While most headaches in children are not signs of serious, underlying disorders, some headaches may be the first presentation of a migraine headache. Migraine is the most common cause of recurrent, intermittent headaches in children.1-3 However, migraine headaches often are underdiagnosed and undertreated in children.
Migraine symptoms, in general, and especially in children, can vary dramatically in terms of character and severity. The diagnosis of migraine headache is based primarily on the history of symptoms and supported by a positive family history and a normal physical examination. Neurodiagnostic tests often are unnecessary and serve only to exclude nonmigraine disorders.
Recent advances in the understanding of the pathophysiology and genetics of migraine have led to new therapeutic interventions for the treatment of migraine headaches.
This review presents a comprehensive approach to the child with migraine headaches. An overview of the current understanding of the pathophysiology of migraine headaches is presented, followed by a description of common and classic migraine headaches, migraine variants, migraine equivalents, and treatment options. The author concludes with a summary of the therapeutic approach to the child who presents acutely with a migraine headache.—The Editor
Introduction
Headaches commonly occur in children. Interestingly, many children who present with headaches are suffering from migraines. However, many parents, and even clinicians, are unaware that migraine head-aches commonly occur in pediatric patients.
Migraine headaches are considered to be a hereditary disorder, characterized by autosomal dominant inheritance with incomplete penetrance, and are the most common cause of recurrent intermittent headaches in children.1-3 Migraine headaches occur in 3-5% of all children and in as many as 18% of adolescents.4 Prevalence rates in preschool children probably are underestimated, as migraine symptoms tend to be atypical in the younger age group and rarely are identified as migraines.
Prior to puberty, prevalence rates in children are equal among both sexes, but post-pubertal girls are more than twice as likely as boys to suffer from migraine headaches, most likely because of the triggering effect of the menstrual cycle on migraine headaches.1 A 1999 population based survey found that in individuals 12 years of age and older, 18.2% of females were found to have migraine headaches compared to 6.5% of males.5
It is important to recognize that many children begin to have migraine headaches at a young age. A prospective, longitudinal, 10-year follow-up study of pediatric patients with migraine found that 24.3% of patients had their first headache before 6 years of age and 57% at 6-10 years of age.6 Among adults with headaches, nearly half say that their headaches began before they were 10 years of age.7
Most investigations into the diagnosis and management of migraine headaches have occurred in the adult population. However, our current understanding of migraine headache suggests that the diagnosis, presentation, natural history, prognosis, and response to medications are different for children than for adults. Unfortunately, only a few controlled trials have investigated the acute and prophylactic use of medications in the treatment of migraine in children.
The Pathophysiology of Migraine
Understanding the mechanisms by which migraines occur in children has led to new therapeutic options and more effective treatments for migraine headaches and symptoms.
Previously, three major mechanisms for the pathogenesis of migraine had been proposed: vascular, humoral, and neural. The vascular theory suggested that during the initial phase of a migraine headache, a wave of cortical excitation followed by cortical depression spread over both hemispheres from back to front, in association with decreased regional blood flow and transitory neurologic disturbances.8 In subsequent phases of migraine progression, increased blood flow was thought to occur in the internal and external carotid circulation, distending pain-sensitive extra-cranial arteries and resulting in a sterile inflammation.
The humoral theory proposed that increased serotonin levels resulted in vasoconstriction of the innervated vascular system and decreased cerebral blood flow. As hypoperfusion progressed, aura and headache developed.
Finally, the neural mechanism proposed that migraine headaches occur due to an inherited sensitivity of the trigeminal vascular system.8-12 This mechanism suggested that cortical, thalamic, or hypothalamic mechanisms initiated an attack due to some internal or external stimuli. The locus ceruleus and nucleus raphe dorsalis were stimulated, which in turn stimulated the cortex via serotoninergic and noradrenergic pathways and produced a spreading wave of neuronal depression. The cranial vasculature also was stimulated, resulting in neurogenic inflammation and secondary vascular reactivity. Released vasoactive peptides stimulated endothelial cells, mast cells, and platelets, creating a cascade that resulted in sterile inflammation of dural and pial blood vessels from which nociceptive afferents transmitted pain signals centrally via the trigeminal nerve.
Currently, most investigators believe that migraine is a disorder that combines aspects of both the neural and vascular theories. In fact, serotonin is believed to play a key role in the pathophysiology of migraine headaches and has been the focus of some of the newer antimigraine medications.
The Diagnosis of Migraine
While children often present to the ED complaining of a headache, diagnosing a child with a migraine headache can be difficult. While there are many reasons why making the diagnosis of migraine is difficult, uncertainty about the definition of a migraine headache, its varied presentations, and lack of a clear understanding of its pathophysiology are of particular concern. The International Headache Society (IHS) has developed criteria for the diagnosis of migraine headaches and classifies migraines as either migraine without aura or migraine with aura.8 (See Table 1.)
|
In essence, the diagnosis of migraine headache in children is based on an evaluation of the presenting clinical signs and symptoms. However, many investigators believe that the IHS criteria for migraine without aura are relatively insensitive for the diagnosis of migraines in children and have suggested several revisions to the criteria. Two modifications to the original criteria, a reduction in the minimal time required for the duration of the headache and the inclusion of a bifrontal location for the headache, increase the sensitivity of the criteria for diagnosing migraine headaches in children from 66% to 88%.13 Table 2 lists the proposed revisions to the IHS criteria for the diagnosis of migraine without aura in children.
|
History and Physical Examination. The evaluation of the child who presents with a migraine headache begins with the history and physical examination. In particular, the history often will provide clues to the diagnosis, with the physical examination excluding other causes of headaches.
A history of migraine headaches often is documented in at least one parent in 90% of children with migraine. In addition, a family history of motion sickness also is common, as well as a history of the child suffering from motion sickness, bruxism, fainting spells, sleep talking, and sleepwalking.14,15 Children with a history of migraine headaches also are more likely to suffer from ice cream headaches than children without such a history.16
Interestingly, infantile colic also may be a migraine-related phenomenon. Recent studies have suggested that compared to control subjects, children with migraine headaches have a higher prevalence of sleep disturbances and infantile colic.17,18 Children with a history of infantile colic also are more likely to have a family history of migraine.17 In a recent case study of an infant with colic who also was thought to have migraine headaches, complete resolution of the symptoms of colic occurred following the institution of anti-migraine therapy (cyproheptidine).19
While migraine attacks can begin at any time of the day, they more commonly occur during the late afternoon in children and even earlier in the day for adolescents. Most children who suffer from migraine headaches will have 1-4 attacks per month. However, children may be asymptomatic for long intervals and then suffer a cluster of attacks. While migraine typically is one-sided in adult patients, a bilateral headache is more common in children. In addition, the headache more often is described as throbbing.
