Identifying and Treating Seizures and Epilepsy
Authors: Michael D. Privitera, MD, Professor and Vice Chair, Department of Neurology, Director, Comprehensive Epilepsy Treatment Program, Medical Director, UC Physicians, University of Cincinnati Medical Center, Cincinnati, Ohio; and Jennifer Cavitt, MD, Clinical Instructor, University of Cincinnati Medical Center, Cincinnati, Ohio.
Editor’s Note—A seizure is an abnormal, hypersynchronous discharge of a population of cortical neurons that may be associated with clinical manifestations corresponding to the area of the brain involved. This discharge may produce subjective symptoms or objective signs, in which case it is a clinical seizure, or it may be apparent only on an electroencephalogram (EEG), in which case it is an electrographic subclinical seizure. Epilepsy is a disorder of the central nervous system in which symptoms are 2 or more seizures greater than 24 hours apart, not provoked by another cause. Seizures may be provoked in otherwise normal individuals due to various causes. These causes include metabolic disturbances, acute head trauma, acute CNS infection, or effects of illicit or prescription drugs such as cocaine, amphetamines, tricyclic antidepressants, bupropion, and some antibiotics. Young children may have a provoked seizure due to a high fever. In fact, febrile seizures are the most common type of seizure in children. In addition, seizures may be provoked by withdrawal from chronic alcohol or benzodiazepine use. Thus, even multiple seizures provoked only by alcohol intoxication or withdrawal do not constitute epilepsy.
The incidence of new-onset seizures in the general population is about 80 per 100,000 per year. Many patients will have an underlying cause for the seizures, but others will have a single seizure and no recurrence. Approximately 60% of these patients will go on to have epilepsy, or close to 50 cases per 100,000 per year, making the prevalence of epilepsy 5-9 cases per 1000 persons (approaching 1%). Clinical presentation, including history, physical exam, and risk factors, directs the diagnostic workup of patients with a new onset seizure, as well as any subsequent therapy.
Evaluation and Treatment of a First Seizure
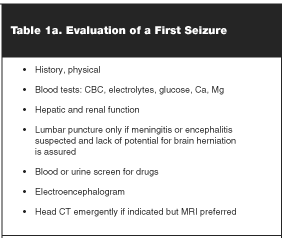
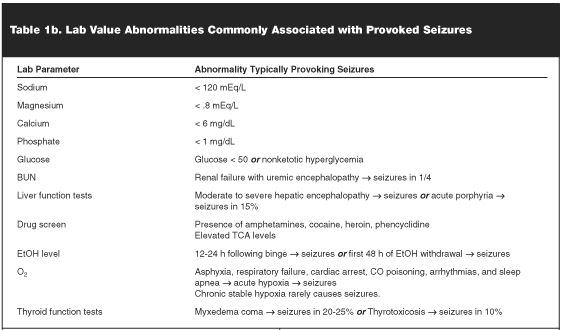
The patient who presents shortly after a first seizure should be screened for symptoms and signs of an acute medical or neurologic illness. Table 1a outlines the evaluation of a first seizure. Careful physical examination and routine blood tests will detect common provoking factors including infection; abnormal electrolyte, glucose, calcium, or magnesium values; and compromised cardiorespiratory, liver, or kidney function. See Table 1b for a list of lab value abnormalities commonly associated with provoked seizures. In addition, a careful medication history will screen for potential prescription drugs that may provoke seizures. Any suspicion of meningitis or encephalitis mandates lumbar puncture once signs and symptoms of increased intracranial pressure have been excluded, but otherwise this procedure is generally not necessary. The use of illicit drugs is an increasingly common cause of provoked seizures, and blood or urine samples should be screened for evidence of substance abuse in almost all cases of unexplained first seizures in age ranges of adolescence through middle age.
Many disorders can present with loss or brief alteration of consciousness. Correct identification of seizures vs nonepileptic events is of utmost importance. When taking a careful history, consider possible nonepileptic events such as syncope, breath holding, panic, cataplexy, transient ischemic attack, and psychogenic events. Ask about behavior, loss of consciousness, amnesia, abnormal movements or inability to move, feelings leading up to the event, duration of the event, and whether confusion was present afterward. Table 2 lists a brief differential diagnosis, and Table 3 has some differentiating characteristics between seizure and syncope, one of the common mimics of seizure.


