Tick-borne Illness in the ED: Part I
February 9, 2014
Reprints
Tick-borne Illness: Evaluation and Management in the Emergency Department: Part I
Authors:
Medley O'Keefe Gatewood, MD, Assistant Professor, Division of Emergency Medicine, University of Washington Medical Center, Harborview Medical Center, Seattle, WA.
Mitchell Kim, MD, Resident, Division of Emergency Medicine, University of Washington, Seattle.
Peer Reviewer:
Dan Quan, MD, Department of Emergency Medicine, Maricopa Medical Center, Phoenix, AZ.
Executive Summary
- Lyme disease is the most common vector disease. It often presents with erythema chronicum migrans in its earliest and most treatable stage. Systemic involvement, including carditis, neurological, and ocular, can occur soon after the tick bite. Later, arthritis and neuropsychiatric changes can occur.
- Patients with erythema chronicum migrans should be treated empirically without serologic testing. Patients who present within 72 hours of a tick bite should be treated prophylactically.
- Babesiosis is a tick-related illness seen more commonly in the Midwest. It causes hemolysis and the classic finding of "Maltese cross" formations within the red cells.
- Anaplasmosis is a bacterium that affects granulocytes and causes fever, chills, and altered mental status.
Introduction
Ticks are obligate, blood-feeding arthropods that are closely related to mites, spiders, and scorpions. There are 865 species of ticks worldwide, approximately 80 of which are endemic to the United States. The majority (approximately 700 species) belong to the family Ixodidae, also known as "hard ticks." Roughly 180 belong to the family Argasidae ("soft ticks"), and one species, only found in Africa, belongs to the family Nuttalliellidae.1,2
Ticks are an important vector for arthropod-borne disease throughout the world. Their disease burden ranges from local inflammation to fulminant systemic infection by transmitting viruses, bacteria, and/or parasites as they feed on the unsuspecting person. As one tick may transmit multiple microbial pathogens, there is the potential for significant morbidity and mortality related to a single exposure. It is now widely known that ticks are the source of multiple diseases throughout the United States.2
The life cycle of a tick begins when a larva hatches from the egg. The larva, once large enough, will attach to a host to feed. It then molts into a nymph. The nymph attaches, feeds, drops, and molts into an adult. The adult female tick will feed on its host, engorge, produce 1,000-18,000 eggs, and die. The transmission of diseases occurs during the days when the tick is attached to its host to feed.2
Simple techniques to prevent insect bites, including wearing long-sleeved clothing and using insect repellent, can help reduce the likelihood of tick attachment. Patients who live in locations endemic to ticks can be counseled to examine their skin for ticks following outdoor activities in grassy or forested areas. If found, the tick may be removed by using thin-tipped tweezers to grasp the tick as close as possible to the skin and pulling with steady pressure without using any twisting motion. The tick should be saved for future reference.2
Of the approximately 80 species of ticks in the United States, roughly 12 species are known to be of health or veterinary significance.2 The majority of these are hard ticks that belong to the family Ixodidae. This two-part review will discuss the major tick-borne illnesses seen in the United States. Diseases endemic to other countries, including Crimean-Congo hemorrhagic fever and Helvetica spotted fever, will not be discussed in this review.
Ixodes Scapularis
Ixodes scapularis (formerly also referred to as Ixodes dammini),3 more commonly referred to as the deer tick or the blacklegged tick (see Figure 1), is one of the most common species of ticks known to transmit disease in the United States. It is widely distributed in the northeastern, midwestern, and southern portions of the United States.4 (See Figure 2.)