Many triggers have been identified for the initiation of migraine headaches in both children and adults. Common triggers include stress, fatigue, hunger, head injury, exercise, menses, foods, and weather changes. Many of the foods that have been identified as triggers of migraine headaches contain tyramine, phenylethylamine, caffeine, or artificial sweeteners and colorings. Often, a headache diary can help identify migraine triggers in children.
A child who presents with a headache should have a thorough medical history obtained and a complete physical examination performed, including the measurement of vital signs. The physical examination should include a thorough neurological examination and an examination of the optic fundus to exclude the diagnosis of a more serious neurological condition, such as a brain tumor.
Parents should be informed that most children with brain tumors will present with other concerning clinical signs and symptoms in addition to that of a headache. In a review of children with known brain tumors, investigators found that 85% of children had an abnormal physical examination within two months of the onset of headache.21 Common findings included ataxia, head tilt, and papilledema. Historically, the following factors were found to be more commonly associated with children with a brain tumor headache: 1) recurrent morning headaches; 2) headaches that repeatedly awaken the child from sleep; 3) intense, prolonged, incapacitating headaches; and 4) changes in the quality, frequency, and pattern of headaches. Seventy-eight percent of patients with a brain tumor headache presented with repeated episodes of emesis.
Diagnostic Testing. Currently, no consensus exists among investigators and clinicians as to the role of routine diagnostic testing in the evaluation of children with headache. This includes the use of routine laboratory testing, cerebrospinal fluid examination, electroencephalographs (EEG), and neuroimaging. It is important to remember, however, that while the child who presents with a classic presentation of migraine headache may not require routine diagnostic testing, the patient who presents acutely with a severe headache that is not classic for migraine still may require testing to determine whether an underlying disease process is present. This review will concentrate on the evaluation of the child with a headache thought to be migraine in origin. As such, there is no evidence to suggest a role for routine laboratory testing, lumbar puncture, and EEG testing in the evaluation of the child with migraine headache.20
More problematic is the routine use of neuroimaging, either computed tomography (CT) or magnetic resonance imaging (MRI), in the evaluation of children with migraine headaches. Often, parents, and even children, may be concerned that the headache is a symptom of a more serious underlying problem, such as a brain tumor. In fact, parents may be insistent on radio-graphic imaging of the head. In general, however, CT and MRI are not required for the standard evaluation of a child presenting with a migraine headache.
Recently, Lewis and Dorbad conducted a retrospective review of the use of neuroimaging in the evaluation of children presenting with a migraine headache who had a normal neurological examination.22 Of 107 patients with migraine, 40% had CT scans, only two of which were considered abnormal. Twelve patients had MRIs, of which two were considered abnormal. Abnormalities included a Chiari type 1 malformation (N = 2), an arachnoid cyst (N = 1), and a dilated Virchow-Robin space (N = 1). None of the findings changed the diagnosis, management, or outcome of patients. The authors concluded that neuroimaging is not warranted in the routine evaluation of children presenting with a migraine headache and a normal neurological examination.
Similarly, Maytal and colleagues studied 133 patients presenting with headache and reported that of 78 patients who had either an MRI or CT scan, only four patients were found to have abnormalities,23 and none of the abnormalities were considered clinically relevant or related to the presenting complaint.
Classic Migraine—Migraine with Aura. While classic migraine is the best-recognized presentation of migraine, it occurs in fewer than one-third of children with migraine head-aches.24 Historically, classic migraine has been described as a biphasic event. Typically, symptoms of aura occur during the first phase, and headache, nausea, and vomiting occur during the second phase. The phrase "classic migraine" largely has been replaced by the phrase "migraine with aura."
During a migraine with aura, symptoms may occur only during the first phase, resulting in what is termed a migraine equivalent; only during the second phase, resulting in headache and vomiting; or during both. An aura is defined as any abrupt neurological change that is fully reversible and precedes a migraine headache. The most common symptoms to occur during the first phase of a migraine headache include visual aberrations, such as the perception of dancing lights, blind spots, blurred vision, visual hallucinations, or transitory blindness (the aura). Visual symptoms tend to be specific for each child suffering from migraine headaches.
Migraine headaches may terminate after the first phase without headache or proceed to the second phase with symptoms of headache and nausea. Headaches tend to be dull at first, becoming throbbing, pulsating, or pounding. Headache is unilateral in two-thirds of older children and adult patients and most intense in the region of the eye, forehead, or temple. However, younger patients with migraine headaches often will complain of bilateral temporal pain. Eventually, the headache becomes constant and diffuse, lasting a variable length of time. Anorexia and photophobia often are present.
Common Migraine. Common migraine is the most common form of migraine in children. Common migraines differ from classic migraine in that the symptoms do not regularly develop in a biphasic mode of visual aura followed by headache. Most children with common migraine often will present with malaise, dizziness, nausea, and vomiting that is followed by either a unilateral or bilateral, pounding headache. The child will appear sick, often will want to lie down, and will be extremely sensitive to light and sound. The headache often will end when the child falls asleep. The phrase "common migraine" largely has been replaced by the phrase "migraine without aura."
Migraine Equivalents. Migraine equivalents or complicated migraines are migraine headaches that are associated with transient neurological deficits or alterations in states of consciousness. Migraine equivalents are thought to occur due to prolonged vasoconstriction and ischemia of specific cerebral areas. The type of neurological deficit that occurs, and thus the type of complicated migraine, is dependent on the vascular territory affected. In migraine equivalents, neurological deficits often will precede the symptom of headache, but can occur following it instead. In some instances, a headache may not even occur. Migraine equivalents usually are benign, and many children will go on to develop more typical migraine headaches later in life. Types of migraine equivalents include hemiplegic or hemisensory migraines, ophthalmoplegic migraines, basilar artery migraines, acute confusional migraines, and the Alice in Wonderland syndrome. (See below.)
