Massive Transfusion: Part I
March 9, 2014
Reprints
Massive Transfusion: Part I
This is a two-part article on the treatment of massive hemorrhage, which is something that can be seen in any emergency department, small or large, rural or urban. There have been recent changes in the use of blood and adjuvant therapies, in part from our military advances. These articles will review the current recommendations for massive transfusion. Part II of the article will review adjunct therapies, scoring systems, and complications of massive transfusion.
— Sandra M. Schneider, MD, Editor
Executive Summary
- After severe trauma with blood loss, the "lethal triad" of acidosis, coagulopathy, and hypothermia is associated with higher mortality. The goal of resuscitation is to prevent or reduce these factors.
- Traditional resuscitation with large amounts of crystalloid leads to worsening coagulopathy, acidosis, and blood loss. It is now recommended that the blood pressure be allowed to be as low as 90 systolic if the patient has a normal mental status.
- Hypothermia should be avoided and treated when present, as it shifts the oxygen hemoglobin dissociation curve and worsens coagulopathy.
Introduction
Patients with significant blood loss due to various etiologies, be it from trauma, ruptured ectopic pregnancy, or ruptured abdominal aortic aneurysm, are encountered in the emergency department (ED). Massive transfusion is defined as a transfusion requiring greater than 10 units of packed red blood cells (PRBCs) in a 24-hour period. Historically, massive transfusion research has come from the trauma data; however, hemorrhages as a result of gastrointestinal bleeding and obstetric and intraoperative emergencies are equally relevant. Although such subsets of patients require similar volumes of PRBCs, the need for other blood products may be variable.
Epidemiology
Traumatic injury continues to be the leading cause of death in people younger than the age of 40 worldwide.1 In fact, traumatic injury is a leading cause of mortality and accounts for approximately 10% of all deaths worldwide.2 Massive transfusion is only required in 1-2% of civilian trauma patients3 and in approximately 7% of patients in military settings.4 Yet, the mortality of patients who require massive transfusion ranges between 20% and 50%.5 Death from uncontrolled hemorrhage will typically occur within the first 6-12 hours following injury, and accounts for more than 50% of all trauma-related deaths that occur within the first 48 hours of hospital admission.6,7 As a result, hemorrhage necessitating transfusion of large amounts of blood products remains a major cause of potentially avoidable deaths.
Obstetric hemorrhage is the leading cause of maternal death worldwide and accounts for approximately 150,000 deaths annually.8 Obstetric hemorrhage has fallen from the first to the fifth leading cause of maternal death in the United States.9 Postpartum hemorrhage is among the most common causes of maternal hemorrhage, with the majority of these cases due to uterine atony.10
Massive Transfusion in Trauma
Traumatic injury requiring massive transfusion is associated with coagulopathy. This coagulopathy is multifactorial, resulting from initial tissue injury and dilution and consumption of clotting factors and platelets. Coagulopathy plus hypothermia and acidosis that occur in severe traumatic injury has been termed the "lethal triad" due to its high mortality. There is mounting evidence that treating early coagulopathy in trauma patients improves survival.
Traditional resuscitative efforts based upon aggressive fluid resuscitation with crystalloid to treat hypotension and tachycardia have fallen out of favor due to mounting evidence that they worsen coagulopathy, acidosis, and blood loss. Instead, the idea of damage control resuscitation has come into clinical practice. This concept revolves around the idea of rapid hemorrhage control through permissive hypotension, rapid correction of coagulopathy, acidosis, and hypothermia, in concurrence with damage control surgical techniques.
The Lethal Triad
A complex relationship exists between acidosis, hypothermia, and coagulopathy. Each factor compounds the other, leading to a worsening cycle and high mortality rate. (See Figure 1.) This cycle can be extremely difficult to break.
Figure 1: The Lethal Triad
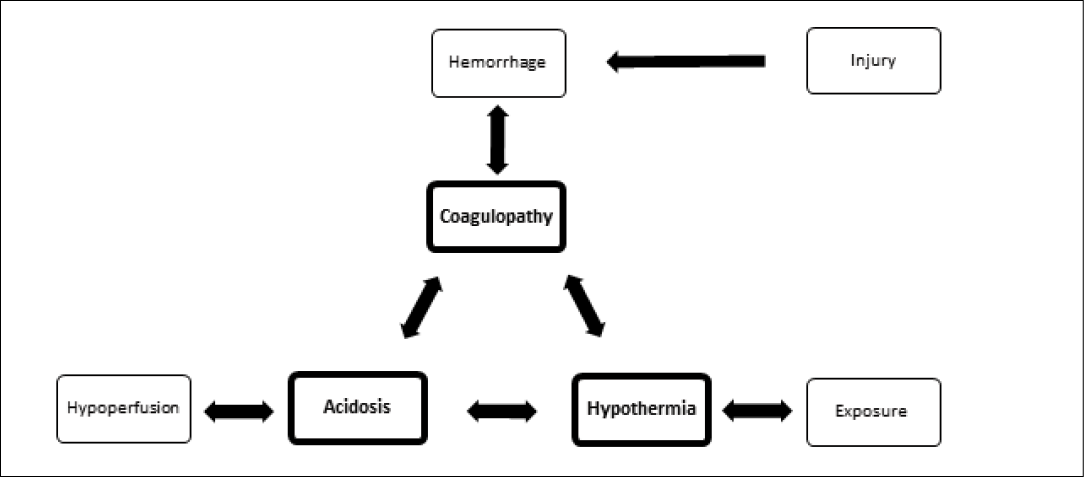
Coagulopathy
Traditional doctrine suggests that coagulopathy associated with trauma results from consumption of clotting factors, in addition to the dilutional effects of resuscitation fluid. We know that the injury itself causes exposure of tissue factor (TF), which consequently causes thrombin and fibrin generation. In its most extreme form, disseminated intravascular coagulation (DIC) occurs.11 It is also known that hyperfibrinolysis occurs after endothelial damage due to the effects of naturally released tissue plasminogen activator (tPA).
