Urinary Tract Infection: Risk Stratification, Clinical Evaluation, and Evidence-Based Antibiotic Therapy, Part II
Part II: Antibiotic Selection, New Treatment Options, and Special Considerations
Authors: Romolo Gaspari, MD, FACEP, Research Director, Assistant Professor, Department of Emergency Medicine, University of Massachusetts School of Medicine, Worcester; and Gideon Bosker, MD, FACEP, Assistant Clinical Professor, Yale University School of Medicine, New Haven, CT.
Peer Reviewers: David S. Howes, MD, FACEP, Program Director and Chairman, Residency Program, Department of Emergency Medicine, University of Chicago Hospitals and Clinics; Associate Professor, Pritzker School of Medicine, Chicago, IL; and Ralph J. Riviello, MD, FACEP, Assistant Professor, Department of Emergency Medicine, Thomas Jefferson University, Philadelphia, PA.
This issue is the second and final part in our series on urinary tract infection (UTI). Part I of the series examined epidemiology, emerging resistance patterns, and patient-specific treatment strategies. In part II, we will cover antibiotic selection, new treatment options, and special considerations.—The Editor
Antibiotic Selection for UTI: General Principles and Overview of Therapeutic Options
Because of the relative predictability of uropathogens, and the time delay associated with urine culture results, antibiotic treatment for UTIs relies heavily on empiric therapy. Recent changes in antibiotic resistance trends, however, have forced a reassessment of empiric choices for managing UTI. As is the case for nearly all infections, the ideal antibiotic for UTI is one that provides predictable coverage against all pathogens likely to cause the disease, offers significant penetration of the urinary system and adequate urine concentrations, has few side effects, and shows low resistance rates in the local community to the expected uropathogens. A wide range of treatment options has been studied extensively and reported in the medical literature; however, interpretation of older studies, in particular, must be considered in light of current resistance patterns.
Fluoroquinolones: Current Agents of Choice. With rapidly changing resistance patterns among the common uropathogens, standard first-line treatment (i.e., trimethoprim-sulfamethoxazole [TMP-SMX]) is being replaced in many instances by the fluoroquinolone class. Derivatives of nalidixic acid, fluoroquinolones were discovered accidentally in the early 1960s during the synthesis of the anti-malarial agent chloroquine.1 To date, more than 10,000 analogues of nalidixic acid have undergone initial screening, and the first fluoroquinolone antibiotic was approved for clinical use in the late 1980s.1 These highly effective antimicrobials act on bacterial topoisomerases, a class of enzymes that is essential for maintaining the physicochemical stability and biological activity of bacterial DNA.1 In general, the newer quinolones have longer serum half-lives, with proven post-antibiotic effects from one to six hours; this allows patient-friendly, single- or twice-daily dosing and higher peak levels for maximum bactericidal activity. Recent approval of extended release ciprofloxacin (Cipro XR®)2 has made available an effective, well-tolerated, and safe once-daily preparation of what most clinicians concur has become the gold standard of therapy for UTI.1
In addition, fluoroquinolones are well-absorbed from the gastrointestinal tract, and in the case of ciprofloxacin, equivalent clinical outcomes in selected patient populations with moderate to severe UTI have been established between patient groups who received this drug intravenously and those who received oral therapy.3-5 The fluoroquinolones have excellent penetration into various tissues; they are well-distributed intracellularly, and have the added benefit of eliminating perineal, vaginal, and perirectal reservoirs of uropathogens without altering normal bowel or vaginal flora.1,6
As mentioned, the high oral bioavailability of fluoroquinolones allows switching from intravenous to oral therapy without dosage adjustments.7 Excretion is primarily renal, although some of the compounds have exclusive hepatic metabolism or a combination of the two.1 They have an extended spectrum of bactericidal activity against gram-negative rods, including Pseudomonas, gram-positive cocci, and intracellular pathogens.6,7 Fluoroquinolones remain classified as category C drugs, requiring practitioners to rule out pregnancy before prescribing them to potentially pregnant patients.1
The armamentarium of commonly used fluoroquinolones is expanding at a rapid rate. Ciprofloxacin (Cipro®), which has been a clinically proven gold standard for oral and intravenous-based therapy of UTIs, has been joined by other agents, many of which also are indicated for community-acquired pneumonia (CAP). The new extended release formulation of ciprofloxacin likely will become the new standard of care for uncomplicated UTI. Other members of this class include gatifloxacin (Tequin®), levofloxacin (Levaquin®), and ofloxacin (Floxin®). Low levels of resistance to fluoroquinolones are beginning to appear through two mechanisms: chromosomal mutations or alterations affecting the ability of fluoroquinolones to permeate the bacterial cell wall.1 Fortunately, separate isomerases are required to produce this form of resistance; therefore, the emergence of a predictably resistant organism would require a rare double mutation.1
An extensive body of clinical research confirms that fluoroquinolones are extremely effective for the treatment of UTIs ranging in severity from uncomplicated cystitis to urosepsis.8 As would be expected, many studies evaluating newly introduced quinolones compare clinical trial outcomes to the established track record of ciprofloxacin, which has become a standard choice for initial, empiric therapy for most UTIs. In a clinically controlled trial comparing three days of oral ciprofloxacin with seven days of TMP-SMX or nitrofurantoin, bacteriologic cure rates for uncomplicated UTI after 4-6 weeks were 91%, 79%, and 82%, respectively.9 Clinical cure rates after 4-10 days were similar among the three groups, as was the overall incidence of adverse events. The superior efficacy of ciprofloxacin as compared to TMP-SMX also has been confirmed in patients with acute pyelonephritis.10
In certain studies of acute uncomplicated cystitis, levofloxacin preliminarily has been shown to have equal efficacy in single doses as in the standard longer dosing regimens.11,12 Ciprofloxacin and norfloxacin are effective in either once- or twice-daily dosing regimens in uncomplicated UTI.13,14 For complicated UTIs, including pyelonephritis, levofloxacin and lomefloxacin have equivalent bacteriologic and clinical cure rates to ciprofloxacin. Of the newer fluoroquinolones, only levofloxacin is approved for both upper and lower UTIs.
Despite the effectiveness of newer fluoroquinolones for UTI, overuse of the extended spectrum fluoroquinolones (i.e., levofloxacin and gatifloxacin) for outpatient and hospital-based management of UTI must be considered in light of recommendations made by the Centers for Disease Control and Prevention (CDC). The CDC has documented concerns about emerging resistance to common pathogens implicated in CAP. The fluoroquinolone ciprofloxacin is a preferred oral agent for the treatment of Pseudomonas aeruginosa urinary infections.10 It should be emphasized that although other quinolones may demonstrate activity against, and may be indicated for treatment of gram-negative organisms implicated in UTI, some of these antibiotics, especially those extended spectrum fluoroquinolones that also are used for initial, empiric treatment of CAP, are active against Streptococcus pneumoniae.