Hemiplegic or hemisensory migraines, more common in younger children than in adults, are characterized by the sudden onset of hemiparesis or hemisensory loss followed by a contralateral headache. Symptoms are thought to occur due to vasoconstriction and neuronal dysfunction resulting in ischemia in the distribution of the middle cerebral artery.25 Symptoms can last hours to days, though the hemiparesis often outlasts the headache.25 Interestingly, the hemiparesis may alternate sides during subsequent attacks.25
Ophthalmoplegic migraines are characterized by unilateral eye pain, headache, and transient ipsilateral third nerve palsy and is thought to occur either because of edema involving the internal carotid artery within the cavernous sinus or because of edema involving the distal basilar artery.25 Third nerve involvement occurs in 80% of cases.26 The eye pain in ophthalmoplegic migraines often is severe and located behind the eye.25 On examination, the affected eye will be noted to move laterally due to the unopposed action of the sixth nerve. In addition, ptosis, diplopia, and mydriasis may occur. Ophthalmoplegic migraines have been known to occur in babies younger than 1 year of age. During an attack, headache symptoms can last for hours, but the ophthalmoplegia can last days to weeks. Early, high-dose corticosteroid treatment is recommended to rapidly resolve symptoms of an acute episode and potentially to prevent permanent oculomotor nerve injury.27
Basilar artery (or Bickerstaff) migraines often present with a constellation of visual symptoms, including blindness, vertigo, ataxia, loss of consciousness, and drop attacks. Basilar artery migraines are the most common form of migraine equivalent to occur in children (3-19%) and occur more frequently in girls.25,28 The initial symptoms of basilar artery migraine usually are visual and the episode usually is associated with an occipital headache.
Acute confusional migraines rarely occur in children. Difficult to diagnose, acute confusional migraines are characterized by restlessness, combative or hyperactive behavior, and occasional loss of consciousness. A headache usually precedes the symptoms, and the attacks can be triggered by mild head trauma.25 Attacks usually begin when the child is 5-15 years of age. Males more often are affected than females. Symptoms of acute confusional migraine typically last 4-6 hours but can last for days.
Micropsia, metamorphosia, olfactory, auditory, or gustatory hallucinations and distortion of body image, spatial relations, and time sense characterize the Alice in Wonderland syndrome. The Alice in Wonderland syndrome sometimes is described as a migraine variant rather than as a complicated migraine. A headache may or may not occur with this syndrome, and most attacks are not associated with a headache.
Migraine Variants. Migraine variants are defined as the occurrence of episodic neurological complaints not associated with headache, in children who develop typical migraine headaches later on in life. Migraine variants are felt to be related to migraine by their periodicity, paroxysmal nature and the fact that children who have these symptoms often develop true migraine headaches. However, a family history of migraine may or may not be present. Difficult to diagnose, the relationship of migraine variants to migraine headache often is made after more typical migraine symptoms develop later in the child’s life.
A number of distinct migraine variants have been recognized. These include benign paroxysmal vertigo, cyclic vomiting, abdominal migraine, and benign torticollis. A recent investigation into the occurrence of migraine variants in a pediatric neurology practice found that of 5848 patients seen during an eight-year period, 1106 had migraines and 108 (1.8% of total patients, 9.8% of patients with migraines) had a history of a migraine variant.29 The most common migraine variant reported was benign paroxysmal vertigo, occurring in 38% of all patients with migraine variants.
Children with benign paroxysmal vertigo usually will present with monthly attacks of vertigo that decrease in frequency as the child grows older. Attacks often begin when the child is 2-6 years of age.25 Symptoms generally last several minutes and the child will appear frightened, often grabbing a stationary object for stability. Nystagmus and ataxia commonly occur, and the child will complain of nausea and vomiting. Specific triggers, such as fatigue, often are identified. If attacks are frequent and disabling, diphenhydramine may be of benefit, though acute therapy usually is not needed due to the brief nature of the attacks.30 Benign paroxysmal vertigo is the most common cause of vertigo in young children.31 Attacks typically will resolve in 1-2 years and be supplanted by more typical migraine headaches.32
Cyclic vomiting usually occurs in children between the ages of 4-8 years. Episodes often occur monthly and are characterized by episodes of abdominal pain, nausea, and vomiting. Autonomic symptoms, including lethargy and pallor, also can occur.33 Episodes will occur frequently and regularly. A headache may or may not be present during an attack. Between episodes, the child appears well.33 In most children, the disorder will last several years and tends to resolve by late childhood or early adolescence.33
Similarly, abdominal migraine is characterized by episodes of crampy or colicky abdominal pain located in the periumbilical or epigastric areas. Attacks can last minutes to hours and can be accompanied by nausea and vomiting. In between attacks, the child appears well. Abdominal migraine often develops in children 4-10 years of age and typically resolves in 1-2 years, only to be replaced by more typical migraine headaches.
Because both cyclic vomiting and abdominal migraines share similar historical and clinical features and respond similarly to the blockade of serotonin receptors, they probably represent related conditions. Evaluation should focus on eliminating possible gastrointestinal or metabolic causes. Affected children can be treated with intravenous hydration and antiemetic medications such as ondansetron. Sumatriptan has been used to treat acute episodes of cyclical vomiting.34 Effective prophylactic medications used in the prevention of abdominal migraine include propanolol and cyproheptadine.35
Benign torticollis is defined as recurring episodes of head tilt (torticollis) in a child younger than 1 year of age. Torticollis may be accompanied by pallor, headache, nausea, and vomiting, irritability, and drowsiness. The side of the torticollis often will vary during attacks. Extra-ocular movements are normal, and attacks are not related to feeding or changes in positioning. The condition is short-lived and resolves spontaneously, though rarely symptoms can persist for days. The child appears well between episodes. A family history of migraines or motion sickness often is found, and many infants with torticollis develop benign paroxysmal vertigo and more typical migraine headaches later in life.
Treatment
Many children who present to the ED with a headache or symptomatology consistent with migraine will require emergent treatment for their symptoms. Two treatment strategies should predominate during the ED visit—aborting the acute attack and preventing future attacks. While the physician often will concentrate on providing acute relief for the headache, preventing future attacks and recurrences also should be considered. Importantly, many patients who receive abortive treatment for a migraine headache will have recurrence of symptoms within 24-72 hours.
Acute Therapy. Effective treatment of migraine headaches often begins with reassuring the child and his or her family that the headaches are treatable and do not represent an underlying problem such as a brain tumor, and in appropriate situations ordering diagnostic testing to exclude more serious pathology. In addition, the clinician should explain to the parents that the headaches are not a psychological illness or a ploy on the part of the child to avoid school.
The symptoms that patients present with directly affect the types of therapies used to treat the migraine. Patients who are in severe pain should receive parenteral medications as therapeutic drug levels can be reached much more quickly intravenously compared to the oral route.
