‘Making it personal’ improves patient care
Making it personal’ improves patient care
Personal histories increase patient satisfaction
Sheila Brune, RN, BS, CPHQ, CPUR, says the quality of direct patient care is the most important predictor of patient satisfaction. In the past few years, Brune, CMC director of Utilization Management/Living History Program at Great River Medical Center in West Burlington, IA, has proved her point emphatically with an innovative program inspired by her desire to create closer connections with patients.
The Living History program involves the creation of "a living, breathing chronicle of the patient’s nonmedical history." The intent of the history is to empower caregivers to deliver care to the heart and soul of the patient, Brune says.
Brune first began thinking about the program about two years ago, when her CEO returned from a training session led by Quint Studer of The Studer Group. "What impacted me were two issues," she recalls. "The first was a question: Are you part of the problem or part of the solution? The second was the assertion that you’ll be judged by the people you touch."
The task she decided to undertake didn’t even fit her job description. "I was director of utilization management; people always said I was the dollars-and-days dame,’" she notes. "But at my heart, I am a nurse."
Brune was aware that often patients would be with the hospital for a long time, and then one day she would by chance read their obituaries. "I realized that there was a lot more to those people than we had thought," she explains. "I wanted to explore how we could get that information before they died. I like telling patients that I want to know what they do when they’re not here."
Why do it?
It’s all well and good to be curious about a patient’s personal history, by why is it important from a quality standpoint? Why is it important to "deliver care to the heart and soul of the patient?"
"There are lots of reasons," Brune says. "It makes the patient feel more valued — that you are thinking about them not as a number, but as a person. What people want most is to feel valued and to be listened to. Also, I believe if you improve the patient/caregiver relationship, not only does the patient feel better, but the caregiver does, too. It increases their satisfaction with their job."
She recalls comments from nurses like: "I can’t believe what you did for me with this story. We found connections that went way back."
Brune cites a number of occasions where patients had actually worked with relatives of caregivers, and, in at least one case, a nurse found out much more about a relative who had passed away than she ever would have known had she not connected with the patient.
This is one of the three different ways in which caregivers are encouraged to build bridges with patients. They are:
- Real Connections: "I know your daughter."
- Compassionate Connections: "You have been through a lot in your life."
- Scripted Connections: "I see you like to do woodworking. What do you like to make?"
Getting started
Brune decided to build the program through story writers — special employees selected to get the patients’ stories. She also determined that, initially, stories would focus on chronically ill patients with diagnoses that caused multiple admissions — i.e., seriously ill, terminally ill, or very elderly patients, and/or patients on dialysis or in hospice care.
"We went through the DRGs and picked longer-stay, high-volume, high-risk patients, but now we go more on our gut," Brune says. "Age is first, because the extreme elderly have fascinating stories. We also look at diagnoses — cancer, stroke/CVA, COPD, and CHF, as well as surgicals who will be here longer, like hips, knees, and colonoscopies. Now, we will also take referrals," she adds.
In the beginning, however, she had to spread the word. "I just went out and talked to everyone, in every department," she recalls. She started with the CEO, who said yes; then, the senior management team, who said, Make it happen,’ then to the middle managers, and then to staff meetings.
"We also went out into the community, through TV and radio," Brune says. "And we elicited people from each department to be story writers; almost every department was represented." This also helped involve employees who would not normally come in contact with patients. "Clinical information is not often shared with librarians," Brune notes.
In the beginning, Brune picked the story writers. "Now, I let them pick me," she says. If they show interest, their manager must sign off, because they spend an average of two hours on each assignment (the story writer’s commitment is for one story a week.)
Once the selection has been approved, there is a one-day training session, facilitated by an educator, a social worker, a recreation therapist, a journalist/editorial review writer, and Brune. Following that, the assignments are made, and the story writers visit the patients, who tell their personal stories.
Interestingly, the profile of story writers has changed over the years. "We only have two of the original story writers left," Brune says. "The people I first picked were outwardly, openly enthusiastic, and those criteria may not have worked; maybe they were just big talkers, but short on action. My best story writers have been the sleepers’ — those people who quietly work every day," she explains.
The Living Histories are used and shared in a number of ways. They are presented as a visual depiction, known as a bridge poster (Milestone events and family facts are depicted, centered around a logo of a bridge), for the patient’s room; the Living History itself is placed as the first item on the patient’s chart. (Click here for an example of a Living History, and see an example of a bridge poster below.)
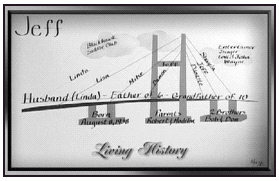
There is an absolute expectation that all of the patient’s caregivers will read the history. "One of our deals with our CEO is non-negotiables,’" Brune explains. "We say things like, always wear your name tag, always lead people who are lost to the department they need, and always read the Living History."
The copy that is placed in the chart is put in a plastic sleeve protector. One copy is given to the patient — laminated if they request it. They then receive as many additional copies as they want. They also receive one Bridge Poster — laminated, again, upon request.
The stories also live on through Meditech, the facility’s computerized record medical system. "I save the stories to a Word file and then enter them into the Meditech screen, so you have a record of the patient’s story and who wrote it," Brune says.
To date, 1,700 stories have been written. "We need more story writers," she says, noting that care is changing and patient satisfaction is growing. The current Press, Ganey Associates satisfaction rate is over 90%, up considerably from two years ago.
"We have no reason to believe it will not continue to climb," she says.
Brune is eager to share her success story with other institutions.
"We have two hospitals starting their own programs [soon], and we probably have 20 out there who have placed phone calls, have come here or are planning to come to visit," she says, noting that the best way to contact her is via e-mail ([email protected]).
For more information, contact:
• Sheila Brune, RN, BS, CPHQ, CPUR, CMC, Director, Utilization Management/Living History Program, Great River Medical Center, 1121 S. Gear Ave., West Burlington, IA 52655. Telephone: (319) 768-4951.
The Living History program involves the creation of a living, breathing chronicle of the patients nonmedical history. The intent of the history is to empower caregivers to deliver care to the heart and soul of the patient.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