The EEG is most useful for classifying the seizure type into partial or generalized. In generalized-onset seizures, the EEG usually shows a generalized spike-and-wave pattern from the onset of the seizure or interictally. In partial-onset seizures, the interictal EEG abnormalities are focal. A normal EEG, however, does not exclude the diagnosis of epilepsy since the EEG is only a very brief time sample (20-30 minutes) of the patient’s brain electrical activity.
Anatomic imaging is mandatory in most cases of seizures. Computed tomography (CT) has a role largely confined to emergent assessment of new-onset seizures or seizures. This is especially true when a serious head injury with intracranial hemorrhage or other life-threatening disorders are suspected. The presence of new focal deficits, persistent alteration in mental status, recent head trauma, fever, persistent headache, history of cancer, history of anticoagulation, or suspicion of AIDS all necessitate emergent CT while the patient is still in the emergency department to immediately assess for the possibility of a life-threatening lesion.1 However, MRI is the procedure of choice for anatomic imaging in patients with seizures. MRI with thin cuts through the temporal lobe with T1, T2, and FLAIR sequence is more sensitive than routine brain MRI in detecting abnormalities of the medial temporal structures, from which many partial-onset seizures originate.
Whether antiepileptic drug (AED) therapy should be initiated after a first seizure is the subject of considerable controversy (see Table 4). It is clear that AEDs reduce the likelihood of another seizure, but the risk of serious adverse effects from the AED must be weighed against the benefits. Any patient with a second unprovoked seizure should be treated because of the high risk of a third.

One of the most important distinctions to make is whether the seizures are partial or generalized onset. Partial-onset seizures arise from a focal area of the brain and then spread to involve other areas. The clinical manifestations depend on where in the brain the seizure originates and how far it spreads. For example, a seizure originating in the thumb area of the primary motor cortex may cause twitching of the thumb, whereas a seizure originating in the visual cortex may cause unformed visual hallucinations like swirling colors or flashing lights. Generalized-onset seizures start in the whole brain at once without a focal onset. Either seizure type can eventually involve the entire brain and manifest as a tonic-clonic (convulsive or previously known as "grand mal") seizure, so it is important to take a careful history about how the seizure started.
Clinical Manifestations of Seizures
A common presentation of seizure to the primary care physician is the patient with blanking out episodes, staring spells, or episodes of loss of time. A family member may be the first to notice something is wrong. The two most common seizure types producing these symptoms are absence ("petit mal") seizures or complex partial seizures. Other patients may present with a history of convulsions, jerks, or drop attacks (see Table 5).
Classification of Epilepsies
Although the seizures occurring in patients with epilepsy are not acutely provoked, epilepsy is often related to another neurological disease or insult. The underlying disease or insult generally leads to some type of CNS injury that ultimately increases the risk of seizures emanating from the injured portion of the cortex. Common examples include stroke, brain tumors, previous CNS infection, previous CNS trauma, degenerative diseases, and developmental disorders. These disorders are all associated with an increased risk of epilepsy. In all of these examples, the type of epilepsy syndrome would be considered remote symptomatic. More than half of new cases of epilepsy in elderly patients are related to cerebrovascular disease. On the other hand, 15-30% of new cases of childhood-onset epilepsy are associated with cerebral palsy and/or mental retardation.
Some patients have idiopathic epilepsy syndromes, in which the constellation of age of onset, family history, seizure type, EEG, imaging, physical exam, and natural history of disease fits a particular recognized pattern. These are generally felt to be genetic in origin, even when the genetics of a particular syndrome are not known. Juvenile myoclonic epilepsy would be an example of an idiopathic generalized epilepsy syndrome, and benign rolandic epilepsy (ie, benign epilepsy of childhood with centrotemporal spikes) is an idiopathic partial epilepsy syndrome. Both are relatively common and familial, and each diagnosis carries specific implications about treatment and prognosis.
Finally, there are cryptogenic epilepsy syndromes, in which a remote symptomatic cause cannot be identified and the features do not fit any of the many recognized idiopathic epilepsy syndromes. While idiopathic syndromes are assumed to be genetic in origin, and remote symptomatic epilepsies have an identifiable lesion, in cases of cryptogenic epilepsies, no lesion can be found, though one may be suspected. The number of cryptogenic cases has been decreasing as the quality of available testing such as MRI improves.