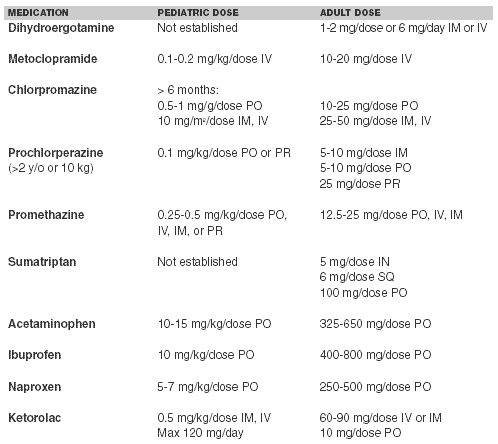
In general, prior to the use of any medication, the child should be placed in a dark, quiet environment. Ice packs can be applied to the head to help alleviate pain. Following a complete history and physical examination that includes an assessment of the patient’s severity of pain and hydration status, a decision on the most appropriate treatment option can be made. Table 3 lists the medications most commonly used in the treatment of migraine headaches in children. A description of commonly used treatment modalities follows.
|
Sleep. Sleep often is effective in relieving most migraine attacks.36 Investigators reported in a recent study of 133 children younger than 8 years of age who had presented to an outpatient setting with a migraine attack that 62% of episodes resolved following a period of sleep. However, having a child sleep in the ED as the sole treatment option may not be practical. Instead, sleep can be used as an adjunctive treatment to other treatment options.
Alternative Therapies. Relaxation techniques, self-hypnosis, and biofeedback all have been evaluated as treatment options for pediatric migraine.36-42 All three treatment modalities have shown some success in relieving or preventing the symptoms of pediatric migraine. However, these therapies may not be practical as a treatment option in the ED setting.
Intravenous Fluids. Since gastric stasis often accompanies migraine headaches, and patients often are dehydrated due to the vomiting associated with their migraines, intravenous fluids should be given when parenteral medications are administered. Rehydration may help alleviate the nausea and vomiting associated with migraine headaches and may provide some pain relief.43
Acetaminophen. Acetaminophen has been shown to be highly effective for treating the pain, functional disability, photophobia and phonophobia in adult patients with migraine.43 In comparison to ibuprofen and placebo, acetaminophen has been shown to be superior to placebo and slightly less effective than ibuprofen in the treatment of migraine headaches in children.44 A child who presents to the ED with a migraine headache, who has not been treated with over-the-counter medications prior to arrival, and who has milder symptoms can be treated with acetaminophen early during the course of his or her evaluation.
Non-steroidal Anti-inflammatory Drugs (NSAIDs). NSAIDs often are used in the initial treatment of children with migraine headaches. Many theories have been proposed as to the role of NSAIDs in this setting, but most investigators believe that they act via inhibition of prostaglandins and of platelet aggregation.
During the initial phase of migraine attacks, plasma serotonin levels increase, and as the attack progresses, decrease. Serotonin is carried almost exclusively by platelets. NSAIDs may treat or prevent migraine headaches by inhibiting platelet aggregability and thus decrease serotonin levels.45 Many NSAIDs currently are available for use and no one oral NSAID has been shown to be superior to any other in the treatment of migraine headaches.8
Ibuprofen, at a dose of 7.5-10 mg/kg, has been shown to be effective in the treatment of migraine headaches in children.44,46 Ketorolac has been found to be highly effective in the treatment of adult patients with migraine headaches.47,48 However, ketorolac has not been well studied in the treatment of children with migraine headaches. Naproxen sodium has been found to reduce the severity and duration of headache and photophobia in adult patients with migraine headache without aura.49 However, naproxen sodium also has not been extensively evaluated in the treatment of children with migraine headaches.
A child who presents to the ED with a migraine headache, who has not been treated with medications prior to arrival, and who has milder symptoms can be treated with an oral NSAID early in his or her evaluation. Intravenously or intramuscularly administered ketorolac can be used for patients with more severe symptoms or for those who cannot tolerate an oral medication.
Opiates. Opiates have not been found to be consistently effective in the treatment of migraine headaches. In addition, opioids are believed to be less effective as a pain reliever in a serotonin depleted state such as that found in migraine.50 Therefore, opiates should be prescribed rarely, if at all, for the treatment of migraine headaches in children and should be considered a treatment of last resort.
Triptans. Increasingly, triptans are being used in the acute treatment of migraine headaches in children. Triptans act as 5HT-receptor agonists and their use results in vasoconstriction of intracranial arteries.
Sumatriptan is the most common triptan agent used and has been used in the treatment of pediatric migraine.51 Sumatriptan is available in three forms; subcutaneous injectable, tablet, and nasal spray. Intranasally administered sumatriptan appears to have a more rapid onset of effect than the oral formulation and results in fewer adverse reactions than the subcutaneous form.52
Intranasal sumatriptan has been found to be efficacious in the treatment of migraine headaches in adolescents.53-55 Nasal sumatriptan also has been shown to be effective in children 5-12 years of age.56
Subcutaneous sumatriptan has been shown to be effective in the treatment of migraine headaches in adolescents.57,58 Oral sumatriptan, however, has not been found to be efficacious in the treatment of migraine headaches in children.
Side effects related to the use of sumatriptan include flushing, chest pain, and scalp burning. In addition, sumatriptan is relatively expensive and is contraindicated in those who are intolerant of its smooth muscle stimulating properties, such as those with a history of reactive airway disease.59
A number of new formulations of triptans recently have been approved for the treatment of migraine headaches. Several have been evaluated in the management of acute attacks. Eletriptan, zolmitriptan, rizatriptan, and almotriptan have been shown to be effective in the treatment of migraine in adults.60-62 While few data pertaining to their use in children exist, both rizatriptan and zolmitriptan have been shown to be effective in the treatment of migraine headaches in adolescents.63,64
Triptans as a class of medication are considered contraindicated for the treatment of complicated migraines because of their vasoconstrictive properties. The neurological symptoms associated with these migraine subtypes are thought to occur due to vasoconstriction, and that by increasing vasoconstriction, triptans could increase the risk of brain infarction. However, investigators have not found that the use of triptans results in an increase in blood flow velocity in the basilar artery or middle cerebral artery, as would be seen if vasoconstriction of one of the arteries was occurring.65,66 In addition, the safe use of triptans in the treatment of basilar migraine and migraine with prolonged aura has been reported.67 Along these same lines, triptans should not be given concomitantly with ergotamines.
