Health care worker illness may be the clue to next SARS outbreak
Health care worker illness may be the clue to next SARS outbreak
EHPs should monitor employees with pneumonia
Health care workers with pneumonia may be the sentinels for a new outbreak of severe acute respiratory syndrome (SARS). Faced with the dilemma of identifying the first suspected cases of SARS amid a backdrop of widespread, seasonal respiratory illness, public health authorities are urging hospitals to monitor their employees’ health.
Hospitals should report clusters of two or more health care workers involved in direct patient care who have pneumonia that was confirmed through chest X-rays to their local or state health department, the Centers for Disease Control and Prevention (CDC) says in draft recommendations.
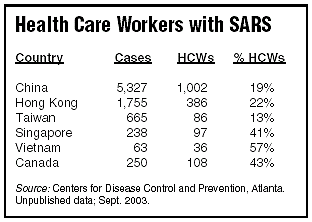
Most likely, those health care workers won’t have SARS. But with no reliable laboratory test that can be used as a diagnostic tool, SARS surveillance depends on astute observance of patterns, CDC medical epidemiologists said. Being a health care worker was one of the greatest risk factors in the past outbreak, which sickened more than 1,700 health care workers in the six hardest-hit countries. (See chart, below)
"It’s going to be the combination of clinical and epidemiologic features that’s going to be the key in identifying SARS," says John Jernigan, MD, MPH, medical epidemiologist in the CDC division of healthcare quality promotion and a member of the CDC’s SARS Preparedness Task Force. (Editor’s note: One case of SARS was confirmed in September in a medical researcher in a laboratory in Singapore. The CDC and other international health agencies now are reviewing biosafety precautions.)
If SARS recurs, U.S. hospitals may not be as fortunate as they were in the past outbreak. Last winter, only eight U.S. patients had laboratory-confirmed cases of SARS, including one health care worker. Yet an unpublished CDC survey of 110 health care workers involved in their care revealed numerous unprotected exposures.
Some 44% of health care workers entered a patient room or were within 10 feet of a patient without wearing a mask. A similar proportion (40%) of those with exposure to a coughing patient failed to wear a respirator, and 39% had direct contact with one of the SARS patients without wearing gloves.
Goggle use was the most neglected form of protective equipment (PPE); 70% of the health care workers surveyed said they provided care for a SARS patient without wearing goggles.
The confirmed SARS patients had less severe illness, and few required droplet- or aerosol-producing procedures, such as intubation or bronchoscopy, compared with those in countries that suffered from hospital-based outbreaks. "The bottom line is we don’t know why [the U.S. experience differed from that of Canada, Hong Kong, and other countries]," says L. Clifford McDonald, MD, a CDC medical epidemiologist and SARS task force member. "There was a lack of transmission to health care workers despite opportunity."
Worldwide, hospitals were a major focus of SARS transmission, not just among health care workers, but of patients and visitors, as well. For example, in Toronto, 28% of all suspected and probable cases occurred among hospital patients and visitors.
Now the CDC is focused on improving SARS preparedness in hospitals. At a meeting with representatives from leading health organizations, including the World Health Organization, Health Canada, the American Hospital Association, the Joint Commission on Accreditation of Healthcare Organizations, the American College of Occupational and Environmental Medicine, and other physician organizations, the CDC solicited ideas about how to prevent hospital spread if SARS recurs.
"We need some new initiatives in terms of early recognition," McDonald adds. "When the hospitals recognize the patients early on, there is going to be less exposure. . . . We [also] need to redouble our educational efforts to get people to use the personal protective equipment."
Early detection and protection — those key responsibilities will involve employee health, along with infection control. Hospitals should report any cluster (two or more cases) of confirmed pneumonia among health care workers to the health department, CDC officials say.
Physicians should evaluate the cases for an alternative diagnosis. If none is found after 72 hours, they should consult with the health department and consider SARS testing, according to the draft recommendations.
Abnormal chest X-rays are a key clinical feature of the disease. For example, all of the U.S. patients with laboratory-confirmed SARS had abnormal chest X-rays by day 10. "It appears this is pneumonic illness almost exclusively," Jernigan says.