Previously, it was thought that dilution of clotting factors did not occur until at least one blood volume (defined as the volume of blood in the body) had been transfused.4 However, newer data suggest that significant acute traumatic coagulopathy is often present upon presentation to hospital, prior to any resuscitative efforts. A recent study demonstrated that significant coagulopathy exists in 20-30% of trauma patients upon presentation to the ED.4 This phenomenon has been referred to as acute traumatic coagulopathy or early trauma-induced coagulopathy (ETIC).
Early Trauma-induced Coagulopathy (ETIC)
Acute traumatic coagulopathy is a marker of injury severity and is related to mortality. Macleod et al found that elevated prothrombin time (PT) and activated partial thromboplastin time (aPTT) upon arrival are independent predictors of mortality.12 In fact, initial abnormal PT increases the odds ratio of dying by 35%, and initial abnormal aPTT increases the odds ratio of dying by 326%.12 Thus, initial coagulation screens are important early tests in severely injured patients.13
Although the mechanism behind acute traumatic coagulopathy is believed to be multifactorial and remains poorly understood, various mechanisms have been proposed. Some believe it to be a consequence of rapidly occurring consumptive coagulopathy, while others are less sure. An alternative theory infers that hypoperfusion results in expression of endothelial thrombomodulin, the activation of protein C, and resultant inhibition of the clotting cascade and activation of fibrinolysis.14
Regardless of mechanism, it is evident that this early coagulopathy of trauma is a clear prognostic indicator.
Hypothermia
Severe hemorrhage leads to hypoperfusion, resulting in decreased aerobic metabolism and reduced heat generation.15 It is also well documented that there is a loss of thermoregulation in severe traumatic injury. These factors, combined with the prolonged environmental exposure, are proven to be a deadly combination.
Hypothermia becomes clinically significant when body temperature drops to less than 36°C for more than 4 hours. It can result in cardiac arrhythmias, decreased cardiac output, increased systemic vascular resistance, left shift of the oxygen-hemoglobin dissociation curve, and worsening coagulopathy.15 Coagulopathy and temperature are directly proportional. At 33°C, clotting factor activity is at approximately 50% of normal. For every degree Celsius the temperature is decreased, a reduction of 10% in coagulation factor activity is observed.16 At 34°C, markedly reduced platelet function and increased fibrinolysis are observed. Severe trauma-related hypothermia (less than 32°C) is associated with 100% mortality.17
Acidosis
Anaerobic metabolism, due to prolonged hypoperfusion, results in lactate formation and subsequent metabolic acidosis. Acidosis decreases myocardial contractility and cardiac output. pH is inversely proportional to clot formation. In vitro studies have shown a substantially reduced clot formation rate, as detected by thromboelastography, in normal blood brought to pH of 7.18 This is also multifactorial, as pH affects clotting factor activity, in addition to platelet effectiveness. At a pH of 5.5, platelets form spheres that are devoid of aggregating tendency, whereas platelets at pH 9.0 form pseudopodia that increase aggregation properties.19
Damage Control Resuscitation
The historic practice of aggressive crystalloid resuscitation has been shown to dilute clotting factors, promote acidosis and intestinal edema, and impede microcirculation and tissue perfusion. The term damage control resuscitation was coined to convey strategies used to reverse anemia, coagulopathy, acidosis, and hypothermia in the initial 24-48 hours of injury.4
Damage control resuscitation is now defined as permissive hypotension, recognition and prevention of hypothermia, temporization of acidosis (or at least prevention of the worsening of acidosis), and immediate correction of coagulopathy. This can be achieved through the appropriate choice of resuscitation fluids and blood products, their ratios, timing of their administration, and the use of adjunct therapy.
Permissive Hypotension
The natural response to blood vessel injury and subsequent hemorrhage is an activation of clotting cascade and vessel spasm. Resultant hypotension from acute blood loss, in conjunction with the body’s natural response, can often temporarily arrest traumatic hemorrhage. This is, perhaps, best demonstrated with proximal limb amputation. Patients can present with no apparent bleeding from the traumatically amputated limb site only to have rapid arterial bleeding resume once resuscitation begins and hypotension is corrected.20
Current military guidelines stress minimizing the administration of fluid or blood products in the pre-hospital setting for those patients with a palpable radial pulse and normal mental status.21 This has been shown to prevent unnecessary blood loss in the field prior to obtaining surgical control.
Permissive hypotension is defined as allowing systolic blood pressure (SBP) to remain at approximately 90 mmHg when the patient has normal mental status. In the setting of traumatic brain injury, an SBP of 110 mmHg is accepted.
Recognition and Prevention of Hypothermia
Preventing unnecessary heat loss is paramount. Care must be taken to limit environmental exposure from the onset of injury. Simple steps, such as minimizing unnecessary skin exposure, removing wet clothing, and covering the patients with blankets, can make a significant difference. When fluids are administered, they should be warmed when possible. In severe hypothermia, active rewarming techniques should begin immediately.