Dihydroergotamine/Ergotamines. Ergot derivatives, potent vasoconstrictors, commonly are used in the treatment of migraine headaches. Dihydroergotamine (DHE) is an ergot derivative that results in vasoconstriction of the external carotid arteries by directly affecting serotonin receptors and through alpha-adrenergic blockade.68 Given parenterally in combination with an anti-emetic, DHE has been found to be safe and effective in treating children with migraine headache.69 The addition of an antiemetic such as metoclopramide, in combination with DHE, can help reduce the symptoms of nausea and vomiting associated with migraine headaches and can enhance the effect of DHE. A common side effect noted with DHE in children is a sense of terror on the part of the child and extreme agitation. These side effects usually resolve within five minutes following administration of the medication. DHE can be given intravenously, intramuscularly, subcutaneously, or intranasally. A sublingual preparation is available. DHE has been shown to be better tolerated than ergotamine.
Ergot derivatives are contraindicated in patients with peripheral vascular disease, hypertension, coronary artery disease, and pregnancy. Ergot derivatives should not be used with the triptan class of medications, potentially compounding each medication’s vasoconstrictive effect. In addition, ergot derivatives may exacerbate the gastrointestinal complaints associated with migraine. However, dihydroergotamine has less peripheral vasoconstrictive effects than most other ergot derivatives, and thus causes fewer side effects.
Phenothiazines. Phenothiazines are centrally acting dopamine antagonists that produce an antiemetic effect at the chemoreceptor trigger zone. Phenothiazines, such as chlorpromazine and prochlorperazine, have been used to treat migraine headaches. Both exert neuroleptic effects. Chlorpromazine has been shown to significantly improve symptoms in adults with migraine headache.70 Chlorpromazine may act either by altering serotonin levels through inhibition of monoamine reuptake or by a direct effect at serotonergic receptors, or through its neuroleptic effects.71
Prochlorperazine also has been used in the treatment of children with migraine headaches. A prospective, randomized, double-blind, placebo controlled trial compared prochlorperazine to metoclopramide and placebo in the ED treatment of migraine headaches in adults.59 Intravenous prochlorperazine was shown to be superior to both metoclopramide and placebo in relieving headache and decreasing symptoms of nausea. Recently, the use of prochlorperazine buccal tablets was compared to ergotamine tartarate and placebo in the acute treatment of adults with migraine headaches.72 The buccal preparation produced faster improvement and greater efficacy than either placebo or ergotamine. Promethazine hydrochloride suppositories also have been shown to be effective in relieving the symptoms of migraine headache in children. Finally, prochlorperazine has been shown to be highly effective in the treatment of severe, intractable migraine in children.73
Metoclopramide. Metoclopramide is a dopamine antagonist that directly acts at the chemoreceptor trigger zone in the brain.74 In addition, investigators have found that it may interact with the serotonergic system as well, specifically as an antagonist at the 5-HT3 receptor located in the trigeminovascular system.68 Interestingly, metoclopramide is pharmacologically similar to phenothiazines and has been shown to increase the absorption of analgesics by promoting gastric motility.75 Because of its actions, metoclopramide has been found to be an effective treatment in the management of migraine headaches.
Metoclopramide recently has been studied as a single agent in the treatment of adults with migraine headaches.74 Ellis and colleagues evaluated metoclopramide alone and in combination with ibuprofen in a randomized, prospective, double-blinded, placebo-controlled study of the treatment of migraine headaches.74 Metoclopramide was found to be highly effective when used alone in the treatment of migraine headache. Ibuprofen was not found to act additively or synergistically with metoclopramide.
More often, however, metoclopramide is used in conjunction with other pharmacological agents in the treatment of migraine headaches.75 Metoclopramide can be given as an oral preparation but also can be given parenterally or rectally. As an intravenous preparation, metoclopramide can be paired with ketorolac in the acute treatment of migraine headaches in children. Metoclopramide also often is given with DHE to treat the nausea that frequently accompanies its use. The IM and PR preparations of metoclopramide also have been used for the treatment of migraine headaches.
Valproate. Antiepileptic medications have been used in the acute management of migraine headaches in both children and adults. Intravenous valproate has been shown to be highly effective in the acute management of migraine headaches in adolescents and has been shown to be highly effective in adult patients as well.76,77 In an open-label, randomized trial, intravenous valproate compared favorably to intramuscular dihydroergotmine, used in combination with metoclopramide, for the acute treatment of migraine headache in adults.78 However, headache relief was not as likely to be sustained at 24 hours in those patients treated with valproate.
Lidocaine. Lidocaine long has been known for its anesthetic properties and has been used most commonly for local and regional anesthesia. Recently, lidocaine has been used in the acute management of migraine headaches. In a recently conducted randomized, double-blind, controlled trial of intranasal lidocaine used in the management of adult patients with migraine headache, 55% of patients treated with intranasal lidocaine had relief of their head-aches following its use.79 Relapse of headache, however, occurred early and often following treatment. One possible mechanism by which intranasal lidocaine is thought to relieve the headache of migraine is through its effects on the sphenopalatine ganglion. However, the exact mechanism is unclear. More recently, a similarly conducted study has reported that intranasal lidocaine may not nearly be as effective.80 In a randomized, double-blind, placebo-controlled clinical trial, no difference was found in the number of patients who experienced pain relief when treated with intra-nasal lidocaine or when treated with placebo. Intranasal lidocaine has not been evaluated in the treatment of children with migraine headaches and its use cannot be advocated at this time.
Corticosteroids. Many patients who present with an acute migraine headache successfully can be treated with one of the many available therapeutic options. However, some patients may be much more difficult to treat and may in fact present with severe, intractable headaches (status migrainosus). Such patients may benefit from treatment with parenterally administered corticosteroids. In addition, corticosteroid treatment has been shown to decrease the duration of ophthalmoplegia and decrease pain in patients with ophthalmoplegic migraine.25 Corticosteroids also have been used in the treatment of more typical migraine head-aches. However, in general, steroid therapy should be reserved for those patients with more severe and intractable headaches.
Preventive Therapy. While most clinicians caring for a child with a migraine headache will focus on the immediate relief of symptoms, the clinician also should consider the use of preventive therapy for the child with frequent and severe headaches once the acute episode has been managed. In addition, many patients who receive treatment in the ED for an acute headache, and have relief of symptoms, will return to the ED within the next 48 hours with recurrence of symptoms. Therefore, preventive therapy, including not only the use of pharmacologic agents but also a complete assessment of the patient’s lifestyle and possible headache triggers, can help prevent patients from having recurrence of symptoms and can lead to an improvement in their daily lives.