Medical Treatment of Epilepsy
For epilepsy, the drug of choice should have the best efficacy and fewest adverse effects. For generalized-onset seizures, specifc AEDs may be indicated, while others would be contraindicated, possibly making seizures worse. In contrast, several comparison studies have shown minimal differences in efficacy of the standard AEDs in partial-onset seizures, the most common seizure type. Thus, differences in expected adverse effect profile, pharmacokinetic profile, and expense should help guide AED choice. There is no convincing clinical evidence that AED choice (for monotherapy or combinations) should be based upon mechanism of action. Many patients can be optimally managed on a single AED. It is essential to ensure that a drug has failed before moving on to an alternative drug or a 2-drug combination. A drug has failed when it has been given at doses high enough to produce persistent side effects and seizures are still not controlled. Most epileptologists consider seizure freedom good control. A patient who continues to have seizures is not "well controlled." Most neurologists will try 2-3 drugs as monotherapy before resorting to a drug combination.2
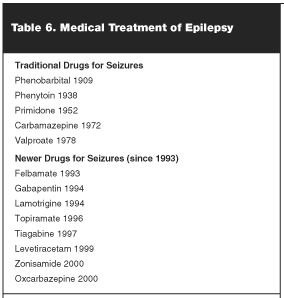
AEDs are divided between "standard" and "new" drugs. Between 1978 and 1993, no new drugs were approved by the FDA. Phenytoin, the most commonly used AED in the United States has been used to treat epilepsy since the 1930s. Starting in 1993, 8 new AEDs, a new stimulator device, and a new formulation of intravenous phenytoin have come on to the market. None of these new medications has characteristics that make it likely to completely replace the use of the standard medications, but they offer modest improvement in efficacy, important improvements in adverse effects, and more options for individual patients (see Table 6).
Treatment of Generalized-Onset Epilepsy
In patients with generalized-onset epilepsy, the choice of drug depends on the specific epileptic syndrome being treated. Valproate is the drug of choice in patients who have myoclonus, photosensitive epilepsy, or absence with generalized tonic-clonic seizures. In children with only absence seizures (petit mal of childhood) and no generalized tonic-clonic seizures, ethosuximide and valproate are equally effective. Some clinicians consider ethosuximide to be safer in children because of the rare but severe hepatotoxicity that may occur with valproate. In a retrospective review, the risk of valproate-induced hepatotoxicity was maximal in children younger than 2 years, especially those treated with multiple AEDs or who had congenital metabolic disorders. Thus, avoiding valproate use in these subgroups may reduce the risk of hepatotoxicity. In patients with generalized-onset tonic-clonic seizures, phenytoin and valproate were equally effective and safe in a randomized comparison trial. Patients with Lennox-Gastaut syndrome, a particularly severe epileptic syndrome associated with multiple seizure types, usually a high seizure frequency and some degree of cognitive impairment, showed significant seizure reductions when treated with felbamate, lamotrigine, or topiramate in randomized trials. There is preliminary information that lamotrigine and topiramate are effective in various generalized epilepsy syndromes. Clonazepam and phenobarbital can also be useful, but both tend to have substantial sedative adverse effects. Clonazepam, a benzodiazepine, tends to have a duration of maximal effect of less than 6 months.
Treatment of Partial-Onset Epilepsy
In partial-onset seizures with secondary generalization, carbamazepine, phenytoin, valproate, phenobarbital, and primidone can be effective. In partial seizures without generalization, phenytoin and carbamazepine may be slightly more effective than phenobarbital or primidone. These conclusions are based on direct randomized comparison studies of these medications.3,4 The place of the new AEDs in epilepsy treatment is still evolving. All 8 drugs and the new device (felbamate, gabapentin, lamotrigine, topiramate, tiagabine, levetiracetam, oxcarbazepine, zonisamide, and the vagus nerve stimulator) have been proven superior to placebo as adjunctive treatment in patients with medication-resistant partial seizures. Few direct comparisons among the new drugs or among the new and older drugs have been performed. However, in a series of studies in Europe, lamotrigine was shown to be equally effective and better tolerated than the first-line drugs carbamazepine and phenytoin in new onset seizures.5-7 In a head-to-head study, topiramate was equal to carbamazepine and valproate. On the other hand, in monotherapy trials, gabapentin has not been particularly promising. The best way to choose among these drugs is using adverse effect profile and pharmacokinetics. For example, gabapentin and levetiracetam have no liver metabolism and almost no drug interactions; lamotrigine is associated with little sedation; felbamate is rarely used because of an association with aplastic anemia (~1/4500, 30% mortality) and hepatic failure (~1/22,000, 50% mortality).8 We must await further comparison studies to identify the drug or drugs that are clearly superior overall. Tables 7a and 7b summarize the important characteristics of AEDs.