Given the recently reported increase in resistance among S. pneumoniae species to levofloxacin, attempts should be made to limit selective pressures caused by the overuse of these agents. Consequently, the use of so-called advanced generation fluoroquinolones (AFQs) as initial, first-line agents for UTI should be discouraged because of concerns about emerging resistance among S. pneumoniae species implicated in CAP. This cautionary approach is supported by a recent guidelines document issued by the CDC’s Drug-Resistant Streptococcus Pneumoniae Therapeutic Working Group.
In this regard, because of significant concerns about, as well as documentation of, emerging resistance to S. pneumoniae, the CDC panel has recommended that extended spectrum fluoroquinolones (i.e., levofloxacin, gatifloxacin, etc.) be reserved for selected patients with CAP. In light of this position, which is intended to prevent excessive use of advanced fluoroquinolones and reduce selective pressures against pulmonary pathogens causing CAP, it appears prudent to limit their potential for inducing resistance in the community and reserve such antibiotics as alternative agents in patients with UTI. This approach appears to be justified, especially because an effective and safe fluoroquinolone (i.e., extended release ciprofloxacin ) is available for uncomplicated UTI, and does not have significant activity against gram-positive organisms causing CAP. Accordingly, ciprofloxacin is recommended as the initial fluoroquinolone of choice for managing patients with UTI.
Outcome-Optimizing and Compliance-Enhancing Antimicrobials for Uncomplicated UTI: Guiding the Gold Standard
Optimizing Clinical Outcomes in Uncomplicated UTI. The recent introduction of extended release ciprofloxacin has made it possible to potentially enhance medication compliance through once-daily administration of this gold standard antimicrobial for uncomplicated UTI with a preparation that achieves an area under the curve (AUC) that is equivalent to conventional BID ciprofloxacin, and a Cmax that is 40% higher.2
The new, extended release formulation features a number of attributes, including absorption that is limited to the upper gastrointestinal tract, and a unique bilayer matrix design that permits about 35% of the dose to be released immediately and the remaining 65% to be released over an extended period. Good urine concentrations are maintained throughout the dosing interval.
Because of its potentially compliance-enhancing properties (once-daily dosing and a well-tolerated side effect profile), extended release delivery system, and clinically effective urine concentrations, the extended release formulation represents a risk-management upgrade as compared to BID ciprofloxacin; therefore, it should replace the older formulation as the clinical standard for treatment of uncomplicated UTI when indicated. A well-designed clinical trial (please see "Clinical Studies" below) supports this shift to the once-daily, extended release formulation.
Clinical Studies. To evaluate the clinical usefulness and possible advantages of extended release ciprofloxacin, a study was designed to compare the efficacy and safety of extended release ciprofloxacin 500 mg QD to conventional immediate-release ciprofloxacin 250 mg BID for women with uncomplicated UTI. This study design, which represented the U.S. pivotal trial, was a double-blind, randomized phase III study enlisting adult, non-elderly, non-pregnant, outpatient women with acute uncomplicated UTI.2
With 422 total evaluable patients, the two treatment arms compared a three-day course of extended release 500 mg once-daily vs. conventional 250 mg twice-daily administration. Efficacy of these regimens, which included assessment of bacteriological eradication and clinical cure, was measured at 4-11 days (test-of-cure visit) and at 25-50 days (late follow-up visit) following completion of therapy. In addition, adverse event monitoring, which included documentation of possible drug-related adverse events as well as laboratory parameter evaluation, was included in the study design.
To ensure the study population reflected real world patients with uncomplicated UTI, inclusion criteria required that at least two of the following signs and symptoms of uncomplicated UTI be present: dysuria, frequency, urgency, or suprapubic pain. An infectious etiology for this symptom complex was confirmed on the basis of a positive mid-stream, clean-catch urine culture, demonstrating a uropathogen 105 cfu/mL or greater, and pyuria (> 10 leukocytes/mm3). The study excluded individuals with asymptomatic bacteriuria, evidence of complicated UTI, three or more UTIs in the previous year, or anatomic/medical factors predisposing to UTIs.
Baseline Characteristics. The extended release ciprofloxacin (500 mg QD x 3 days) and conventional ciprofloxacin (250 mg BID x 3 days) treatment groups were well-matched with respect to baseline characteristics. The mean age of patients in the ciprofloxacin extended release group was 34.3 years, and 35.1 years in the ciprofloxacin conventional group (CipBID). Eighty-nine percent of the extended release ciprofloxacin patients had a duration of infection lasting for two or more days, and 82% of those in the CipBID group had a duration of two or more days prior to treatment.
Clinical Cure and Bacteriologic Eradication Rates. The causative organism at time of enrollment was E. coli in about 80% of patients in both treatment groups, with E. faecalis, K. pneumoniae, P. mirabilis, and S. saprophyticus each being encountered in fewer than 10% of cases. Overall, 99% of the pre-therapy isolates were susceptible to ciprofloxacin. Clinical cure rates were 95% for extended release ciprofloxacin vs. 93% for CipBID for efficacy-valid comparisons. Intent-to-treat results were similar, with a 90% cure rate for QD extended release ciprofloxacin vs. 93% for CipBID. Clinical response at late follow-up visits also were reported in this study, and revealed that continued clinical cure rates were 89% for extended release ciprofloxacin vs. 87% for CipBID. Failures were seen in only 9% of QD extended release ciprofloxacin and in 16% of patients in the CipBID treatment arms.2
With respect to bacteriologic eradication by organism, extended release ciprofloxacin and CipBID demonstrated comparable results at the test-of-cure visit. Overall, 97% of E. coli were eradicated in both groups, with comparable rates of bacteriologic eradication, ranging from 79% to 98%, observed for both formulations among such uropathogens as E. faecalis, P. mirabilis, S. saprophyticus, and K. pneumoniae. Continued eradication was reported for 86% of QD extended release ciprofloxacin and 81% of CipBID patients. Recurrence was reported at a similar rate in both treatment groups (8% each).
Drug-Related Adverse Events. The extended release formulation, extended release ciprofloxacin, demonstrated a side effect, safety, and tolerability profile that was comparable to CipBID, with an overall drug-related adverse event rate of 10% (46/444 patients) for the extended release formulation and 9% (41/447) for the conventional formulation. (See Table 1.) No serious drug-related adverse events were seen in either treatment arm.
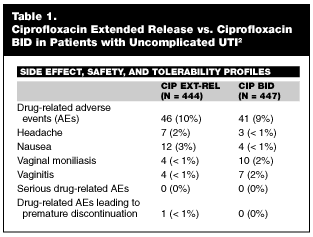
Conclusions. This study demonstrated that once-daily extended release ciprofloxacin achieved bacteriologic eradication and clinical cure in greater than 94% of patients, had a comparable safety profile to ciprofloxacin BID, and was as effective as ciprofloxacin BID in treating women with uncomplicated UTI.
