EMRs: Risk of the Mouse Click
April 1, 2014
Reprints
EMRs: Risk of the Mouse Click
By Kevin Klauer, DO, EJD, Chief Medical Officer, Emergency Medicine Physicians, Canton, OH
Electronic medical records (EMRs) have quickly become the standard in most U.S. emergency departments. A few short years ago, working with an EMR was largely the exception and not the rule. However, following implementation of the meaningful use program, and its associated financial incentives, EMR use has exploded and become the new standard. Unfortunately, as with any other initiative, when incentives are misaligned, the consequences can be disastrous. Although many hospital administrators and providers are quick to embrace improved information exchange, data collection, patient tracking, and improved patient safety, the incentive that resulted in widespread EMR adoption was ultimately financial from revenue generated from meaningful use incentives and improved documentation and charge capture. However, currently available systems have not only fallen short in improving safety and reducing medical-legal risk, many providers and patients have fallen victim to the law of unintended consequences.
EMRs conceptually offer a great potential upside, particularly with broader application, such as a hospital system, but it cannot be overstated that much of actualized benefit is financial and results from standardization, reduced transcription costs, economies of scale, and found money (e.g., meaningful use payments). Data collection, for the purpose of performance improvement and utilization tracking of systems, individual departments, and providers is a value-added benefit if used effectively. You just simply can’t expect to get something for nothing; there are real (not hypothetical) trade-offs with the use of EMRs.
Those trade-offs include reduced physician/provider productivity, billing and coding compliance issues, and new medical-legal threats uniquely introduced by EMRs themselves.
So, the ship has sailed. The days of running an ED without an EMR are virtually over. For hospitals, the math is just too simple. The sticker shock associated with EMRs was a previous barrier to implementation, a barrier allowing for healthy skepticism. However, once meaningful use incentives were entered into the equation and large-scale operational efficiencies (economies of scale) have been proved with their use, there is little hesitation on the part of hospital administrators. Unfortunately, the return on investment seems pragmatically clear, but the inherent risks are not, and are only being recognized as our experience with EMRs grows.
The Business Case: Return on Investment
There are sufficient published data to seal the deal with hospitals, and particularly hospital systems. In a recent discussion paper published by the Institute of Medicine in January of this year, the case for the return on investment is adeptly made, highlighting the experience of three hospital systems, Kaiser Premanente, the U.S. Department of Veterans’ Affairs, and Sentara (a small- to medium-sized system operating more than 100 sites of care, including seven acute care hospitals).1 This is a 24-page report, highlighting their experiences with EMR implementation. The report stated that Kaiser: "Anticipated $2 billion cash flow from the $1 billion investment over the 10-year investment horizon (using medium implementation scenario). Long-term hospital cost structure reduction of up to 2.3% and increased revenue by 0.6%."1 The V.A. system reported substantial value from implementation: "The total net value exceeded $3.09 billion, with annual net value exceeding $687 million. The gross value of the benefits was projected to be $7.16 billion, with 65% resulting from prevention of unnecessary care and 27% from eliminated redundancies. Reduced work, decreased operating expenses, and freed space accounted for the rest."1 Sentara also made their business case for EMR implementation: "Higher benefit-to-cost ratios during each implementation year, resulting in cumulative benefits of $48.5 million for 2010."1
In a deeper exploration of Sentara’s experience, they implemented EPIC across all of its seven acute care hospitals. The ownership costs were $237 million, $170 million of operational expense, and $67 million in capital expenditures. Their meaningful use revenue was $70 million, and their projected annual savings was $53 million.2 Publishing such data will most likely prompt even the most reluctant hospital CEO to adopt this technology, and it is strongly suspected that once health information systems (HIS) are adopted, it is very unlikely that we will return to our former low- tech era; de-installations are fairly uncommon.
