Benchmark program sees improved infection rates
Benchmark program sees improved infection rates
Data encourage information exchange
Preventing, diagnosing, and treating infections in home care patients require careful surveillance and a high level of awareness of infection control on the part of a home health nurse. You may think your agency is doing a good job of preventing infections, but how can you tell?
"It’s hard to find infection rate data that are specific to home health," says Mary Schantz, executive director of the Missouri Alliance for Home Care in Jefferson City.
In fact, she says, it was this difficulty that prompted a home health nurse who was given the responsibility of infection control and quality improvement in her agency to call the home care association and ask for help in developing a benchmarking program for home health agencies.
"When we contacted our membership in 1993 to see who might participate in an infection control monitoring program, I was overwhelmed by the level of interest. We started with a detailed literature search, developed a tool to gather data, modified definitions of infection control for home care settings, and field tested the tool between 1993 and 1995," she says.
The program officially began collecting data in 1995 and now has more than 105 agencies in 26 states reporting infection control rates, Schantz says. Agencies collect and report on infections related to indwelling bladder catheters and central venous catheters. Results for the third quarter of 2002 show a total average infection rate of 3.1 infections per 1,000 days for bladder catheters and 0.6 infections per 1,000 days for central venous catheters. (See graphs, below.)
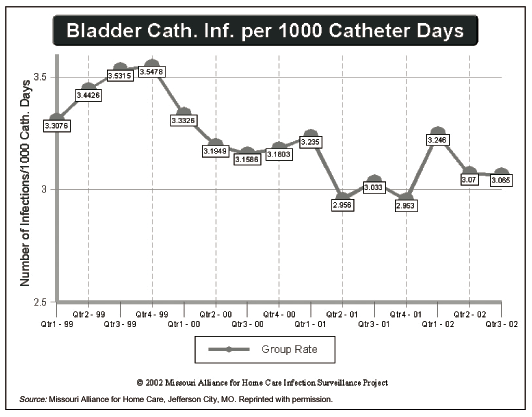
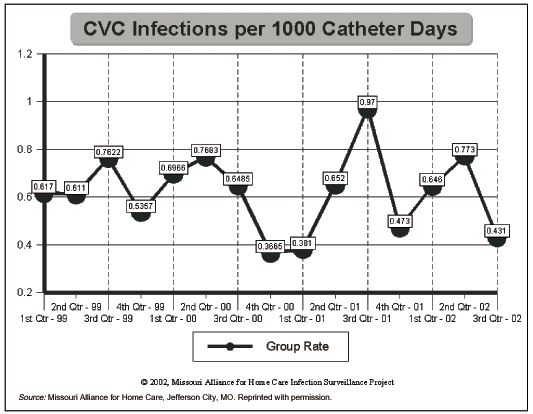
"The data collected represent active surveillance rather than passive surveillance so we know we are receiving the most accurate, up-to-date information possible," says Carolyn Crumley, RN, MSN, CS, SWPOCJ, wound, ostomy, and continence clinical nurse specialist and president of WOC Care in Lee’s Summit, MO. Active surveillance relies upon the chart review of current patients by a nurse who is reviewing nurse’s notes, lab results, and changes in orders, such as the addition of an antibiotic. "This differs from passive surveillance that relies upon a nurse notifying someone in infection control or quality improvement when a patient develops an infection," she explains.
Basing your infection rates only upon cases reported by staff members may not be accurate for several reasons, Crumley says. "When I began reviewing charts, I continued having nurses report infections to me so I could see how accurate their reports were," she says.
"I found that only 25% of all infections were reported," she adds. The low rate of reports may be due to busy schedules, a lack of awareness of the need to report infections, or a fear that the infection may reflect negatively on the nurse’s performance evaluation, she adds.
Actively reviewing patient charts takes Crumley about eight hours each month to review charts from three different offices. "It gets easier as you do it more often, and the amount of time depends on the size of the agency," she says. One tip she offers is to identify one spot within the record to indicate infections. "I worked with the nurses to designate one spot on our flowsheet for them to note infections," she says.
A benchmarking program for infection control can help a home health agency in many ways, Crumley points out. "Obviously, when someone starts with this study, the goal is to reduce infection rates to reflect the national average. It is just as important to continue looking at your infection rates over a period of time, even when you’ve reduced them dramatically," she says.
One way the Missouri Home Care project helps participants continue reducing infection rates is a bimonthly conference call for all participants to exchange information, ask questions, and share suggestions with each other, Schantz says.
A key to controlling infections that has been discovered by project participants is adequate teaching of family caregivers, Schantz says. "By making sure that caregivers understand proper cleaning and care of catheters, our participants have decreased their rates over time," she adds.
To participate in the infection control project,
a home health agency has to agree to use active surveillance and to develop internal policies, procedures, and tracking documents that will result in data that meet the same definitions and goals as all other participants, Schantz says.
"At first, only Missouri home care agencies could participate because we required face-to-face meetings at which nurses visited the agencies to train them in surveillance methods and data collection," she says.
"Now, we’ve developed a quality training program that can be conducted over the telephone with fax and e-mail support." There is no cost to Missouri agencies, but others pay $400 for the first year of participation and $300 for subsequent years, Schantz adds. The additional cost for the first year is to cover the extra training costs, she explains.
Even if your agency chooses not to participate, the Missouri Alliance for Home Care will share policies, definitions, and forms with home health agencies that are interested in tracking infections internally, Schantz says.
"Even though each agency participating in the project receives reports on how it’s data compared to other agencies, the most important thing is to evaluate individual patients as you gather your data," Crumley suggests. "A small agency might see a significant increase in the infection rate as a result of one patient," she points out.
As you review your monthly data, be sure to see if proper protocols are also followed, Crumley says. "It’s very important to make sure that antibiotics are not being ordered before lab results are returned because it might be the wrong antibiotic," she says.
"Many of our bladder and central venous catheters [patients] are susceptible to infections, and we want to make sure we don’t put them at risk for developing a resistance to certain antibiotics. The best way to minimize the risk is to make sure the antibiotic ordered is appropriate for the bacteria causing the infection, she adds.
Another step in the infection control project is the development of a best practices report, says Schantz.
"We’re trying to develop this report by asking participants to let us know what they have learned," she says. "Knowing that increasing the size of the catheter increases risk of infection and learning other tips from our group will help all home care agencies provide better care for patients."
[For more information about the Missouri Alliance for Home Care infection control project, go to: www.infectioncontrolathome.org or contact:
- Mary Schantz, Missouri Alliance for Home Care, 2420 Hyde Park, Suite A, Jefferson City, MO 65109-4731. Telephone: (573) 634-7772. Fax: (573) 634-4374. E-mail: [email protected].
- Carolyn Crumley, RN, MSN, CS, SWOCN, Wound, Ostomy, and Continence Clinical Nurse Specialist and President of WOC Care, 3712 N.E. Beechwood Drive, Lee’s Summit, MO 64064. Telephone and fax: (816) 478-6019. E-mail: [email protected].]
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
