Improving Adherence: Who's Doing the Work?
January 1, 2014
Reprints
Authors:
Dean A. Bricker, MD, Associate Professor, Department of Internal Medicine, Boonshoft School of Medicine, Wright State University, Dayton, OH
Paul J. Hershberger, PhD, Professor, Department of Family Medicine, Boonshoft School of Medicine, Wright State University, Dayton, OH
Peer Reviewer:
Robert B. Taylor, MD, Professor Emeritus, Oregon Health & Science University, Portland, OR
Executive Summary
- Approximately 50% of patients with chronic illnesses are not adherent to indicated medications, treatment regimens, and healthy lifestyle changes, which can lead to increased morbidity, excess mortality, and tremendous cost.
- Nonadherence is a challenging problem for clinicians because of the myriad barriers that may contribute and the many complexities of human behavior involved.
- Barriers to adherence can be patient-related, physician-related, and system- or health team-related.
- Physicians should be aware that adherence in one behavioral realm does not mean that a patient is adherent to other aspects of a treatment regimen.
- Motivational interviewing is a one approach to improve adherence in individuals struggling with behavior change.
- Reflective statements can be used to emphasize content, emotion, both sides of the discrepancy, or an alternative way to frame what the patient has said.
- Behavioral research demonstrates that patient motivation is a dynamic state that is influenced by the interviewer's style.
Nonadherence to indicated medications, treatment regimens, and healthy lifestyle changes is both common and costly.1,2 Average medication adherence rates among patients with chronic illnesses are only on the order of 50%.1,3 This poor adherence results in increased morbidity, excess mortality, and tremendous cost.2 Nonadherence is a contributing factor in at least 10% of all hospital admissions,4 and accounts for one- to two-thirds of all medication-related admissions. In the United States, poor adherence also may be responsible for 125,000 deaths annually (a number far exceeding the number of motor vehicle accident-related deaths) and may cost society in excess of $100 billion annually.1,2
Although still commonly used by many physicians, the term noncompliance may connote patient blame. The alternative terms adherence and nonadherence emphasize the patient's autonomy to follow or choose not to follow a physician's advice and are thus recommended by many experts studying this topic.1
Assessing adherence is difficult. For research purposes, the possibilities include a range of methods: history taking, written questionaires, pill counts, computer refill records, montoring therapeutic blood levels, assessing biomarkers, or using electronic pill dispensers.5,6,7 While there is no agreed-on gold standard, patients usually are considered adherent if they take at least 80% of their medication as prescribed. For example, if the number of pills absent in a given time period divided by the number of pills prescribed exceeds 80%, the patient is considered to be adherent.1 In day-to-day practice, the most common method of assessment is simply to ask about adherence during history taking. Not surprisingly, however, most patients overestimate their adherence and when asked, "Are you taking your medication?" will commonly report, "Yes." Simply asking patients if they have any problems taking their medications and assuming their response to be accurate may easily result in poor adherence not being discovered and consequently not being addressed.8,9
Epidemiology
Nonadherence to health care recommendations in general is ubiquitous; no person is perfectly adherent. Even among patients considered adherent to medications, it is assumed that some doses are missed or taken incorrectly. Primary nonadherence, defined as failing to fill an initial prescription, occurs with 20% or higher prevalence.10,11 Sustained adherence to many chronic medications, like statins and antiplatelet therapy, tends to wane with time, decreasing from 25-50% within 6 months to 1 year, down to as low as 25% by the end of 2 years after initiation.1,3,12 Regardless of the well-known benefits of lipid-lowering and diabetes medications, or those of antihypertensive medications, long-term adherence to these classes in particular is poor, even among patients who have already suffered events like myocardial infarction or stroke.1,3 Despite the prevalence and cost, nonadherence remains a challenging problem for clinicians, perhaps because of the myriad barriers that may contribute and the many complexities of human behavior involved in adherence.14 For example, even a patient with a single chronic illness must first receive a diagnosis, then seek and remain in care, acquire a drug, then consistently ingest or inject the medication. Furthermore,
most providers are not formally trained to look for and specifically address nonadherence.