Disease-Specific Urinary Tract Infection Syndromes: Antimicrobial Management
Asymptomatic Bacteriuria. Treatment recommendations for asymptomatic bacteriuria are consistent for most patient populations. There is little evidence that attempting to eradicate bacteria from the urine of most patients who are asymptomatic has any clinical benefit. The largest potential risk when repeatedly treating asymptomatic bacteriuria is in the selection of more virulent or resistant pathogens. The one patient subgroup for which treatment uniformly is recommended is in pregnancy. Pregnant women with asymptomatic bacteriuria should be treated with three days of a beta-lactam, nitrofurantoin, or in unusual cases, TMP-SMX.15 However, TMP-SMX should not be used during the first trimester or near term. Treatment is not recommended for asymptomatic bacteriuria in non-pregnant patients.
Acute Bacterial Cystitis. Available therapies for uncomplicated acute bacterial cystitis include a wide range of antibiotic options and treatment durations. Fortunately, guidelines issued by the Infectious Disease Society of America in 1999 provide a practical, evidence-based guide for the practitioner.16 Additional research and focus on resistance issues have helped refine the clinical approach to management of UTI.
The appropriate length of treatment for uncomplicated UTI has received a considerable amount on attention, with recommended treatment regimens ranging from 1-14 days of duration. A review of the literature suggests that three days of therapy with appropriate antibiotics is more effective than one day, but equally effective as longer courses.16 It should be noted that, despite its widespread use, the commonly employed three-day treatment course with TMP-SMX does not currently carry a formal FDA indication for the treatment of cystitis. Some antibiotics, such as the beta-lactams and nitrofurantoin, may be less effective when given for three days as compared to longer periods of time.17,18 However, three days of therapy with approved fluoroquinolones is sufficient for the treatment of acute, uncomplicated cystitis.
A variety of antimicrobial agents can be used in the treatment of uncomplicated lower UTIs. Among the most commonly used are beta-lactams, fluoroquinolones, TMP-SMX, nitrofurantoin, and fosfomycin. Beta-lactams were used extensively in the 1970s, but increasing resistance has led to the dependence on other antibiotics. Recent studies, however, demonstrate that 40% of the most common uropathogens are resistant to beta-lactams.19,20 Nevertheless, beta-lactams are still the drug of choice in some patient populations, including pregnant women and individuals with UTIs caused by enterococcus. Recommended therapy for cystitis during pregnancy is a three-day course with either amoxicillin 500 mg PO TID; cephalexin 250 mg PO QID; or a 10-day treatment course with nitrofurantoin 100 mg PO QHS.15 Sulfonamides may interfere with bilirubin binding and cause hyperbilirubinemia in newborns; therefore, they are not recommended near term.
TMP-SMX has been used extensively during the past decade for the treatment of lower UTIs, and was considered the antibiotic of choice until recently.21 A meta-analysis encompassing several studies evaluating the efficacy of TMP-SMX indicates a cure rate of 93% using a three-day course.16 The slightly increased relapse rate of the three-day vs. the seven-day treatment course was counterbalanced by the decrease in side effects. The three-day regimen for TMP-SMX is 160/800 mg orally every 12 hours.
As stressed earlier, the use of TMP-SMX for first-line therapy in cystitis has been affected by recent recognition of increasing resistance rates in most areas of the United States.19,22,23 The current recommendations are to use TMP-SMX as the first-line agent for cystitis in areas where TMP-SMX resistance is less than 10-20%, as there is evidence that other antibiotics are more effective from both a clinical and cost perspective when the resistance rates exceed 10-20%.16 In one important analysis, researchers conducted a cost analysis for uncomplicated UTIs that supported switching from empiric treatment with TMP-SMX to ciprofloxacin when community resistance to TMP-SMX surpassed 20%.24
Nitrofurantoin is a well-established urinary tract antibiotic that, to a great degree, has fallen out of favor because of its four-times-daily dosing schedule. A newer formulation permits twice-daily dosing. Nitrofurantoin is highly concentrated in the urine and achieves minimal tissue levels, making it an ideal antibiotic for UTIs. Unfortunately, the cure rates for this antibiotic can be as low as 80%.18,25 The newer formulation is given 100 mg BID for 7-10 days. Nitrofurantoin remains a second- or third-line therapy in most patient populations.
Fosfomycin tromethamine is a newer antibiotic that has been approved for single-dose therapy of uncomplicated UTI. Although some trials have found that fosfomycin is as effective as other first-line agents,26 this is not universally accepted. A study in 1999 evaluating fosfomycin in UTI found a clinical cure rate of 80%.27 Two other small studies found fosfomycin to be as effective as norfloxacin, but with a higher rate of side effects.28,29 The clinical data on fosfomycin still is evolving, and further information is needed before it can be advocated as a first-line agent.
In most areas of the country, fluoroquinolones have become the first-line agent of choice for uncomplicated lower UTI. Of the fluoroquinolones, ofloxacin, norfloxacin, ciprofloxacin, gatifloxacin, and levofloxacin all either partially or totally are cleared by the kidneys and cover the majority of uropathogens.30 Some of the newer fluoroquinolones have little or no renal penetration and are not suitable for treating UTIs. As a group, the fluoroquinolones have been found to be highly effective for treatment of UTI. As outlined earlier, the recently introduced extended release formulation of ciprofloxacin should replace the older formulation as the clinical standard for treatment of uncomplicated UTI when indicated. (See Table 2.)
