Special Feature - The Electrocardiogram in Wolff-Parkinson-White Syndrome Part II: The Arrhythmias
The Electrocardiogram in Wolff-Parkinson-White Syndrome Part II: The Arrhythmias
By William J. Brady, MD
Wolff-Parkinson-White syndrome (WPW) is a well-described form of ventricular pre-excitation. In 1930, Wolff, Parkinson, and White described the "combination of bundle branch block, abnormally short PR interval, and paroxysms of tachycardia occurring in young, healthy patients with normal hearts."1 This syndrome involves an accessory conduction pathway, termed the bundle of Kent. The bundle of Kent bypasses the atrioventricular (AV) node, creating a direct electrical connection between the atria and ventricles. The importance of recognizing this syndrome is that WPW patients are prone to develop a variety of tachyarrhythmias which may lead to unpleasant, disabling symptoms and, in the extreme, sudden cardiac death. The vast majority of patients with ventricular pre-excitation remain asymptomatic; in those patients who develop symptoms related to pre-excitation, tachyarrhythmias are responsible. Reentrant tachyarrhythmias (paroxysmal supraventricular tachycardia or PSVT) account for most presentations (70%) followed by atrial fibrillation (25%) and less frequently by atrial flutter (< 5%); fortunately, ventricular fibrillation is a highly unusual complication of the previously diagnosed and properly managed patient. (See Figure 1.) The physiology of ventricular pre-excitation and related findings on the non-arrhythmic ECG were discussed in Part I of this article (Emerg Med Alert 2003;9:68-70).
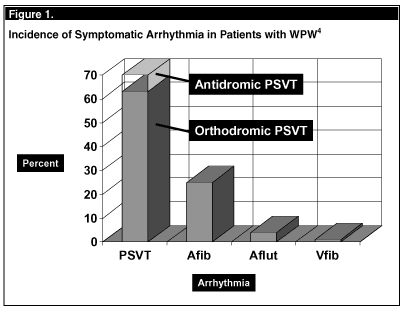
The most frequently encountered arrhythmia seen in WPW is PSVT, also referred to as AV reciprocating tachycardia. In this instance, activation of the ventricle occurs through either the normal conduction system or the accessory pathway with return of the impulse to the atrium by the other pathway. The particular path chosen by the individual arrhythmia determines not only the nomenclature used to describe the rhythm disturbance but also the electrocardiographic findings and level of clinical concern. Regarding terminology, such PSVT is referred to as either orthodromic (antegrade conduction via the AV node) or antidromic (retrograde conduction via the AV node).
The orthodromic AV reciprocating tachycardia is a re-entrant tachycardia in which the atrial stimulus is conducted to the ventricles through the AV node with a return of the impulse to the atria through the AP. (See Figure 2A.) Such tachycardia represents approximately 90% of PSVT cases seen in the WPW patient. The electrocardiographic characteristics of this tachycardia include a regular, narrow QRS complex without a delta wave, in that the ventricles are being activated through the normal conduction pathway. (See Figure 2A.) In a relative sense, the AV node is able to control the ventricular rate, which ranges from 160-220 bpm in the adult and 160-260 bpm in the child.
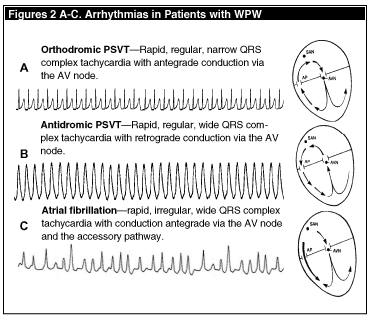
In approximately 10% of PSVT patients with WPW, an antidromic (retrograde) reciprocating tachycardia is observed. In this instance, the re-entrant circuit conducts in the opposite direction, with anterograde conduction down the AP and retrograde return of the impulse to the atria via the AV node. (See Figure 2B.) With this pathway, the QRS complexes appear wide (a pronounced delta wave). The ECG demonstrates a very rapid, regular, wide-complex tachycardia; this arrhythmia is nearly indistinguishable from ventricular tachycardia. (See Figure 2B.) Atrial fibrillation occurs in up to 20% of patients with symptomatic arrhythmia and WPW.2 In patients with normal conducting systems, the AV node acts to slow conduction and prevents the transmission of the rapid atrial beats to the ventricles—essentially, the AV node "protects" the ventricles from excessive rates. Accessory pathways, however, lack the feature of slow, decremental conduction—thus the pathway can conduct atrial beats at a rate that can approach or exceed 300 bpm, subjecting the ventricle to very rapid rates. (See Figure 2C.) With ventricular responses at or above 300 beats per minute, the risk of ventricular fibrillation is greatly increased—due not only to the poor coronary and systemic perfusion which results from such excessive ventricular rates but also to the arrival of a subsequent depolarization while the heart is repolarizing from the previous cycle—in essence, the R-on-T phenomenon.3 The features suggestive of atrial fibrillation with preexcitation are the irregularity of the rhythm, the rapid ventricular response (much too rapid for conduction down the AV node) and the wide, bizarre QRS complex, signifying conduction down the aberrant pathway.
Ventricular fibrillation in the setting of pre-excitation presents in similar fashion to the non-WPW scenario. When the patient presents with arrhythmia, the diagnosis of WPW may not be known nor apparent due to the arrhythmia. The rhythm scenarios and/or features should suggest, not confirm, the diagnosis of WPW:
• Rapid, regular, narrow QRS complex tachycardia with ventricular rate greater than 220 bpm for adults, greater than 240-260 bpm for children;
• Rapid, irregular, widened QRS complex tachycardia with ventricular rate greater than 180 bpm, beat-to-beat variation in QRS complex morphologies, and/or bizarre QRS complex morphologies; and
• In the setting of any tachyarrhythmia, excessively high ventricular rates and/or widened QRS complex.
Dr. Brady, Associate Professor of Emergency Medicine and Internal Medicine, Vice Chair, Emergency Medicine, University of Virginia, Charlottesville, is on the Editorial Board of Emergency Medicine Alert.
References
1. Wolff L, et al. Bundle-branch block with short PR interval in healthy young people prone to paroxysmal tachycardia. Am Heart J 1930;5:685-704.
2. Sheinman BD, et al. Acceleration of ventricular rate by amiodarone in atrial fibrillation associated with Wolff-Parkinson-White syndrome. BMJ 1982;285:999-1000.
3. Klein GJ, et al. Ventricular fibrillation in the Wolff-Parkinson-White syndrome. New Engl J Med 301; 1979:1080-1085.
4. Colovita PG, et al. Frequency, diagnosis and clinical characteristics of patients with multiple atrioventricular APs. Am J Cardiol 1987;59:601-606.
When the patient presents with arrhythmia, the diagnosis of Wolff-Parkinson_White (WPW) may not be known nor apparent due to the arrhythmia. The rhythm scenarios and/or features should suggest, not confirm, the diagnosis of WPW.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