Some of the AEDs have "broad spectrum" efficacy. This implies that they work for either partial-onset or generalized-onset seizures. Valproate, topiramate, lamotrigine, and possibly levetiracetam and zonisamide have broad-spectrum efficacy (see Table 8).

Practical Pharmacology of AEDs
Three important pharmacological considerations in using AEDs are: (1) phenytoin exhibits saturation (nonlinear) kinetics; (2) AED combinations can cause induction or inhibition of hepatic metabolism or changes in protein binding, so monotherapy is desirable whenever possible; and (3) serum concentrations of AEDs should be used as general guidelines in determining dose.
Phenytoin (Dilantin) exhibits nonlinear kinetics because the metabolic enzymes saturate at commonly used doses. This means that small changes in dose can produce large changes in serum concentration; these changes get even larger as serum concentrations increase. Accurate clinical rules to use are: (a) if the initial serum concentration is below 7 and the dose needs to be increased, increase the daily dose by 100 mg; (b) if the serum concentration is between 7 and 12 and the dose needs to be increased, increase the daily dose by 50 mg; (c) if the serum concentration is above 12 and the dose needs to be increased, increase the daily dose by 30 mg.9
AED monotherapy can simplify treatment, reduce adverse effects, and often improve seizure control. Several studies have shown that many patients with seizures, even patients whose seizures are not well controlled, may have equal or fewer seizures and fewer adverse effects by using high doses of a single AED rather than drug combinations. When seeing patients on multiple AEDs, attempt to withdraw sedative ones first (barbiturates and benzodiazepines). When trying to reach monotherapy, withdrawal of concomitant AEDs should be done slowly, usually over several months. Some patients truly benefit from AED combinations, but there are no reliable studies showing which combinations are most effective.
AEDs that are highly bound to serum proteins (phenytoin and valproate) may be displaced from binding sites by other medications that are also highly protein bound (eg, aspirin, warfarin, phenothiazines). In these cases, the serum concentration may not accurately reflect the unbound proportion of drug. Unbound ("free") serum concentrations should be obtained in patients taking phenytoin or valproate who have altered protein binding, such as those on other drugs that are highly protein bound, or patients with significant renal or hepatic disease, AIDS, or hypoalbuminemia from any cause.
Most AEDs are metabolized by hepatic enzymes and may either induce or inhibit hepatic metabolism of other drugs. The exceptions are the new AEDs gabapentin and levetiracetam, which have no measurable hepatic metabolism. Induction of hepatic enzymes by AEDs such as carbamazepine, phenytoin, and phenobarbital may cause increased metabolism and decreased serum concentrations of other drugs (including oral contraceptives). Valproate tends to be a metabolic inhibitor and increases serum concentrations of other hepatically metabolized drugs. Conversely, other nonantiepileptic drugs (eg, erythromycin, a potent metabolic inhibitor) may inhibit the metabolism of carbamazepine, leading to an increase in side effects. Similar effects may occur with other macrolides or with propoxyphene. Monitoring serum concentrations of AEDs is particularly important when using drug combinations (see Table 9).

Antiepileptic serum concentrations that are likely to provide seizure control without significant toxicity have been derived from small studies and from clinical experience. Although not a substitute for the individual patient’s clinical response, which is still the basis for assessment of AED performance, the range of recommended concentrations may be a useful guide when AED therapy is initiated or when therapy is adjusted in response to breakthrough seizures or toxicity—especially when using the standard AEDs. Several studies have shown, however, that many patients can experience excellent seizure control without adverse effects with serum concentrations above or below the "therapeutic range." "Therapeutic ranges" for the new antiepileptic drugs are probably even less reliable than for the standard drugs. Clinicians should not rigidly adhere to a therapeutic range for AEDs but rather use serum concentrations to "benchmark" the level at which a patient has good seizure control and minimal side effects, thus achieving the goal of balancing AED antiseizure efficacy and toxicity.
Pharmacokinetic factors should also be considered when interpreting AED serum concentrations. A drug’s half-life in serum is the time required for the drug’s serum concentration to drop to one half its original value. Most drugs need 5 half-lives to reach steady state. Drugs with long half-lives, such as phenytoin and phenobarbital, may require 3-4 weeks to reach steady state. Thus, serum concentrations drawn before that time interval after drug initiation or a dose change may not accurately reflect steady state. Conversely, the serum concentrations of drugs with short half-lives may be significantly affected by the time interval between the last dose and the serum sample.
