Beat the Heat: Recognizing and Managing Pediatric Heat-Related Illness
Author: S. Margaret Paik, MD, FAAP, Assistant Professor of Pediatrics, The University of Chicago Children’s Hospital, Chicago, IL.
Peer Reviewer: John P. Santamaria, MD, FAAP, FACEP, Medical Director, After Hours Pediatrics; Associate Clinical Professor of Pediatrics, University of South Florida School of Medicine, Tampa.
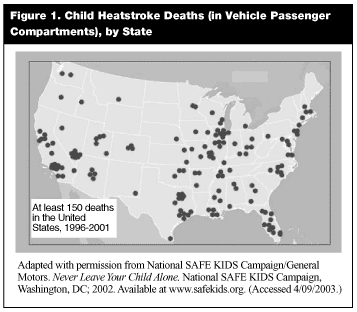
As the seasons change and summer approaches in the United States, the risk of heat-related illness for pediatric patients climbs. Since 1996, at least 150 children have died as a result of being trapped in hot, parked vehicles.1 Contrary to what would be expected, these deaths occurred throughout all regions of the United States, making it important for all emergency medicine physicians to be familiar with the resuscitation of a child with a heat-related illness. (See Figure 1.) Children are particularly vulnerable to heat, whether trapped in a parked vehicle or participating in athletic events, and early recognition and aggressive resuscitation can significantly impact the child’s outcome. This article provides an overview of heat-related illnesses in children and prevention and management strategies to facilitate care.—The Editor
Scope of the Problem
Excessive heat exposure caused more than 8000 deaths in the United States between 1979 and 1999, with fewer than half being due to weather conditions. Of the total, 142 deaths occurred in children younger than 4 years of age.2 In Chicago from July 11-27, 1995, 465 deaths were certified by the Cook Country Medical Examiner’s Office as heat-related.3 A second heat wave in Chicago, during the summer of 1999, resulted in at least 80 deaths.4 Despite widespread media coverage of the heat waves and their related morbidity and mortality,5,6 and despite efforts to educate the public, children still are dying from excessive heat exposure. Among fatal injuries in children younger than 14 years who were left unattended in or around motor vehicles, more than one-third were the result of children being left in motor vehicles in hot weather.7
Although annual warnings are issued, parents—particularly young parents—fail to recognize the dangers of leaving children unattended in parked cars. A poll by the national SAFE Kids campaign and General Motors found that as many as 1 in 5 young parents believe it is acceptable to leave their children alone in parked cars.
Even well-conditioned athletes are at risk. There have been numerous reports of athletes dying from heatstroke in their efforts to achieve superior advantage in competition.8,9 Exertional heat stroke also has been noted in individuals exercising in a cool-to-moderate climate.10
Individuals most at risk for heat-related illness include the elderly, people with mental illness and chronic diseases, and alcoholics.10 Additionally, certain medications also will contribute to the risk of developing heat-related illness.12
Mechanisms of Thermoregulation and Heat Loss
Core body temperature is in a constant state of equilibrium between heat production and heat dispersion. Our body temperatures are closely regulated to cycle through a diurnal rhythm, starting at about 36°C in the early morning and increasing throughout the day to reach about 37.5°C by the late afternoon.13 Heat is produced as an end product of energy metabolism, especially from active muscle.14 In addition, heat is gained from the environment when the ambient temperature exceeds the body temperature.15
Loss of body heat occurs in one of four ways—convection, conduction, radiation, and evaporation.16,17
Convection allows heat to be transferred from a surface to a gas or fluid via the circulating air or water molecules. The overall effectiveness of heat loss by this method is dependent on how rapidly the air or water near the body exchanges after it has become warmed.
Conduction is the direct transfer of heat between surfaces, either through a liquid, solid, or gas. The rate of body heat loss is dependent on the temperature gradient created between the skin and the surrounding contacted surfaces.
Radiation is the transfer of heat between objects via electromagnetic waves. Since our bodies usually are warmer than the surrounding environment, radiant heat energy is lost from our bodies through the air to the solid, cooler objects nearby. Radiation is responsible for up to 65% of heat loss when resting in a temperate climate, but also is a major cause of heat gain when an individual lies directly in the hot sun.
Evaporation is the major physiologic mechanism used to prevent overheating. Water, vaporized from the lungs and skin, transfers the heat to the environment. The body loses 580 kcal of heat energy from every liter of water evaporated.