Etiology
Numerous factors contribute to poor medication adherence, ranging from the practical to the predominantly psychological.15 Table 1 lists a number of adherence factors. It is helpful for clinicians to appreciate that not all barriers are patient-related, but many are physician-related and system- or health team-related. Regarding patient-related factors, poor understanding of disease processes, suboptimal understanding of medications, or general low health literacy may contribute. In the United States, approximately 90 million adults have inadequate health literacy. This difficulty reading and understanding medical terminology contributes to increased hospital admissions and poorer health outcomes.1 Other patient-related factors may include low self-efficacy (not believing one has the ability to perform the target behavior),16 or simply the challenge of remembering to take medications (the most commonly reported reason for nonadherence). Personal health care beliefs are yet another patient-related factor to consider. For instance, some patients prefer herbal or "natural" remedies to medications but may be reluctant to share that information with their physician unless questioned specifically about that.14 Some important medication-related factors that affect adherence include cost, complexity of medication regimens, and medication side effects.
Table 1: Factors that Can Influence Adherence
with Medical Regimens
Adherence Factors
- Cost of medication
- Health insurance
- Complexity (dosing frequency, injections, etc.)
- Accessibility (transportation, etc.)
- Health literacy (ability to read/understand health or medication information)
- Beliefs (perceptions of risks, benefits, self-efficacy)
- Understanding of health problems or diagnosis
- Knowledge about prescribed medications
- Memory (remembering to take the medication)
- Side effects
Suboptimal rapport with patients as well as insufficient or ineffective communication are common physician-related barriers to satisfactory adherence.1,17 Attentive physicians should consider how complexity (tid medications, injections, etc.), cost, and side effects (for example, erectile dysfunction from antihypertensives) may be affecting adherence, even though patients often may not readily volunteer such information. In addition, failing to suspect incomplete adherence or to inquire about that possibility in a non-threatening, open-ended manner may leave poor adherence undiscovered, unaddressed, and unimproved.
Health care system factors also may contribute to suboptimal adherence. Time constraints, imperfect patient handoffs, and frequent transitions of care all continue to hamper ideal communication.1
Clinical Features
When therapy for a chronic illness is not achieving the desired results, inadequate medication adherence should be high on the differential diagnosis. Consider the common office scenario of a hypertensive patient already prescribed three or even four medications, but who returns to the office with poorly controlled blood pressure. While a long list of causes — ranging from refractory essential hypertension to uncommon secondary causes (e.g. pheochromocytoma) — may be considered, the more likely instance of medication nonadherence should first be entertained. Without accurate information about what patients are actually doing with their medications, physicians may make poor treatment decisions like unnecessary increases in doses or adding new medications.18 Prescribing a fourth oral diabetic medication will not likely result in good glucose control for a patient who already has adherence problems.16,19 Polypharmacy itself contributes to poor adherence. Similarly, a common mistake made by physicians with respect to patient adherence is to assume that adherence in one behavioral realm means that the patient is adherent to other aspects of a treatment regimen. For example, diet planning, exercise, home glucose monitoring, appointment keeping, medication acquisition, pill taking, and insulin injecting may all be planned elements of a patient's diabetes management. A given patient may have excellent adherence to some elements, but poor or no adherence to others. Adherence in one area is not necessarily predictive of adherence in another area.20 Each aspect of a treatment regimen or recommended lifestyle change contains its own set of behaviors and challenges.
Solutions
Adherence is not a single construct, but rather a number of complex behaviors. For instance, a yearly adherence schedule for a patient with diabetes, hypertension, and hyperlipidemia taking several medications may add up to thousands of individual actions, especially when considering self-monitoring of blood glucose and blood pressure readings together with other prescribed dietary and exercise regimens.20 Perhaps it should not be surprising then that no one simple intervention and relatively few complex ones have been found to be effective in improving chronic adherence and health outcomes, according to a Cochrane review of 78 randomized trials.21,22,23 Some examples of complex interventions showing modest improvement in adherence include intense interdisciplinary assessment coupled with case management — or telephone, mail, and video education with behavioral counseling support.20 While the role of electronic reminders and smartphone adherence apps may still be evolving,23 focusing on the patient-physician relationship plays a pivotal role in providing the best chronic care and optimal support of medication adherence. Improving medication adherence is challenging but physicians can take several steps to assist patients' medication-taking behavior.