Starting and Stopping AEDs
Before starting a new AED, the expected adverse effect profile should be discussed with the patient along with some realistic expectations of efficacy (fewer than 50% of adults with partial-onset seizures will remain seizure-free for more than 12 months).
AEDs can eventually be withdrawn successfully in more than 60% of patients who remain seizure-free for 2-4 years.10 The longer the patient remains free of seizures on medication, the lower the risk of recurrence if medication is stopped; the risk is never zero. Most drugs are withdrawn over 2-6 months. The underlying epileptic syndrome influences the prognosis for remaining seizure-free after AED withdrawal. Alcohol consumption can make seizures more likely, but medications should not be stopped and started based on alcohol intake.
Seizures in Children
Because efficacy data in childhood epilepsy are limited, antiepileptic selection for children relies on comparative efficacy studies in adults. Fortunately, the efficacy of most agents in children parallels the adult experience. Efficacy is not the only consideration, however, because adverse effects and toxicity are of paramount importance in pediatrics and often are the major determinant of drug selection. Pharmacokinetics, especially rate of elimination, may differ from adults and also vary greatly depending on the age of the child. The FDA is now encouraging pharmaceutical companies to include some information on kinetics in children in product labeling, even when the drug is not approved in children, because it is likely the drug will be used in younger patients.
Seizures in the Elderly
It is surprising to many clinicians that beyond childhood, the incidence of epilepsy is highest in the elderly. Older patients may have seizure manifestations that are somewhat atypical, like confusional or aphasic spells, so a careful history and an EEG are important. When treating an older patient with AEDs, it is best to choose drugs with the lowest likelihood of interacting with the older patient’s other medications. Usually this means choosing AEDs with low protein binding and little or no hepatic metabolism. Older patients often need lower doses and slower titration than younger patients because they have slower hepatic metabolism and are more sensitive to adverse effects. In the elderly, AED dosing should be "low and slow."
Medication-Resistant Epilepsy
Most patients with epilepsy can have seizures completely controlled with minimal or no adverse effects. About 15-37% of patients will fail many AEDs. In one study, failure of 2 AEDs was highly predictive of resistance to all medical treatment.11 Patients whose seizures cannot be controlled with medications are considered medically intractable. The goal of therapy is no seizures. Those who continue to have seizures despite trials with maximal tolerated doses of standard anticonvulsants (phenytoin, carbamazepine, and valproate) should be referred to a comprehensive epilepsy center with video/EEG monitoring. Video/EEG can accurately identify patients with nonepileptic events, characterize seizure type for better treatment choice, and identify epilepsy surgery candidates. There are several nondrug treatments for epilepsy, usually reserved for patients who have failed 1 or more AEDs. Most epilepsy experts suggest referring patients to a comprehensive epilepsy center who have failed 3 or more AEDs singly or in combination.2
Nondrug Treatments for Epilepsy
Epilepsy Surgery
Surgical treatment of epilepsy, first performed 100 years ago, has seen resurgence in the last 2 decades due to better and safer techniques for seizure localization and surgery. Epilepsy surgery was more effective and not more risky than continued medical treatment in a recent randomized, controlled trial.12 After a failure to respond to maximal tolerated doses of 3 different drugs, the likelihood a patient will become seizure-free with additional drug trials is < 5%. On the other hand, epilepsy surgery performed at specialized epilepsy centers can result in seizure-free rates of up to 80% of patients who have failed available drug treatment. The best outcomes are seen in patients with seizures emanating from the medial temporal structures, who also have MRI abnormalities consistent with mesial temporal sclerosis (MTS). An MRI protocol with thin cuts through the temporal lobe is most sensitive in picking up this type of abnormality. Patients with unilateral temporal lobe epilepsy without MTS have slightly lower seizure-free rates postoperatively, but they typically have better outcomes than expected with continued medical treatment. The risk for complications associated with surgery (bleeding, infection, visual field cut, language, and memory disturbance) is ~2%. An intracarotid amytal test is performed to determine each patient’s language dominant hemisphere, as well as the memory function of each hemisphere. This helps to exclude those patients at increased risk for postoperative complications. Patients with extratemporal epilepsy may also be candidates for surgery, depending on seizure localization and the presence of focal lesions on MRI.