Temporization of Acidosis
Reversal of acidosis in the severely injured patient is difficult. Treatment aimed toward its prevention, or at least its temporization, should be attempted. Achieving this goal is dependent upon rapid control of hemorrhage and the restoration of tissue perfusion. Current measures of acidosis are limited to serum lactate and base deficit, but the ability to improve these values has shown prognostic significance.22
Avoidance of interventions that worsen acidosis are equally, if not more, important. These include prevention of hypoventilation and its resultant respiratory acidosis, as well as limiting use of crystalloid fluids. Lactated Ringers solution has a pH of 6.0, whereas normal saline has a pH of 4.5. Acidosis is also worsened by PRBC transfusions. One study demonstrated that the pH of one unit of PRBCs dropped to 6.9 within 3 hours of initial banking and fell to 6.7 after 3 weeks of storage.23 The use vasopressors, certain procedures, such as aortic cross-clamping, as well as impaired myocardial performance have also been shown to worsen acidosis.15
Methods to temporarily reverse acidosis, such as bicarbonate or tris(hydroxymethyl)aminomethane, remain controversial, and alone are insufficient to reverse acidosis-induced coagulopathy.24
Correction of Coagulopathy
Correction of coagulopathy is a complex task. How best to approach this multifaceted issue is a matter of debate and is fundamental to the discussion of optimal transfusion protocols. It will be discussed at length in this paper. However, in order to understand how best to treat coagulopathy, one must first understand the complex mechanisms behind clot formation. This involves the interplay between the clotting cascade, platelets, and damaged endothelium.
As seen in Figure 2, the simplified clotting cascade is separated into the intrinsic and extrinsic pathways. These lead the common pathway by the activation of factor X. It is important to note that although they are separated for the sake of explanation, there is no clinical separation, as both occur simultaneously.
Figure 2: The Clotting Cascade
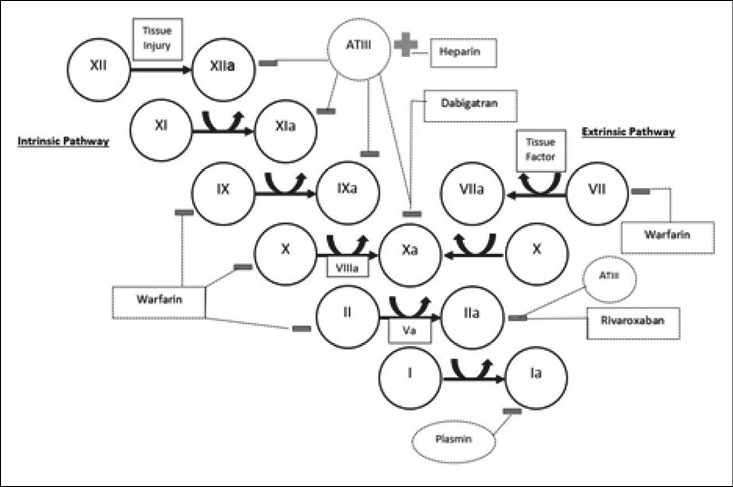
The intrinsic pathway, otherwise referred to as the contact activation pathway, is activated by damaged surface. Factor XII, or Hageman factor, is initiated. This triggers a cascade in which activated factor XII activates factor XI, which activates factor IX, which activates factor X with the assistance of cofactor VIIIa. (See Figure 2.)
The extrinsic pathway is also referred to as tissue factor pathway. Tissue injury results in the exposure of tissue factor, which binds to circulating factor VII. This results in the activation of factor VII, which, in turn, activates factor X.
The activation of factor X leads to the activation of the common pathway. With the assistance of cofactor Va, activated factor X activates factor II (prothrombin) to factor IIa (thrombin). Thrombin activates factor I (fibrinogen) into factor Ia (fibrin). Fibrin crosslinking with platelets gives a clot its strength. Depletion of any one clotting factor yields significantly less fibrin and, thus, significantly weaker clot.
The clotting cascade is regulated through a series of proteins. Plasmin is a naturally occurring protease that cleaves fibrin, thus breaking down clots. Protein C inactivates cofactors VIII and V, while antithrombin III (ATIII) is a protein that prevents the activation of factors XII, XI, IX, X, and II.
It is through the manipulation of these various regulating proteins that many of the anticoagulating drugs exert their activity. For instance, heparin and enoxaparin exert their mechanism of action by promoting the activity of ATIII. Warfarin prevents the synthesis of vitamin K-dependent factors (II, VII, IX, and X). Tissue plasminogen activator (tPA) acts by catalyzing the cleavage of plasminogen into plasmin and, thus, increases the concentration of circulating plasmin. The novel anticoagulants exert their action on specific factors and generally fall into two categories: direct thrombin inhibitors (such as rivaroxaban) and factor X inhibitors (such as dabigatran). (See Emergency Medicine Reports, September 24, 2012, "Newer Anticoagulants in the Emergency Department.")
Platelet activity is equally as important in hemostasis. Platelets must be activated to begin the process of clot formation. Under normal conditions, endothelial cells inhibit platelet activation through nitric oxide, endothelial ADPase, and prostaglandin I2. After endothelial injury, exposed collagen results in adhesion and subsequent activation of platelets via various surface glycoproteins. This activation leads to a confirmation change, degranulation, and thromboxane A2 (TxA2) synthesis. Degranulation releases various molecules, such as clotting factors, ADP, and calcium, into the surrounding bloodstream. ADP and TXA2 serve to further activate surrounding platelets. GIIb/IIIa on the surface of activated platelets serve as binding sites for fibrinogen and vWF, thus forming the crosslinks between neighboring platelets. Through the manipulation of this activation and aggregation, the various antiplatelet drugs exert their activity. Aspirin acts as an irreversible cyclooxygenase 1 (COX1) inhibitor and prevents the synthesis of TXA2. Clopidogrel irreversibly binds to surface protein P2Y12, reducing adhesion and aggregation. Eptifibatide and other drugs in its class bind the GIIb/IIIa receptor and prevent crosslinking.