Physiology
The preoptic nucleus of the anterior hypothalamus regulates body temperature through a series of complex mechanisms.13,16 These mechanisms do not allow the heat to be turned down or turned off, as with a thermostat, but instead are activated to defend against heat loss or heat gain. The free nerve ending thermal receptors in the skin quickly sense changes in temperature and send this information to the hypothalamus. The temperature of the blood circulating through the anterior hypothalamus is the direct way by which the thermoregulatory center is stimulated.14 When the core body temperature increases, the thermoregulatory center, via the autonomic nervous system, generates cutaneous vasodilation, causing heat dissipation through convection. There also is an increase in the amount and rate of sweating, resulting in heat loss as the water evaporates from the skin surface.13,14
The thermal control center continuously compensates for any increases in heat production to regulate the core body temperature.15 Hyperthermia is a rise in body temperature when heat production exceeds heat loss. This is in contrast to fever, which is a rise in the core body temperature in response to an increase in the hypothalamic set point from circulating pyrogenic cytokines. Hyperthermia occurs when there is a failure of the normal thermoregulatory system due to extreme heat production (e.g., exertional heat stroke, thyrotoxicosis, or malignant hyperthermia), extremes in the environmental heat (as in a heat wave), or impaired heat loss (e.g., classic heat stroke, dehydration, or clothing). Hyperthermia also will occur when there is loss of full hypothalamic function, as seen in individuals with a history of severe head injury or cerebrovascular accidents.13,15
Heat Gain from the Environment
High Ambient Temperatures. The effectiveness of heat dissipation by conduction, convection, and radiation is reduced greatly as the ambient temperature increases. Heat is gained when the ambient temperature begins to exceed the body temperature. At this point, water evaporation from the lungs and sweat evaporation become the only avenues for heat loss.14
High Humidity. Sweating is initiated as the core body temperature rises. The amount of sweat evaporated depends on the ambient temperature and relative humidity, as well as the amount of skin exposed and the air currents surrounding the body.14 Under conditions of low humidity, 1.7 mL of sweat will expend 1 kcal of heat energy during evaporation.16 In conditions of high humidity, sweat evaporation is reduced drastically. Water is lost as sweat beads leave the skin surfaces (either by rolling off or being wiped off), but heat is not lost. This process eventually leads to dehydration and hyperthermia.14
Heat Waves. There are numerous case reports of increased morbidity and mortality during heat waves (defined as three or more consecutive days of air temperatures of 90°F or 32.2°C or greater).2,3,18-20 In these reports several risk factors are described. These include advanced age, mental illness, chronic conditions (e.g., cardiovascular or respiratory diseases), alcoholism, and the use of certain medications (i.e., neuroleptic agents). During the 1995 heat wave in Chicago, those at greatest risk of dying were individuals living in social isolation and those with a lack of access to air conditioning.4 The most common cause of death in children left unattended in and around motor vehicles was excessive heat exposure, as reported by the Centers for Disease Control and Prevention.7
Increased Heat Production
Exercise. Metabolic rate can increase 20-25 times above the resting level during periods of continual vigorous exercise. In theory, this would cause the core body temperature to rise 1°C every 5-7 minutes.14 In response, vasodilation, tachycardia, and increased cardiac output allow for the warm blood to be shunted to the skin surface, where the heat is lost.17
The water and electrolyte content in sweat will change as an individual exercises. Exercising in hot weather will cause release of aldosterone, increasing reabsorption of sodium from the renal tubules with a reduction in sweat osmolality. Release of vasopressin from the pituitary gland during heat stress will increase water reabsorption from the tubules, as well.13
Medications. Certain classes of medication can increase heat production. These include some neuroleptic agents and certain anesthetic agents.12,15 Drugs of abuse, such as hallucinogens (phencyclidine hydrochloride-PCP and lysergic acid diethylamide-LSD) and stimulants (amphetamines and cocaine), increase the metabolic state leading to tachycardia, hypertension, agitation, and increased muscle activity.
Factors Influencing Heat Loss
Body Fat. Excess body fat has a negative effect on heat loss by several mechanisms. Fat, acting as an insulator, impedes heat conduction. There also are increased metabolic demands that accompany excess body fat. Death from heatstroke occurs 3.5 times more often in obese individuals than in those with normal body mass.14
Dehydration. Dehydration, regardless of the etiology, will cause a reduction in the plasma volume. With progressive losses, there will be a reduction of cardiac output, leading to an increase in the systemic vascular resistance. Blood flow to the skin is thereby reduced, decreasing the amount of warm blood normally shunted to the skin surfaces. The rate of sweating also decreases in the dehydrated state.14,23
Age. Both extremes of the age spectrum are at risk for heat-related illness. The elderly are more likely to have chronic medical conditions, such as cardiovascular disease and diabetes, which can impair their response to heat stress. Persons chronically bedridden also are at risk.
Children have a greater risk of heat-related illness for both physiological and psychosocial reasons. The younger child has a greater surface area-to-body mass ratio, leading to greater heat gain on hot days (as well as greater heat loss on cold days). During exercise, as well as with walking at a steady pace, a child produces more metabolic heat per mass unit than an adult does. Additionally, children do not sweat as effectively as adults under the same climatic conditions.21 They have an immature sweating mechanism and fewer sweat glands.24 There also are differences in the sweat composition between children and adults, with a higher concentration of sodium and chloride in the sweat produced by children.21 These differences probably last through puberty or later.14,22 It is obvious that young children are unable to control their environment and sometimes are left in compromising situations that can lead to heatstroke.7,18,20 Children often do not drink enough during exercising to compensate for fluid losses, leading to dehydration and increased body temperature, thereby increasing the risk of heat-related illness.21 It has been shown that individuals often do not voluntarily drink enough fluid to replace their losses (voluntary dehydration) when working in the heat.15 Children voluntarily would replace only 50% of their fluid deficit if not forced to increase their fluid intake.25 Overall, thirst is a poor gauge of hydration status.