The Negative Impact on Productivity
Regarding provider productivity, EMRs have been reported to reduce productivity. With the combination of computerized entry (CPOE), with its complex matrix of drop-down menus and often intrusive attempts at clinical decision support, many physicians have reported increased charting time, less time at the bedside, and decreased productivity. Installations have been associated with reduction in physician productivity that, after considerable effort, may improve, but not necessarily return to baseline. A recent article in the American Journal of Emergency Medicine reported that 43% of emergency physician time is spent on data entry, while only 28% on direct patient care. In addition, the least number of mouse clicks necessary to complete an action was six (ordering an aspirin) and the highest number was 227 to complete documentation of a record for a patient with right upper quadrant abdominal pain. In addition, the authors estimate that a 10% increase in productivity in the community hospital studied would result in $1.77 million in increased revenue. Finally, seeing 2.5 patients per hour while working a 10-hour shift would require 4,000-mouse clicks.3
Other studies have also reported the increased workload created by EMRs. When the provider’s attention and efforts are diverted from the bedside and away from direct patient care, the primary provider interface becomes with the computer, as opposed to the patient. Less face-to-face time with patients may result in a greater risk of medical error and suffering a risk management event (i.e., incident reports, claims, and lawsuits). In 2005, Poissant reported that EMRs increase documentation time by 17%, while CPOE was associated with a 98% increase in documentation time.4 In addition to increased documentation time of four- to five-fold following EMR implementation in an academic emergency department, Park reported that the number of incomplete charts increased, attending documentation was exchanged for disproportionately more resident documentation, less time was spent at the bedside, and there was "increased cognitive burden."5 In other words, the authors identified the additional concern that the complexities of EMR use added to the intellectual or cognitive burden of an already mentally exhausting environment.
In the family practice setting, arguably less challenging than an emergency department, productivity increased (1.49 to 1.79 relative value units [RVUs]/hr) and documentation improved, but 66% of physicians stated that their workload was increased by the EMR.6
Despite the fact that sufficient evidence exists to support the negative impact EMRs have on physician productivity, it appears that as the transition becomes more commonplace, not all will experience the same impact. In January of this year, Ward et al evaluated the effects of electronic health record (EHR) implementation on 8 metrics (e.g., arrival to provider, overall length of stay, length of stay for admitted patients, length of stay for discharged patients, left before treatment complete, significant returns, overall patient satisfaction, and provider efficiency) in 23 community emergency departments.7 They found no statistical differences in those categories. Nonetheless, the preponderance of data more than suggests that most EDs will be negatively impacted, in one way or another, by EMR implementation, and issues such as time spent away from the bedside, increased cognitive burden, and increased workload are likely to result in a commensurate increase in professional liability.
Many strategies have been utilized to buffer the negative impact on productivity, including increasing physician and advanced practice provider (non-physician clinician) coverage, increased resident coverage, and the introduction of scribes into the ED workflow. Perhaps, the most widely utilized and cost-effective option is the latter. Scribes have proven more valuable than ever when EMRs are implemented in the ED. Beyond documentation assistance, their role can be expanded to additional non-medical roles such as setting up suture trays and notifying the physician when a complete data set is available for a given patient, expanding their role to that of a patient flow tech. Becker’s review reported that ED scribe programs may increase RVUs per visit and hour, reduce lost revenue from deficient charting, and reduce the number of incomplete and unbillable charts.8 The business case for scribes is outlined in an information paper released by the American College of Emergency Physicians (ACEP) in 2011. The paper highlights that scribe expense ranges from $10 per hour to $26 per hour and that in one example, the use of scribes increased productivity by 17%.9 Although scribes have proven to be a viable solution for EMR-induced productivity issues, there are limits to the application, and exceeding those limitations can result in serious compliance issues. First and foremost, scribes are not to provide medical treatment. For scribes without medical training, this is a very easy directive to follow. However, when a medical provider is functioning as a scribe, his or her duties must not include the provision of medical care.
For example, in 2007, a Tampa, Florida jury awarded a plaintiff $217 million for a missed cerebellar stroke. The physician assistant (PA) involved in the care of the patient was actually hired as an "expediter" or scribe.10 However, it was later discovered in deposition testimony that the PA was unlicensed due to not passing the state licensing examination on four occasions. Although an extreme example, it is applicable nonetheless, illustrating how medical providers being employed as scribes can easily expand beyond their job description, resulting in disastrous consequences. What is the provision of medical care? Per The Joint Commission, entering orders via CPOE constitutes the provision of medical care, and scribes are prohibited from performing this function. The rationale is that when clinical decision support prompts are encountered, medical decision-making is required to address them. Thus, scribes are not qualified or allowed to make such judgments.11
Figure 1: Percentage of E/M Codes Billed for ED Visits from 2001-2010
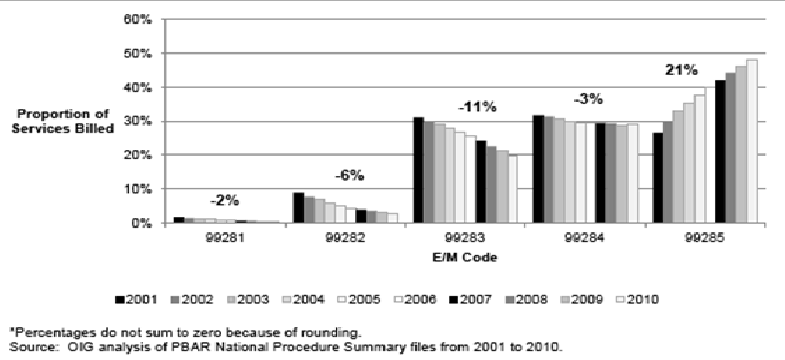
EMRs Improve Charge Capture While Raising Red Flags
Enhanced charge capture is an inevitable incentive for EMR adoption. What is perplexing is that the Centers for Medicare & Medicaid Services (CMS) and the Office of Inspector General (OIG) have identified EMR abuse as the newest target for false claims fraud and abuse surveillance, investigation, and enforcement. It is truly unconscionable that the OIG has been empowered to pursue increased revenues from EMR use as fraud and abuse when the federal government was the driving force for adoption of this technology, and that increased charge capture and associated Medicare claims was foreseeable.