It is very easy and perhaps natural for physicians to believe that providing patients with more information (i.e., educating them) will lead to improved adherence. However, what proportion of smokers does not know the risks of smoking? Or, what proportion of patients for whom medications have been prescribed do not know why those medications have been prescribed? While knowledge about healthful behaviors is necessary for patients, information itself is insufficient. In many cases, if not most, patients already know what they need to do to be healthier, or to better manage their chronic illnesses. Therefore, patients may feel some defensiveness and annoyance when a physician again reiterates something they already know about a needed change in health behavior. Debating with patients or telling them what they should do tends to be ineffective and frustrating, both for the patient and the physician. There is an alternative approach.
Motivational interviewing (MI) has become a widely used approach to individuals struggling with behavior change in a wide array of domains.24 Adherence to any treatment regimen (including medication-taking) or health promotion endeavors involves behavior change that needs to be sustained. Motivational interviewing, therefore, is clearly applicable to addressing adherence, including barriers to adherence.
The emphasis in motivational interviewing is guiding patients to resolve ambivalence they have about behavior change. A motivational interviewing conversation with a patient is collaborative (rather than confrontive), evokes the patient's own thoughts/concerns/goals (rather than educating the patient), and stresses patient autonomy (rather than physician authority). See Table 2 describing the "Spirit of Motivational Interviewing." Undergirding this approach to patients are the following principles:
- Express empathy: seeing and understanding circumstances from the patient's perspective, and expressing this understanding through reflective statements.
- Support self-efficacy: highlighting patient skills and strengths, and calling attention to previous successes/achievements.
- Roll with resistance: avoiding confrontation and negative interaction with the patient by acknowledging/emphasizing patient autonomy and encouraging the patient to define her/his own goals/solutions.
- Develop discrepancy: bringing attention to mismatches between the patient's stated goals and current behavior.
Table 2: Key Features of Motivational Interviewing
Spirit of Motivational Interviewing
- Collaboration vs Confrontation
- Evocation vs Education
- Autonomy vs Authority
Principles of Motivational Interviewing
- Express Empathy
- Support Self-efficacy
- Roll with Resistance
- Develop Discrepancy
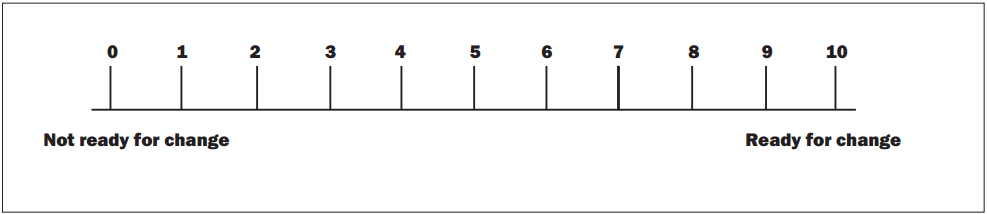
The following describes several of the important skills that are utilized with this approach to patients. Keep in mind that the skills are best implemented with the perspective that the patient is the expert on her/his behavior, that behavior change is the responsibility of the patient, that human behavior is affected by numerous factors, that behavior change takes time, and that ultimately the patient is the decision-maker. Behavior change and management represent work for the patient to do. The skills to be highlighted here are listening for ambivalence, open-ended questions, reflective statements, and the use of "change rulers." (1-10 scale, see Figure 1)
Figure 1: Change Ruler
Ambivalence is about the "buts." "I know I need to take this medication, but I cannot afford it." "I know I should quit smoking, but it helps me relax." "I know I need to lose weight, but I don't have time to cook healthy food." "I don't want to have to go on dialysis, but I just feel overwhelmed with all there is to do to contol my diabetes." Most patient-physician conversations will include the patient using a "but" with reference to her/his behavior. A motivational interviewing approach involves having the patient examine and talk about both sides of the "but."
