ED Nursing Reports: Update on Wound Closure - Evidence-Based Strategies for Optimizing Outcomes
Nurse Editor: Reneé Semonin Holleran, RN, PhD, Chief Flight Nurse, Clinical Nurse Specialist, University Hospital, Cincinnati.
Peer Reviewer: Darlene Bradley, RN, MSN, MAOM, CNS, CCRN, CEN, University of California Irvine Medical Center, Orange, CA.
Introduction
Collectively, wounds are the third most common problem seen in the emergency department (ED).1 In 2000, more than 7 million wounds were treated in EDs in the United States.2 Although the ultimate aims in wound treatment are to prevent infection and to obtain a functional and attractive scar, patient priorities also include, in descending order of importance, normal function, the least visible scar possible, and the least painful repair possible.3,4 These goals may be achieved by decreasing tissue contamination, properly debriding devitalized tissue, and performing a well-approximated skin closure.5 (See Rapid Access Management Guidelines.)
Epidemiology
Almost one-third of wounds occur in adult males between ages 19 and 35 years. Most of these wounds are located on the head or neck (50%) or on an upper extremity (35%), and the fingers or hands usually are involved.5 The most common method of injury is blunt trauma, such as bumping the head against a hard surface. Other common sources of injury include sharp instruments, glass, and wooden objects.6 Mammalian bites are a relatively uncommon cause of significant lacerations.
The magnitude and direction of the injuring force and the volume of tissue on which the force is dissipated determine the type of wound sustained. The resulting disruption or loss of tissue determines the configuration of the wound. Based on these mechanisms, wounds have been classified into six types: abrasions, lacerations, crush wounds, puncture wounds, avulsions, and combined wounds.7
Methods of Wound Closure
Tissue Adhesives. Tissue adhesives are being used with increasing frequency in the United States since the introduction of octylcyanoacrylate (Dermabond, Ethicon) after Food and Drug Administration (FDA) approval in 1998. A tissue adhesive offers many potential advantages over standard wound closure, including ease of use, decrease in pain and time to apply, as well as not requiring a follow-up visit for suture removal.8
When applied to tissues, cyanoacrylate adhesives polymerize rapidly through an exothermic reaction catalyzed by a small amount of moisture. This produces heat, which is more pronounced the more heavily the adhesive is applied. Adhesives can cause an intense inflammatory reaction in the subcutaneous tissues and never should be applied within wounds.9
A study in 1998 compared the one-year cosmetic outcome of wounds treated with octylcyanoacrylate tissue adhesive vs. monofilament sutures and correlated the early, three-month and one-year cosmetic outcomes.10 This study led the authors to recommend indications for the use of tissue adhesives shown in Table 1.10 If wound edges are separated more than 5 mm by underlying skin tension, the wound is unlikely to stay closed with tissue adhesives alone.9 Relatively short wounds also are preferred candidates for tissue adhesive closure.

A recent Cochrane review of tissue adhesives was done to summarize the best available evidence for the effect of tissue adhesives in the management of lacerations in children and adults.8 Included in the review were eight studies that compared a tissue adhesive with standard wound care. No significant difference was found for cosmesis at any of the time points examined. Pain scores and procedure time significantly favored tissue adhesives. A small but statistically significant increase in wound dehiscence was found in the tissue adhesives group. Until recently, Dermabond was the only FDA-approved tissue adhesive being used in the United States. In September 2002, n-butyl-2-cyanoacrylate (Indermil) was approved for use.
Wounds that are to be closed with a tissue adhesive should be cleaned and irrigated in a similar manner as for lacerations that would be closed with sutures or staples. The wound edges should be approximated with fingers or forceps, and the skin surface must be dry. To use Dermabond, the inner glass vial must be cracked by squeezing the outer plastic cylinder and forcing the liquid through the applicator tip onto the wound surface.11 Three to four thin layers of Dermabond should be painted over the opposed wound edges, extending at least 5 mm beyond the edges of the wound, in the direction of the long axis of the wound. The wound edges should be held together manually for at least 30 seconds after Dermabond application to complete polymerization.10,11 (See more on problems and prevention, Table 2, p. 3.)