Medications. Use of certain medications will contribute to the risk of heat-related illness. Drugs with anticholinergic properties, such as antihistamines, atropine, neuroleptic agents, antispasmodics, tricyclic antidepressants, and those used in the treatment of Parkinson’s disease, can inhibit sweating and induce tachycardia, thereby reducing heat elimination and increasing heat production, respectively.15,16,26
Sympathomimetics drugs, such as amphetamines, cocaine, and ephedrine/pseudoephrine (found in decongestants) will increase the core body temperature either by peripheral vasoconstriction, thus restricting heat loss or increasing heat production due to amplified muscle activity from agitation and/or seizure activity.26
Beta-blockers and diuretics inhibit the normal cardiovascular response to heat stress. These medications, usually taken by the elderly for cardiovascular disease, add to risk of heat illness in this population.15 Some athletes induce weight loss by abusing diuretics and laxatives to reach a certain weight class, hoping to gain a competitive advantage.14
Acclimatization. Acclimatization is the physiologic adaptation that occurs when a normal person works or exercises repeatedly in a hot environment, thus allowing a person to tolerate a greater level of heat stress. Most adults can achieve this adaptation within 7- 10 days.15,17 The rate of acclimatization is slower in children and may require up to two weeks.24,27 The American Academy of Pediatrics recommends acclimatization be facilitated through 8-10 sessions of 30-45 minutes in the new environment.21
The physiologic changes that occur during acclimatization are as follows:14,17
• There is a more effective and efficient cardiac output with more even distribution of the circulation to the skin and muscles. Blood pressure is maintained more evenly during exercise and greater quantities of blood are shunted to the skin surface. Plasma volume is increased; and
• There is increased sweating capacity and concomitant production of more dilute sweat due to the activation of the renin-angiotension-aldosterone system. The sodium concentration in the sweat can be reduced up to 50%.23 Threshold for sweating is lowered, and the sweat is distributed more evenly on the skin surface, thus maximizing evaporative heat loss.
Children, with their smaller respiratory and circulatory systems, are less efficient in the process of acclimatization.25
Clothing. Clothing is a barrier to heat loss. Dry clothing will reduce heat exchange more than wet clothing. Dark-colored clothing will increase the amount of heat gained by radiation; light-colored clothing tends to reflect heat rays. Loosely fitted clothing allows for convection air currents to pass between the skin and the environment.14
Pre-existing Medical Conditions. Several conditions increase the risk of heat-related illness. Patients with cystic fibrosis will underestimate their fluid needs during exercise.28,29 Children with concurrent febrile or gastrointestinal illnesses, diabetes mellitus, and diabetes insipidus are prone to excessive fluid losses. Very young children and those with mental retardation may not understand the necessity of drinking more fluids during heat exposure.21
Minor Heat-Related Illnesses
Heat Rash (Prickly Heat, Miliaria Rubra). During sweating, sweat ducts become obstructed with macerated cellular material as the sweat duct ruptures. An acute inflammatory response results in pruritic, 2-4 mm papules and papulovesicles with surrounding erythema. Rupture of an obstructed duct produces a vesicle deeper within the dermis and usually is not pruritic. This profunda stage may persist for weeks. Secondary infection with Staphylococcus aureus produces pustules. Flexural regions, especially in infants during hot, humid weather or in areas of occlusive dressing, are most frequently affected.30,31
Treatment consists of allowing the affected surface to become cool and dry and to minimize further sweating in that area. Some authors recommend the use of chlorhexidine lotion or cream, either with or without concomitant usage of 1% topical salicylic acid. Antibiotics are used if there is concern of a secondary bacterial infection.15,30 Talcum baby powder should be avoided.
Heat Edema. Heat edema is swelling in the dependent areas of nonacclimatized individuals, especially the elderly. Heat stress causes peripheral vasodilation and orthostatic pooling of the blood, resulting in increased interstitial fluid from the increased hydrostatic pressure. This entity usually is self-limited without systemic involvement and resolves in a few days, after acclimatization. Elevation of the legs may help.12,15,30
Heat Cramps. Heat cramps are painful, involuntary muscle spasms, usually occurring in large muscle groups (i.e., arms, legs, or abdomen) fatigued by intense physical activity. This usually is seen in athletes, coal miners, construction workers, and roofers following strenuous physical activity.12,16,30 The cramps are thought to be due to a sodium deficit following the use of large amounts of hypotonic fluids to replace fluids lost from copious sweating. Hyponatremia and hypochloremia commonly are seen.15 There is a lack of systemic symptoms, and the body temperature may or may not increase.14,30
Mild cases are treated with oral replacement of sodium using either a commercially produced electrolyte solution or 1 teaspoon of table salt mixed in 500 cc of water. Intravenous normal saline is used in more severe cases.12,15
Heat Tetany. Heat tetany occasionally is confused with heat cramps. Heat tetany is characterized by the presence of carpopedal spasms with paresthesias in the perioral region and distal extremities.15,30
Heat Syncope. Heat syncope is seen in individuals who either have been standing for a prolonged period of time or rise suddenly from a sitting or recumbent position in a hot environment. Cerebral blood flow is reduced as a result of reduced venous return and cardiac output from peripheral blood pooling. Orthostatic hypotension also is seen.
Recovery occurs once the individual is supine. Treatment consists of replacing any fluid deficit. Heat syncope can be prevented by avoiding protracted periods of standing in hot weather and flexing the leg often to help increase venous return. Individuals also should sit or lie down at the first signs of weakness, dizziness, or lightheadedness.12,15,30
Heat Exhaustion. Heat exhaustion or heat prostration is a result of volume depletion, as much as 6-10%,10 during heat stress. Signs and symptoms are listed in Table 1.

