The WHI Reports on Fracture and Gynecologic Cancers
Abstracts & Commentary
The Women’s Health Initiative (WHI) reports that estrogen-progestin therapy reduces fractures, but the number of gynecologic cancers observed precludes a definitive statement on the risk of endometrial and ovarian cancers.
The report on fractures from the canceled arm of the WHI was based on an average of 5.6 years of follow-up, comparing placebo treatment with daily 0.625 mg conjugated estrogen and 2.5 mg medroxyprogesterone acetate (see Table 1).
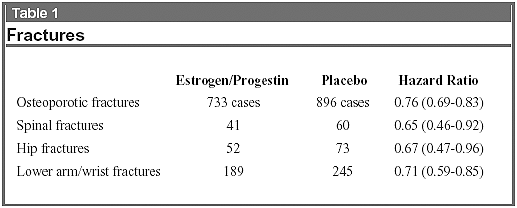
The WHI concluded the reduction in fractures was not great enough to alter their position that hormone therapy had no net benefit on their model of the global risk:benefit ratio. The gynecologic cancer diagnoses are listed in Table 2.
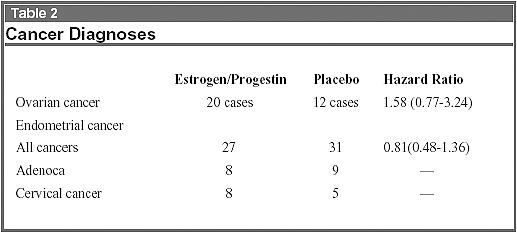
The WHI concluded that combined estrogen-progestin treatment prevented the increase in endometrial cancer associated with unopposed estrogen, and that this treatment may increase the risk of ovarian cancer. Not unexpectedly, the women in the treated group underwent interventions (biopsies and ultrasound) at a greater rate. (Cauley J, et al. JAMA. 2003;290:1729-1738; Anderson GL, et al. JAMA. 2003;290:1739-1748).
Comment by Leon Speroff, MD
The Fracture Report
There are reasons to believe that the impact of hormone therapy could be greater than reported by the WHI. The Kaplan-Meier estimates of the impact of hormone therapy indicated that the reduction in fractures continued to increase over time, suggesting that a very powerful effect would be achieved with treatment of a long duration. In addition, spinal fractures included only clinically symptomatic fractures (known to represent about one-third of vertebral fractures); again the overall effect was probably greater if all vertebral fractures had been included. The beneficial effect was achieved even though the use of a bisphosphonate increased from 1% at baseline to about 6% in the hormone group and 10% in the placebo group. The effect would have been even greater if bisphosphonates had not been prescribed by the participants’ clinicians. The reduction in fractures was also underestimated because the WHI participants were not selected to obtain a group of women at high risk for fracture, but to the contrary, these women overall were at low risk for fractures.
The diagnoses of hip fracture in this update were centrally adjudicated, resulting in a 6% disagreement. Whether this was balanced or favored one group or another is not shared with us.
There are some puzzling conclusions. For example, the report states that there was no evidence that the effect differed by years since menopause. However, the reduced risk of hip fracture was 0.58 (0.36-0.94) for women 20 or more years since menopause in contrast to a nonsignificant 0.80 (0.42-1.53) in women 10-19 years since menopause. The report states that there was no evidence of an interaction between treatment and race/ethnicity, but at the same time it is pointed out that the small number of fractures in the subgroups limited meaningful conclusions.
The report stated that hormone therapy decreased the risk of hip fracture by 60% among women with adequate calcium intake at baseline, but not in those with a lower intake. This underscores the importance of emphasizing to patients the consequences of inadequate calcium and vitamin D intake. The effect of hormone therapy was greater in leaner women, as one would expect.
Most importantly, the WHI concluded in the discussion that the fracture results indicated that this benefit did not outweigh the risks of cardiovascular disease and breast cancer. However, this conclusion could be influenced by several important points. The conclusion depends upon the judgment that the global index created by the WHI is a valid measure. For example, vertebral fractures were not included in the WHI global index. The cardiovascular risk was derived from the initial July 2002 report and not from the updated report a year later where after central adjudication the results were no longer statistically significant.1 In addition, because the WHI trial underestimated the impact of hormone therapy on fractures, a more representative population may have yielded a greater overall benefit. Finally, the WHI buttresses its conclusion with their previous report of a two-fold increase in dementia among older, treated women. However, keep in mind that the only statistically significant finding was increased dementia in elderly women (75 and older) who had been exposed to a relatively short term of estrogen-progestin therapy, and that this was vascular dementia, not Alzheimer’s.2
The GYN Cancer Report
The strength of the gynecologic cancer report is diluted by the small number of cases. To respond to this publication as if hormone therapy increases the risk of ovarian cancer, as some media reports did, is not justified. The WHI appropriately concludes that this is a worrisome issue and requires further epidemiologic assessment. A major problem is that the risk of ovarian cancer is influenced by so many factors. The WHI report stated that many observational studies have found a modest increase in the risk of ovarian cancer, but in fact most studies have not, and those reporting an increased risk have been plagued by incredibly small numbers making it impossible to control for all influencing factors.
The WHI found no interaction with previous oral contraceptive use, parity, family history of breast, ovarian, or colorectal cancer, and the WHI appropriately observed that the power to examine these relationships was too limited by the small number of cases. Thus even its overall conclusion regarding ovarian cancer could be modified by a shift of a few cases. Only greater numbers and longer duration of treatment could clarify this subject; for example, there were 2 cases of endometrioid ovarian cancers in the treated group and none in the placebo group, a result that should be reversed, and I believe a reversal would ultimately be achieved.
The results with endometrial cancer are also hampered by small numbers. Note that adenocarcinoma of the endometrium (the cancer most likely to be affected by estrogen-progestin therapy) accounted for only 8 cases in the treated group of 8506 subjects and 9 in the placebo group of 8102 subjects. The literature on hormone therapy and the risk of endometrial cancer does not suggest that a beneficial reduction in risk with estrogen-progestin combined treatment should be expected within a time period of a few years.
Conclusion
These 2 reports from the WHI should have no appreciable effect on current decision-making regarding postmenopausal hormone therapy. The reduction in fractures associated with hormone therapy agrees with the accumulated literature (although it probably underestimates the impact). The effect on the risk of endometrial cancer is consistent with what we have learned from smaller trials, case-control studies, and cohort follow-up reports. The effect of hormone therapy on the risk of ovarian cancer remains an unsettled issue, although the majority of case-control studies find no increase. It is noteworthy that the media highlighted ovarian cancer and neglected the good news in the report on fractures, especially because the prevalence, mortality, and morbidity of osteoporotic fractures in postmenopausal women add up to one of the most expensive and important health problems in modern life.
Dr. Speroff is Professor of Obstetrics and Gynecology Oregon Health Sciences University Portland.
References
1. Manson JE, et al. N Engl J Med. 2003;349:523-534.
2. Shumaker SA, et al. JAMA. 2003;289:2651-2662.
The Womens Health Initiative (WHI) reports that estrogen-progestin therapy reduces fractures, but the number of gynecologic cancers observed precludes a definitive statement on the risk of endometrial and ovarian cancers.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