Aftercare instructions should include prohibiting the use of antibacterial or other petroleum-based products on the wound as these hasten the breakdown of the adhesive. The wound should not be soaked in water and should not be scrubbed. It may be washed gently after 24 hours. No dressing is required, as tissue adhesives provide their own dressing. The adhesive typically sloughs off in 7-10 days.10,12,13
Staples. Closing lacerations with skin staples has several advantages over suturing: speed of repair, lower cost, and low level of tissue reactivity. In prospective, randomized studies of stapling vs. suturing, stapling was shown to be less costly than suturing (with that advantage increasing as the laceration length increases), overall time for wound care was shorter, and there were no additional complications.14,15 Overall, staples have been shown to produce cosmesis identical to that from sutures when used on the scalp, neck, trunk, and extremities.14-16 Wounds that can be considered for staple closure include linear lacerations with sharp, straight edges on the extremities, scalp, or trunk. Prior to stapling a wound, the wound edges should be approximated, but this often is difficult to do adequately. Staples should not be used for deep scalp lacerations with active bleeding or on the face, neck, hands, or feet. Deep sutures should be placed when necessary to reduce skin tension. Avoid placing staples too tightly, as this can lead to tissue ischemia and necrosis. The timing of staple removal is the same as the timing of suture removal and is specific for the body part involved.
Sutures. The goal of suturing is to reduce skin tension while approximating opposing wound edges. Excessive tension leads to unnecessary scarring, wound necrosis, and possible dehiscence. Placement of deep sutures helps reduce skin tension and decrease dead space and hematoma formation. All of these factors likely will improve cosmetic outcome, although well-designed trials to prove this are lacking.5
The use of subcuticular or subcutaneous sutures had both advantages and disadvantages. The use of buried, absorbable subcuticular sutures decreases the tension on wound edges, maintains eversion for a prolonged period of time, and provides tensile support. This allows for early removal of transdermal sutures, which decreases the likelihood of suture track marks and minimizes scarring overall.17-19 It probably is best to avoid subcuticular sutures for acute wounds, except for the cleanest wounds in cosmetically important areas.
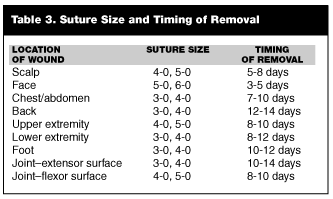
Deep sutures do not increase infection rate in low-risk wounds20,21 Sutures should not be placed through adipose tissue, as they will not hold tension and will increase the infection rate.5 Using the smallest diameter suture that adequately will close the wound can minimize scarring. Characteristics of the various suture types as well as size choices and time to removal are summarized in Table 3.
Skin-Closure Tapes. Skin closure tapes can be used to close a wound primarily or to provide additional support after suture or staple removal. Skin tapes work best for a superficial straight laceration that is under little tension. They also can be used to close lacerations that are under a splint or cast to preclude the need for suture or staple removal. Skin tapes can be used to repair skin tears in the elderly, as their skin often is too friable to hold suture. Tapes alone cannot maintain wound integrity in areas subject to tension.5
The wound and surrounding skin must be clean and dry. Adherence of the tape to the skin is improved by the use of benzoin painted on the skin 2-3 cm beyond the wound edges. Care should be taken not to allow any benzoin to enter the wound, as this can cause induration and wound infection.18 If properly applied, the tapes will fall off in a few days when the skin exfoliates.9
(Editor’s note: This story originally was written by Lisa Freeman, MD, FACEP, assistant professor, associate program director, department of emergency medicine, University of Texas Medical School at Houston; and Rajeev S. Pethe, MD, department of emergency medicine, University of Texas Health Sciences Center, Houston. It was peer reviewed by J. Stephan Stapczynski, MD, professor, department of emergency Medicine, University of Kentucky College of Medicine, Lexington; and Judd Hollander, MD, associate professor, clinical research director, department of emergency medicine, University of Pennsylvania Health System, Philadelphia.
It originally was edited by Gideon Bosker, MD, FACEP, Assistant Clinical Professor, Yale University School of Medicine, New Haven, CT.)
References
1. Hollander JE, Singer AJ, Valentine SM, et al. Risk factors for infection in patients with traumatic lacerations. Acad Emerg Med 2001; 8:716-720.
2. McCaig LF, Nghi L. National Hospital Ambulatory Medical Care Survey: 2000 Emergency Department Summary. Advance data from Vital and Health Statistics, no. 326. Hyattsville, MD: National Center for Health Statistics, 2000.
3. Singer AJ, Hollander JE, Quinn JV. Evaluation and management of traumatic lacerations. N Engl J Med 1997; 337:1,142-1,148.