Heat exhaustion and heat stroke are part of the continuum in the spectrum of heat-related illness and have overlapping symptomatology. In heat exhaustion, there is a lack of major central nervous system (CNS) decompensation (e.g., coma or seizures), and usually an absence of severe hyperthermia (greater than 40-40.5°C), differentiating it from heat stroke. Measurement of hepatic transaminases may be useful if there still is uncertainty; there is elevation to the several thousands in heat exhaustion. Elevation to the tens of thousands occurs in heat stroke patients after 24 hours.15,30 Although core body temperatures are usually above 38°C, expeditious treatment of heat exhaustion has no known harmful, chronic, or long-term side effects.10
Heat exhaustion usually is described as either water depletion or salt depletion; typically there is overlap between the two.32 Water depletion heat exhaustion is a result of inadequate fluid replacement when exposed to heat stress. This tends to occur in the elderly, with their predisposing conditions (i.e., cardiovascular disease), and in individuals without free access to water (e.g., infants). This condition is also more likely to affect laborers and military personnel. Voluntary dehydration is seen in individuals working in the heat and is a contributing factor. Untreated water depletion heat exhaustion may progress to heat stroke.12,15,16,30
Salt depletion heat exhaustion occurs in persons who maintain their volume status with water but do not replace their sodium losses adequately. Laboratory studies show hyponatremia, hypochloremia, and low urinary sodium and chloride concentrations in these individuals.30
Victims of heat exhaustion recovery quickly following fluid administration. Persons with normal vital signs and who are not vomiting can be treated with oral fluid and salt replacement, with recovery in a cool location.12,30
More serious cases require treatment with intravenous fluids. The type of fluid used is based on the estimated amount of dehydration and electrolyte status. Normal saline should be used if hypotension is present. If the patient has hypernatremia, hydration must be accomplished slowly to prevent cerebral edema.15,16
Major Heat-Related Illness
Heat Stroke. Definition. Heat stroke is the most severe heat-related illness, characterized by an elevation of the core body temperature above 40-40.5°C (rectal), coupled with multisystem organ and tissue damage, particularly CNS dysfunction.12,13,16,17,30,33 Acute neurological impairment may include stupor, delirium, confusion, coma, psychotic behavior, and seizures. Hypotension, tachycardia, and tachypnea can be seen initially. Untreated heat stroke progresses to hepatic, renal, cardiac, and pulmonary end-organ damage. Even with aggressive management, mortality of heat stoke victims may be as high as 10%.13,16
Pathophysiology. Research has shown that heat stroke is the end result of an exaggerated acute phase response to heat stress in the setting of thermoregulatory collapse. There is a complex interaction between circulating cytokines, cytokine receptors, and chemokines during heat stress. Heat stroke most likely is due to endothelial cell activation/injury, with release of endothelial vasoactive factors.17,25,34-36 Heat-shock proteins are produced by cells in response to a heat stress, allowing transient tolerance to this situation. Animal studies show that upregulation of these proteins, in particular heat shock protein 70, protects against end-organ injury.37 Antibodies to this protein were more frequently found in patients with severe heatstroke.38
Types of Heat Stroke. The traditional dogma is that persons with heat stroke will present with hyperthermia, significant CNS dysfunction, and hot, dry skin with a lack of sweating. This is not always the case, and these criteria should not used to either rule in or rule out the diagnosis. There have been cases of heat stroke in which sweating was present and rectal temperatures of 41.5-42.4°C were noted.30 Heat stroke usually is subdivided into either classic or exertional heat stroke, based on differing presentations and sequelae. (See Table 2.)
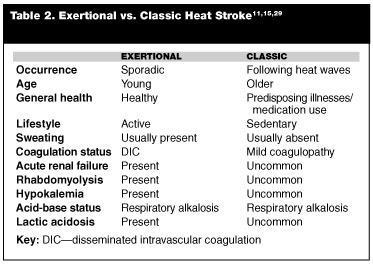
Classic heat stroke usually occurs during the summer months, especially during two- to four-day periods of prolonged high ambient temperatures and humidity.39 It primarily affects the elderly and those with chronic and/or debilitating diseases. Using certain types of medications, as discussed previously, also adds to the risk. Other high-risk individuals are the poor, those living in inadequately ventilated housing, and those with lack of free access to water. The onset is slow and insidious, allowing time for fluid and electrolyte abnormalities to occur. It is noted that sweating is totally absent in most victims of classic heat stroke.15,30
Victims of exertional heat stroke tend to be younger and healthy. They often are athletes, military personnel, or laborers exposed to heat stress. These individuals may be wearing heavy clothing, be dehydrated prior to their exposure to the heat, engaged in strenuous exercise, and/or have a lack of heat acclimatization.10,13,15 In general, these individuals have more rapid elevation of the core body temperature.39
Clinical Manifestations of Heat Stroke
Cardiovascular. Sinus tachycardia commonly is noted in both types of heat stroke, and is caused by peripheral vasodilation and compounded by hypovolemia. A high pulse pressure also is noted. Hypotension is seen as a late finding, as high output failure occurs in those in a hyperdynamic state. Patients also may present in a hypodynamic state; this is dependent on the individual’s volume status and the amount of cardiovascular injury from the heat. There is evidence of myocardial infarction in some patients. Findings reported at autopsy include right heart dilatation, edema, necrotic myocardial fibers, and pericardial effusion.13,15,30
Central Nervous System. CNS dysfunction with altered sensorium is a hallmark of heat stroke. Initially patients may be confused or irritable, but with continued heat exposure, stupor, coma, and delirium may be seen. Patients also may present with muscle rigidity or tremors. Seizures can be seen as the patients are cooled rapidly in ice water immersion. Common cerebellar findings include ataxia and dysarthria. There is clear cerebrospinal fluid with normal pressures if a lumbar puncture is performed. Occasionally, the fluid will show a pleiocytosis and some protein level elevation.5,15,30,39
Hematologic. Physical manifestations of abnormal hemostasis include ecchymosis, purpura, conjunctival hemorrhages, hemoptysis, melena, hematuria, and myocardial and CNS hemorrhage.12,15 Initial coagulation abnormalities can progress to disseminated intravascular coagulation (DIC), with low platelet, Factor V, and Factor VIII levels. Although coagulopathies may be present initially, they are more common on the second or third day. The white blood cell count can be elevated to as much as 30,000-40,000/mL. The pathogenesis of the coagulopathy is multifactorial and includes hepatic damage, activation of clotting factors, and endothelial damage. Presence of coagulation abnormalities indicates a poor prognosis.30