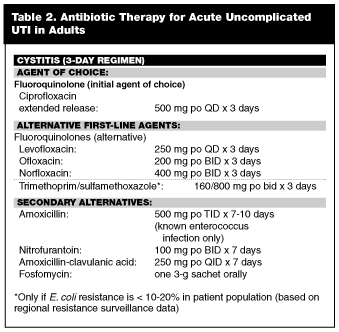
The suprapubic discomfort or dysuria common to UTI can be treated with oral analgesics (i.e., acetaminophen or ibuprofen) or phenazopyridine with a TID dose of 100-200 mg for no more than 48 hours.31 Elderly females with lower UTI symptoms and no systemic complications may be treated for three days with similar regimens as prescribed for younger women.32 In patients suspected of having a complicated UTI, including patients with symptoms lasting longer than one week, diabetic patients, immunocompromised individuals, and nontoxic febrile patients without evidence of acute pyelonephritis, the treatment duration should be between five and seven days.33 Because these patients are less able to tolerate treatment failures and are more susceptible to recurrent infection, ciprofloxacin is recommended as the initial agent of choice. Moreover, in these patients, a urine culture is recommended prior to administration of antibiotics to ensure proper management and identification of the uropathogen in the event of treatment failure or recurrence.33
Complicated Urinary Tract Infections
Adult patients with pyelonephritis can be managed on an inpatient or outpatient basis, depending upon clinical severity. A retrospective comparison of inpatient and outpatient management of pyelonephritis suggested that general guidelines for admission should include the following: 1) underlying anatomical urinary tract abnormality; 2) an immunocompromised host (i.e., diabetes mellitus, cancer, sickle cell disease, transplant patients); 3) urinary tract obstruction; 4) failed outpatient management of pyelonephritis; 5) progression of uncomplicated UTI; 6) persistent vomiting; 7) renal failure; 8) suspected urosepsis; 9) age older than 60; 10) poor social situation; and 11) inadequate access to follow-up.34 If these criteria are used for making in-hospital dispositions, it is estimated that 70% of all patients who are treated for pyelonephritis can be managed as outpatients.35
The general consensus for emergency department management of pyelonephritis is to begin parenteral therapy with a fluoroquinolone (ciprofloxacin) intravenously in patients who meet admission criteria.36 Non-toxic patients with uncomplicated pyelonephritis suitable for outpatient management may receive oral ciprofloxacin for a total of 7-14 days, depending on clinical judgment and hospital protocols.36 Other parenteral therapies include a combination of ampicillin or a third-generation cephalosporin plus an aminoglycoside in extended-interval dosing (i.e., every 24-48 hours).37-40 The extended spectrum cephalosporins, such as ceftriaxone, should be considered for serious urinary infections because of the high urinary concentrations that are achieved.41
If gram-positive cocci are the causative organism, ampicillin/ sulbactam with or without an aminoglycoside is recommended.42 Admitted patients with suspected enterococci may require extended spectrum penicillins or alternative therapies, including nitrofurantoin to treat isolated vancomycin-resistant enterococci (VRE). Because multi-drug resistance is common in VRE isolates, susceptibility testing is recommended for ampicillin, aminoglycosides, chloramphenicol, fluoroquinolones, minocycline (a tetracycline), and rifampin.41 UTI caused by Pseudomonas often will require double antimicrobial coverage.
Acute Pyelonephritis. Patients with pyelonephritis generally are more ill than those with uncomplicated cystitis. As would be expected for a more invasive infection, the recommended treatment duration is significantly longer. Although some studies have shown a shorter duration of therapy may be effective,43-45 most authors recommend a seven- to 14-day treatment course for pyelonephritis.16,21 Intravenous therapy commonly is administered to patients with more severe illness, with oral therapy reserved for outpatient treatment. However, there are few data demonstrating superiority of intravenous over oral antibiotics. Even for patients who will be managed as outpatients, many physicians will give at least one dose of IV antibiotic, followed by oral therapy for the duration of the treatment course.
To evaluate the efficacy and cost of antibiotics used in pyelonephritis, a randomized, double-blind, multicenter trial analyzed 255 women with acute uncomplicated pyelonephritis. These patients received either ciprofloxacin 500 mg BID for seven days or TMP-SMX 160/180 mg BID for 14 days.10 More than 90% of UTI culture isolates from both groups were E. coli. Bacteriologic and clinical cure rates were greater at 4-11 days in the ciprofloxacin group (99% and 96%, respectively) than the TMP-SMX group (89% and 83%, respectively). At 22-28 days, bacteriologic and clinical cure rates were 84% vs. 74% and 82% vs. 74%, respectively. Bacterial and clinical cure rates with TMP-SMX in patients found to be infected with resistant E. coli were only 50% and 35%, respectively. Adverse effects were similar among groups, occurring in 24% with ciprofloxacin and in 33% with TMP-SMX. Health care resource use and estimated total treatment costs were calculated, from initial evaluation to prescription pad to cure, including needed hospitalization, lab testing, office visits, and other procedures. Mean total cost per patient was 29% higher for TMP-SMX-treated patients than for ciprofloxacin-treated patients.10
Because of additional interventions and antibiotic prescriptions required in the TMP-SMX group to achieve a cure, the mean cost per cure also was 25% higher in the TMP-SMX group than in the ciprofloxacin-treated patients. These studies help confirm that knowledge of local resistance rates is imperative in deciding which antibiotics should be used in the treatment of UTI. They support the use of ciprofloxacin as a first-line agent in the management of uncomplicated pyelonephritis. With the current outcome- and cost-sensitive environment of managed care, clinicians must make informed choices in the management of their patients.10,42 A related randomized trial found that oral and intravenous ciprofloxacin equally are effective in the empiric treatment of severe pyelonephritis or complicated UTIs, provided that severe sepsis, obstruction, and focal renal suppuration are not present.46 Since all patients in this study were hospitalized, a direct comparison between inpatient and outpatient treatment with ciprofloxacin still is needed.
In pregnant women, pyelonephritis tends to occur more commonly during the second half of pregnancy.47 In general, outpatient treatment is not the standard of care for pregnant women. Inpatient treatment with intravenous antibiotics and close monitoring usually are required to maximize outcomes. Treatment options are similar to other adult regimens, including ampicillin with gentamicin, cephalosporins, and extended spectrum penicillins or aztreonam.47 Patients may be discharged safely and parenteral therapy stopped after defervescence within 48-72 hours of admission.48 Persistent fever or symptoms require further evaluation and consultation.
A study of more than 100 women with uncomplicated pyelonephritis at fewer than 24 weeks gestation found that almost 10% of those treated initially as outpatients eventually required hospitalization.49 Two additional studies suggest that, in very carefully selected patients, outpatient treatment may be a safe option.50,51 However, without concise, evidence-based protocols or guidelines to guide this decision, the acceptable and prudent choice in pregnant women is to admit them for initial parenteral antibiotics and supportive care. In both nonpregnant adults and pregnant patients, failure to respond to appropriate antibiotics requires emergent radiologic studies, including ultrasound and possible computed tomography (CT) scan, to evaluate for obstruction, masses, and renal and perirenal abscess. All patients should have follow-up urine cultures 1-2 weeks after completion of therapy to ensure eradication of infection. (See Table 3.)
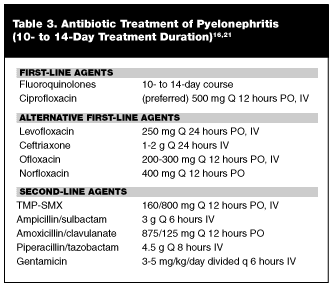
UTI Management in High Risk Populations
Catheterized Patients (Indwelling and Intermittent). A significant percentage of complicated UTIs originate in patients with chronic indwelling bladder catheterization. Studies show that following initial indwelling bladder catheterization, 5% of patients per day will develop bacteriuria.52 Patients with long-term catheterization invariably are bacteriuric.53-54 Prophylactic antibiotics lower the incidence of bacteriuria,55-56 at the expense of selecting out more virulent organisms.57-59 Currently, prophylactic antibiotics in catheterized patients are not recommended.60
A small percentage of patients with bacteriuria will progress to symptomatic UTI.57 However, the vast majority will clear spontaneously.61 In an autopsy study comparing catheterized and uncatheterized patients, catheterized patients were seven times more likely to have renal inflammation or pyelonephritis.62 Although smaller studies have shown an increased mortality associated with nosocomial UTIs,53,63 definitive investigations in this area have not yet been conducted.