Table 1: Blood Products and Their Components30
Blood Product |
Amount (mL) |
Components |
ABO Compatibility |
Rh Compatibility |
Shelf Life |
|
PRBCs |
330 |
Plasma: 30 mL Fibrinogen: < 100 mg Citrate: 3 grams |
Yes |
No* |
42 days |
|
Platelets (six pack) |
Fibrinogen: 48 mg Plasma: 240-360 mL (pooled); 200-400 mL (apheresis) |
No |
No |
5 days (4 hours once pooled) |
|
|
FWB |
500 |
HCT: 38-50% Plts: 150-400,000 Fibrinogen: 750-1000 mg Full coagulation function |
Yes |
Yes |
35 days |
|
FFP |
250 |
Normal coagulation factors at normal concentrations** Fibrinogen: 400 mg |
Yes |
No |
1 year frozen (5 days once thawed) |
|
1 unit PRBC 1 unit plts 1 unit FFP |
660 |
HCT: 29% Plts: 87,000 65% coagulation function Fibrinogen: 750 mg |
See above |
See above |
See above |
|
Cryo (one unit but usually transfused as 6 units) |
15 mL per unit |
Fibrinogen 250-350 mg/unit Factor VIII: 100 IU vWF Factor XIII |
Yes when possible |
1 year (24 hours once pooled) |
|
|
*Type O, Rh-negative PRBCs can be used for all patients but are reserved for pediatric and female patients of childbearing age. Type O, Rh-positive can be used for males or females over 50 years old. **Contains decreased levels of factors V (approximately 66% of normal) and VIII (approximately 41% of normal). |
|||||
Whole Blood and Component Blood Products
In 1840, 60 years prior to Karl Landsteiner’s discovery of ABO blood types, Samuel Armstrong Lane reported the first successful whole blood transfusion in London.25 For many years, without the ability of storage, transfusions were a direct procedure in which blood was directly transfused from the donor to the recipient. Richard Lewisohn discovered, through the use of sodium citrate as an anticoagulant, that donated blood had the potential for storage, thus revolutionizing the potential of transfusion medicine.25
In 1940, Edwin Cohn made a huge breakthrough in the field. While working as professor of biological chemistry at Harvard, he developed cold ethanol fractionation.25 This process of breaking plasma down into its components allowed for the revolution of component therapy. Ten years later, in one of the single most influential technical developments in blood banking, Carl Walter and W.P. Murphy Jr. introduced the plastic bag for blood collection. These new durable plastic bags led to the creation of a collecting system capable of the preparation of multiple blood components from a single unit of whole blood.
In 1960, A. Solomon and J.L. Fahey reported the first therapeutic plasmapheresis procedure, a process that rapidly separates whole blood into plasma and red blood cells. Similarly, in 1965, J. Pool and A. Shannon reported a method for producing cryoprecipitate, while in 1969, S. Murphy and F. Gardner demonstrated the ability to store platelets at room temperature.25 The era of component blood therapy had begun.
Fresh Whole Blood (FWB)
As its name suggests, fresh whole blood (FWB) consists of blood that has been drawn within 24 hours, but not separated into its components. One unit of FWB is approximately 500 mL, with a hematocrit ranging from 38-50%. It contains platelets in the range of 150,000-400,000/µL, with approximately 1500 mg fibrinogen and full coagulation function. In comparison, one unit PRBCs plus one unit FFP plus one unit of apheresis platelets contains approximately 660 mL, a hematocrit of 29%, platelets of 87,000/µL, 65% coagulation activity, and 750 mg fibrinogen.4
FWB has been used by the military for casualty resuscitation since World War I. In such settings, FWB is often the only source of blood available. Indications for use in civilian settings are limited today because of the ready availability of fractionated components and a relatively small body of data to support FWB.
A study performed on swine showed whole blood to be the best 24-hour hypotensive fluid after severe hemorrhage.26 Spinella et al found, in a retrospective review of combat casualties with hemorrhagic shock, that resuscitation strategies that include FWB may improve 30-day survival.27
However, FWB is currently not indicated for routine civilian use. FWB carries the risk of transmission of blood-borne diseases. Current military guidelines state that the use of FWB should be reserved for trauma victims who are anticipated to require massive transfusion, who have clinically significant shock or coagulopathy, and when optimal component therapy is unavailable or when stored component therapy is not adequately resuscitating a patient with immediate life-threatening injuries.28
Packed Red Blood Cells (PRBCs)
One unit of PRBCs contains approximately 200 mL RBCs, 100 mL of fluid, and, to extend shelf life, 30 mL plasma and 3 grams of citrate for anticoagulation.29 Once packed, PRBCs must be stored at 1-6°C and have a shelf-life of 42 days.31 As storage time increases, degradation occurs, and this results in an increase in inflammatory response to transfusion and an increase in sepsis, organ failure, and mortality.
All PRBC transfusions must be ABO/Rh compatible with the recipient. When time does not permit a type and cross match, type O Rh-negative PRBCs can be used for all patients. In general, this is reserved for pediatric and female patients of childbearing age. Type O, Rh-positive can be used for males or females older than 50 years old.30
In addition to their primary task of oxygen delivery, RBCs affect coagulation. At normal hematocrits, RBCs promote marginalization of platelets along the endothelium. They also support thrombin generation through membrane phospholipids. Further studies are required to determine the ultimate hematocrit goal in massive transfusion.