Hepatic. Hepatic injury is one of the most consistent findings in heat stroke. There is marked elevation of the serum transaminases, with jaundice noted 24-72 hours later. Hypoglycemia is common in patients with exertional heat stroke. Survivors usually do not have permanent hepatic impairment.15,30
Renal. Acute renal failure can be seen in 25-30% of exertional heat stroke victims and in 5% of classic heat stroke patients. DIC, hypotension, and myoglobinuria may precipitate acute tubular necrosis. Urinalysis can show proteinuria, granular, and red blood cell casts. Kidneys studied at autopsy show numerous petechial hemorrhages.15,30
Electrolytes and Acid-Base Status. Hypernatremia is seen in patients who are dehydrated whereas hyponatremia is seen in patients who have had excessive sodium losses in sweat or have used hypotonic solutions to replenish their fluid losses. Hypo-kalemia is common and is associate with a total body potassium deficit. Hypocalcemia, hypophosphatemia, and hypomagnesemia also can be found. Initially, respiratory alkalosis is seen due to hyperventilation. Later findings in exertional heat stroke patients include increasing levels of lactic acid, resulting in severe metabolic acidosis, and hyperkalemia.13,15,16,25
Musculoskeletal. Rhabdomyolysis develops as a consequence of rigid and contracted muscles. There is elevation of the muscle enzymes (CPK) and myoglobinuria is present.13,15
Pulmonary. Most patients will present with hyperventilation. The degree of hyperventilation can be severe enough to result in tetany. Pulmonary edema becomes evident as circulatory failure progresses, due to cardiac dysfunction and DIC. Noncardiogenic pulmonary edema with DIC is severe and carries a high mortality. Hemoptysis and pulmonary infarct also can be seen.15,33,40 Adult respiratory distress syndrome (ARDS) also is a complication of heat stroke and can be seen in up to 25% of patients. Recent findings suggest that ARDS may be due to DIC with the ensuing activation of complement, and not necessarily due to the aspiration of gastrointestinal contents, as previously was thought.27,33,41
Treatment of Heat Stroke
Early recognition of heat stroke reduces morbidity and mortality.15 The mainstay of treatment is the reduction of the core body temperature. Following assessment of airway competency competency and effectiveness of breathing, the patient should be moved to a cool, shady area until transportation to a hospital arrives. The clothing should be removed and ice packs or a cooling blanket should be applied to the axillae, groin, and neck regions. If possible, cover the patient with water. Fanning will cause evaporative heat loss. Obtain intravenous access and begin rehydration if circumstances allow.
Upon the patient’s arrival to the ED, the airway status should be reassessed and supplemental oxygen administered. In patients with severe altered mental status, elective intubation with mechanical ventilatory support needs to be considered early to protect against aspiration and to support the increased oxygen needs in this hypermetabolic state. Intravenous access is essential. Blood chemistries and other laboratories should be obtained. Continuous cardiovascular monitoring is also crucial. Rectal temperature should be measured with a thermometer able to record temperatures above 41°C. It should be noted that the initial temperature reading in the ED may not be reflective of the peak body temperature, as cooling may have begun prior to arrival.10,39,42
Cooling methods should be used only until the patient’s core body temperature is 39°C, to avoid hypothermia. Continuous monitoring of the vital signs are essential during this process. Shivering may occur during this stage and should be aggressively treated to avert the increased heat production and oxygen consumption caused by shivering. Diazepam (0.1-0.3 mg/kg/dose IV) can be used to inhibit shivering. Chlopromazine also has been used.12,15,25,42
Several methods have been used to rapidly cool the patient. External methods of cooling include evaporative cooling methods and ice water immersion. Although ice water immersion is effective and has been shown to decrease the core body temperature by 0.13°C/min, this technique is cumbersome and makes monitoring of the patient’s vital signs and core body temperature difficult. Ice water immersion can cause peripheral vasoconstriction, resulting in shunting of blood away from the skin, and can induce shivering. This approach no longer is the preferred method for cooling by some authors. Cold water immersion results in similar rate of cooling, but has been found to have fewer disadvantages than ice water immersion. In both cases, efficient monitoring and resuscitation of the patient may be challenging.15,43 Several evaporative cooling methods have been developed. Cool or room temperature water is sprayed over the patient, with simultaneous fanning of the patient. Others have placed a patient on a suspended, netted surface, allowing for atomized water (15°C) to be sprayed from above and below the patient. Air warmed to 45-48°C then is blown over the patient.15,16,42
Internal cooling methods include cold-water irrigation of the stomach, rectum, and peritoneal cavity, as well as cardiopulmonary bypass. These methods should be considered when external cooling measures have been ineffective.12
Sponge bathing with alcohol should be avoided. Large amounts of absorbed alcohol will result in alcohol toxicity. There is no role for the use of antipyretics in the treatment of heat stroke. Any coagulopathy can be made worse with the use of nonsteroidal anti-inflammatory drugs, and acetaminophen may potentiate liver dysfunction.15,30,42 Presently, there is no role for the use of steroids in the management of heat stroke patients.15,30
Meticulous supportive care with stabilization of the basic ABCs (airway, breathing, and circulation) is critical. Careful hemodynamic monitoring is essential during fluid resuscitation so as to avoid cerebral and pulmonary edema. Electrolytes should be corrected as needed and inotropic medications may be indicated after intravascular volume has been replaced adequately. A minimum urine output of 0.5 mL/kg/hr should be achieved. Fresh frozen plasma and platelets transfusions may be indicated, depending on the amount of coagulopathy present.13,15,42
Prognosis. The prognosis of a heat stroke patient is dependent on several variables, including the patient’s general state of health and the ability to maintain sufficient cardiac output as the circulatory and metabolic needs increase.42 (See Table 3.) One study found that a delay in diagnosis and cooling worsened the patient’s prognosis, even if the initial laboratory studies were normal. Rapid cooling within one hour results in a better prognosis, and decreasing the body temperature to less than 38.9°C within 30 minutes improved the overall survival rate.44 Other indicators of poor outcome include coma that persists after cooling, and elevation of aspartate aminotransferase (AST) to greater than 1000 IU/L.

