Readers share views on common OC challenges
Readers share views on common OC challenges
The next patient on your schedule is a 41-year-old woman who smokes 12-15 cigarettes a day. She would like to use combined oral contraceptives (OCs). Will she leave your office with a prescription for the Pill?
If results of Contraceptive Technology Update’s 2003 Contraception Survey are any indication, she’ll be offered another form of birth control. The majority of 2003 survey respondents say they will not provide pill prescriptions for older women who smoke 10 cigarettes a day. For women ages 35-39, about 76% say they will not supply OCs, and for women ages 40 and older, the number climbs to almost 90%. These findings closely follow those found in the 2002 survey responses.
Use the "4 As" in your clinical approach when it comes to smoking:
• Ask all patients about smoking.
• Advise all patients to quit.
• Assist with motivation and assess nicotine dependence.
• Arrange for a follow-up appointment.1
When talking with patients, find out how much they smoke, how ready they are for a change, whether they have tried to quit in the past, and their motivation for smoking cessation. For women who continue to smoke, counsel on use of intrauterine devices or progestin-only methods.2
What is your approach to providing combined pills for a new mother who chooses not to breast-feed? About 39% of 2003 CTU survey respondents say they would prescribe OCs four to six weeks postpartum, a decrease from 2002’s 46% level. About 29% say they would initiate OCs one to three weeks postpartum, with 10% providing pills upon hospital discharge. About 10% would start pills at first menses, with about 7% using other approaches. These views are consistent with those reported in the 2002 survey.
For new mothers who wish to breast-feed, about 36% of respondents say they would begin progestin-only pills (POPs) at four to six weeks postpartum, a slight decline from 2002’s 44.4% figure. A total of 26% note they would initiate POPs at one to three weeks postpartum. About 20% would initiate POP use at hospital discharge, with about 2% starting minipills at first menses. About 7% say they would use other approaches.
Review the stance of the Elk Grove Village, IL-based American Academy of Pediatrics about OC use in breast-feeding women, advises Anita Nelson, MD, professor in the obstetrics and gynecology department at the University of California in Los Angeles (UCLA) and medical director of the women’s health care clinic and nurse practitioner training program at Harbor-UCLA Medical Center in Torrance.3 The AAP is comfortable with combined OC use once women have introduced another source of calories into the infant’s diet, she notes.
Which OC for nausea?
For women who have experienced bothersome nausea on previous OCs, but can’t remember the brand name of the pill used, clinicians continue to use Alesse, a monophasic 20-mcg pill from Wyeth-Ayerst Laboratories of Philadelphia. About 54% named the pill as their first choice in this category, and the percent was up from 2002’s 49.7% figure.
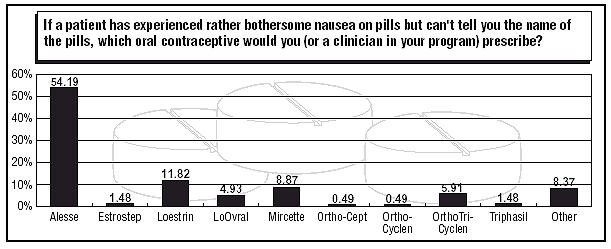
Alesse is the first-choice OC for patients who have experienced nausea with previous pills, reports Patricia Bauer, MSN, RNC, a nurse practitioner at the Benzie Leelanau District Health Department in Benzonia, MI. The pill is the lowest estrogen effect pill that the agency carries, she notes.
Other pills named as first choices in the 2003 survey include Loestrin 1/20, a 20-mcg monophasic pill from Pfizer of New York City, and Mircette from Organon of West Orange, NJ, a pill with a unique dosing schedule (21 days of 150 mcg desogestrel/20 mcg ethinyl estradiol, two days of placebo pill, followed by five days of 10 mcg ethinyl estradiol). About 12% of 2003 survey respondents chose Loestrin, compared to 20.2% in 2002, while about 9% named Mircette, compared to 10.2% in 2002.
References
1. Manley M, Epps RP, Husten C, et al. Clinical interventions in tobacco control: A National Cancer Institute training program for physicians. JAMA 1991; 266:3,172-3,173.
2. Kaunitz AM. Oral contraceptives, smoking, and the risk for myocardial infarction. Journal Watch Women’s Health 2002. Accessed at: womens-health.jwatch.org/cgi/content/full/2002/219/1.
3. Committee on Drugs. American Academy of Pediatrics: The transfer of drugs and other chemicals into human milk. Pediatrics 2001; 108:776-789.
The next patient on your schedule is a 41-year-old woman who smokes 12-15 cigarettes a day. She would like to use combined oral contraceptives (OCs). Will she leave your office with a prescription for the Pill?Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