Open-ended questions cannot be answered with a "yes" or "no." They often begin with: What, How, When, Who, Where, or Why (judicious use of "Why" is recommended as it can be experienced as judgmental in certain contexts or with certain tones/nonverbals). "Tell me about" can function as an open-ended question, even though gramatically it is not a question. Questions that begin with the following are closed questions (even if they are open-ended in spirit): Can you…, Do you…, Are you…, Is there…. Open-ended questions invite the patient to share her/his concerns, perspective, ideas, and goals. See Table 3 for examples of how common closed questions can be modified to be open ended.
Table 3: Changing Closed Questions to Open-ended Questions
Instead of asking ...
Are you taking your medications?
Do you know what medications you are taking?
Can you tell me more about…?
Have you discovered anything that makes it worse?
Is there anything that makes it better?
Ask ...
What difficulties are you having in taking all of your medications as prescribed? How many days a week would you say you are able to take your medications as prescribed?
What medications are you taking?
Tell me more about… (using a supportive tone of voice)
What makes it worse?
What makes it better?
Specifically with regard to medication adherence, the closed question, "Are you taking your medications?" is typically answered with a "yes." Patients perceive that this is the desired response to give, but it essentially yields useless information for the physician given the prevalence of medication nonadherence. Open-ended questions can facilitate collaborative discussion of a given patient's unique adherence challenges: "What difficulties do you have in taking your medications?" "On a scale of 0-10, with 0 indicating that you take none of your medications and 10 indicating that you always take all of your medications, where would you place yourself on the scale?" Such nonjudgmental questions invite the patient to acknowledge barriers to adherence and/or suboptimal adherence, which can lead to further conversation about identified challenges. To this point, on a recommended eight-item screening tool for medication adherence, the only open-ended question was the item found to have the strongest correlation to adherence.25
Perhaps even more important than open-ended questions is the use of reflective statements. A reflective statement is a comment that conveys understanding of what the patient has said. Reflective statements may emphasize content, emotion, both sides of the discrepancy, or an alternative way to frame what the patient has said. See Table 4 for examples of reflective statements.
Table 4: Examples of Reflective Statements
| Types of Reflection | Asking |
| Rephrasing | Patient: I just can't afford all these medications.Physician: So cost is a major barrier to taking your medications. |
| Empathic Reflection | Patient: I'm just not able to fall asleep.Physician: It sure can be frustrating to not be able to sleep. |
| Reframing | Patient: I've tried to lose weight many times but I just keep failing.Physician: You certainly have been persistent in trying to improve your health. |
| Double-Sided Reflection | Patient: I know I need to keep my blood pressure down but I just don't like having to use the bathroom so often.Physician: On the one hand, you understand the importance of taking this medication for your blood pressure, but on the other hand the side effects are quite disruptive for you. |
| Rolling with Resistance | Patient: You don't know what its like to have to take all of these medications.Physician: Since I'm not in your shoes, it is hard to imagine that I could understand how frustrating this is for you. |
Reflective statements serve several purposes. Conversationally, good reflective statements function like open-ended questions, inviting the patient to say more, provided that the physician is silent after making the statement. Silence invites further comment on the patient's part. "It sounds like you are bothered by potential side effects of your medications."…silence. Reflective statements are an excellent way to express empathy; good reflective statements can go a long way toward building the collaborative relationship. Reflecting the emotion associated with what the patient is saying is particularly important, as motivation is greater for matters about which the patient has strong feelings. An example of such a reflective statement is, "You seem worried about possibly needing dialysis in the future." The use of reflective statements requires careful listening on the part of the physician. For this reason, making good use of reflective statements is more difficult to do well than asking open-ended questions, because of the necessity of careful listening.
Use of the 1-10 scale for rating pain is now commonplace in medical settings. "Change Rulers," as 1-10 scales are named in motivational interviewing parlance, can be used for the patient to rate the perceived importance of a potential change or a desired goal, confidence in one's ability to make a change, or likelihood of implementing a change. The following is an example of a 1-10 scale question: "On a scale of 1 to 10, with 1 being not at all confident and 10 being 100% confident, how would you rate your current confidence about quitting smoking?"