Intermittent bladder catheterization may substitute for chronic indwelling catheters in some patient populations. Spinal cord injury (SCI) can cause a neurogenic bladder, resulting in functional obstruction during urination. These patients have a much higher rate of UTI,64 and the value of intermittent catheterization has been well established.65-67 One study followed daily urine culture and analysis for 60 days of intermittent catheterization and found a total of 178 episodes of bacteriuria from 25,780 catheterizations.68
The consequences of and approach to asymptomatic bacteriuria in SCI patients is not universally agreed upon, as some authors believe that bacteria in the urine serves as a reservoir for more serious infections.69 Studies reviewing various methods of ridding SCI patients of bacteria in their urine have shown mixed results.64,70,71 Using antibiotics to prevent UTI does not seem to have any lasting effect and may pre-select out more virulent pathogens. One consensus panel of experts in the field recommends no treatment of asymptomatic bacteriuria in this population.72
Urinary Tract Infection in Men. UTIs in young men are uncommon and, consequently, they are classified as complicated by some authors.21 The significant difference in UTI rates between men and women of the same age is thought to be due to anatomical differences between the sexes. Among other factors, the length of the urethra, a drier environment surrounding the meatus, and antibacterial properties of prostatic fluid contribute to a lower rate of infection in men.73 Some of the risk factors that have been identified in men are homosexuality,72 sex with an infected partner,74 prostatic hypertrophy,73 and lack of circumcision,75 but this is not agreed upon universally.76
Some of the differences between UTIs in men and women support the classification of male UTIs as complicated. E. coli has been found to be the most common infectious agent in male UTIs, with a distribution of pathogens closer to that found in complicated female UTIs.73,76 Although uropathogens in men show an increased virulence as compared to those seen in women,77 the symptoms of male cystitis are similar to those seen in women.76 A urine culture is recommended in the workup of male patients with dysuria, with 103 cfu/mL considered to be positive.
Because of the relatively small number of clinical studies on UTIs in men, treatment recommendations in this population are based on studies in women.78 As a rule, seven days of antibiotic therapy are recommended for the treatment of a lower UTI, and 14 days for pyelonephritis. Recurrent UTIs require a six-week regimen.73 Studies in men have shown that asymptomatic bacteriuria in men does not require treatment.79,80
Prostatitis always must be considered in the differential diagnosis. The male urethra courses through the center of the prostate on its way to the bladder. This relationship allows for invasion of urinary tract pathogens into the prostate, causing acute bacterial prostatitis. Patients with prostatitis will present with symptoms of a UTI and a large, tender prostate.81 The enlarged prostate also may cause symptoms of bladder obstruction by physically blocking urine flow. The agents that cause prostatitis are the same gram-negative agents that cause UTI. Treatment for acute bacterial prostatitis may include TMP-SMX or a fluoroquinolone and should last four weeks. Ciprofloxacin is recommended for treatment for chronic prostatitis and requires a treatment duration of 6-12 weeks.82
Renal Stones and UTIs. Although not common, the coexistence of nephrolithiasis and infection may have serious consequences. Renal stones associated with infection usually are one of two types: struvite or apatite, although any type of renal stone may be associated with infection. Struvite stones usually are found in women with recurrent infections and are associated with urease-producing organisms such as Proteus mirabilis and Providencia stuartii.83 Apatite renal stones also commonly are associated with infection and are formed of calcium phosphate. Many of the struvite stones form what are called "staghorn calculi," with large, branching stones located within the renal pelvis. Smaller calcium phosphate stones (typical renal stones) also may become associated with infection, but this is even less common.
Patients with infected renal stones usually do not present with signs of renal colic. The growth of these stones is slow and insidious, and patients may present with chronic complaints. Such symptoms may include fever, hematuria, vague abdominal pain, recurrent UTIs, or urosepsis.83 The exception to this is the infection of a typical calcium phosphate stone, which may present with renal colic. Complications of infected renal stones include recurrent stones, renal failure, sepsis, and death.
Treatment for most infected stones focuses on removal of the stone, but advanced disease may require nephrectomy.83 Studies evaluating conservative treatment vs. surgical removal found a higher rate of kidney failure and mortality in patients managed conservatively.84,85 Although antibiotics are recommended in patients with stones, if significant obstruction is present, the antibiotic will not be filtered by that kidney and will be unable to penetrate to the source of infection.86 For smaller non-obstructing stones, antibiotics and close follow-up for stone passage may be acceptable.
Pregnancy. UTIs in pregnancy are associated with a number of serious side effects generally not encountered in the general population. The most important risk stems from the effect of the infection on the unborn fetus. Multiple studies have shown that untreated UTI increases the rate of prematurity as well as fetal morbidity and mortality. In one study of pregnant women with pyelonephritis, 15% of the newborns weighed 2500 grams or fewer.87 A retrospective study looking at 41,000 matched pregnant women with and without UTIs found an increased rate of fetal death as well as developmental delay later in life.88
Although pregnancy does not predispose a patient to acquire bacteriuria, it is associated with an increased incidence of pyelonephritis.89 The reasons for this most likely are related to the hormonal effects on the ureters and mechanical effects of the uterus.15 Accordingly, most cases of pyelonephritis occur in the second and third trimesters. A small minority (1-2%) of these patients may present in septic shock.84 The physical exam and most laboratory findings are similar to non-pregnant patients with pyelonephritis. One important difference, however, is that a urinalysis may be inaccurate in pregnant patients and should not be relied upon for diagnosing a UTI.90
The treatment of pregnant patients with UTIs differs from that of non-pregnant patients. Due to the consequences of UTI in pregnancy, treatment of asymptomatic bacteriuria is recommended for all patients. A three-day course of a beta-lactam, nitrofurantoin, or a sulfonamide is recommended for both cystitis and asymptomatic bacteriuria.15 Follow-up is critical for these patients, as one-third of them will become reinfected during their pregnancies. Urine cultures also are recommended due to the high levels of beta-lactam resistance (up to 40%) seen in most communities. The length of treatment for both asymptomatic bacteriuria and cystitis is controversial and can range from three to seven days.
The treatment of pyelonephritis is more aggressive in pregnant patients. All pregnant patients with pyelonephritis should be hospitalized for at least 24 hours. Hydration is critical, as many of the patients will be dehydrated from vomiting. Beta-lactams are considered the agents of choice until culture results return. Ceftriaxone is one recommended agent of choice for initial empiric therapy. (See Table 4.)