|
Figure 1: Deer Tick 
The adult female deer tick is shown at the top of the image. To the left is the nymph, and to the right is its larval form. Source: US Centers for Disease Control and Prevention (CDC), Atlanta, GA. CDC Public Health Image Library. |
Figure 2: Distribution of the Blacklegged Tick, Ixodes scapularis 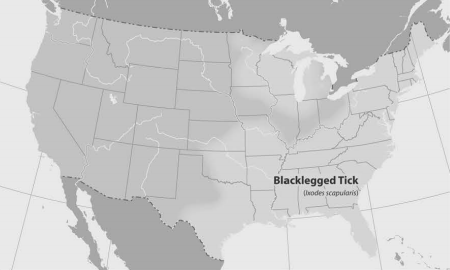
Source: US Centers for Disease Control and Prevention (CDC), Atlanta, GA. CDC Public Health Image Library. |
The distribution of Ixodes scapularis is closely related to the abundance of its primary host, the white-tailed deer. The population growth of the white-tailed deer in the northeastern United States in the 20th century allowed populations of deer ticks to thrive.3 An unintended consequence of this is the current high incidence of diseases carried by this tick.
Blacklegged ticks are characterized by being dark brown to black in color. They have no white markings. The adult forms exhibit sexual dimorphism, with female ticks having an orange-red area on the caudal aspect of their bodies. (See Figure 1.) The adult male tick feeds sparingly, and is a less significant contributor to disease. Due to their sheer number, small size, and coincident increased outdoor activity of people in the early summer, the blacklegged tick nymph carries the greatest disease burden.3
Lyme Disease
A 37-year-old man presents after a syncopal event. He felt palpitations prior to loss of consciousness for about 20 seconds. He was slightly confused after waking up. He relates having flu-like symptoms two weeks prior to his presentation. The patient last went on a hike one month ago. He is bradycardic, and the exam shows an erythematous rash on his posterior neck extending into his scalp. He has a third-degree heart block on EKG.
Introduction
The most widely recognized tick-borne infection is Lyme disease. In the 1970s, following a small epidemic of a mysterious inflammatory arthritis that occurred in children residing in and around Lyme, Connecticut, an association between Lyme disease and the spirochete Borrelia burgdorferi was made. (See Figure 3.)
Figure 3: Borrelia burgdorferi

The spirochetes of Borrelia burgdorferi, the causative agent of Lyme disease, visualized under dark field microscopy. Magnification x400.
Source: US Centers for Disease Control and Prevention (CDC), Atlanta, GA, USA. CDC Public Health Image Library.
Epidemiology
Lyme disease is the most commonly reported vector-borne disease in the United States, with 248,074 cases reported to the CDC between 1992 and 2006. It is also reported in Asian and European countries. Its incidence peaks in the midsummer months. The primary vector is Ixodes scapularis, especially in the eastern United States. However, Ixodes pacificus is the principal vector for Lyme disease in the western part of the country. Its incidence has steadily increased, with 9,908 cases in 1992 and 19,931 cases in 2006. The majority of cases are reported from the northeastern and north central states. It is reported more frequently in children between the ages of 5 years and 14 years of age, with no significant difference between genders.6
Clinical Presentation
The presentation for Lyme disease is variable during the course of illness. The dermatologic, neurologic, musculoskeletal, and cardiac systems may be involved. Its presentation is broadly categorized into three different stages: early localized, early disseminated, and late disseminated.
Early Localized. The earliest stage of Lyme disease in all populations is manifested by the characteristic skin lesion known as erythema chronicum migrans (ECM). ECM (see Figure 4) usually presents as a solitary lesion that occurs at the site of the tick bite three to 30 days following the bite. Most patients do not remember a tick bite, so the absence of a tick bite on the history does not exclude Lyme disease. ECM is characterized as a non-tender, erythematous, annular lesion that expands centrifugally, with partial central clearing that is greater than 5 cm at its widest point. This lesion should be differentiated from a lesion that can occur due to a localized allergic reaction near the site of the bite. The central aspect of this lesion may become vesicular or necrotic. It is important to note that a minority (about 20%) of infected patients may not exhibit ECM.7
Figure 4: Erythema Chronicum Migrans
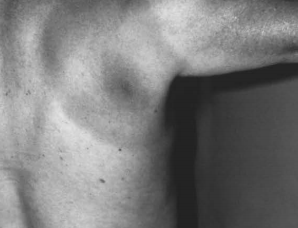
Erythema chronicum migrans, the characteristic rash of Lyme disease. Note the "bulls eye" appearance of this rash.