Preventive therapy should begin with an assessment of the patient’s headache frequency and severity. While this may not be practical in an ED, headache calendars can be provided to families to document the frequency, severity, and associated symptoms of their child’s headaches and to identify potential triggers, environmental factors, and life stressors. The elimination of potential triggers should be the primary goal of migraine prophylaxis.
Once the physician has begun an investigation into the potential triggers of the child’s migraine headaches, attention can be turned to preventing future episodes. While avoiding potential triggers should be the ultimate goal of preventive therapy, this may not be practical, especially after an initial attack.
Both pharmacologic and nonpharmacologic preventive measures have been described in migraine prophylaxis in children. Nonpharmacologic preventive measures have been shown to reduce the frequency of migraine headaches in adults and may play a role in the management of migraine headaches in children. However, these measures have not been well studied in children.
Pharmacological agents used in migraine prophylaxis should be started only in collaboration with the child’s primary care physician. Migraine prophylactic medications should be considered when children are having more than two headaches per month that are treated inadequately with standard migraine medications, or if children are suffering from attacks that are so severe that their quality of life is impacted. Medications that have been used in migraine prophylaxis include beta blockers such as propranolol, calcium channel blockers, serotonin receptor antagonists, antidepressants such as tricyclic antidepressants, antiepileptics, NSAID agents, cyproheptadine, and sodium valproate.
When a decision has been made to begin prophylactic medications, medications should be started at a low dose and increased slowly. New medications should be tried for 1-2 months and tapered and discontinued once headaches are well controlled.
Beta-blockers are the most common medications used in migraine prophylaxis. Beta-blockers are thought to prevent migraine headaches by antagonism of serotonin receptors or through modulation of adrenoreceptors.81 Investigations that have evaluated the use of beta-blockers in the prevention of migraine headaches in children, however, have not shown consistent results, with some studies even suggesting that beta-blockers were no more effective than placebo in the prevention of migraine headaches.12,82 Therefore, it is not clear if beta-blockers should be routinely used for migraine prophylaxis in children. In addition, beta-blockers should not be used when patients have a history of reactive airway disease, diabetes mellitus, orthostatic hypotension, or cardiac disorders associated with bradyarrhythmias.
Both tricyclic antidepressants and selective serotonin re-uptake inhibitors have been used for migraine prophylaxis in children. The antimigraine effects of tricyclic antidepressants seem to be independent of their antidepressant effects. No controlled studies of the use of these agents in children or adolescents have been reported.
Cyproheptadine is an antihistamine with both antiserotonergic and calcium channel blocking properties. Cyproheptadine has been used widely for migraine prophylaxis in children. While safe and efficacious in young children, the medication is not well tolerated in adolescents. Cyproheptadine has been compared to placebo, propanolol, and a combination of cyproheptadine and propanolol in the prophylactic treatment of migraine headaches in children.83 While cyproheptadine reduced the frequency, duration and severity of migraine headaches as compared to placebo, the combination of cyproheptadine and propanolol provided the greatest relief. Cyproheptadine has a sedative effect in children and is also an appetite stimulant.
Sodium valproate long has been used as a prophylactic agent for adults with migraine headaches. However, pediatric studies have been limited. A recent study in children with migraines, however, suggests that sodium valproate may be highly effective and safe as a preventative medication.84 Topiramate, a broad-spectrum antiepileptic drug used for the treatment of multiple seizure types, also has been shown to be highly effective when used as a prophylactic agent for migraine headaches.85
Therapeutic Approach to the Child with a Migraine Headache
When a child presents to the ED with a headache, the first objective for the clinician is to determine if the headache is a symptom of a serious underlying disorder. Once the clinician determines that the headache does not herald a serious problem and decides that the headache is in fact a migraine, attention should be turned to treatment strategies.
The management of migraine headache in children should be individualized to the patient, taking into account the frequency and severity of attacks, the presence and degree of disability and the presence of associated symptoms such as nausea and vomiting. The patient’s history of, response to, and tolerance for specific medications also should be considered.
A reasonable first-line approach in a child who presents with a migraine headache, who is not vomiting and is able to tolerate oral medications, will be to treat first with ibuprofen. If treatment is unsuccessful, parenteral medications often will be given, in particular a combination of metoclopramide and ketorolac. If the child with a migraine headache presents with significant vomiting or cannot tolerate oral medications, parenteral medications will be given first. Again, first-line treatment consists of a combination of intravenous metoclopramide and ketorolac along with intravenous fluids.
If first-line parenteral therapy fails, and the child does not have a complex migraine, DHE would be the next agent of choice and the child would be admitted to the hospital for further treatment and observation. It is at this time that the neurology subspecialist often is consulted.
A recent trend is to use intravenous valproate when first-line therapy fails. Again, if a decision is made to use valproate, the patient will be admitted to the hospital, and the neurology subspecialists will be consulted.
Regardless of the treatment used to alleviate the migraine headache attack in the ED, patients who are discharged from the hospital will often be started on naproxen sodium as both prophylactic and acute therapy. In addition, parents will be encouraged to keep a headache diary to identify potential triggers of migraine attacks.
Summary
Migraine headaches are a common problem of childhood and are associated with significant morbidity, school absence, and lifestyle disruption. However, migraine headaches often are under recognized in the pediatric population and often are undertreated.
Migraine symptoms in children can vary dramatically in their character and severity. Diagnosis primarily is based on the patient’s history and a thorough physical examination. Laboratory and radiographic testing rarely, if ever, are required. Effective medications are available for the acute and prophylactic treatment of migraine headaches in children. However, most medications effectively have been studied only in adult patients. Currently, there are very few well controlled trials of migraine medications in children.
References
1. Forsyth R, Farrell K. Headache in childhood. Pediatr Rev 1999;20:39.
2. Winner PK. Headaches in children. When is a complete diagnostic workup indicated? Postgrad Med 1997;101:81.
3. May A, Ophoff RA, Terwindt GM, et al. Familial hemiplegic migraine locus on 19p13 is involved in the common forms of migraine with and without aura. Hum Genet 1995;96:604-608.
4. Wober-Bingol C, Wober C, Wagner-Ennsgraber C, et al. HIS criteria for migraine and tension-type headache in children and adolescents. Headache 1996;36:231-238.
5. Lipton RB, Stewart WF, Diamond S, et al. Prevalence and burden of migraine in the United States: Data from the American Migraine Study II. Headache 2001;41:646-657.