Prevention
Heat Index. Prevention of heat-related illness requires the recognition of the high-risk situations with respect to the environment. The National Weather Service provides information on the heat index, a measurement of how hot it feels when the relative humidity and effects of the air temperature are combined. A heat index between 105-129°F makes heat cramps and heat exhaustion likely, and heat stroke possible. A heat index of 130°F or higher increases the likelihood of heat stroke. During high-risk conditions, the elderly, chronically confined, and those talking certain medications need to avoid the heat and maintain a good hydration state.33 Individuals should wear light-colored, loose-fitting clothing when going outdoors. Staying indoors in an air-conditioned environment is the best preventative measure.
Wet Bulb-Globe Temperature. The United States military developed the wet bulb-globe temperature (WB-GT) using the measurements of the ambient temperature, relative humidity, and radiant heat in the following formula:14 WB-GT = 0.1(DBT) + 0.7(WBT) + 0.2(GT)
DBT (dry bulb temperature) is the dry-bulb temperature, or air temperature measured in the shade by a mercury thermometer. WBT (wet bulb temperature) is the temperature measured by a mercury thermometer with a surrounding wet wick exposed to air movements in the direct sunlight. The device notes the relative humidity. GT (globe temperature) is measured by a thermometer with a black metal sphere surrounding the bulb in direct sunlight. The black sphere absorbs radiant energy.
The wet-bulb temperature, which factors in the amount humidity, is 70% of the index. See Table 4 for the American College of Sports Medicine’s recommendations for WB-GT during continuous activities such as running and cycling.10,14
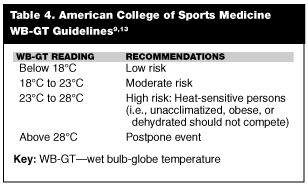
Acclimatization. The acclimatization process should be gradual. Generally, young children will take longer to complete this process than adolescents, adults, or well-conditioned athletes. Acclimatization may take up two weeks, as previously discussed.24,25,27 Adults in general require 4-7 sessions of 1-4 hours in the heat to acclimate. This process can be facilitated by the continual replacement of wet clothing with dry clothing.

Hydration. Adequate hydration is of paramount importance. It is recommended that children weighing up to 40 kg should ingest 150 mL (5 ounces) and adolescents weighing up to 60 kg should drink 250 mL (9 ounces) of either cold tap water or a flavored salt beverage every 20 minutes while exercising.21 This requirement should be enforced even if the child is not thirsty, as thirst is not a good indicator of hydration status. For older individuals it is recommended that up to 448 mL (16 ounces) of fluid be drunk before exercising, and another 224 mL (8 ounces) be taken every 20 minutes while exercising. A flavored carbohydrate-electrolyte solution elicited the largest volume of voluntary total consumption when compared to flavored drink or plain water.14 The goal is to avoid feeling thirsty during heat stress.
Entrapment in Cars
Despite annual warnings by both General Motors and SAFE Kids, many children—about 30 in 2001—die from hyperthermia secondary to prolonged exposure to heat in unattended cars. Between 1996 and 2001, the majority of deaths (90%) occurred in children younger than 3 years of age. (See Figure 2.) The deaths are distributed throughout the United States, with a broad regional distribution. (See Figure 1.) Many parents fail to recognize the danger of leaving a child unattended in a parked car. One survey conducted by General Motors and the national SAFE Kids Campaign found that although more adults are aware of the potential danger associated with leaving a child unattended in a parked car, one in five young parents still finds it an acceptable behavior. Also, parents fail to recognize the danger of leaving an unlocked vehicle in direct sunlight, where a child might inadvertently trap himself. Currently, one in five parents never locks his or her vehicle, results similar to those from a survey conducted in 1999.
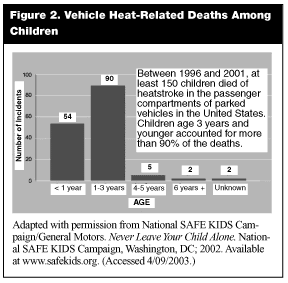
Parents and physicians frequently are unaware of the rate of air temperature increase in the passenger compartment of a car. (See Figure 3.) For example, a car left outside in 85°F temperature will reach an interior temperature of almost 120°F within 30 minutes. Even in relatively mild temperatures, a closed vehicle can pose serious risk to a child left strapped in a car seat in an unattended car. As previously mentioned, children younger than 3 years of age are particularly vulnerable to heat-related injury and subsequently have the highest rates of heat-related illness. Infants may be particularly vulnerable when positioned in a car seat (with cushioned seats) and fully clothed, which decreases their evaporative surfaces.