Source: US Centers for Disease Control and Prevention (CDC), Atlanta, GA, USA. CDC Public Health Image Library.
ECM does not always present classically. The lesion may be pruritic, tender, multiple in number, or without central clearing. Constitutional symptoms, including fatigue, arthralgia, myalgia, headaches, meningeal signs, fevers, and chills, may be present.8
Early Disseminated. Following the initial localized infection, the Borrelia spirochetes spread hematogenously throughout the body, leading to systemic, cardiac, neurological, ocular, and dermatological findings. Patients may present in this stage of Lyme disease without a history of localized ECM. In the weeks to months following the bite, patients exhibit severe nonspecific symptoms that resemble many other infectious, rheumatologic, or malignant diseases. Symptoms include fatigue, headache, myalgia, meningismus, fever, chills, migratory polyarthralgia, and malaise. ECM or other rashes may occur at multiple sites. Hepatosplenomegaly or lymphadenopathy may be present. Fatigue and lethargy are the symptoms that are most constant in this stage of disease. Other manifestations may be fleeting. Ocular involvement may occur with anterior uveitis or conjunctivitis.7 Other cutaneous manifestations, including lymphocytoma, can occur, but are more frequently observed in Europe.
Early Neurological Involvement. Acute neurological involvement often occurs during this stage. This includes lymphocytic meningitis, cranial neuropathies (especially of the seventh cranial nerve, which can be bilateral), cerebellar ataxia, mononeuritis multiplex, and polyneuropathy (axonal sensorimotor neuropathy).10 Optic nerve inflammation leading to blindness may occur in children,7 and cases of pseudotumor cerebri as a presentation of Lyme disease have been reported in both children and adults.11 A lumbar puncture in Lyme meningitis shows laboratory abnormalities similar to a viral infection.
Early Cardiac Involvement. Cardiac manifestations of Lyme disease occur weeks to months following the bite. There is a gender predilection for men (3:1 male to female ratio). Atrioventricular block is the most common conduction abnormality seen with Lyme carditis. It usually presents with a third-degree block, although second-degree and first-degree blocks (most common in children) occur. Escape rhythms, brief asystoles, and fluctuating bundle branch blocks portend a poorer prognosis. CHF, dilated cardiomyopathy, carditis, and non-sustained ventricular tachycardia are other cardiac manifestations of Lyme disease.12
Late Disseminated. Late Lyme disease occurs months to years following the initial infection. This clinical syndrome presents with arthritis, encephalopathy, and dermatologic changes. Arthritis presents with episodes of oligoarticular arthritis of large joints, most commonly affecting the knees. Patients present with an acutely inflamed joint, with aspiration showing elevated white blood cell counts ranging from 500-110,000 cells/microliter with a PMN predominance, consistent with other inflammatory or infectious arthritides. Chronic central nervous system (CNS) findings of late Lyme disease include neuropsychiatric symptoms affecting mood, sleep, and memory. Encephalomyelitis, while rare, can lead to spastic quadraparesis or bowel/bladder dysfunction. Acrodermatitis chronica atrophicans is a dermatological complication of late Lyme disease that presents with insidious violaceous discolorations of the acral surfaces of arms or legs that causes sclerosis and atrophy over years. This is most often reported in women from Europe.7
Diagnosis
Lyme disease should be suspected in patients presenting with ECM or Lyme-associated symptoms such as unexplained heart block in patients who live in a location endemic to Ixodes scapularis. A careful travel history or history of tick bites should be obtained in cases in which Lyme disease is suspected.
The presence of ECM in the setting of a consistent clinical history is the only manifestation of Lyme disease that is characteristic enough for it to be diagnosed without further laboratory testing. This must be differentiated from tick bite hypersensitivity reaction, which presents as an urticarial rash less than 5 cm at its greatest width that disappears over 1-2 days.
