Better Targeting of Antibiotic Therapy Against the GramPositive Coccal Infections of Neutropenic Patients
Better Targeting of Antibiotic Therapy Against the GramPositive Coccal Infections of Neutropenic Patients
Abstract & Commentary
Synopsis: Indices have been developed to help assess the risk of neutropenic patients developing Gram-positive infections when they become febrile that might allow strategies to be developed for managing these infections.
Source: Cordonnier C, et al. Epidemiology and risk factors for Gram-positive coccal infections in neutropenia: Toward a more targeted antibiotic strategy. Clin Infect Dis. 2003; 36: 149-158.
Gram-positive cocci continue to harass neutropenic patients and perplex physicians because detection of these bacteria need not necessarily represent true infection. It is, however, often a direct consequence of the treatment or supportive care given to the patient as a result of mucositis and the widespread use of central venous catheters. These bacteria also account for more infections than do the Gram-negative bacilli. Moreover, we are seldom dealing with professional pathogens such as Staphylococcus aureus or Streptococci pyogenes in this patient population but rather their less pathogenic relatives, namely the viridans streptococci (mainly Streptococcus mitis and Streptococcus oralis) and the coagulase-negative staphylococci (mainly Staphylococcus epidermidis) that form a conspicuous part of the normal commensal flora of the oral cavity and skin, respectively. Infections due to Gram-positive cocci are usually indolent, but some viridans streptococci, particularly S mitis, are associated with sepsis and adult respiratory distress syndrome, which can prove fatal. The objective of this particular study was to determine the prevalence of Gram-positive coccal infections among febrile neutropenic patients and to develop a risk index to allow physicians to identify patients at risk for Gram-positive coccal infections and choose the most appropriate therapy. This last aspect is important given the predominance of the Gram-positive cocci and the fact that most empirical regimens are not optimal in this regard, being primarily intended to treat infections caused by Gram-negative bacilli, such as Escherichia coli, Pseudomonas aeruginosa, and the like.
The study was conducted over a 2-month period in 36 French hospitals. The first episode of fever during neutropenia was registered for 513 patients. The presence of microbiologically defined infections were established in 168 (33%) and clinically defined infections in 40 (8%) episodes. No infection was identified in the remaining 305 (59%) episodes. Gram-positive cocci were involved in 108 (21%) episodes altogether and Gram-negative bacilli accounted for 55 (11%) of all episodes of fever. Twenty-eight patients died within a month of becoming febrile, and the primary infection contributed to 9 of these deaths. A wide range of factors that might influence infection were recorded, including age, hematology (diagnosis and status), the cause of neutropenia (conditioning regimen for transplantation when applicable, chemotherapy received during the month before enrollment), location during the week before the onset of fever (laminar air-flow room, single room, 2-bed room, or outpatient), any drugs used (growth factors and any anti-infective drugs including antifungal agents and drugs used for selective decontamination of the gut, anti-ulcer drugs, and antacids), and the site of the intravenous catheter (central or peripheral). The signs and symptoms likely to be associated with infection were recorded on the day of fever, and at least 2 samples of blood were obtained for aerobic and anaerobic culture before antibiotic therapy was started. The regimen for empirical therapy consisted of a ß-lactam antibiotic in 466 (91%) cases in combination with an aminoglycoside in 338 (66%) cases and/or a glycopeptide in 159 (31%) cases.
After conducting a multivariate analysis, the occurrence of Gram-positive coccal infections was found to be significantly associated with 4 factors: high-dose cytarabine therapy; treatment with proton pump inhibitors; oral treatment with colimycin (colistin, polymyxin E) without a glycopeptide for gut decontamination; and the presence of chills.
Each episode was scored for each of these factors (0 = absent, 1 = present) to assign a Gram-positive infection risk index (GPRI), which was the sum of all the factors ranging from 0 to 4. The risk for Gram-positive infection increased 3, 3.9, 7, and 17.5 times when the GPRI was 1, 2, 3, and 4, respectively. A score of 3 or 4 effectively excluded a Gram-negative infection (see Figure). Further analysis showed that streptococcal infections were significantly associated with high-dose cytarabine therapy; oral treatment with nonabsorbable antifungal agents (nystatin, amphotericin B); oral treatment with colimycin; and diarrhea.
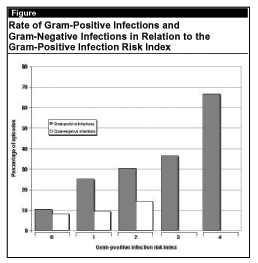
The only identified association with staphylococcal infections was the use of the polymyxin.
Each episode was subjected to a streptococcal infection risk index constructed in a similar way to the GPRI from these 4 factors. While the odds ratio increased from 3 to almost 20 with an increasing index, so, too, did the odds ratio for staphylococcal infection. Cordonnier and associates are now conducting a prospective study of neutropenic patients to evaluate these indices with a view toward addressing the question of which is the best strategy for managing Gram-positive infections in this vulnerable patient population.
Comment by J. Peter Donnelly, PhD
This study represents a novel approach to solving a perennial problem, namely how to recognize Gram-positive infections in neutropenic patients ahead of time. A risk index such as described heightens the awareness of the specific risk factors involved and might even help determine which antibiotic regimen is best suited to dealing with the problem. As Cordonnier et al realize, it is not just important to recognize the patient at risk for Gram-positive infections but more specifically to distinguish those likely to have streptococcal infection from those who have staphylococcal infections, as the treatment options differ. Managing a staphylococcal infection may require treatment with a glycopeptide, removal of the central venous catheter, or the application of an antibiotic block to tide the patient over until the device can be removed. By contrast, early recognition of an incipient streptococcal infection would allow treatment with penicillin or even therapy with corticosteroids to prevent ARDS.1 The indices presented seem unlikely to be able to achieve latter objective on the basis of the evidence presented so far, although it is clearly worthy of further investigation. Some other aspects of this report have to be set in context. First, it remains standard practice to assume that every episode of fever that occurs is due to a Gram-negative bacillus and to start treatment promptly with a regimen consisting of a broad-spectrum ß-lactam such as ceftazidime or meropenem. Even if the fever remains unexplained or another etiology has been established, it is still common practice to continue the initial core regimen and to complement it with other antimicrobial agents as circumstances dictate. Second, many physicians feel compelled to complement the core regimen with one of the glycopeptides, vancomycin or teicoplanin, regardless, as occurred in almost a third of patients in this study. Given the risks attached, it is clearly desirable to establish objective criteria by which patients who need these drugs get them while others are spared. Third, and importantly, 3 of the 4 factors identified will vary from center to center since oral treatment with nonabsorbable antifungal agents like nystatin or amphotericin B has largely been supplanted by other drugs such as fluconazole for prophylaxis against fungal infections. Similarly, oral treatment with colimycin has been all but abandoned in many countries and was never used in other regions such as the United States. It is biologically plausible that each of the factors incorporated into the risk indices actually does increase the risk of infection in some way; however, the use of the indices will very much depend upon the practices of one’s own hospital.
Dr. Donnelly is Clinical Microbiologist University Hospital Nijmegen, The Netherlands Section Editor, Microbiology.
References
1. Dompeling EC, et al. Pre-emptive administration of corticosteroids prevents the development of ARDS associated with Streptococcus mitis bacteremia following chemotherapy with high-dose cytarabine. Ann Hematol. 1994;69:69-71.
Indices have been developed to help assess the risk of neutropenic patients developing Gram-positive infections when they become febrile that might allow strategies to be developed for managing these infections.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