Figure 3.
Rate of Air Temperature Increase
in Vehicle
Passenger Compartment
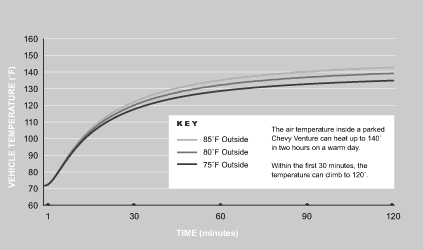
Adapted with permission from National SAFE KIDS
Campaign/General Motors. Never Leave Your Child Alone.
National SAFE KIDS Campaign, Washington, DC; 2002.
Available at
www.safekids.org. (Accessed 4/09/2003.)
Two common myths propagated are that light-colored cars repel heat and that allowing the windows to remain partially open will reverse the effects of the heat. A study conducted in 1995 evaluated the temperature rise inside an enclosed, dark-colored vehicle and compared it to the rate of temperature rise in a light-colored vehicle. Although the temperature rise in this study was more severe in the dark-colored vehicle, the temperature in both vehicles exceeded 125°F within 20 minutes (outdoor temperature was 93°F).45 As several studies (including this one) demonstrate, opening the windows a little also is an ineffectual strategy to keep the interior environment of the car at an acceptable level.46
Although the auto industry is continuing to design and develop technology that may reduce the risk to a child left unattended in a closed vehicle, the important message to parents is that children should never be left unattended in a vehicle. In addition, parents should be reminded that unlocked vehicles may pose a risk to children who unsuspectingly may trap themselves within the car and have no means of escape.
Summary
The scope of heat-related illness is wide ranging from relatively minor problems to heat stoke, associated with major morbidity and mortality. Early recognition of heat exhaustion with appropriate treatment will avoid progression to heat stroke. Heat stroke is a life-threatening emergency and aggressive measures are needed to reduce morbidity and mortality.
Since the start of the 20th century, there has been a rise in the global mean temperature of about 0.6°C.46 There are concerns that this trend will continue. There is a need to develop warning systems, allowing our public health agencies to advise the public on imminent heat waves.47 Physicians, coaches, and athletes need to use guidelines outlined for exercising and training in the heat. Prevention and education remain the keys to combating heat-related illness.
References
1. National SAFE KIDS Campaign/General Motors. Never Leave Your Child Alone. National SAFE KIDS Campaign, Washington, DC; 2002. Available at www.safekids.org. (Accessed 4/09/2003.)
2. Centers for Disease Control and Prevention. Heat-related deaths—four states, July-August 2001, and United States, 1979-1999. MMWR Morb Mortal Wkly Rep 2002;51:567-570.
3. Centers for Disease Control and Prevention. Heat-related mortality—Chicago, July 1995. MMWR Morb Mortal Wkly Rep 1995;44: 577-579.
4. Naughton MP, Henderson A, Mirabelli MC, et al. Heat-related mortality during a 1999 heat wave in Chicago. Am J Prev Med 2002;22:221-227.
5. Semenza JC, Rubin CH, Falter KH, et al. Heat-related deaths during the July 1995 heat wave in Chicago. N Engl J Med 1996;335: 84-90.
6. Dematte JE, O’Mara K, Buescher J, et al. Near-fatal heat stroke during the 1995 heat wave in Chicago. Ann Int Med 1998;129: 173-181.
7. Centers for Disease Control and Prevention. Injuries and deaths among children left unattended in or around motor vehicles—United States, July 2000-June 2001. MMWR Morb Mortal Wkly Rep 2002;51:570-572.
8. Centers for Disease Control and Prevention. Hyperthermia and dehydration-related deaths associated with intentional rapid weight loss in three collegiate wrestlers—North Carolina, Wisconsin, and Michigan, November-December 1997. MMWR Morb Mortal Wkly Rep 1998;47:105-108.
9. Sandor RP, Howe WB. Emergencies in sports. Phys Sportsmed 1997;25:35-40.
10. American College of Sports Medicine position stand: Heat and cold illnesses during distance running. Med Sci Sports Exerc 1996;28:i-x.
11. Kilbourne EM, Choi K, Jones TS, et al. Risk factor for heatstroke. A case—Control study. JAMA 1982;247:3332-3336.
12. Barrow MW, Clark KA. Heat-related illnesses. Am Fam Phys 1998;58:749-756, 759.
13. Simon HB. Current concepts: Hyperthermia. N Engl J Med 1993; 329:483-487.
14. McArdle WD, Katch FI, Katch VL. Exercise thermoregulation, fluid balance, and rehydration. In: Johnson E, ed. Sports and Exercise Nutrition. Philadelphia: Lippincott Williams and Wilkins; 1999:262-291.
15. Khosla R, Guntupalli KK. Heat-related illnesses. Crit Care Clin 1999;15:251-263.
16. Wexler RK. Evaluation and treatment of heat-related illnesses. Am Fam Phys 2002;65:2307-2314.
17. Bouchama A, Knochel JP. Medical progress: Heat stroke. N Engl J Med 2002;346:1978-1988.
18. Centers for Disease Control and Prevention. Heat-related illnesses and deaths—Missouri, 1998 and United States, 1979-1996. MMWR Morb Mortal Wkly Rep 1999;48:469-472.