Serological testing, the diagnostic method of choice for Lyme disease, should be reserved for patients with a high clinical suspicion for Lyme disease, as they have a poor positive predictive value. The United States Centers for Disease Control and Prevention currently recommends a two-step approach to the diagnosis of Lyme disease. Initial screening is performed with an ELISA, which is then confirmed with a Western blot. IgM antibodies are detectable in the first 1-2 weeks following exposure. Serological testing is highly insensitive in the first few week of infection, as antibodies may not have developed yet. In endemic areas, testing should be performed for coinfection with babesiosis and anaplasmosis.13 CSF can be tested similarly if neurological involvement is suspected.9 Other commercially available methods, including urine antigen testing, PCR, and immunofluorescent staining, are available, but their clinical usefulness has not been validated.14
Treatment
The recommended treatment regimen depends on the disease stage and patient characteristics. These recommendations are based on expert opinion.
Early Localized or Disseminated Lyme Disease Without Neurological or Cardiac Involvement. Oral doxycycline (100 mg BID), amoxicillin (500 mg TID), or cefuroxime axetil (500 mg BID) for 14 days are considered the first-line treatment choices. Doxycycline is often used in non-pregnant patients older than 8 years of age, as it covers anaplasmosis and other rickettsial diseases that may co-infect or be confused with early manifestations of Lyme disease. Amoxicillin is recommended for pregnant patients or children younger than 8 years old. Cefuroxime can be used in pencillin-allergic patients.15
Early Disseminated Disease: Neurologic Lyme Disease (Encephalitis, Meningitis, or Radiculopathy). Intravenous ceftriaxone (2 g daily) for 14 days is recommended for adults with neurological Lyme disease. Cefotaxime or penicillin G are suitable alternatives. Oral doxycycline can be used (100-200 mg BID for 10-28 days) in patients who are intolerant of beta-lactams or those with isolated facial nerve palsy. This recommendation is similar for children.15 These patients usually require admission to initiate intravenous antibiotics and to exclude other causes of meningitis.13
Early Disseminated Disease: Lyme Carditis. Patients who present with symptomatic cardiac disease (chest pain, dyspnea) or advanced heart block (first-degree with PR interval > 300 ms, second- or third-degree) should be admitted to the hospital and treated with intravenous antibiotics. The treatment regimen is similar to patients with early neurological Lyme disease (as above). Temporary pacemaker placement may be necessary, and consultation with a cardiologist should be pursued. Oral doxycycline is sufficient for minor cardiac involvement that is treated as an outpatient.15
Late Disseminated Disease: Lyme Arthritis. If there is no evidence of neuroborreliosis, oral doxycycline (100 mg BID) for 28 days is the recommended regimen for adults. Oral amoxicillin (first line in children younger than 8 years of age, and in pregnant women), and cefuroxime for 28 days may also be used.
If there is CNS involvement, patients of all ages should receive 2-4 weeks of intravenous ceftriaxone, cefuroxime, or penicillin G. Any patients who presents to the ED with persistent joint swelling following therapy should be given another four-week course of oral antibiotics, or 2-4 weeks of intravenous ceftriaxone.15
Late Disseminated Disease: Late Neurological Disease. Treatment is similar to the treatment for early disseminated neurologic disease (see above). The recommended length of treatment is longer, at 2-4 weeks.15
Prophylaxis. Recent studies have demonstrated that a single prophylactic dose of doxycycline (200 mg PO) given within 72 hours of a known I. scapularis tick bite reduces the incidence of subsequent ECM, the only reliable clinical marker for Lyme disease (0.4% vs 3.2% for placebo).17 As there are minimal adverse effects with this treatment, patients with known I. scapularis tick bite within the past 72 hours can be given a dose of this in the ED and provided close follow-up. If the tick bite is less than 36 hours old, no further prophylactic treatment is necessary following the removal of the tick. A vaccine was previously available, but this was discontinued in 2002 due to poor sales and questionable efficacy.16
Chronic Lyme Disease. Chronic Lyme disease is a syndrome in which persistent, nonspecific symptoms without medical explanation are attributed to this infection. Patients with a diagnosis of "chronic Lyme disease" may or may not have a history of a tick bite or acute Lyme disease. The current literature does not support the existence of a syndrome due to a persistent infection with B. burgdorferi. Nonetheless, many physicians and laypeople are convinced that it exists. It has led to patients being unnecessarily treated with long courses of intravenous antibiotics. Until there is further evidence to support its existence, chronic Lyme disease should not be an entity to work up or treat aggressively in an ED setting.18
Summary of Lyme Disease
- The most commonly reported vector-borne disease in the United States;
- Caused by the spirochete Borrelia burgdorferi, transmitted by Ixodes scapularis;
- Cutaneous, cardiac, musculoskeletal, and neurologic systems can be affected;
- Clinical diagnosis can only be made in the setting of ECM and appropriate history;
- In the absence of ECM, serology is often used to make the diagnosis;
- Treatment is with doxycycline in early disease for nonpregnant adults;
- Amoxicillin is used in pregnant women and children younger than 8 years of age;
- Intravenous ceftriaxone is generally used for disseminated disease;
- A single prophylactic dose of doxycycline 200 mg can be given to asymptomatic patients within 72 hours of I. scapularis bite.