The logistics of monitoring health care workers may be difficult, particularly since some are contract employees. It requires follow-up of workers who are hospitalized with pneumonia of unknown etiology, CDC officials explain.
Hospitals and physicians should add the question "Are you a health care worker?" to their work-up of patients with pneumonia, Jernigan adds.
CDC is tailoring its recommendations to the level of SARS activity worldwide, in the community, and in the facility, from category 0 (no cases) to category 3 (nosocomial spread with no clear source). The presence of SARS in the community brings more intense surveillance of employee illness. For example, at Scarborough Grace Hospital in suburban Toronto, employee health professionals contacted all health care workers who were considered at risk because of possible contact with a SARS patient. They regularly screened employees for SARS symptoms. That surveillance of health care workers led to the detection of a second phase of the SARS outbreak, after Toronto officials believed the disease was under control.
CDC also advocates more widespread use of contact precautions. Every patient presenting with respiratory symptoms should be given a surgical mask to prevent droplet spread, CDC officials advised. Triage nurses and emergency department (ED) staff may choose to wear masks to provide additional protection.
In the first days of the SARS illness, the symptoms may be mild and vague, such as fever, aches, chills, and headache. Only 30% of SARS patients have respiratory symptoms at the onset of the disease, Jernigan says. "There’s going to be no way to tell who has SARS and who doesn’t," he says. "It’s going to be the epidemiologic link [that’s important]."
The antibody response may take up to 28 days to reach a detectable level. And the PCR test, which measures that antibody response, has a low specificity when there are few or no confirmed cases of SARS worldwide. In other words, sporadic reports of SARS infection may reflect false positives, CDC officials point out.
With that in mind, EDs may need to reevaluate their overall approach to PPE, explains Henry Siegelson, MD, FACEP, an emergency physician at WellStar Cobb Hospital in Austell, GA, and clinical assistant professor of emergency medicine at Emory University in Atlanta. Siegelson, who represented the American College of Emergency Physicians at the CDC meeting, says information presented about SARS transmission is influencing his attitude toward PPE.
"Based upon the potential consequences of uncontrolled nosocomial infection, we need to be proactively involved in [prevention]," he says. "I think when you go into the clinic environment in the emergency department, where you have contact with the family and with patients, you should wear contact precautions."
In the past SARS outbreak, questions arose about the appropriate use of PPE. The CDC is still developing guidance on what protection health care workers should wear and when they should wear it. But the draft recommendations reflect one conclusion: PPE and hand hygiene can prevent spread of SARS — if employees are vigilant.
The CDC recommends the use of standard, contact, and airborne precautions, which include goggles, gloves, gowns, and respiratory protection. (The use of head covers and shoe covers has not been recommended.)
"Experience has shown that rigid adherence to infection control procedures is essential in controlling outbreaks of SARS, and that even minor lapses in technique can lead to transmission," the CDC draft recommendations state.
How employees don the gear, or even how they remove it, may not be the key concern, as long as they practice hand hygiene to prevent self-contamination, says Linda Chiarello, RN, MS, of CDC’s division of healthcare quality promotion.
"What’s more important is how people are wearing it," she says. "People touch their eyes; they touch their face. They’re not aware of it."
Hospitals should provide education about the use of PPE, including N95 fit-testing, CDC advises. They should also consider the staffing that would be required to treat SARS patients, allowing for employees to take breaks and remove the PPE, Chiarello adds. "People were absolutely exhausted [after wearing PPE]. People need to be able to get out of the [SARS-affected] area."
PPE is just one facet of an overall SARS preparedness plan. Here are some other considerations, according to CDC:
- SARS preparedness may be incorporated into preparedness plans for smallpox or other infectious disease emergencies, such as pandemic influenza.
- Coordination with public health departments to create communitywide planning is crucial.
- Hospitals should plan for different scenarios. What would happen if a SARS patient comes to the ED? What if you realize an existing patient has SARS?
- Assessment of staffing needs should include housekeeping. Hospitals may consider training staff designated to clean SARS patient rooms.
- Hospitals should have a plan for screening patients, visitors, and health care workers on entry to the facility, if that should be indicated due to concerns about SARS transmission.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