Vagus Nerve Stimulator
The vagus nerve stimulator is a medical device approved by the FDA in 1997 for adjunctive treatment of medically refractory partial-onset seizures in patients older than 12 years. The mechanism of action is not well understood. The device, similar in size and shape to a cardiac pacemaker, is implanted in the left chest wall. The leads wrap around the left vagus nerve in the neck. The device is interrogated and programmed using a computer and programming wand. The device is programmed to stimulate the vagus nerve intermittently throughout the day and night. A typical program consists of 30 seconds of "on time" (active stimulation) and 5 minutes of "off time" (no stimulation). In addition, the patient is provided with a handheld magnet that when swiped over the device will immediately initiate the programmed "on" sequence. This is helpful in aborting or shortening seizures in some patients. Overall, efficacy is similar to that of medications: 50% seizure reduction in one- to two-thirds of patients. In addition, some patients note an improvement in seizure severity and duration. Adverse effects are quite different from those seen with AED use. A sensation or pain in the throat, coughing, subjective dyspnea, and change in voice are noted during stimulation. Discomfort and cough can by minimized by slow adjustment of settings. Unilateral vocal cord paralysis is a complication of implantation in 1%. Prior to implantation, a patient should be evaluated at an epilepsy center to determine whether the procedure is appropriate and whether the patient is a candidate for epilepsy surgery, which has a better prognosis for seizure freedom in appropriate patients.
The ketogenic diet has been used in children with medication-resistant seizures for decades and has seen resurgence in the past few years, due in part to great interest by the media. It is based on the observation that ketosis and acidosis have anti-seizure effects. Initial hospitalization for fasting is followed by a high-fat diet with strict protein, calorie, and especially carbohydrate restriction, which is required to maintain ketosis and may be difficult to maintain. There is little information on the long-term effects of the diet and almost no data on its use in adults.
Epilepsy and Pregnancy
It has become clear that a wide variety of birth defects are associated with the use of virtually all AEDs. The incidence of major birth defects (those requiring medical or surgical intervention) in the normal population is approximately 2%, whereas the offspring of epileptic mothers have a 4-8% incidence of major malformations, with another 5-30% having minor cosmetic anomalies such as shortened distal digits.13-16 The most common major malformations seen with fetal AED exposure are neural tube defects, congenital heart disease, and orofacial clefts. Some of these defects may be genetic or induced by seizures during pregnancy, but the greatest influence appears to be related to AEDs. Greater risk is associated with polytherapy and with high serum AED concentrations in the first trimester. The dilemma is to minimize AED use without risking seizures, which may also be harmful to the fetus. Women of childbearing age with epilepsy should take at least 400 ug/d of folic acid to lower the risk of neural tube defects. Because neural tube formation occurs in the first month, often before women know they are pregnant, and because there is a high rate of unplanned pregnancies, women who have the potential to become pregnant should take folic acid even before planning to conceive. In addition, because AED levels tend to drop throughout pregnancy, levels should be checked monthly with appropriate dose adjustments. Table 10 lists the current guidelines for managing AEDs in women planning pregnancy.14

Driving and Epilepsy
Epilepsy is unique in the variety of legal problems that it creates. Among these, none engenders as much debate and controversy as driving. All states seek to regulate driving by persons with epilepsy. Standards are spelled out by statute, or there are broad guidelines that are used by driving agencies and allied medical review boards. Most states require that patients remain seizure-free for a specified period of time (3-12 months) before they will be permitted to drive again. This is true following every seizure. Thus, if a patient has an average of 2 seizures per year, and if local law requires 6 months seizure-free before the patient may drive, that patient essentially would never be allowed to drive. Thus, this issue has a dramatic effect on patients’ quality of life.
Seizure Recognition and First Aid
An outline follows for recognition and first aid for generalized tonic-clonic and complex partial seizures, the 2 most common seizure types in adults.
Generalized Tonic-Clonic Seizure:
Appearance: Sudden cry, fall, rigidity, followed by muscle jerks, shallow breathing or apnea, possible urinary incontinence, typically lasts 1-2 minutes with post-seizure confusion.
What to do: Turn person on his side to keep airway clear and protect from nearby hazards. If outside the hospital, transfer to the hospital is often unnecessary if there is a history of seizures. Further evaluation is needed if person is pregnant, injured, or diabetic. If multiple seizures, or a seizure longer than 5 minutes occurs, treatment for status epilepticus should ensue.