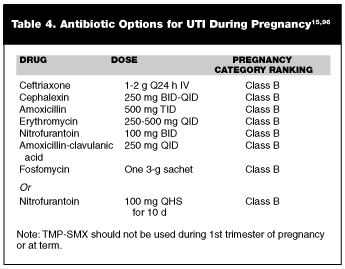
Diabetes. Women with diabetes mellitus are more likely to have UTIs than those without this condition.91 Moreover, diabetic women with asymptomatic bacteriuria also are more likely to progress to pyelonephritis.92 One study reviewing UTIs in diabetics found that the greatest risk factors for developing complicated UTI were the presence of bacteriuria and recent sexual intercourse. Diabetics also are at increased risk for certain complications. About 75% of patients with perinephric abscess and 85-100% of those with emphysematous pyelonephritis have diabetes as a comorbid condition.938
To complicate matters further, diabetes also may be a risk factor for single and multi-drug resistance. One study of multi-drug resistance in the emergency department found that non-catheterized diabetic patients were 2.4 times more likely to have a two-drug resistant urinary pathogen.94 However, increased uropathogen resistance in diabetic patients has not been found by all investigators.95 All diabetic patients with a UTI require a culture and close follow-up.
Summary
UTIs encompass a wide range of disorders, from asymptomatic bacteria to fulminant sepsis. Historically, the treatment of UTI has proven successful with empiric antibiotic therapy. Although the range of pathogens has remained relatively constant over time, the changing spectrum of resistance has altered the treatment landscape dramatically. Antibiotic agents, especially TMP-SMX, which has been a mainstay of therapy, cannot be considered the treatment of choice in areas in which E. coli resistance to TMP-SMX surpasses 10-20%; resistance rates of this magnitude now are reported in all regions of the United States except New England.
New formulations of antimicrobials that historically have been shown to be effective and safe for management of uncomplicated UTI now are available and represent first-line therapy. In this regard, extended release ciprofloxacin has potentially compliance-enhancing properties (once-daily dosing and a well-tolerated side effect profile), an extended release delivery system, and produces clinically effective urine concentrations in patients with uncomplicated UTI. As such, it represents a risk-management upgrade as compared to BID ciprofloxacin and should replace this older formulation as the clinical standard for treatment of uncomplicated UTI when indicated. A well-designed, real world clinical trial supports the shift to the once-daily, extended release formulation.
References
1. O’Donnell JA, Gelone SP. Antibacterial therapy: Fluoroquinolones. Infect Dis Clin North Am 2000;14:489-513, xi.
2. Henry DC, Riffer E, Haverstock DC, et al. Once-daily extended release ciprofloxacin vs. conventional twice-daily ciprofloxacin for the treatment of uncomplicated urinary tract infections. 42nd Interscience Conference on Antimicrobial Agents and Chemotherapy, Sept. 27-30, 2002; San Diego, CA. Abstract L-1800 (oral presentation, E. Riffer, Sept. 30, 2002).
3. Mombelli G, Pezzoli R, Pinoja-Lutz G, et al. Oral vs. intravenous ciprofloxacin in the initial empirical management of severe pyelonephritis or complicated urinary tract infections. A prospective, randomized clinical trial. Arch Intern Med 1999;159:53-58.
4. Wiseman LR, Balfour JA. Ciprofloxacin, a review of its pharmacological profile and therapeutic use in the elderly. Drugs & Aging 1994;4:145-173.
5. Gomolin IH, Siami P, Haverstock D, et al. Efficacy and safety of oral ciprofloxacin suspension vs. TMP/SMX for treatment of community- and nursing home-residing elderly women with acute urinary tract infection. Presented at the 6th International Symposium on New Quinolones; Nov. 15-17, 1998; Denver, Colorado.
6. San Joaquin VH, Stull TL. Antibacterial agents in pediatrics. Infect Dis Clin North Am 2000;14:341-355, viii.
7. Langtry HD, Lamb HM. Levofloxacin: Its use in infections of the respiratory tract, skin, soft tissues and urinary tract. Drugs 1998;56:487-415.
8. Ronald A. The quinolones and renal infection. Drugs 1999;58(suppl 2):96-98.
9. Iravani A, Klimberg I, Briefer C, et al. A trial comparing low-dose, short-course ciprofloxacin and standard 7 day therapy with co-trimoxazole or nitrofurantoin in the treatment of uncomplicated urinary tract infection. J Antimicrob Chemother 1999;43 (suppl A):67-75.
10. Talan DA, Stamm WE, Hooton TM, et al. Comparison of ciprofloxacin (7 days) and trimethoprim-sulfamethoxazole (14 days) for acute uncomplicated pyelonephritis in women. JAMA 2000;283:1583-1590.
11. Koyama Y, Mikami O, Matsuda T, et al. Efficacy of single-dose therapy with levofloxacin for acute cystitis: Comparison to three day therapy. [Japanese] Hinyokika Kiyo 2000;46:49-52.
12. Perry CM, Barman-Balfour JA, Lamb HM. Gatifloxacin. Drugs 1999;58: 683-696.
13. Krcmery S, Naber KG. Ciprofloxacin once vs. twice daily in the treatment of complicated urinary tract infections. German Ciprofloxacin UTI Study Group. Int J Antimicrob Agents 1999;11:133-138.
14. Pimentel FL, Dolgner A, Guimaraes J, et al. Efficacy and safety of norfloxacin 800 mg once-daily vs. norfloxacin 400 mg twice-daily in the treatment of uncomplicated urinary tract infections in women: A double blind, randomized clinical trial. J Chemother 1998;10:122-127.
15. Gilstrap LC 3rd, Ramin SM. Urinary tract infections during pregnancy. Obstet Gynecol Clin North Am 2001;28:581-591.
16. Warren JW, Abrutyn E, Hebel JR, et al. Guidelines for antimicrobial treatment of uncomplicated acute bacterial cystitis and acute pyelonephritis in women. Infectious Diseases Society of America (IDSA). Clin Infect Dis 1999;29:745-758.
17. Pitkajarvi T, Pyykonen ML, Kinnisto K, et al. Pivmecillinam treatment in acute cystitis. Three versus seven days study. Arzneimittelforschung 1990;40: 1156-1158.
18. Spencer RC, Moseley DJ, Greensmith MJ. Nitrofurantoin modified release versus trimethoprim or co-trimoxazole in the treatment of uncomplicated urinary tract infection in general practice. J Antimicrob Chemother 1994; 33(Suppl A):121-129.
19. Kahlmeter G. The ECO*SENS Project: A prospective, multinational, multicentre epidemiological survey of the prevalence and antimicrobial susceptibility of urinary tract pathogens-interim report. J Antimicrob Chemother 2000;46(Suppl A):15-22.
20. Gupta K, Stamm WE. Pathogenesis and management of recurrent urinary tract infections in women. World J Urol 1999;17:415-420.
21. Hooton TM, Stamm WE. Diagnosis and treatment of uncomplicated urinary tract infection. Infect Dis Clin North Am 1997;11:551-581.
22. Gupta K, Scholes D, Stamm WE. Increasing prevalence of antimicrobial resistance among uropathogens causing acute uncomplicated cystitis in women. JAMA 1999;281:736-738.
