West Nile Virus: Sound the Alarm from Coast to Coast
Abstract & Commentary
Source: Centers for Disease Control and Prevention. Provisional surveillance summary of the West Nile virus epidemic-United States, January-November 2002. MMWR Morb Mortal Wkly Rep 2002;51:1129-1133.
West Nile virus (WNV) erupted unexpectedly in the United States in 1999 with an outbreak among residents of New York City. Intense and systematic clinical, epidemiologic, and public health investigation followed, and publication of the analysis of 59 hospitalized patients provided guidance for recognition of additional cases. In conjunction with the Centers for Disease Control and Prevention (CDC), the ArboNet surveillance network of state and local public health departments was established to monitor WNV activity reported in humans, animals, and mosquitoes during the ensuing three years.
The facts from this database are alarming. From a single epicenter of human cases in 1999, WNV all-source activity has now expanded south- and westward in dramatic fashion to involve 44 states plus Washington, DC, by the conclusion of 2002. In striking contrast to the 149 cases of human WNV infection in 10 states reported for the three-year period of 1999-2001, the reported number of cases for 2002 alone totaled 3389, among whom 2354 (69%) suffered from the most invasive manifestation, West Nile meningoencephalitis (WNME). Of these, 199 (9%) died. Taken together, these data sound a sobering note for our nation: since 1999, a total of 3955 cases of West Nile infection (either febrile illness (WNF) alone or WNME) have been documented across 37 states, with 254 deaths. This represents the largest arboviral meningoencephalitis epidemic ever observed in the western hemisphere, eclipsing the 1975 outbreak of a related flavivirus, St. Louis encephalitis, which swept through the midwestern United States. Furthermore, this is the largest WNME epidemic ever reported worldwide.
Commentary by Michael Felz, MD
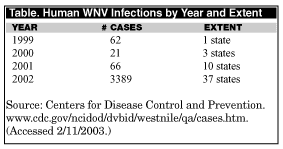
Since the last review of WNV in this publication (Emerg Med Alert 2002;9:25-26), this emerging mosquito-borne epidemic has expanded dramatically. (See table.) The explosive quantity, severity, and geographic range of human infection in America are worrisome indeed. Equally disturbing is ArboNet surveillance data demonstrating that WNV has now been detected in a total of 44 states among 111 species of birds (chiefly crows, blue jays, and raptors), nine mammalian species (primarily humans and horses, but also dogs, cats, squirrels, rabbits, skunks, chipmunks, and bats), and 36 species of mosquitoes (mainly Culex, but also Aedes and Anopheles).
From the standpoint of the emergency department (ED) physician, WNV must now be centered prominently in the differential diagnosis of patients presenting with ever, headache, vomiting, mental status change, stiff neck, proximal muscle weakness or flaccid paralysis, and cerebrospinal fluid (CSF) revealing lymphocytes with elevated protein and negative bacterial pathogens. Empiric treatment for bacterial meningitis and/or herpes simplex virus encephalitis is appropriate until results of testing for WNV-IgM in serum and CSF are clarified. Ventilatory support may be required, especially for those older than age 65, in whom respiratory failure and death from WNME are at least six-fold higher than in younger patients.
To further unsettle our troubled nation, 2002 marked a number of firsts for WNV infection. The first cases of transfusion-related WNV infection were reported and confirmed in six instances; 27 other cases are under investigation by the CDC. The first cases of organ-donor transmission were reported among four recipients of separate organs from a 20-year-old woman who had received numerous blood products prior to her death (heart, liver, and both kidneys were donated). Three of these recipients developed WNME, two were intubated, and one died. The first case of maternal transmission to a breast-fed infant occurred in a mother who developed WNME after transfusion for postpartum hemorrhage; WNV IgM was detected in maternal serum and CSF, breast milk, and infant serum. The first report of in utero
WNV infection occurred in a 20-year-old woman with fever, leg weakness, hyporeflexia, lymphocytosis in CSF, and WNV-IgM in serum and CSF at 27 weeks gestation. Upon delivery at 38 weeks, her infant had chorioretinitis, severe white matter and cortical destruction on magnetic resonance imaging, and WNV-IgM in cord blood and CSF. Placenta was positive for WNV by PCR.
And finally, two microbiologists were documented in 2002 with the first incidence of laboratory-acquired WNV infection. Each had a finger puncture wound while dissecting brain tissue from WNV-infected wildlife. Seroconversion to positive WNV-IgM occurred in each researcher.
So what is the ED physician to do? Be vigilant for encephalitis and aseptic meningitis patients, or apparent Guillain-Barré patients with atypical features such as fever and CSF pleocytosis. Each could represent a case of WNME, especially in areas recently discovered to have dead crows, jays, hawks, and eagles, and sick horses. Advise 20-30% DEET repellant and long sleeves to reduce mosquito exposure. Hope that health departments and the CDC develop improved mosquito control measures or an effective vaccine. Be ready for an epidemic of WNV of ominous proportions among humans, birds, and horses, from coast to coast, this summer. It may not be a pleasant picnic any more, any place.
Dr. Felz, Associate Professor, Department of Family Medicine, Medical College of Georgia, Augusta, GA, is on the Editorial Board of Emergency Medicine Alert.
In conjunction with the Centers for Disease Control and Prevention, the ArboNet surveillance network of state and local public health departments was established to monitor West Nile virus activity reported in humans, animals, and mosquitoes for three years.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