After a patient has given a rating on a 1-10 scale, there are two other potentially fruitful questions that can be asked. To better understand what contributes to the patient's stated level of confidence, importance of a potential change, or readiness to implement change, one might ask: "How is it that you rate yourself a 5 with respect to your confidence in quitting smoking, rather than a 3 or 4?" To foster patient thought about what will help the patient move forward on the continuum of change, one might ask: "What would it take to move you from a 5 to a 6 or 7?"
While formal and intensive training in motivational interviewing is available (www.motivationalinterview.org), practicing physicians can certainly learn to modify their approach to patients and incorporate basic tenets of motivational interviewing without such formal training. While intensive training has its advantages, there is much room for behavior change by physicians in how they interact with patients that can be done informally. However, this does require much self-awareness, practice, and persistence. It should be emphasized that motivational interviewing is not a technique, but rather a different manner of interacting with patients that aims to elicit patient behavior change.26,27,28 A recent meta-analysis of randomized, controlled trials of motivational interviewing in primary care settings found significant effect sizes for studies addressing adherence, and that in some cases, one motivational interviewing encounter may effect change.29
Promoting Adherence in the Physician-Patient Encounter
One of the biggest challenges physicians have in addressing nonadherence is dealing with their own frustrations when advice to patients appears to be ignored or rejected. A common (natural) response is to educate more and with a more authoritative style. (After all, "doctor" is derived from the Latin word docere, meaning "to teach.") However, behavioral research demonstrates that patient motivation is a dynamic state that is influenced by the interviewer's style. An authoritative style may be counterproductive, increasing resistance and thereby hindering change.30 While patient understanding is necessary for behavioral change, knowledge alone is insufficient motivation for change. The savvy practitioner will elicit patient understanding first and educate sparingly, at the patient's request or with their permission: "What is your understanding about…? How might you find out more information on…? If it is OK with you, I could review…."31 Regarding treatment plans that involve a change in behavior (diet, exercise, medication adherence), a collaborative approach carries a greater likelihood of success ("What ideas do you have for ways to increase your physical activity?"). This approach emphasizes the patient doing the hard work of behavior change: Only the patient can truly change his/her own behavior (the provider cannot change them). Acknowledging and collaboratively working with the patient's autonomy not only increases the likelihood for improvements, it goes a long way for preventing provider bewilderment and burnout. This is a win-win approach.
Conclusion
Nonadherence to medications and other health advice is prevalent and costly. The issue is complex with contributing factors from patients, physicians, and health care systems. Although a number of interventions aimed at improving adherence have been studied, improvements are generally modest and no simple, single intervention has proven superior. The principles of motivational interviewing have increasingly been applied to the issue of nonadherence.31 To the extent that adhering to medications and healthy lifestyles involves behavior change, many of the tenants of motivational interviewing are applicable to addressing this problem. Clinicians do not need formal training to understand and begin to apply this patient-centered approach.29,32 The result may be more accurate assessment of suboptimal adherence and more collaborative approaches to improvements in adherence.
Only the patient can implement true change. Physicians who appreciate patient autonomy will go a long way in preventing provider burnout even when patient improvements are modest. The patient owns the hard work of change. Physicians have the lighter task: to guide, collaborate, and keep the ball in the patient's court.
References
- Brown MT, Bussell JK. Medication adherence: WHO cares? Mayo Clinic Proc 2011;86:304-314.
- Sokol MC, et al. Impact of medication adherence on hospitalization risk and healthcare cost. Med Care 2005;43:521-530.
- Dunlay SM, et al. Medication adherence among community-dwelling patients with heart failure. Mayo Clin Proc 2011;86:273-281.
- Viswanathan M, et al. Interventions to improve adherence to self-administered medications for chronic diseases in the United States: A systematic review. Ann Intern Med 2012;157:785-795.
- Garfield S, et al. Suitability of measures of self-reported medication adherence for routine clinical use: A systematic review BMC Med Res Methodol 2011;11:149.
- guyen TM, et al. What are validated self-report adherence scales really measuring? A systematic review. Br J Clin Pharmacol 2013 Jun 26. doi: 10.1111/bcp.12194.
