Foolproof ways to improve physician handwriting
Process at medical center impresses JCAHO
During a recent Joint Commission on Accredita-tion of Healthcare Organizations (JCAHO) survey at Regional Medical Center of Orangeburg (SC) and Calhoun Counties, surveyors were very impressed with the process developed to assess and improve physician handwriting, reports Indun Whetsell, the facility’s director of quality management.
"We have done a lot in this area," she says. "Some physicians were very unhappy about the changes we made, but the Joint Commission was very pleased. It’s not an easy thing to do, and we did incur some wrath, but it’s very much worth it."
Here are some effective ways to improve physician handwriting:
• Perform random audits.
"We are addressing physician legibility full force," says Larry Dunham, RHIA, director of health information management at Baylor Uni-versity Medical Center in Dallas. He explains that physicians are subject to "legibility audits," which are done by random selection.
"Our goal is to review each of our active medical staff members within the year, which is aggressive based on our size," says Dunham.
Pharmacy has teamed up with health information management to screen 100% of all orders for legibility, he adds.
Illegible orders are clarified with the physician prior to any order being carried out related to medication administration, Dunham says. "All cases that they deem illegible are routed to us for further review and investigation."
The following criteria for medication orders are used:
- Name, dose, route, frequency included?
- Order legible?
- Order signed?
- Signature legible and/or transcription (physician) number included?
- Date included?
- Are abbreviations used? And if so, are they approved?
Health information management pulls the records, and the facility’s Center for Quality Care Coordination reviews them clinically to determine the impact on patient care, if any, Dunham says.
Regardless of whether the review is positive or negative, each physician receives a letter from the hospital’s chief of staff, he says. Physicians who have met all the criteria are alerted that their records were reviewed and found to be in good order. If a physician doesn’t meet the criteria, he or she receives a letter stating the findings and that the findings will result in further review.
• Have physicians use ID numbers with their signatures.
Physicians are encouraged to use their hospital-assigned identification numbers alongside their signatures for written orders, says Whetsell.
"We made copies of many doctor’s signatures and handed them out at the medical staff meeting — where they couldn’t read the names either!" she says. "This was a great visual aid."
• Send samples to be graded by anonymous reviewers.
At Regional Medical Center, handwriting samples were taken for all members of the medical staff, and copies were sent to three anonymous reviewers, consisting of a physician, nurse, and medical records director, to be graded on a "pass" or "fail" basis. (See Handwriting Analysis Flowchart, below.)
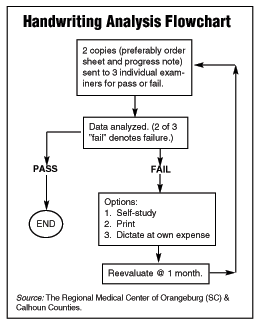
If the physician is failed by two or more reviewers, they are given the options of taking a remedial course, printing all orders, or dictating at their own expense, says Whetsell, who adds that handwriting is reevaluated every six months for all physicians. "This has made a huge difference in some physicians’ handwriting," she says.
• Routinely monitor compliance with the medical staff’s handwriting policies.
The monitoring of medical records is completed quarterly as part of the hospital’s multidisciplinary chart reviews, Dunham adds.
Retrospective review also is done and is trended by physician to monitor any ongoing issues, he says. Physicians are notified to let them know that their documentation was screened and was secondarily reviewed for quality issues. If no problems are identified, the physicians are notified of this and informed that review will continue, along with ongoing education on legibility requirements.
• Take action when a physician repeatedly fails to comply with the legibility requirements.
If the physician fails, he or she is notified that further review will take place, Dunham says. "We also educate them on what we are looking for, and what the penalties may be if they do not show marked improvement."
If no improvement is, penalties include:
- Physician must pay for transcription of all notation.
- Physician must take handwriting course work.
- Physician must pay for scribes to make readable notations.
"If marked improvements are not seen through these means, the physician will be removed from the medical staff and will lose all privileges to care for patients at this facility," Dunham says.
During a recent Joint Commission on Accredita-tion of Healthcare Organizations (JCAHO) survey at Regional Medical Center of Orangeburg (SC) and Calhoun Counties, surveyors were very impressed with the process developed to assess and improve physician handwriting, reports Indun Whetsell, the facilitys director of quality management.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
