The Documentation-Coding Connection: Benchmarking ED physician billing
Benchmarking ED physician billing
By Myra Wiles, CPC
Physician Reimbursement Specialist
Administrative Consultant Service Inc.
Shawnee, OK
It’s a common practice to benchmark physician-billing patterns against those of peer groups. Most practices benchmark against data furnished by the Medical Group Management Association (MGMA) or against Medicare data available through the Centers for Medicare & Medicaid Services (CMS).
Benchmarking data skewed
Unfortunately, benchmarking against such data is misleading, since it is based upon three incorrect assumptions.
When benchmarking ED physician billing, the first incorrect assumption is that all emergency departments (EDs) are alike. CMS and most other insurance carriers do not differentiate between EDs in urban and rural communities. Nor do they classify Level I trauma centers differently from other EDs. Thus, within a particular state you have only one designation (one classification) for emergency departments and all EDs within the state are lumped into that same category without regard to size or resources.
The second incorrect assumption is that all services were billed at appropriate levels. Insurance carriers pay claims based upon the assumption that the service is billed at a level appropriate for the problem(s) addressed and that documentation supports the code billed. However, as one who has audited various types of practices (including EDs) for more than 10 years, I can assure you that this is simply not true. While most physicians and practices are making a concerted effort to properly bill and document their services, most practices are still far from meeting the criteria set by the American Medical Association and CMS. Many services are billed too aggressively; others, too conservatively.
The third bad assumption is that every provider working in the ED is credentialed with the insurance company in the specialty of "Emergency Medicine." Yet, a large number of hospitals contract with family practice, general practice, internal medicine and various extenders (PAs, NPs, etc.) to staff their EDs. Thus, any emergency department billing by individuals in those practices are excluded from the benchmarking numbers for emergency medicine. This greatly skews any comparisons.
Why benchmark?
Insurance carriers realize that the data against which you are compared are inaccurate. But it is the only means by which they can focus their auditing efforts toward those practices with billing patterns most likely to be a) in need of additional education and training; or b) defrauding the program. Similarly, it is the most obvious tool available to assess your own billing practice and detect unique billing patterns that increase your risk of carrier audit.
That does not mean that you should try to mirror the pattern set by your peer group. Benchmarking is a risk measurement tool and nothing else. I have seen practices with billing patterns that mirror the national averages but have still billed inappropriately for the services provided.
Instead, your goal should be to bill and document at levels appropriate for the patients and problems treated — regardless of the benchmarking data. By doing so, you can be assured that, should an audit occur, your organization can defend the services billed.
Benchmark properly
As much as possible, compare apples to apples and oranges to oranges. Don’t try to benchmark all of your ED personnel against the data for Emergency Medicine. Instead, benchmark the ED codes billed by your PA against national data for PAs billing the same codes. Do the same thing for the family practitioner with whom you contract. Benchmark against the data for Emergency Medicine only if you know that your contracted physician has been credentialed in that field.
2001 Billing Pattern for Medicaid
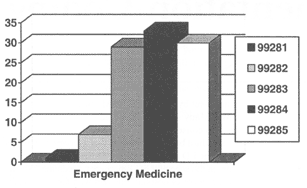
The above chart reflects the 2001 Medicare billing pattern for emergency medicine. It is expressed in percentages and does not reflect ED billing by physicians (or nonphysicians) in other specialties.
What level is appropriate?
The formula for determining the appropriate code for a service is complex and depends upon the amount of history taken, exam performed, condition(s) treated and recommendations for care. But we suggest the following common sense guide toward quick selection of the appropriate code. Keep in mind that these suggestions have nothing to do with selecting the correct facility code.
• Level I (99281) — Appropriate for patients with simple problems that require little or no treatment. This may include patients coming in for scheduled injections or testing, for dressing changes or removal of sutures. Treatment usually is limited to ice packs, bandages, or simple over-the-counter (OTC) meds. The history can be extremely brief, and you need examine no more than one system (using 1994 documentation guidelines).
• Level II (99282) — This level describes many of your patients that use the ED as an urgent care clinic and is comparable to the level III office visit for established patients. Patients at this level usually have a simple acute infection (UTI, URI, BOM, etc.), a sprain or strain. Treatment at this level usually is limited to simple blood work, X-rays without contrast or recommendations for meds (OTC or prescription) or physical therapy. When billing this level, your history must include a little more detail (including a review of systems) and the exam should cover at least two systems.
• Level III (99283) — The patient at this level is a little more complicated than at Level II but not so bad as to require a more detailed work-up. Typically, these are patients with mild exacerbations, simple injuries, or new problems that don’t require a detailed workup. The history and exam doesn’t require any more detail than at Level II.
• Level IV (99284) — Now we’re talking true emergency. This level is appropriate for a patient with an acute exacerbation or severe trauma that requires a detailed work-up. Treatment usually includes extensive testing, use of prescription meds, scopes, arteriograms, fracture care, or recommendations for major surgery.
• Level V (99285) — This code represents the high-risk patient with a high-risk treatment plan. These patients frequently qualify for critical care codes when properly documented. These are patients with multiple trauma, acute MIs, suicidal patients, strokes, system failure, and similar scenarios. The treatment plan should be complex and require extensive testing and/or treatment with high-risk meds or surgery. Take no shortcuts on documentation of these cases. Get a comprehensive history (including four facts about the present illness, a review of 10 systems, a past, family, and social history) and a comprehensive exam of eight systems (using 1994 documentation guidelines).
Benchmark at least quarterly to detect potential problems and analyze risk. Work with your ED staff on a regular basis to provide ongoing education on billing and documentation issues. At least annually, have an outside firm perform a review of a random sample of ED physician charts to detect any problems that may have gone unnoticed and to correct any internal spread of inaccurate information.
Its a common practice to benchmark physician-billing patterns against those of peer groups. Unfortunately, benchmarking against such data is misleading, since it is based upon three incorrect assumptions.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