Platelets
Critical in achieving hemostasis, platelets are commonly available in two forms: pooled platelet units and apheresis platelet units. Both contain small amounts of plasma, RBCs, and leukocytes. Both types must be stored at room temperature and continuously agitated to prevent aggregation. In hemorrhaging patients, a goal of 50,000/µL is widely accepted.30
Pooled Platelet Units
Pooled platelet units are collected from separate random donors of the same ABO type and harvested by centrifuging FWB. The usual adult dose of pooled platelets is referred to as a "six pack" because it consists of platelets pooled from 6 units of FWB platelets. This contains approximately 360 mL of fluid. Once pooled, platelets have a four-hour life span.30
Apheresis Platelet Units
Apheresis platelet units are collected from a single donor and are equivalent to a six pack of pooled platelets. A unit contains 200-400 mL of fluid. Apheresis platelets also expire four hours after processing from a blood bank.30
Fresh Frozen Plasma (FFP)
A unit of FFP consists of plasma taken from one unit of FWB. This amounts to approximately 250 mL and contains normal coagulation factors at normal concentrations. It must be ABO compatible, but Rh is not a factor. Once isolated, it must be frozen within eight hours, as this vastly increases its shelf life. Once thawed, FFP has a maximum shelf life of five days. At this time, however, it contains decreased levels of factors V (approximately 66% of normal) and VIII (approximately 41% of normal).30
Dosing and timing of FFP administration remain controversial. Usually a 10% increase in factor level is required before any clinically significant improvement in coagulation status is observed. Under normal conditions, a dose of 10 mL/kg can achieve this goal. In a 70 kg adult, this amounts to four units of FFP.
Cryoprecipitate (Cryo)
Cryoprecipitate is prepared from plasma and contains high molecular weight plasma proteins, such as fibrinogen, von Willebrand factor, factor VIII, factor XIII, and fibronectin. Despite the recent development of recombinant fibrinogen, cryoprecipitate remains the primary source of fibrinogen. Fibrinogen is converted by thrombin into fibrin, which is essential in clot formation. Fibrinogen is the first coagulation factor to reach critically low levels (less than 1.0 g/L) during major hemorrhage (normal levels range from 2.0 to 4.5 g/L), and current guidelines recommend maintaining the plasma fibrinogen level above 1.5 g/L.31
Cryoprecipitate is available in pre-pooled concentrates of six units. Each unit is derived from a separate donor and suspended in 15 mL plasma prior to pooling. Because each unit provides about 350 mg of fibrinogen, the standard dose of six units contains 2.1 g fibrinogen. In comparison, one unit of FFP contains approximately 400 mg, a six pack of platelets contains approximately 48 mg, one unit of FWB contains approximately 1 g, and one unit of PRBCS contains less than 100 mg. Given only 75% recovery with transfusion, 6 units of cryoprecipitate will raise fibrinogen levels by 45 mg/dL in a 70 kg adult.31 Cryoprecipitate should be considered in patients with refractory coagulopathy after FFP or with a measured fibrinogen level lower than 100 mg/dL.32
In spite of the large concentration of fibrinogen in cryoprecipitate relative to other blood products, its utilization in the setting of massive transfusion is greatly varied. As part of the PROMMTT study, Holcomb et al examined the use of cryo in the setting of massive transfusion in 10 Level 1 trauma centers in the United States. They found that not only did the practice standards vary, but three of the sites did not have cryo in their massive transfusion protocol.33 Additionally, of the 98 patients who died within the first 24 hours of hospital admission, 67% never received cryo.33
Optimal Ratios for Blood Product Administration
The traditional, conservative blood product ratios were based on research and opinions derived from old, non-trauma literature. For instance, the plasma exchange transfusion study, cited by Ho et al, demonstrating that approximately one-third of clotting factors are still present after an entire blood volume has been exchanged, is based upon physiology under euvolemic conditions.34 Under rapidly hemorrhaging conditions, a different physiology exists.