Nonetheless, the OIG has made it clear that it has identified increased charges under the Medicare program between the years 2001 and 2010, and that it believes that such increases are substantially in part due to E/M service vulnerability to fraud and abuse.12
"OIG is conducting a series of evaluations of E/M services provided to Medicare beneficiaries in 2010. OIG plans to issue two others in addition to this report. One will determine the appropriateness of Medicare payments for E/M services. The other will assess the extent of documentation vulnerabilities in E/M services using electronic health record systems."12
Figure 3 from the report reflects the growth in E/M code 99285 (level 5) from 27% of charts billed to 48%, an increase of 21%.
For surveillance purposes, the OIG’s report states that 1,700 physicians were identified with increased billing of higher E/M levels (e.g., the two highest codes in a visit type 95% of the time).12
In a rebuttal article in the New England Journal of Medicine, Pitts stated that use of lower codes has declined and use of higher codes has increased due to an aging and sicker Medicare population, as opposed to upcoding and improved documentation from EMR use.13
In January of 2014, the OIG fulfilled their promise from 2012 and released their report regarding EHR vulnerabilities and "program integrity practices" that have been implemented.14 Two of the highlighted initiatives are "copy-pasting" and "over documentation." Although the OIG accepts transfer of information if accuracy is ensured, their description and intent are clear. Successfully complying with the regulations if you choose to cut and paste into the records is so unlikely, the practice should be abandoned. Below is the language directly from the report.14
"Copy-pasting, also known as cloning, enables users to select information from one source and replicate it in another location. When doctors, nurses, or other clinicians copy-paste information but fail to update it or ensure accuracy, inaccurate information may enter the patient’s medical record and inappropriate charges may be billed to patients and third-party health care payers. Furthermore, inappropriate copy-pasting could facilitate attempts to inflate claims and duplicate or create fraudulent claims."
Although inadvertent over-documentation is relatively easy to do within an EMR with its various drop-down menus and auto-populated fields, the OIG has a zero-tolerance policy. The following outlines the OIG’s expectations.14
"Over-documentation is the practice of inserting false or irrelevant documentation to create the appearance of support for billing higher level services. Some EHR technologies auto-populate fields when using templates built into the system. Other systems generate extensive documentation on the basis of a single click of a checkbox, which if not appropriately edited by the provider, may be inaccurate. Such features can produce information suggesting the practitioner performed more comprehensive services than were actually rendered."
Risks Inherent to EMRs
Beyond compliance, EMRs have been shown to introduce new sources of risk and liability. In a landmark article published in the New England Journal of Medicine, several liability risks associated with EMRs were identified. Specifically, the authors note the potential risks during three phases of EMR use: implementation, as systems mature in place, and as EHRs become more widespread.15
Potential risks during initial implementation include:
• Transition from paper to electronic record may create documentation gaps.
• Failure to implement procedures that a prudent or reasonable provider would implement to avoid errors during the transition period may leave providers vulnerable in tort.
• Inadequate training on EHR systems may create new error pathways.
• Errors by new system users may create incorrect or missing data entries.
• Failure of clinicians to use EHRs consistently may lead to gaps in documentation and communication.
• Systemwide EHR "bugs" and failures could adversely affect clinical care, leading to injuries and claims.
As systems mature in place, the following risks are identified:
• E-mail advice multiplies the number of clinical encounters that could give rise to claims and may heighten the risk of claims if advice is offered without thorough investigation and examination of the patient.
• More extensive documentation of clinical decisions and activity creates more discoverable evidence for plaintiffs, including metadata.
• Temptation to copy and paste patient histories instead of taking new histories risks missing new information and perpetuates previous mistakes.