23. Gupta K, Sahm DF, Mayfield D, et al. Antimicrobial resistance among uropathogens that cause community-acquired urinary tract infections in women: A nationwide analysis. Clin Infect Dis 2001;33:89-94.
24. Le TP, Miller LG. Empirical therapy for uncomplicated urinary tract infections in an era of increasing antimicrobial resistance: A decision and cost analysis. Clin Infect Dis 2001;33:615-621.
25. Hooton TM, Winter C, Tiu F, et al. Randomized comparative trial and cost analysis of 3-day antimicrobial regimens for treatment of acute cystitis in women. JAMA 1995;273:41-45.
26. Stein GE. Fosfomycin tromethamine: Single-dose treatment of acute cystitis. Int J Fertil Womens Med 1999;44:104-109.
27. Stein GE. Comparison of single-dose fosfomycin and a 7-day course of nitrofurantoin in female patients with uncomplicated urinary tract infection. Clin Ther 1999;21:1864-1872.
28. Boerema JB, Willems FT. Fosfomycin trometamol in a single dose versus norfloxacin for seven days in the treatment of uncomplicated urinary infections in general practice. Infection 1990;18(Suppl 2):S80-S88.
29. de Jong Z, Pontonnier F, Plante P. Single-dose fosfomycin trometamol (Monuril) versus multiple-dose norfloxacin: results of a multicenter study in females with uncomplicated lower urinary tract infections. Urol Int 1991; 46:344-348.
30. O’Donnell JA, Gelone SP. Fluoroquinolones. Infect Dis Clin North Am 2000;14:489-513, xi.
31. Shaw KN, Gorelick MH. Urinary tract infection in the pediatric patient. Pediatr Clin North Am 1999;46:1111-1124.
32. Stalam M, Kaye D. Antibiotic agents in the elderly. Infect Dis Clin North Am 2000;14:357-369.
33. Wood CA, Abrutyn E. Urinary tract infection in older adults. Clin Geriatr Med 1998;14:267-283.
34. Safrin S, Siegel D, Black D. Pyelonephritis in adult women: Inpatient vs. outpatient therapy. Am J Med 1988;85:793-798.
35. Lutters M, Herrmann F, Dayer P, et al. Antibiotic utilization in a university geriatric hospital and drug formularies. [French] Schweiz Med Wochenschr 1998;128:268-271.
36. Klimberg IW, Cox CE II, Fowler CL, et al. A controlled trial of levofloxacin and lomefloxacin in the treatment of complicated urinary tract infections. Urology 1998;51:610-615.
37. Delzell JE, Lefevre ML. Urinary tract infection in pregnancy. Am Fam Phys 2000;61:713-721.
38. Anonymous. A meta-analysis of studies on the safety and efficacy of aminoglycosides given either once daily or as divided doses. In: Database of Abstracts of Reviews of Effectiveness, Vol. 1, 2000. NHS Center for Reviews and Dissemination.
39. Anonymous. A meta-analysis of extended-interval dosing vs. multiple daily dosing of aminoglycosides. In: Database of Abstracts of Reviews of Effectiveness, Vol. 1, 2000. NHS Center for Reviews and Dissemination.
40. Anonymous. A meta-analysis of the relative efficacy and toxicity of single daily dosing vs. multiple daily dosing of aminoglycosides. In: Database of Abstracts of Reviews of Effectiveness, Vol. 1, 2000. NHS Center for Reviews and Dissemination.
41. Virk A, Steckelberg JM. Clinical aspects of antimicrobial resistance [symposium on antimicrobial agents-part XVII]. Mayo Clin Proc 2000;75:200-214.
42. Bosker GB. Pharmatecture: Minimizing Medications to Maximize Results: A Systematic Approach to Outcome-Effective Drug Selection. St. Louis, Missouri: Facts and Comparisons; 1999.
43. Talan DA, Stamm WE, Hooton TM, et al. Comparison of ciprofloxacin (7 days) and trimethoprim-sulfamethoxazole (14 days) for acute uncomplicated pyelonephritis pyelonephritis in women: A randomized trial. JAMA 2000;283:1583-1590.
44. Bailey RR, Peddie BA. Treatment of acute urinary tract infection in women. Ann Intern Med 1987;107:430.
45. Bailey RR. Duration of antimicrobial treatment and the use of drug combinations for the treatment of uncomplicated acute pyelonephritis. Infection, 1994;22(Suppl 1):S50-S52.
46. Mombelli G, Pezzoli R, Pinoja-Lutz G, et al. Oral vs intravenous ciprofloxacin in the initial empirical treatment of severe pyelonephritis or complicated urinary tract infections: A prospective randomized clinical trial. Arch Intern Med 1999;159:53-58.
47. Roberts JA. Management of pyelonephritis and upper urinary tract infections. Urol Clin North Am 1999;26:753-763.
48. Engel JD, Schaeffer AJ. Office management of urologic problems: Evaluation of and antimicrobial therapy for recurrent urinary tract infections in women. Urol Clin North Am 1998;25:685-701.
49. Millar LK, Wing DA, Paul RH, et al. Outpatient treatment of pyelonephritis in pregnancy: A randomized controlled trial. Obstet Gynecol 1995;86: 560-564.
50. Wing DA, Hendershott CM, Debuque L, et al. A randomized trial of three antibiotic regimens for the treatment of pyelonephritis in pregnancy. Obstet Gynecol 1998;92:249-253.
51. Wing DA, Hendershott CM, Debuque L, et al. Outpatient treatment of acute pyelonephritis in pregnancy after 24 weeks. Obstet Gynecol 1999;94: 633-638.
52. Garibaldi RA, Mooney BR, Epstein BJ, et al. An evaluation of daily bacteriologic monitoring to identify preventable episodes of catheter-associated urinary tract infection. Infect Control 1982;3:466-470.
53. Warren JW. Catheter-associated urinary tract infections. Infect Dis Clin North Am 1987;1:823-854.
54. Warren JW, Tenney JH, Hoopes JM, et al. A prospective microbiologic study of bacteriuria in patients with chronic indwelling urethral catheters. J Infect Dis 1982;146:719-723.
55. Garibaldi RA, Burke JP, Dickman MC, et al. Factors predisposing to bacteriuria during indwelling urethral catheterization. N Engl J Med 1974;291: 215-219.
56. Hustinx WN, Mintjes-de Groot AJ, Verkooyen RP, et al. Impact of concurrent antimicrobial therapy on catheter-associated urinary tract infection. J Hosp Infect 1991;18:45-56.
57. Stark RP, Maki DG. Bacteriuria in the catheterized patient. What quantitative level of bacteriuria is relevant? N Engl J Med 1984;311:560-564.
58. Warren JW, Anthony WC, Hoopes JM, et al. Cephalexin for susceptible bacteriuria in afebrile, long-term catheterized patients. JAMA 1982;248: 454-458.