6. Hernandez-Latorre MA, Roig M. Natural history of migraine in childhood. Cephalalgia 2000;20:573-579.
7. Raskin NH. Migraine: Clinical aspects. In: Headache. 2nd ed. New York: Churchill Livingstone; 1988:41-98.
8. Bulloch B, Tenenbein M. Emergency department management of pediatric migraine. Pediatr Emerg Care 2000;16:196-204.
9. Moskowitz M. The visceral organ brain: Implications for the pathophysiology of vascular head pain. Neurology 1991;41:182.
10. Welch KMA, Barkley GL, Tepley N, et al. Central neurogenic mechanisms of migraine. Neurology 1993;43:S21.
11. Solomon GD. The pharmacology of medicines used in treating headaches. Semin Pediatr Neurol 1995;2:165.
12. Lewis DW, Scott D, Rendin V. Treatment of pediatric headaches. Expert Opin Pharmacother 2002;3:1433-1442.
13. Cano A, Palomeras E, Alfonso S, et al. Migraine without aura and migrainous disorder in children: International Headache Society (IHS) and revised IHS criteria. Cephalalgia 2000;20:617-620.
14. Barabas G, Ferrari M, Matthews WS. Childhood migraine and motion sickness. Pediatrics 1983;33:188.
15. Barabas G, Ferrari M, Matthews WS. Childhood migraine and somnambulism. Neurology 1983;33:948.
16. Raskin NH, Knittle SC. Ice cream headache and orthostatic symptoms in patients with migraine. Headache 1976;16:222-225.
17. Jan MMS and Al-Buhairi AR. Is infantile colic a migraine-related phenomenon? Clin Pediatr 2001;40:295-297.
18. Bruni O, Fabrizi P, Ottaviano S, et al. Prevalence of sleep disorders in childhood and adolescence with headache: A case-control study. Cephalalgia 1997;17:492-498.
19. Katerji MA, Painter MJ. Infantile migraine presenting as colic. J Child Neurol 1994;9:336-337.
20. Lewis DW, Ashwal S, Dahl G, et al. Practice parameter: Evaluation of children and adolescents with recurrent headaches. Report of the Quality Standards Subcomittee of the American Academy of Neurology and the Practice Committee of the Child Neurology Society. Neurology 2002;59:490-498.
21. Honig PJ, Charney EB. Children with brain tumor headaches: Distinguishing features. Am J Dis Child 1982;136:121-124.
22. Lewis DW, Dorbad D. The utility of neuroimaging in the evaluation of children with migraine or chronic daily headache who have normal neurological examinations. Headache 2000;40:629-632.
23. Maytal J, Bienkowski RS, Patel M, et al. The value of brain imaging in children with headaches. Pediatrics 1995;96:413-416.
24. Chu ML, Shinnar S. Headaches in children under 7 years of age. Ann Neurol 1990;28:433.
25. Rothner AD. Complicated migraine and migraine variants. Semin Pediatr Neurol 2001;8:7-12.
26. Lewis DW. Migraine and migraine variants in children and adolescents. Semin Pediatr Neurol 1995;2:127.
27. Carlow TJ. Oculomotor ophthalmoplegic migraine: Is it really migraine? J Neuro-Ophthalmol 2002;22:215-221.
28. Singer HS. Migraine headaches in children. Pediatr Rev 1994;15:94.
29. Al-Twaijri W, Shevell MI. Pediatric migraine equivalents: Occurrence and clinical features in practice. Pediatr Neurol 2002;26:365-368.
30. Fenichel GM. Migraine as a cause of benign paroxysmal vertigo of childhood. J Pediatr 1967;71:114-115.
31. Shevell M. A guide to migraine equivalents. Contemp Pediatr 1998;15:71.
32. Lanzi G, Balottin U, Fazzi E, et al. Benign paroxysmal vertigo childhood: A long-term follow-up. Cephalgia 1994;6:458.
33. Li BUK. Cyclic vomiting syndrome: Age-old syndrome and new insights. Semin Pediatr Neurol 2001;8:13-21.
34. Benson J, Zorn S, Book L. Sumatriptan (Imitrex) in the treatment of cyclic vomiting. Ann Pharmacol 1995;29:997-998.
35. Russell G, Abu-Arafeh I, Symon DN. Abdominal migraine: Evidence for existence and treatment options. Paediatric Drugs 2002;4:1-8.
36. Aaltonen K, Hmalainen ML, Hoppu K. Migraine attacks and sleep in children. Cephalalgia 2000;20:580-584.
37. Holden EW, Levy JD, Deichmann MM, et al. Recurrent pediatric headaches: Assessment and intervention. J Develop Behavior Pediatr 1998;19:109.
38. McGrath PJ, Humphreyes P, Goodman JT, et al. Relaxation prophylaxis for childhood migraine: A randomized placebo-controlled trial. Dev Med Child Neurol 1988;30:626.
39. McGrath PJ, Humphreys P, Keene D, et al. The efficacy and efficiency of a self-administered treatment for adolescent migraine. Pain 1992;49:321.
40. Hermann C, Blanchard EB, Flor H. Biofeedback treatment for pediatric migraine: Prediction of treatment outcome. J Consult Clin Psychol 1997; 65:611.
41. Allen KD, McKeen LR. Home-based multicomponent treatment of pediatric migraine. Headache 1991;31:467.
42. Baumann RJ. Behavioral treatment of migraine in children and adolescents. Paediatric Drugs 2002;4:555-561.
43. Lipton RB, Baggish JS, Stewart WF, et al. Efficacy and safety of acetaminophen in the treatment of migraine: Results of a randomized, double-blind, placebo-controlled, population-based study. Arch Intern Med 2000;160: 3486-3492.
44. Hamalainen ML, Hoppu K, Valkeila E, et al. Ibuprofen or acetaminophen for the acute treatment of migraine in children: A double-blind, randomized, placebo-controlled, crossover study. Neurol 1997;48:102-107.
45. Diamond S, Freitag FG. Do non-steroidal anti-inflammatory agents have a role in the treatment of migraine headaches? Drugs 1989;37:755.
46. Lewis DW, Kellstein D, Burke B, et al. Children’s ibuprofen suspension for the acute treatment of pediatric migraine. Headache 2002;42:780-786.
47. Shrestha M, Singh R, Moreden J, et al. Ketorolac vs chlorpromazine in the treatment of acute migraine without aura. A prospective, randomized, double-blind trial. Arch Int Med 1996;156:1725.
48. Davis CP, Torre P, Schafer N, et al. Ketorolac as a rapid and effective treatment of migraine headache: Evaluation by patients. Am J Emerg Med 1993;11:573.