- Omole FS, et al. Interacting with patients' family members during the office visit. Am Fam Physician 2011;84:780-784.
- Ose D, et al. Let's talk about medication: concordance in rating medication adherence among multimorbid patients and their general practitioners. Patient Prefer Adherence 2012;6:839-845.
- Wilson IB, et al. Physician-patient communication about prescription medication nonadherence: A 50-state study of America's seniors. J Gen Intern Med 2007;22:6-12.
- Karter AJ, et al. Primary non-adherence to prescribed medications. J Gen Intern Med 2010;25:763; author reply 765.
- Raebel MA, et al. Characteristics of patients with primary non-adherence to medications for hypertension, diabetes, and lipid disorders. J Gen Intern Med 2012;27:57-64.
- Epstein RS. Medication adherence: Hope for improvement? Mayo Clin Proc 2011;86:268-270.
- Ho PM, et al. Medication adherence: Its importance in cardiovascular outcomes. Circulation 2009;119:3028-3035.
- Rosenbaum L, Shrank WH. Taking our medicine — improving adherence in the accountability era. N Engl J Med 2013;369:694-695.
- Brunton SA. Improving medication adherence in chronic disease management. J Fam Pract 2011;60(4 Suppl Improving):S1-8.
- Rosenbek Minet LK, et al. The effect of motivational interviewing on glycemic control and perceived competence of diabetes self-management in patients with type 1 and type 2 diabetes mellitus after attending a group education program: A randomized controlled trial. Diabetologia 2011;54:1620-1629.
- Butterworth SW. Influencing patient adherence to treatment guidelines. J Manag Care Pharm 2008;14(6)(S-b):S21-S25.
- Velligan DI, Sajatovic M. Practical strategies for improving adherence to medication and outcomes. World Psychiatry 2013;12:233-234.
- Rubak S, et al. Effect of "motivational interviewing" on quality of care measures in screen detected type 2 diabetes patients: a one-year follow-up of an RCT, ADDITION Denmark. Scand J Prim Health Care 2011;29:92-98.
- Steiner JF. Rethinking adherence. Ann Intern Med 2012;157:580-585.
- Haynes RB, et al. Interventions for enhancing medication adherence. Cochrane Database Syst Rev 2008;(2):CD000011.
- Cutrona SL, et al. Targeting cardiovascular medication adherence interventions. J Am Pharm Assoc (2003) 2012;52:381-397.
- Vervloet M, et al. The effectiveness of interventions using electronic reminders to improve adherence to chronic medication: a systematic review of the literature. J Am Med Inform Assoc 2012;19:696-704.
- Miller WR, Rollnick S. Motivational Interviewing: Preparing People for Change (2nd ed.). New York, New York: The Guilford Press. 2002.
- Morisky DE, et al. Predictive validity of a medication adherence measure in an outpatient setting. J Clin Hypertens (Greenwich) 2008;10:348-354.
- Miller WR, Rollnick S. Ten things that motivational interviewing is not. Behavioural Cog Psychotherapy 2009:37;129-140.
- Rollnick S, et al. Motivational Interviewing in Health Care: Helping Patients Change Behavior. New York, New York: The Guilford Press. 2008.
- Rosengren DB. Building Motivational Interviewing Skills. New York: Guilford Press. 2009.
- VanBuskirk KA, Wetherell JL. Motivational interviewing with primary care populations: A systematic review and meta-analysis. J Behav Med 2013. (Published online 11 August 2013). DOI 10.1007/s10865-013-9527-4.
- Hall K, et al. Motivational interviewing techniques: facilitating behavior change in the general practice setting. Aust Fam Phys 2012;41:660-667.
- Lavoie KL, et al. Does motivational interviewing improve medication adherence? Arch Intern Med 2012;172:1351-1352; author reply 1351-1352.
- White LL, et al. Teaching students behavior change skills: Description and assessment of a new motivational interviewing curriculum. Med Teach 2007;29:e67-e71.
Approximately 50% of patients with chronic illnesses do not adhere to indicated medications, treatment regimens, and healthy lifestyle changes.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