59. Alling B, Brandberg A, Seeberg S, et al. Effect of consecutive antibacterial therapy on bacteriuria in hospitalized geriatric patients. Scand J Infect Dis 1975;7:201-207.
60. Nicolle LE. A practical guide to the management of complicated urinary tract infection. Drugs 1997;53:583-592.
61. Warren JW, Damron D, Tenney JH, et al. Fever, bacteremia, and death as complications of bacteriuria in women with long-term urethral catheters. J Infect Dis 1987;155:1151-1158.
62. Warren JW, Muncie HL Jr, Hall-Craggs M. Acute pyelonephritis associated with bacteriuria during long-term catheterization: A prospective clinicopathological study. J Infect Dis 1988;158:1341-1346.
63. Platt R, Polk BF, Murdock B, et al. Mortality associated with nosocomial urinary-tract infection. N Engl J Med 1982;307:637-642.
64. Reid G, Howard L. Effect on uropathogens of prophylaxis for urinary tract infection in spinal cord injured patients: Preliminary study. Spinal Cord 1997;35:605-607.
65. Walsh JJ. Further experience with intermittent catheterisation. Paraplegia 1968;6:74-78.
66. Stover SL, Miller JM 3rd, Nepomuceno CS. Intermittent catheterization in patients previously on indwelling catheter drainage. Arch Phys Med Rehabil 1973;54:25-30.
67. Donovan WH, Kiviat MD, Clowers DE. Intermittent bladder emptying via urethral catheterization or suprapubic cystocath: A comparison study. Arch Phys Med Rehabil 1977;58:291-296.
68. Donovan WH, Stolov WC, Clowers DE, et al. Bacteriuria during intermittent catheterization following spinal cord injury. Arch Phys Med Rehabil 1978; 59:351-357.
69. Montgomerie JZ, Chan E, Gilmore DS, et al. Low mortality among patients with spinal cord injury and bacteremia. Rev Infect Dis 1991;13:867-871.
70. Reid G, Hseihl J, Potter P, et al. Cranberry juice consumption may reduce biofilms on uroepithelial cells: Pilot study in spinal cord injured patients. Spinal Cord 2001;39:26-30.
71. Sandock DS, Gothe BG, Bodner DR. Trimethoprim-sulfamethoxazole prophylaxis against urinary tract infection in the chronic spinal cord injury patient. Paraplegia 1995;33:156-160.
72. The prevention and management of urinary tract infections among people with spinal cord injuries. National Institute on Disability and Rehabilitation Research Consensus Statement. Jan. 27-29, 1992. J Am Paraplegia Soc 1992;15:194-204.
73. Lipsky BA. Urinary tract infections in men. Epidemiology, pathophysiology, diagnosis, and treatment. Ann Intern Med 1989;110:138-150.
74. Barnes RC, Daifuku R, Roddy RE, et al. Urinary-tract infection in sexually active homosexual men. Lancet 1986;1:171-173.
75. Spach DH, Stapleton AE, Stamm WE. Lack of circumcision increases the risk of urinary tract infection in young men. JAMA 1992;267:679-681.
76. Krieger JN, Ross SO, Simonsen JM. Urinary tract infections in healthy university men. J Urol 1993;149:1046-1048.
77. Ulleryd P, Lincoln K, Scheutz F, et al. Virulence characteristics of Escherichia coli in relation to host response in men with symptomatic urinary tract infection. Clin Infect Dis 1994;18:579-584.
78. Lipsky BA. Managing urinary tract infections in men. Hosp Pract (Off Ed). 2000;35:53-59; discussion 59-60, 144.
79. Nicolle LE, Bjornson J, Harding GK, et al. Bacteriuria in elderly institutionalized men. N Engl J Med 1983;309:1420-1425.
80. Mims AD, Norman DC, Yamamura RH, et al. Clinically inapparent (asymptomatic) bacteriuria in ambulatory elderly men: Epidemiological, clinical, and microbiological findings. J Am Geriatr Soc 1990;38:1209-1214.
81. Harwood-nuss A, Etheredge W, McKenna I. Urological Emergencies. In: Emergency Medicine Concepts and Clinical Practice. Rosen P, Barkin R, Ling LJ, eds. St. Louis: Mosby; 1998;2227-2261.
82. Lipsky BA. Prostatitis and urinary tract infection in men: What’s new, what’s true? Am J Med 1999;106:327-334.
83. Gleeson MJ, Griffith DP. Struvite calculi. Br J Urol 1993;71:503-511.
84. Rous SN, Turner WR. Retrospective study of 95 patients with staghorn calculus disease. J Urol 1977;118:902-904.
85. Koga S, Arakaki Y, Matsuoka M, et al. Staghorn calculi—long-term results of management. Br J Urol 1991;68:122-124.
86. Manthey DE, Teichman J. Nephrolithiasis. Emerg Med Clin North Am 2001;19:633-654, viii.
87. Gilstrap LC, Leveno KJ, Cunningham FG, et al. Renal infection and pregnancy outcome. Am J Obstet Gynecol 1981;141:709-716.
88. McDermott S, Daguise V, Mann H, et al. Perinatal risk for mortality and mental retardation associated with maternal urinary-tract infections. J Fam Pract 2001;50:433-437.
89. Gilstrap LC 3rd, Cunningham FG, Whalley PJ. Acute pyelonephritis in pregnancy: An anterospective study. Obstet Gynecol 1981; 57:409-413.
90. Tincello DG, Richmond DH. Evaluation of reagent strips in detecting asymptomatic bacteriuria in early pregnancy: Prospective case series. BMJ 1998;316:435-437.
91. Geerlings SE, Stolk RP, Camps MJ, et al. Consequences of asymptomatic bacteriuria in women with diabetes mellitus. Arch Intern Med 2001;161: 1421-1427.
92. Geerlings SE, Stolk RP, Camps MJ, et al. Asymptomatic bacteriuria may be considered a complication in women with diabetes. Diabetes Mellitus Women Asymptomatic Bacteriuria Utrecht Study Group. Diabetes Care 2000;23:744-749.
93. Kawashima A, Sandler CM, Goldman SM. Imaging in acute renal infection. BJU Int 2000;86(Suppl 1):70-79.
94. Wright SW, Wrenn KD, Haynes M, et al. Prevalence and risk factors for multidrug resistant uropathogens in ED patients. Am J Emerg Med 2000;18: 143-146.
95. Wright SW, Wrenn KD, Haynes ML. Trimethoprim-sulfamethoxazole resistance among urinary coliform isolates. J Gen Intern Med 1999;14: 606-609.
96. Delzell JE Jr., Lefevre ML. Urinary tract infections during pregnancy. Am Fam Physician 2000;61:713-721.
This issue is the second and final part in our series on urinary tract infection. Part I of the series examined epidemiology, emerging resistance patterns, and patient-specific treatment strategies. In part II, we will cover antibiotic selection, new treatment options, and special considerations.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