4. Singer AJ, Mach C, Thode HC Jr, et al. Patient priorities with traumatic lacerations. Am J Emerg Med 2000; 18:683-686.
5. Hollander JE, Singer AJ. Laceration management. Ann Emerg Med 1999; 34:356-367.
6. Hollander JE, Singer AJ, Valentine S, et al. Wound registry: Development and validation. Ann Emerg Med 1995; 25:675-685.
7. Lammers RL. "Principles of Wound Management." In: Roberts JR, Hedges JR, eds. Clinical Procedures in Emergency Medicine, 3rd ed. St. Louis: W.B. Saunders Co.; 1998: p. 535.
8. Farion K, Osmond MH, Harting L, et al. Tissue adhesives for traumatic lacerations in children and adults (Cochrane review). Cochrane Database Syst Rev 2002; (3):CD003326.
9. Kroot LJ. Emergency wound management. In: Tintinalli JE, Kelen GD, Stapczynski JS, eds. Emergency Medicine: A Comprehensive Study Guide, 5th ed. New York City: McGraw Hill; 2000:293.
10. Quinn J, Wells G, Sutcliffe T, et al. Tissue adhesive versus suture wound repair at 1 year: Randomized clinical trial correlating early, 3-month and 1-year cosmetic outcome. Ann Emerg Med 1998; 32:645-649.
11. Yamamoto LG. Preventing adverse events and outcomes encountered using Dermabond. Am J Emerg Med 2000; 18:511-515.
12. Singer AJ, Quinn JV, Clark RE, et al. Closure of lacerations and incisions with octylcyanoacrylate: A multicenter randomized controlled trial. J Fam Pract 2002; 51:517.
13. Seropian R, Reynolds BM. Wound infections after preoperative depilatory versus razor preparation. Am J Surg 1971; 121:251-254.
14. Orlinsky M, Goldberg RM, Chan L, et al. Cost analysis of stapling versus suturing for skin closure. Am J Emerg Med 1995; 13:77-81.
15. Kanegaye JT, Vance CW, Chan L, et al. Comparison of skin stapling devices and standard sutures for pediatric scalp lacerations: A randomized study of cost and time benefits. J Pediatr 1997; 130:808-813.
16. Bickman KR, Lambert RW. Evaluation of skin stapling for wound closure in the emergency department. Ann Emerg Med 1989; 18:1,122.
17. Austin PE, Dunn KA, Eily-Cofield K, et al. Subcuticular sutures and the rate of inflammation in uncontaminated wounds. Ann Emerg Med 1995; 25:328-330.
18. Panek PH, Prusak MP, Bolt D, et al. Potentiation of wound infection by adhesive adjuncts. Am Surg 1972; 38:343-345.
19. Mehta PH, Dunn KA, Bradfield JF, et al. Contaminated wounds: Infection rates with subcutaneous sutures. Ann Emer Med 1996; 27:43-48.
20. Dire DJ, Cpopola M, Dwyer DA, et al. Prospective evaluation of topical antibiotics for preventing infections in uncomplicated soft-tissue wounds repaired in the emergency department. Acad Emerg Med 1995; 2:4-10.
21. Knapp JF. Updates in wound management for the pediatrician. Ped Clin NA 1999; 46:1,201-1,204.
CE Objectives
After reading this issue of Emergency Nursing Reports, the continuing education participant will be able to:
- identify a way to decrease wound infection.
- list the type of wound most appropriately closed with tissue adhesives.
- identify an advantage of using staples for wound closure.
- describe when skin-closure tapes may be used.
CE Questions
1. Wound infection may be decreased by:
A. leaving devitalized tissue in the wound.
B. extending the length of the wound.
C. decreasing tissue contamination.
D. making an effort to minimize only the worst pain involved in wound repair.
2. Tissue adhesives are recommended for closure of which of the following wounds?
A. Dog bites of the hand
B. Knife wounds over the finger joints
C. Short well-approximated facial wounds
D. Crush wounds of the foot
3. An advantage to the use of staples for wound closure include:
A. Time required providing wound care is shorter.
B. There is an increased risk of complications over regular sutures.
C. Staples do not provide good cosmesis.
D. They can be used to close only scalp wounds.
4. Skin-closure tapes may be used to close which of the following wounds?
A. Wounds with a great deal of skin tension
B. Skin tears in the elderly
C. Combination wounds
D. A deep laceration over a finger joint
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