49. Johnson ES, Ratcliffe DM, Wilkinson M. Naproxen sodium in the treatment of migraine. Cephalgia 1985;5:5.
50. Edmeads JG. Migraine. CMAJ 1988;138:107-113.
51. Ferrari MD. Sumatriptan in the treatment of migraine. Neurology 1993;43:S43.
52. Fuseau E, Petricoul O, Moore KH, et al. Clinical pharmacokinetics of intranasal sumatriptan. Clin Pharmacokinetics 2002;41:801-811.
53. Ueberall M. Sumatriptan in paediatric and adolescent migraine. Cephalalgia 2001;21(Suppl 1):21-24.
54. Ueberall MA. Intranasal sumatriptan for the acute treatment of migraine in children. Neurology 1999;52:1507-1510.
55. Winner PW, Rothner AD, Saper J, et al. A randomized, double-blind, placebo-controlled study of sumatriptan nasal spray in the treatment of acute migraine in adolescents. Pediatrics 2000;106:989-997.
56. Hershey AD, Powers SW, LeCates S, et al. Effectiveness of nasal sumatriptan in 5- to 12-year-old children. Headache 2001;41:693-697.
57. Macdonald JT. Treatment of juvenile migraine with subcutaneous sumatriptan. Headache 1994;34:581-582.
58. Linder S. Subcutaneous sumatriptan in the clinical setting: The first 50 consecutive patients with acute migraine in a pediatric neurology office practice. Headache 1996;36:419.
59. Coppola M, Yealy DM, Leibold RA. Randomized, placebo-controlled evaluation of prochlorperazine versus metoclopramide for emergency department treatment of migraine headache. Ann Emerg Med 1995;26:541.
60. Diener HC, Jansen JP, Reches A, et al. Efficacy, tolerability and safety of oral eletriptan and ergotamine plus caffeine (Caffergot) in the acute treatment of migraine: A multicentre, randomized, double-blind, placebo-controlled comparison. Euro Neurol 2002;47:99-107.
61. Geraud G, Compagnon A, Rossi A. The COZAM Study Group. Zolmitriptan versus a combination of acetylsalicylic acid and metoclopramide in the acute oral treatment of migraine: A double-blind, randomized, three attack study. Euro Neurol 2002;47:88-98.
62. Mathew NT. Use of rescue medication in trials of almotriptan versus placebo in the treatment of acute migraine. Clin Therapeutics 2002;24:520-529.
63. Winner P, Lewis D, Visser WH, et al. Rizatriptan 5 mg for the acute treatment of migraine in adolescents: A randomized, double-blind placebo-controlled study. Headache 2002;42:49-55.
64. Linder SL, Dowson AJ. Zolmitriptan provides effective migraine relief in adolescents. Int J Clin Pract 2000;54:466-469.
65. Totaro R, De Mattheis G, Marini C, et al. Sumatriptan and cerebral blood flow velocity changes during migraine attacks. Headache 1997;37:635-639.
66. Limmroth V, May A, Auerbach P, et al. Changes in cerebral blood flow velocity after treatment with sumatriptan or placebo and implications for the pathophysiology of migraine. J Neurol Sci 1996;138:60-65.
67. Klapper J, Mathew N, Nett R. Triptans in the treatment of basilar migraine and migraine with prolonged aura. Headache 2001;41:981-984.
68. Graf WD, Phillip SR. Pharmacologic treatment of recurrent pediatric headache. Pediatr Ann 1995;24:477.
69. Linder S. Treatment of childhood headache with Dihydroergotamine mesylate. Headache 1994;34:578.
70. Bell R, Montoya D, Shuaib A, et al. A comparative trial of three agents in the treatment of acute migraine headache. Ann Emerg Med 1990;19:1079.
71. Lane PL, McClellan BY, Baggoley CJ. Comparative efficacy of chlorpromazine and meperidine with dimenhydrinate in migraine headache. Ann Emerg Med 1989;18:360.
72. Sharma S, Prasad A, Nehru R, et al. Efficacy and tolerability of prochlorperazine buccal tablets in treatment of acute migraine. Headache 2002;42: 896-902.
73. Kabbouche MA, Vockell AL, LeCates SL, et al. Tolerability and effectiveness of prochlorperazine for intractable migraine in children. Pediatrics 2001; 107:E62.
74. Ellis GL, Delaney J, DeHart DA, et al. The efficacy of metoclopramide in the treatment of migraine headache. Ann Emerg Med 1993;22:191.
75. Volans GN. Research review migraine and drug absorption. Clin Pharmacokinet 1978;3:313.
76. Stillman MJ, Zajac D, Rybicki LA. The acute treatment of headaches with intravenous valproate. Neurology 2001;56(suppl. 3):A392.
77. Mathew NT, Kailasam J, Meadors L, et al. Intravenous valproate sodium (depacon) aborts migraine rapidly: A preliminary report. Headache 2000; 40:720-723.
78. Edwards KR, Norton J, Behnke M. Comparison of intravenous valproate versus intramuscular Dihydroergotamine and metoclopramide for acute treatment of migraine headache. Headache 2001;41:976-980.
79. Maizels M. Scott B, Cohen W, et al. Intranasal lidocaine for treatment of migraine. A randomized, double-blind, controlled trial. JAMA 1996;276:319.
80. Blanda M, Rench T, Gerson LW, et al. Intranasal lidocaine for the treatment of migraine headache: A randomized, controlled trial. Acad Emerg Med 2001; 8:337-342.
81. Wasiewski WW. Preventive therapy in pediatric migraine. J Child Neurol 2001;16:71-78.
82. Solomon GD. Pharmacology and use of headache medications. Cleve Clin J Med 1990;57:627-635.
83. Rao BS, Das DG, Taraknath VR, et al. A double-blind controlled study of propranolol and cyproheptadine in migraine prophylaxis. Neurol India 2000;48: 223-226.
84. Serdaroglu G, Erhan E, Tekgul H, et al. Sodium valproate prophylaxis in childhood migraine. Headache 2002;42:819-822.
85. Storey JR, Calder CS, Hart DE, et al. Topiramate in migraine prevention: A double-blind, placebo-controlled study. Headache 2001;41:968-975.
Children often present to the emergency department complaining of headaches. While most headaches in children are not signs of serious, underlying disorders, some headaches may be the first presentation of a migraine headache. Migraine is the most common cause of recurrent, intermittent headaches in children. However, migraine headaches often are underdiagnosed and undertreated in children.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.