Surgery centers, hospitals could lose millions under OIG recommendations
Surgery centers, hospitals could lose millions under OIG recommendations
Report suggests uniform payment rates, deletions from ASC list
If implemented, recent recommendations from the Department of Health and Human Services’ Office of Inspector General (OIG) would result in millions of dollars in payment reductions for hospital outpatient departments (HOPDs) and ambulatory surgical centers (ASCs). OIG’s report recommends that the Centers for Medicare & Medicaid Services (CMS) set uniform rates for outpatient services provided in ASCs and HOPDs.
The OIG report claims that reimbursement disparities between hospitals and surgery centers has resulted in $1.1 billion in additional hospital payments. The failure of CMS to remove procedures from the ASC list of covered procedures, when the procedures didn’t meet the agency’s criteria, has resulted in overpayments of $8 million to $14 million, the report says. (For information on accessing the report, see "Resources" at the end of this article.)
Some sources express concern that these changes could cause procedures to shift settings.
"Payment amounts definitely influence the willingness of any provider — hospital, ASC, or physician — to provide services, and thus any changes to lower current amounts would certainly influence their decision," says Craig Jeffries, executive director of the American Association of Ambulatory Surgery Centers in Johnson City, TN.
Safety is an issue being raised by some surgery providers, Jeffries says. The recommendations, if implemented, could push surgeries into physician offices in states that don’t require such settings to meet ASC or hospital standards, he says.
Here are OIG’s recommendations for CMS:
- CMS should seek authority to set rates that are consistent across sites and reflect only the costs necessary for the efficient delivery of health services.
- CMS should conduct and use timely ASC survey data to re-evaluate ASC payment rates.
- CMS should remove the procedure codes that meet its criteria for removal from the ASC list of covered procedures.
CMS has failed to remove 72 procedure codes from the list that don’t meet the agency’s established criteria, the OIG says. Cutting these codes would have reduced ASC payments by $8 million to $14 million, the report says. At press time, the draft final regulation for adding and removing procedures from the ASC list was being circulated among agencies.
According to the OIG, only six of the 72 procedure codes are scheduled for deletion. However, there may be hundreds of procedures proposed for addition. Sources estimate that final rule will be published and implemented before summer.
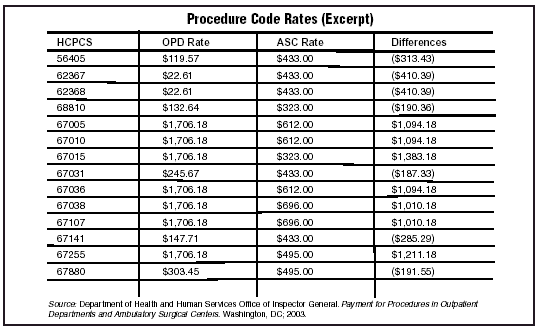
If the recommendation for uniform payments were implemented, it would lower HOPD payments rates for 66% of the 453 procedure codes examined by OIG. The median reduction would be $282.33. Four codes are paid 200% or greater more than ASCs, 69 codes are paid 100% to 199% more than ASCs, 88 are paid 50% to 99% more than ASCs, and 118 are paid 1% to 49% more than ASCs.
If these hospital payments were lowered to the surgery center amount, and hospitals decided to quit performing certain procedures because the payment was too low, then ASCs might benefit from increased business, acknowledges Kathy Bryant, JD, executive director of the Federated Ambulatory Surgery Association in Alexandria, VA. "However, this is too speculative to estimate at this time," she adds. "Reducing the payment for procedures in hospitals would have no immediate effect on ASCs."
In 145 procedure codes examined by the OIG, Medicare reimbursed ASCs more. For those procedures, 12 codes are paid 200% or up more than the hospital rate, 41 codes are paid 100% to 199% more than the HOPD rate, 26 codes are paid 50% to 99% more than the HOPD rate, and 66 are paid 1% to 49% more than the HOPD rate. However, sources point out that CMS has no current data on the cost of these procedures because the ASC cost survey hasn’t been conducted for several years.
If the HOPD and ASC rates were equalized, some procedures, such as cataract removal, might have mixed results, says Eric Zimmerman, JD, partner with McDermott, Will, and Emery in Washington, DC. The payment rate for cataracts is higher in hospitals, but when it’s performed with a YAG laser, the payment in higher in the ASC, Zimmerman says. If the OIG’s recommendation was implemented, more cataract procedures might move to ASCs, but more YAG procedures might move to hospitals, he speculates.
The bottom line would be whether providers could continue to provide the service at the new reimbursement rate, Zimmerman says. "If not, they may stop," he says. "More realistically, a lot of settings will stop providing services to Medicare beneficiaries."
One example is gastrointestinal (GI) procedures, Zimmerman says. The OIG says that there are 13 endoscopy/upper GI that are paid higher in ASCs, and 13 that are paid higher in hospitals. If the recommendation for equal payments is implemented, the OIG estimates the potential savings at $28,370,205. "If reimbursement for GI ASCs comes down as much as OIG says, it will not be cost-effective for ASCs to furnish," he says.
What’s wrong with the recommendations?
It is a logical question to ask why a different rate should be paid to ASCs and HOPDs, Bryant acknowledges. "Right now, the answer is that different statutes provide different ways of calculating rates and are going to result in different payments," she says.
However, sources express these specific concerns about the recommendations:
• Hospitals have different requirements.