It is important to note that all studies thus far addressing blood product ratios in both civilian and military trauma are retrospective, observational studies. Such studies are prone to survivor bias. Deaths occurring in early hospital stay are more likely to fall into the low ratio group, prior to receiving larger amounts of FFP or platelets.35 In addition, patients who have suffered more severe injuries are likely to receive relatively higher volumes of PRBCs (thus a lower FFP:PRBC ratio) and are more likely to die.36
FFP: PRBC Ratio
Ho et al, in a mathematical simulation, presented the first indication of these requirements. They hypothesized that in stable patients who are not severely injured, transfusions maintaining one unit FFP per 4-10 units of RBC may still be adequate. However, in those patients with the loss of one blood volume in a relatively short period, PT/aPTT greater than or equal to 1.5 times the control, injury severity scale (ISS) greater than 30, or unabated hemorrhage, then RBC to FFP ratio approaching that of FWB (i.e., 1:1) should be administered with little or no crystalloid.37
The first major study regarding damage control resuscitation looked at retrospective data from Operation Iraqi Freedom. Borgman et al reviewed data on 252 patients who had received massive transfusions and found a distinct decrease in mortality between patients receiving high plasma to red blood cell ratios compared to those who did not. It demonstrated that the higher the plasma ratio in the transfused blood (approaching 1:1), the lower the risk of mortality.5
In a review of the national trauma database, Gonzalez et al came to similar conclusions. They found that there was inadequate treatment of coagulopathy with their transfusion protocol and noticed an increased survival rate among those who received higher FFP:PRBC ratios.38
Holcomb et al described similar results in a larger retrospective civilian study. They reviewed results in 466 civilian patients transported to 16 different Level 1 trauma centers in the United States. Thirty-day survival was significantly increased in patients with higher FFP: PRBC ratios (greater than 1:2) relative to those with ratios less than 1:2 (59.6% compared to 40.4%). They also showed that high FFP:PRBC ratios (greater than 1:2) increased six-hour and 24-hour survival, with no change in multi-organ failure.39
Platelet: PRBC
In the same study, patients receiving high platelet:PRBC ratios (greater than 1:2) relative to those receiving low ratios (less than 1:2) had better 30-day survival (59.9% compared to 40.1%).39 In another study, patients who received approximately 1:1 platelets:PRBCs had improved 24-hour and 30-day survival rates compared to other groups.40 Holcomb et al queried a transfusion database of patients from 22 Level 1 trauma centers over 12 months. To mitigate survival bias, patients who died within 60 minutes of arrival were excluded from analysis. Outcome data associated with the low (greater than 1:2), medium (1:2), and high (1:1) platelet:PRBC ratios were reported. Similar to previously published data, transfusion of platelet:RBC ratios of 1:1 was associated with improved early and late survival and decreased hemorrhagic death. They concluded, based on this data, that increased and early use of platelets may be justified, pending the results of prospective randomized transfusion data.41
As the name suggests, the Prospective, Observational, Multicenter, Major Trauma Transfusion (PROMMTT) study group conducted a prospective cohort study of severely injured patients who required blood transfusion in 10 Level 1 trauma centers. A total of 1,245 patients were enrolled, with 297 patients receiving massive transfusion.42 They found that higher plasma and platelet ratios early in resuscitation were associated with decreased mortality in patients who received transfusions of at least three units of blood products during the first 24 hours after admission.43
Fibrinogen: PRBC
It had been suggested that early use of cryoprecipitate as a source of fibrinogen may also affect survival. In a retrospective chart review of 252 patients who received massive transfusion, the transfusion of fluids with increased fibrinogen:PRBC ratio was independently associated with improved survival.44 The authors suggested that by transfusing 200 mg of fibrinogen per unit of PRBCs, they could achieve this survival benefit. This level of fibrinogen could be achieved by transfusing either one unit of FFP per two units PRBC, one unit of FWB per four units of PRBC, or one 10-unit cryoprecipitate per 10 units of PRBC.
Massive Transfusion Protocol (MTP)
The potential for improvement in mortality has led many hospitals to implement MTPs.45 Cotton et al published outcome data after instituting an MTP. Their Trauma Exsanguination Protocol (TEP) transfused a ratio of 10 units PRBC:4 units FFP:2 units platelets. The protocol demonstrated lower 30-day mortality, decreased blood product usage, and decreased incidence of pneumonia, respiratory failure, abdominal compartment syndrome, sepsis, and multi organ failure when compared to pre-protocol data.46
O’Keefe et al also published results after the institution of an MTP. In their protocol, 5 units PRBCs: 2 units FFP were followed by one unit of platelets. A further 5 units PRBCs:2 units FFP ratio was followed by a 10 pack of cryoprecipitate and rFVIIa. The cycle was then started again. This study saw no change in overall mortality, but it did show a decrease in time to receive products, a decrease in use of products, and decreased cost (an average saving of $2,270 per patient).47
MTP protocols currently vary among different institutions. Once activated, blood products in predetermined ratios will be delivered until the protocol is deactivated. Such protocols allow for more expeditious product availability, resulting in significant decrease in time to first transfusion of PRBCs, FFP, and platelets. To achieve quick blood product administration, thawed AB plasma is stored alongside emergency release type O blood within the ED.
A review of literature by Neal et al suggests that although the optimal ratio remains inconclusive, observational studies have consistently found ratios of PRBC:FFP and PRBC:platelets greater than 1:2 and approaching 1:1 show improved survival.32 The American Association of Blood Banks currently does not provide a recommendation for or against higher ratios of FFP and platelets to PRBCs, because of the lack of randomized controlled studies.32 The current U.S. military resuscitation guidelines advocate the use of ratios of 1 unit PRBC:1 unit FFP:1 unit of platelets. Many civilian MTPs are now moving toward the same protocol.48
The first multi-center randomized, controlled trial to compare blood ratios in trauma is currently underway. The PROPPR (Prospective Randomized Optimum Platelet and Plasma Ratios, ClinicalTrials.gov Identifier: NCT01545232) trial will randomize patients to either 1:1:1 or 1:1:2 (platelets:plasma:RBCs).49
Other Considerations
MTP has been applied to non-traumatic hemorrhage despite a lack of evidence of benefit in this population.50 In a retrospective cohort study, blood product administration before and after MTP implementation was reviewed. No statistically significant difference in in-hospital mortality was observed in non-trauma patients. They concluded that further studies of non-trauma patients receiving MTP are warranted to ensure benefit in these patients.50
As previously mentioned, obstetric hemorrhage is a chief cause of maternal morbidity and mortality. Coagulopathy can develop rapidly in severe obstetric hemorrhage. Although treatment protocols from trauma patients are applied to obstetric hemorrhage management, distinct differences exist between the two situations.51 They suggest that, until efficacy and safety are demonstrated in obstetric hemorrhage, clinicians should be cautious about wholesale adoption of high FFP: RBC ratio MTP in this subset of patients.51 However, Gutierrez et al noted that MTP activation occurred for 31 patients: 19 with cesarean delivery, 10 with vaginal delivery, and two during dilation and evacuation. Favorable hematologic indices were observed post-MTP resuscitation (mean hemoglobin 10.3 g/dL, platelet count 126,000, and fibrinogen 325 (125) mg/dL). They concluded that although further outcome-based studies are required in this obstetric population, current MTP provides quicker access to blood products.52
Until the literature proves otherwise, the California Maternal Quality Care Collaborative (CMQCC) in their obstetric hemorrhage care guidelines and compendium of best practices recommends using a ratio of PRBCs:FFP:platelets that is 6 units PRBC:4 units FFP:1 unit apheresis platelets. If bleeding continues after initial treatment, strong consideration should be given to increasing the amount of FFP to a ratio of 4 units PRBC:4 units of FFP:1 unit of apheresis platelets.53 These guidelines are currently being updated for 2013.
