ECG Review: A Harbinger of Tachycardia
ECG Review: A Harbinger of Tachycardia
By Ken Grauer, MD
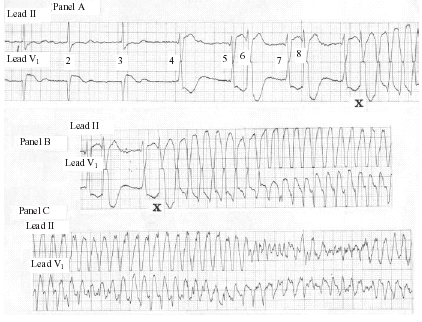
Figure. Series of consecutive rhythm strips obtained from an older woman on multiple medications.
Clinical Scenario: The series of consecutive rhythm strips shown in Panels A, B, and C of the Figure were obtained from an elderly woman on multiple medications including digoxin. She was admitted to the hospital for decreased level of consciousness and recent MI. Are events leading up to the tachycardia that begins with beat X what you would expect? How would you treat this patient?
Interpretation: The rhythm in Panel A begins with atrial fibrillation and a slow ventricular response for the first three beats on the tracing. QRS morphology changes with beat four that looks to be the beginning of a short run of accelerated idioventricular rhythm (AIVR). AIVR is punctuated by several premature ventricular beats from a different focus (beats six and eight) before the onset of the tachycardia that starts with beat X. Thereafter follows an extremely rapid rhythm with changing QRS morphology. This is torsades de pointes. As implied by its name ("twisting of the points"), widened QRS complexes with alternating polarity (initially positive in lead V1—then negative—then rapidly alternating) persist for the rest of the rhythm strip sequence.
Torsades de pointes often (though not invariably) is associated with a prolonged QT interval on the patient’s baseline 12-lead ECG. Nonspecific ST-T wave flattening in lead II of Panel A during the patient’s spontaneous rhythm (beats one, two, and three) precludes accurate determination of the QT interval. Uncertainty about where the T wave ends in lead V1 precludes use of this lead for QT determination, such that without access to a baseline 12-lead ECG tracing, no comment can be made as to whether the QT interval is prolonged. Not commonly appreciated is the precipitating role of preceding bradycardia for initiating episodes of torsades (preceding bradycardia prolongs the subsequent repolarization period and QT interval, and may be contributing to development of torsades in this case).
The key measures for treating torsades include: 1) finding and correcting a precipitating cause whenever possible (e.g., hypokalemia or use of a medication that might further lengthen the QT interval); and 2) administration of magnesium sulfate, often in high dose (1-2 grams IV, which may be repeated several times or given by continuous IV infusion). Magnesium remains the medical treatment of choice for torsades, regardless of whether the patient has pre-existing hypomagnesemia. Overdrive pacing may also be considered if there is no response to repeated magnesium. Finally, while recognizing that torsades is not a common manifestation of digoxin toxicity, this medication should clearly be stopped in a patient with this tachyarrhythmia.
Clinical Scenario: The series of consecutive rhythm strips shown in Panels A, B, and C of the Figure were obtained from an elderly woman on multiple medications including digoxin.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