What not to do: Do not put anything in the person’s mouth or hold the tongue. Do not use artificial respiration unless breathing is absent after jerking subsides.
Complex Partial Seizure
Appearance: Usually starts with blank stare, chewing, and then random activity. The person appears unaware of surroundings and unresponsive to commands. Seizure usually lasts 1-2 minutes, often with post-seizure confusion and memory loss for the event.
What to do: Speak calmly and guide gently away from obvious hazards. If outside the hospital, stay with the person until he or she is completely aware of environment and offer help getting home. Medical evaluation is needed for a new-onset seizure if the person is pregnant or injured.
What not to do: Don’t grab hold or restrain unless there is a dangerous situation like traffic. Don’t shout or expect verbal instruction to be obeyed during or immediately following the seizure.
References
1. Report of the Quality Standards subcommittee of the American Academy of Neurology. Practice Parameter: Neuroimaging in the emergency patient presenting with seizure—Summary statement. Neurology. 1996;47:288-291.
2. Karceski SC, et al. The expert consensus guideline series: Treatment of epilepsy. Epilepsy and Behavior. 2001;2(6):A1-A50.
3. Mattson RH, et al. Comparison of carbamazepine, phenobarbital, phenytoin, and primidone in partial and secondarily generalized tonic-clonic seizures. N Engl J Med. 1985;313:145-151.
4. Mattson RH, et al, for The Department of Veterans Affairs Epilepsy Cooperative Study No. 264 Group. A comparison of valproate with carbamazepine for the treatment of complex partial seizures and secondarily generalized tonic-clonic seizures in adults. N Engl J Med. 1992;327:765-771.
5. Brodie MJ, Dichter MA. Antiepileptic drugs. N Engl J Med. 1996;334:168-175.
6. Reunanen M, et al. A randomized open multicentre comparative trial of lamotrigine and carbamazepine as monotherapy in patients with newly diagnosed or recurrent epilepsy. Epilepsy Res. 1996;23:149-155.
7. Steiner TJ, et al. Lamotrigine monotherapy in newly diagnosed untreated epilepsy: A double-blind comparison with phenytoin. Epilepsia. 1999;40(5):601-607.
8. Pellock JM. Felbamate. Epilepsia. 1999;40(Suppl 5):S57-S62.
9. Privitera M. Clinical rules for phenytoin dosing. Ann Pharmacother. 1993;27(10):1169-1173.
10. Report of the Quality Standards subcommittee of the American Academy of Neurology. Practice Parameter: A guideline for discontinuing antiepileptic drugs in seizure-free patients—Summary statement. Neurology. 1996;47:600-602.
11. Kwan P, Brodie MJ. Early identification of refractory epilepsy. N Engl J Med. 2000;342(5):314-319.
12. Wiebe S, et al. A randomized, controlled trial of surgery for temporal-lobe epilepsy. N Engl J Med. 2001;345(5):311-318.
13. Kelly TE, et al. Teratogenicity of anticonvulsant drugs II: A prospective study. American Journal of Genetics. 1984;19:435-443.
14. Report of the Quality Standards subcommittee of the American Academy of Neurology. Practice parameter: Management of women with epilepsy (summary statement). Neurology. 1998;51:944-948.
15. Samren EB, et al. Maternal use of antiepileptic drugs and the risk of major congenital malformations: A joint European prospective study of human teratogenesis associated with maternal epilepsy. Epilepsia. 1997;38(9):981-990.
16. Steegers-Theunissen RPM, et al. Factors influencing the risk of abnormal pregnancy outcome in epileptic women: A multi-centre prospective study. Epilepsy Res. 1994;18:261-269.
Suggested Reading
1. Brodie MJ, et al. Double-blind comparison of lamotrigine and carbamazepine in newly diagnosed epilepsy. Lancet. 1995;345:476-479.
2. Dichter MA, Brodie MJ. New antiepileptic drugs. N Engl J Med. 1996;334:1583-1590.
3. Rowan AJ. Management of seizures in the elderly. Pharmacotherapy. 2000;20(8 pt 2):178S-184S.
A seizure is an abnormal, hypersynchronous discharge of a population of cortical neurons that may be associated with clinical manifestations corresponding to the area of the brain involved. Epilepsy is a disorder of the central nervous system in which symptoms are 2 or more seizures greater than 24 hours apart, not provoked by another cause.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