References
- Krug EG, Sharma GK, Lozano R. The global burden of injuries. Am J Public Health 2000;90:523-526.
- Murray CJ, Lopez AD. Mortality by cause for eight regions of the world: Global Burden of Disease Study. Lancet 1997;349:1269-1276.
- Como JJ, Dutton RP, Scalea TM, et al. Blood transfusion rates in the care of acute trauma. Transfusion 2004;44:809-813.
- Beekley AC. Damage control resuscitation: A sensible approach to the exsanguinating surgical patient. Crit Care Med 2008;36:S267-S274.
- Borgman MA, Spinella PC, Perkins JG, et al. The ratio of blood products transfused affects mortality in patients receiving massive transfusions at a combat support hospital.
J Trauma 2007;63:805-813. - Maegele M, Brockamp T, Nienaber U, et al. Predictive models and algorithms for the need of transfusion including massive transfusion in severely injured patients. Transfus Med Hemother 2012;39:85-97.
- Sauaia A, Moore FA, Moore EE, et al. Epidemiology of trauma deaths: A reassessment. J Trauma 1995;38:185-193.
- James AH, Paglia MJ, Gernsheimer T, et al. Blood component therapy in postpartum hemorrhage. Transfusion 2009;49:2430-2433.
- Berg CJ, Chang J, Callaghan WM, et al. Pregnancy-related mortality in the United States, 1991-1997. Obstetrics and Gynecology 2003;101:289-296.
- Callaghan WM, Kuklina EV, Berg CJ. Trends in postpartum hemorrhage: United States, 1994-2006. Am J Obstet Gynecol 2010;202:353 e1-6.
- Gando S. Disseminated intravascular coagulation in trauma patients. Semin Thrombosis Hemostasis 2001;27:
585-592. - MacLeod JB, Lynn M, McKenney MG, et al. Early coagulopathy predicts mortality in trauma. J Trauma 2003;55:39-44.
- Brohi K, Singh J, Heron M, et al. Acute traumatic coagulopathy.
J Trauma 2003;54:1127-1130. - Brohi K, Cohen MJ, Ganter MT, et al. Acute coagulopathy of trauma: Hypoperfusion induces systemic anticoagulation and hyperfibrinolysis.
J Trauma 2008;64:1211-1217; discussion 7. - Mohr AM AJ, García-Núñez LM, Petrone P, et al. Guidelines for the institution of damage control in trauma patients. Trauma Care 2005;15:185-188.
- Kettner SC, Kozek SA, Groetzner JP, et al. Effects of hypothermia on thromboelastography in patients undergoing cardiopulmonary bypass. Br J Anaesthesia 1998;80:313-317.
- Jurkovich GJ, Greiser WB, Luterman A, et al. Hypothermia in trauma victims: An ominous predictor of survival. J Trauma 1987;27:1019-1024.
- Engstrom M, Schott U, Romner B, et al. Acidosis impairs the coagulation: A thromboelastographic study. J Trauma 2006;61:624-68.
- Djaldetti M, Fishman P, Bessler H, et al. pH-induced platelet ultrastructural alterations. A possible mechanism for impaired platelet aggregation. Arch Surg (Chicago, Ill : 1960) 1979;114:707-710.
- Beekley AC, Starnes BW, Sebesta JA. Lessons learned from modern military surgery. Surgical Clin North Am 2007;87:157-184, vii.
- Rhee P, Koustova E, Alam HB. Searching for the optimal resuscitation method: Recommendations for the initial fluid resuscitation of combat casualties. J Trauma 2003;54:S52-S62.
- Elliott DC. An evaluation of the end points of resuscitation. J Am Coll Surg 1998;187:536-547.
- Bennett-Guerrero E, Veldman TH, Doctor A, et al. Evolution of adverse changes in stored RBCs. Proc National Acad Sciences of the United States 2007;104:17063-17068.
- Weil MH, Tang W. Management of acidosis: The role of buffer agents. Critical Care (London, England) 1997;1:51-52.
- Highlights of Transfusion Medicine History. Accessed at http://www.aabb.org/resources/bct/Pages/highlights.aspx.
- Sondeen JLW, Dubick MA, Prince MD, et al. Fresh whole blood is the best 24-h hypotensive resuscitative fluid in severe hemorrhage in swine. [Abstract]. Shock 2006;25:21.
- Spinella PC, Perkins JG, Grathwohl KW, et al. Warm fresh whole blood is independently associated with improved survival for patients with combat-related traumatic injuries.
J Trauma 2009;66:S69-S76. - Joint Theater Trauma System Clinical Practice Guideline: Fresh Whole Blood (FWB) Transfusion. 2012. Accessed at http://www.usaisr.amedd.army.mil/assets/cpgs/Fresh_Whole_Blood_Transfusion_24_Oct_12.pdf.