19. Centers for Disease Control and Prevention. Heat-related Illnesses, deaths, and risk factors—Cincinnati and Dayton, Ohio, 1999, and United States, 1979-1997. MMWR Morb Mortal Wkly Rep 2000; 49:470-473.
20. Centers for Disease Control and Prevention. Heat-related Deaths—Los Angeles County, California, 1999-2000, and United States, 1979-1998. MMWR Morb Mortal Wkly Rep 2001;50:623-626.
21. American Academy of Pediatrics Committee on Sports Medicine and Fitness. Climatic heat stress and the exercising child and adolescent. Pediatrics 2000;106:158-159.
22. Falk B, Bar-Or O, MacDougall JD. Thermoregulatory responses of pre-, mid-, and late-pubertal boys to exercise in dry heat. Med Sci Sports Exerc 1992;24:688-694.
23. Sawka MN, Montain SJ, and Latzka WA. Hydration effects on thermoregulation and performance in the heat. Comp Biochem Physiol A Mol Integr Physiol 2001;128:769-690.
24. Stricker PR. Sports training issues for the pediatric athlete. Pediatr Clin North Am 2002;49:793-802, vii.
25. Luke A, Micheli L. Sports injuries: Emergency assessment and field-side care. Pediatr Rev 1999;20:291-302.
26. Martinez M, Devenport L, Saussy J, et al. Drug-associated heat stroke. South Med J 2002;95:799-802.
27. Martin TJ, Martin JS. Special issues and concerns for the high school- and college-aged athletes. Pediatr Clin North Am 2002; 49:533-552.
28. Bar-Or O, Blimkie CJ, Hay JA, et al. Voluntary dehydration and heat intolerance in cystic fibrosis. Lancet 1992;339:696-699.
29. American Academy of Pediatrics Committee on Sports Medicine and Fitness, 2000-2001. Medical conditions affecting sports participation. Pediatrics 2001;107:1205-1209.
30. Yarbrough B, Vicario S. Heat illness. In: Marx JA, Hockberger RS, Walls RM, eds. Rosen’s Emergency Medicine. 5th ed. St. Louis: Mosby; 2002:1997-2008.
31. Weston WL, Lane AT, Morelli JG. Bullous diseases and mucocutaneous syndromes. In: Fathmann EM and Wilke PM, eds. Color Textbook of Pediatric Dermatology. 3rd ed. St Louis: Mosby; 2002:155-167.
32. Backer HD, Shopes E, Collins SL, et al. Exertional heat illness and hyponatremia in hikers. Am J Emerg Med 1999;17:532-539.
33. Bross MH, Nash TN, Carlton FB Jr. Heat emergencies. Am Fam Phys 1994;50:389-396.
34. Bouchama A, Hammami MM, Haq A, et al. Evidence for endothelial cell activation/injury in heatstroke. Crit Care Med 1996;24: 1173-1178.
35. Lin MT, Liu HH, and Yang YL. Involvement of interleukin-1 receptor mechanisms in development of arterial hypotension in rat heatstroke. Am J Physiol 1997;273:H2072-H2077.
36. Bouchama A, Parhar RS, el-Yazigi A, et al. Endotoxemia and release of tumor necrosis factor and interleukin 1 alpha in acute heatstroke. J Appl Physiol 1991;70:2640-2644.
37. Li PL, Chao YM, Chan SH, et al. Potentiation of barorecptor reflex response by heat shock protein 70 in nucleus tractus solitarii confers cardiovascular protection during heatstroke. Circulation 2001;24:2114-2119.
38. Wang ZZ, Wang CL, Wu TC, et al. Autoantibody response to heat shock protein 70 in patients with heatstroke. Am J Med 2001;111: 654-657.
39. Roberts WO. Disturbances due to heat. In: Rakel RE, Bope ET, eds. Conn’s Current Therapy. 54th ed. Philadelphia: W.B. Saunders; 2002:1159-1161.
40. Delaney KA. Disorders of thermoregulation: Hyperthermia and hypothermia. In: Ford MD, Delaney, KA, Ling LJ, et al, eds. Clinical Toxicology. Philadelphia: WB Saunders; 2001;236-243.
41. Jindal SK, Aggarwal AN, and Gupta D. Adult respiratory distress syndrome in the tropics. Clin Chest Med 2002;23:445-55.
42. Hoffman, JL. Heat-related illness in children. In: Krug SE, ed. Clinical Pediatric Emergency Medicine. Philadelphia: W B Saunders; 2001;203-210.
43. Blue JG and Pecci MA. The collapsed athlete. Orthrop Clin North Am 2002;33:471-478.
44. How CK, Chern CH, Wang LM, et al. Heat stroke in a subtropical country. Am J Emerg Med 2000;18;474-477.
45. Gibbs LI, Lawrence DW, Kohn MA. Heat exposure in an enclosed automobile. J La State Med Soc 1995;147545-546.
46. Easterling DR, Meehl GA, Parmesan C, et al. Climate extremes: Observation, modeling and impacts. Science 2000;289;2068-2074.
47. Kalkstein, LS. Saving lives during extreme weather in summer: Interventions from local health agencies and doctors can reduce mortality. Br Med J 2000;321:650-651.
Since 1996, at least 150 children have died as a result of being trapped in hot, parked vehicles. Contrary to what would be expected, these deaths occurred throughout all regions of the United States, making it important for all emergency medicine physicians to be familiar with the resuscitation of a child with a heat-related illness. This article provides an overview of heat-related illnesses in children and prevention and management strategies to facilitate care.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
