Warfarin vs Aspirin in AF: A Meta-Analysis
Abstract & Commentary
Source: van Walraven C, et al. Oral anticoagulation vs aspirin in nonvalvular atrial fibrillation: An individual patient meta-analysis. JAMA. 2002;288:2441-2448.
Patients with nonvalvular atrial fibrillation (AF) have an increased risk of stroke and other vascular events. Treatment with warfarin decreases the risk of stroke by more than 50%. Aspirin (ASA) also decreases stroke risk but to a lesser extent.1 Several clinical trials have randomized patients with AF to an oral anticoagulant or a regimen containing ASA. Three of these studies determined that warfarin was significantly more effective than ASA at reducing thromboembolic events.2,3,4 Nevertheless, considerable concern exists among clinicians regarding the risk-benefit ratio of long-term anticoagulation compared to antiplatelet treatment.
In order to compare the risk of vascular events and bleeding complications in patients with AF, van Walraven and associates analyzed data from 6 randomized clinical trials.2-7 More than 4000 AF patients were assigned randomly to receive oral anticoagulants, in ASA alone or in combination with low-dose oral anticoagulants. Six possible outcomes were studied: ischemic or hemorrhagic stroke, myocardial infarction, systemic embolism, cardiovascular death, major intracranial or systemic bleeding, and death from any cause.
Compared with ASA, oral anticoagulants significantly decreased the rate of all stroke and cardiovascular events (see Table). The decrease in the rate of all stroke was due to a large decrease in ischemic stroke with only a small absolute increase in hemorrhagic stroke.
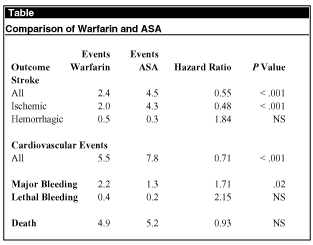
The use of oral anticoagulants significantly increased the rate of major bleeding, and 15% of all major bleeding episodes were fatal. Hemorrhagic stroke accounted for one-quarter of all major bleeding but one-half of fatal bleeding events. Overall mortality, however, did not differ between the oral anticoagulant and ASA patient groups.
The relative benefit of warfarin vs ASA in ischemic stroke prevention was greater for patients younger than 75 years. The absolute risk reduction in ischemic stroke with warfarin was greater in patients at the highest risk of stroke, namely those with a history of previous stroke or transient ischemic attack. Such patients had an absolute risk reduction of 6% per year while patients without previous cerebrovascular events had an absolute risk reduction of 1.2% per year. The increased risk of major bleeding for patients taking warfarin was consistent in all patient subgroups.
Commentary
The meta-analysis of van Walraven et al supports the use of warfarin as first-line preventive therapy for patients with nonvalvular AF. For patients at higher risk of ischemic strokes, the absolute risk reduction in ischemic stroke with warfarin outweighed the associated bleeding risk. Therefore, clinicians must determine baseline risk in order to identify AF patients most likely to benefit from oral anticoagulants.
The present results differ from those of a previous meta-analysis,8 which found no strong evidence to support the clinical practice of long-term anticoagulation in patients with nonrheumatic AF. The previous study8 excluded 2 studies3,7 that showed significant benefits of oral anticoagulants over ASA for strokes and cardiovascular events.
The meta-analysis of van Walraven has clarified the trade-off between the potential harm and benefit of warfarin prophylaxis in AF patients. In high-risk patients, the benefits of warfarin exceed the therapy-associated bleeding events.
— John J. Caronna, MD, Vice-Chairman, Department of Neurology, Cornell University Medical Center; Professor of Clinical Neurology, New York Hospital, Associate Editor, Neurology Alert.
References
1. Hart RG, et al. Antithrombotic therapy to prevent stroke in patients with atrial fibrillation: A meta-analysis. Ann Intern Med. 1999;131:492-501.
2. Petersen P, et al. The Copenhagen AFASAK Study. Lancet. 1989;1:175-179.
3. European Atrial Fibrillation Trial (EAFT) Study Group. Lancet. 1993:342:1255-1262.
4. Stroke Prevention in Atrial Fibrillation Study. Circulation. 1991;84:527-539.
5. Hellemons BS, et al. BMJ. 1999;319:958-964.
6. Gullov AL, et al. Arch Intern Med. 1998;158:1513-1521.
7. The SPAF III Writing Committee for the Stroke Prevention in AF Investigators. JAMA. 1998;279: 1273-1277.
8. Taylor FC, Cohen H, Ebrahim S. Systematic review of long term anticoagulation or antiplatelet treatment in patients with non-rheumatic atrial fibrillation. BMJ. 2001;332:321-326.
Considerable concern exists among clinicians regarding the risk-benefit ratio of long-term anticoagulation compared to antiplatelet treatment. In order to compare the risk of vascular events and bleeding complications in patients with AF, van Walraven and associates analyzed data from 6 randomized clinical trials.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