- Guidelines for Transfusion for Massive Blood Loss. A publication of the British Society for Haematology. British Committee for Standardization in Haematology Blood Transfusion Task Force. Clinical and Laboratory Haematology 1988;10:265-273.
- Blood Component Therapy 2012. 2012. Accessed January 25, 2014, at http://www.psbc.org/therapy/therapy2012.pdf.
- Levy JH, Welsby I, Goodnough LT. Fibrinogen as a therapeutic target for bleeding: A review of critical levels and replacement therapy. Transfusion 2013; Oct. 9 [Epub ahead of print].
- Neal MD, Marsh A, Marino R, et al. Massive transfusion: An evidence-based review of recent developments. Arch Surg (Chicago, Ill : 1960) 2012;147:563-571.
- Holcomb JB, Fox EE, Zhang X, et al. Cryoprecipitate use in the PROMMTT study. J Trauma Acute Care Surg 2013;75:S31-S39.
- Ho AM, Karmakar MK, Dion PW. Are we giving enough coagulation factors during major trauma resuscitation? Am J Surg 2005;190:
479-484. - Ho AM, Dion PW, Yeung JH, et al. Prevalence of survivor bias in observational studies on fresh frozen plasma:erythrocyte ratios in trauma requiring massive transfusion. Anesthesiology 2012;116:716-728.
- Sharpe JP, Weinberg JA, Magnotti LJ, et al. Accounting for differences in transfusion volume: Are all massive transfusions created equal? J Trauma Acute Care Surgery 2012;72:
1536-1540. - Ho AM, Dion PW, Cheng CA, et al. A mathematical model for fresh frozen plasma transfusion strategies during major trauma resuscitation with ongoing hemorrhage. Can J Surg 2005;48:470-478.
- Gonzalez EA, Moore FA, Holcomb JB, et al. Fresh frozen plasma should be given earlier to patients requiring massive transfusion. J Trauma 2007;62:112-119.
- Holcomb JB, Wade CE, Michalek JE, et al. Increased plasma and platelet to red blood cell ratios improves outcome in 466 massively transfused civilian trauma patients. Ann Surg 2008;248:447-458.
- Perkins JG, Cap AP, Spinella PC, et al. An evaluation of the impact of apheresis platelets used in the setting of massively transfused trauma patients. J Trauma 2009;66:S77-S84; discussion S-85.
- Holcomb JB, Zarzabal LA, Michalek JE, et al. Increased platelet:RBC ratios are associated with improved survival after massive transfusion.
J Trauma 2011;71:S318-S328. - Callcut RA, Cotton BA, Muskat P, et al. Defining when to initiate massive transfusion: A validation study of individual massive transfusion triggers in PROMMTT patients. J Trauma Acute Care Surgery 2013;74:59-65, 7-8; discussion 6-7.
- Holcomb JB, del Junco DJ, Fox EE, et al. The prospective, observational, multicenter, major trauma transfusion (PROMMTT) study: Comparative effectiveness of a time-varying treatment with competing risks. JAMA Surgery 2013;148:127-136.
- Stinger HK, Spinella PC, Perkins JG, et al. The ratio of fibrinogen to red cells transfused affects survival in casualties receiving massive transfusions at an army combat support hospital. J Trauma 2008;64:S79-S85; discussion S.
- Schuster KM, Davis KA, Lui FY, et al. The status of massive transfusion protocols in United States trauma centers: Massive transfusion or massive confusion? Transfusion 2010;50:1545-1551.
- Cotton BA, Gunter OL, Isbell J, et al. Damage control hematology: The impact of a trauma exsanguination protocol on survival and blood product utilization. J Trauma 2008;64:1177-1182; discussion 1182-1183.
- O’Keeffe T, Refaai M, Tchorz K, et al. A massive transfusion protocol to decrease blood component use and costs. Arch Surg (Chicago, Ill : 1960) 2008;143:686-690; discussion 690-691.
- Joint Theater Trauma System Clinical Practice Guideline: Damage control resuscitation at level IIb/III treatment facilities. 2013. Accessed January 25, 2014, at http://www.usaisr.amedd.army.mil/assets/cpgs/Damage Control Resuscitation - 1 Feb 2013.pdf.
- Miller TE. New evidence in trauma resuscitation — is 1:1:1 the answer? Perioper Med 2013;2:13.
- Baumann Kreuziger LM, Morton CT, Subramanian AT, et al. Not only in trauma patients: Hospital-wide implementation of a massive transfusion protocol. Transfus Med (Oxford, England) 2013; Dec. 26 [Epub ahead of print].
- Bonnet MP, Basso O. Prohemostatic interventions in obstetric hemorrhage. Semin Thrombosis and Hemostasis 2012;38:259-264.
- Gutierrez MC, Goodnough LT, Druzin M, et al. Postpartum hemorrhage treated with a massive transfusion protocol at a tertiary obstetric center: A retrospective study. International J Obstetric Anesthesia 2012;21:230-235.
- Lyndon A, Lagrew D, Shields L, Melsop K, Bingham B, Main E, eds. Improving Health Care Response to Obstetric Hemorrhage. (California Maternal Quality Care Collaborative Toolkit to Transform Maternity Care) Developed under contract #08-85012 with the California Department of Public Health; Maternal, Child and Adolescent Health Division; Published by the California Maternal Quality Care Collaborative, July 2010. https://cmqcc.org/ob_hemorrhage. Accessed 2/24/14.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