Leveling the playing field to some extent makes sense, acknowledges Ashley Thompson, senior associate director of policy development at the American Hospital Association in Washington, DC. "But the problem is that hospital care is much more expensive in the outpatient setting, due to different requirements that hospitals must meet, such as EMTALA [Emergency Medical Treatment and Labor Act] provisions, life safety code, being open 24 hours a day/seven days a week, and having to treat everyone who walks in the door," Thompson says. "These create a different set of requirements for hospitals."
• Hospitals already are losing money on Medicare outpatients.
Already, 57% of hospitals lose money overall caring for Medicare patients, says Thompson, citing the AHA annual survey. "We think that further reducing payments would have tremendous impact on patients and facilities," she says. "It’s not the right move to make."
• The analysis is flawed, sources say.
The OIG used a simplistic approach, explains Zimmerman. "For example, they didn’t recognize fully that the payment systems are developed in different ways and intended to reimburse for different bundles of costs, and also, in fact, there may be cost differences between the settings that may result in different payment levels," he says. It’s as if the OIG was exaggerating to make a point, he says. "I think it’s almost absurd that they were saying that the payment rate should be paid at the lowest level," he says.
Their report presumes that payment rates for ASC and HOPD services are accurate at the lower of two levels. "Actually, ASC rates aren’t actual reflections of anything because the data are so old," he says. Also, the ASC reimbursement mechanism of nine payment groups is crude, he says.
The HOPD payment data are more current, but the payment rates don’t reflect the cost of providing a service, Zimmerman says.
Also, the OIG report used 1999 volume and 2001 rates, Bryant says. Using 2001 volume and 2003 rates indicates that cutting all ASC payments rates that currently exceed HOPD rates would result in $115 million in payment reductions, she says.
Also, some HOPD rates have changed significantly from the data used to compile the report, Bryant says, For example, HCPCS 52000, which had a significant payment difference in ASCs and HOPDs, is now less than $4 different, she says. FASA offers software that allows individual ASCs to assess the proposed reduction of payment to the HOPE level. (See ordering information in "Resources" section at the end of this article.)
Also, FASA recalculated the overpayments f or the 72 procedures that the OIG recommends deleting from the ASC list of approved procedures. FASA’s recalculations used 2003 data and 2001 volume. "In fact, Medicare would save only $80,000 if the procedures that the OIG recommended were deleted from the ASC list and moved to HOPD," Bryant says. " Of course how much more it might cost beneficiaries is not calculated."
Also, the OIG makes clear in the report that its analysis is simply a financial one, Bryant says. "They note that they did not consider access or quality, but only considered cost," she says.
A better analysis could results in fairer payments and benefit to Medicare patients, says Jeffries.
"CMS certainly can provide a more methodical analysis of the current site of service differential to help achieve a more reasonable payment rate for ASC procedures that are currently underpaid, compared to the HOPD payment, and thus expand beneficiary choice," he says.
FASA has reminded its members through the web site that the OIG report includes recommendations only, and CMS has no immediate plans to implement the recommendations. CMS’s official response to the report says that further compatibility is desirable between ASC and HOPD payments; however, the solution is not obvious.
"One approach would be to use the lower payment rate in all settings," according to the response. "A second approach would be to attempt to pay an amount in each setting that would reflect in a comparable way the relative costs of using each site."
For the recommendations to take effect, CMS or Congress would have to act, Zimmerman points out. While those groups will be looking at payment disparity, they are unlikely to implement the OIG recommendations, he contends. Instead, he expects the groups to give more weight to recommendations that were expected from the Medicare Payment Advisory Commission (MedPAC) at press time. MedPAC will recommend that no surgical procedures be paid more in an ASC than a hospital outpatient department. (See correction below.)

Correction
In the March 2003 issue of Same-Day Surgery, an executive summary of the story on recommendations from the Medicare Payment Advisory Commission (MedPAC) misrepresented the recommendation for hospital and surgery center payments. The recommendation is that surgery centers would not be paid more than hospitals for the same procedures.
Resources
For more information on the payment rate proposals, contact:
• Kathy Bryant, JD, Executive Director, Federated Ambulatory Surgery Association, Alexandria, VA. Telephone: (703) 836-8808. Fax: (703) 549-0976. E-mail: [email protected].
• Craig Jeffries, Executive Director, American Association of Ambulatory Surgery Centers, P.O. Box 5271, Johnson City, TN 37602-5271. Telephone: (423) 915-1001. Fax: (423) 282-9712. E-mail: [email protected]. Web: www.AAASC.org.
• A copy of the new Office of Inspector General report, Payment for Procedures in Outpatient Departments and Ambulatory Surgical Centers, is available on the Internet at oig.hhs.gov/oei/reports/oei-05-00-00340.pdf.
• The Federated Ambulatory Surgery Association (FASA) is offering a computer disc with an Excel program to assess the proposed reduction of surgery center payments to the hospital payment level. To use, you simply insert your center’s volume for each procedure, and the total reduction is provided. The cost is $15 for FASA members and $30 for nonmembers. To order, contact FASA. Telephone: (703) 836-8808.
If implemented, recent recommendations from the Department of Health and Human Services Office of Inspector General (OIG) would result in millions of dollars in payment reductions for hospital outpatient departments (HOPDs) and ambulatory surgical centers (ASCs). OIGs report recommends that the Centers for Medicare & Medicaid Services (CMS) set uniform rates for outpatient services provided in ASCs and HOPDs.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