• Failure to reply to patient e-mails in a timely fashion could constitute negligence and raise patient ire.
• Information overload may cause clinicians to miss important pieces of information.
• Departures from clinical-decision support care guidelines could bolster plaintiffs’ case.
As EHRs and health information exchanges (HIEs) become widespread:
• Better access to clinical information through EHRs could create legal duties to act on the information.
• Widespread use of clinical-decision support may solidify standards of care that might otherwise be subject to debate.
• The rise of HIEs may heighten clinicians’ duties to search for patient information generated by other clinicians.
• Failure to adopt and use electronic technologies may itself constitute a deviation from the standard of care.
Of particular note is the creation of metadata, creating discoverable events and data generated from every entry, mouse click, and query behind the screen. As decision support becomes intrusive, the prompts are largely ignored, and widespread decision support becomes validated with every mouse click-generated answer.
Many other articles have been published highlighting these high-risk items and several others. Of particular importance is the concept of e-discovery. e-discovery is the request for all EMR screen shots and metadata, which is often in excess of $50,000 to produce.15 Even EMR selection, implementation, and every aspect of use may be requested and examined in discovery.17
The OIG and plaintiff’s attorneys have identified the value of audit logs, which can be queried to track chronological changes in a record, including date, time, and user stamps for every entry into an EMR, which are being used for noting inconsistencies in the record.14
The first step to avoiding risk with EMR use is to be aware of the sources of risk or pitfalls. Farley et al published a paper noting four common pitfalls in ED EMRs: communication failures, poor data display, wrong order-wrong patient errors, and alert fatigue.18 Although operational redesign and user-centric solutions are essential to reduce risk, it is unlikely we will see them any time soon. Currently, the best approach is awareness. Being knowledgeable of the common pitfalls of EMR use, plaintiff’s attorney strategies for use of EMR data, and the OIG’s enforcement plan will go a long way to avoiding risk with your EMR.
References
- Adler-Milstein J, Daniel G, Grossmann C, et al. Return on Information: A Standard Model for Assessing Institutional Return on Electronic Health Records. January 6, 2014: Institute of Medicine.
- Gregg H. Beyond the EHR: Sentara Healthcare’s IT Strategy. Becker’s Hospital Review, November 15, 2013.
- Hill RG Jr, et al. 4000 clicks: A productivity analysis of electronic medical records in a community hospital ED. Am J Emerg Med. 2013;31(11):1591-1594.
- Poissant L, et al. The impact of electronic health records on time efficiency of physicians and nurses: A systmatic review. J Am Med Inform. 2005;12:505-516.
- Park SY, et al. The effects of EMR deployment on doctors’ work practices: A qualitative study in the emergency department of a teaching hospital. Int J Med Inform. 2012;81(3):204-217.
- Brotzman GL, et al. Implementing an electronic medical record at a residency site: Physicians’ perceived effects on quality of care, documentation, and productivity. WMJ. 2009;108(2):99-103.
- Ward MJ, et al. The effect of electronic health record implementation on community emergency department operational measures of performance. Ann Emerg Med. 13 January 2014.
- Stafford J. Can Scribes Help Improve Emergency Practice Productivity. Becker’s Hospital Review, April 19, 2012.
- The Use of Scribes: An Information Paper. The American College of Emergency Physicians, June 2011.
- Crane M. Malpractice Risks with NPs and PAs in Your Practice. Medscape Business of Medicine. January 3, 2013.
- FAQs, regarding scribes, published by The Joint Commission on July 12, 2012.
- Levinson DR. Coding Trends of Medicare Evaluation and Management Services: Department of Health and Human Services, Office of Inspector General, May 2012, OEI-04-10-00180.
- Pitts SR. Higher-complexity ED billing codes — sicker patients, more intensive practice, or improper payments? N Engl J Med. 2012;367:26.
- CMS and Its Contractors Have Adopted Few Program Integrity Practices to Address Vulnerabilities in EHRs: Daniel R. Levinson Inspector General January 2014 OEI-01-11-00571.
- Mangalmurti SS, et al. Medical malpractice liability in the age of electronic health records. N Engl J Med. 2010;363:21.
- Gallegos A. Legal risks of going paperless: Electronic medical records are meant to save time and money, but they also can create liability issues for doctors. Amednews.com, Posted March 5, 2012.
- Kane L, MA. Malpractice Discovery’ Dangers in Your HER. Medscape Business of Medicine. July 16, 2012.
- Farley HL, et al. Quality and safety implications of emergency department information systems. Ann Emerg Med. 2013;62:399-407.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