Anaplasmosis
An 84-year-old woman from Long Island presents with worsening flu-like symptoms and confusion for the past three days. She developed fevers, myalgias, fatigue, nonproductive cough, and sore throat three days ago. This was initially thought to be due to a viral upper respiratory infection (URI), but the patient was brought in this morning when she was found lethargic and confused. On examination, the patient is febrile, tachycardic, dehydrated, and ill-appearing. She has diffuse abdominal pain and meningismus.
Introduction
Anaplasmosis, also known as human granulocytic anaplasmosis (HGA), is caused by obligate intracellular, gram-negative coccobacilli called Anaplasma phagocytophilum that infects circulating leukocytes. It has previously been referred to as human granulocytic ehrlichiosis and human granulocytic anaplasmosis. The bacterium is related to the causative agent of human monocytic ehrlichiosis (HME), which will be discussed in part 2. HGA and HME have similar clinical presentations. The characteristic finding of HGA is the presence of morulae within infected granulocytes.19,20 (See Figure 5.) This organism was first identified as the causative agent of HGA in 1994.21
Figure 5: Anaplasma phagocytophilum and Ehrlichia chaffeensis
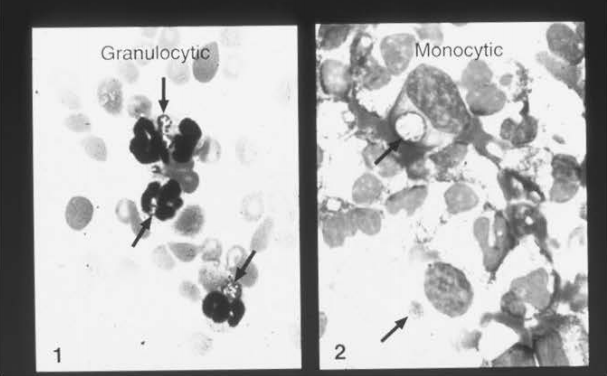
Slide 1 shows morulae characteristic of infection with Anaplasma phagocytophilum and Ehrlichia ewingii, which target granulocytes. Slide 2 shows monocytic morulae due to an infection with Ehrlichia chaffeensis. Ehrlichiosis is caused by bacterium in the genus Ehrlichia.
Source: US Centers for Disease Control and Prevention (CDC), Atlanta, GA, USA. CDC Public Health Image Library.
Epidemiology
HGA is a zoonotic infection that is transmitted by Ixodes scapularis and Ixodes pacificus, the same vectors of Lyme disease and babesiosis. Its geographic distribution mimics that of Lyme disease. (See Figure 2.) The number of reported cases of HGA has steadily increased since it became reportable. There were 348 reported cases in 2000, and 1,761 in 2010. The case-fatality rate is about 1%. Its incidence is higher in older populations, and peaks in the mid-summer months.22
Clinical Presentation
Patients who are infected with Anaplasma phagocytophilum present 1-2 weeks following a tick bite with nonspecific systemic symptoms. These include fevers, headaches, myalgias, malaise, chills, gastrointestinal symptoms, and altered mental status.23 These manifestations are usually mild to moderate in severity, and respond quickly to treatment. Spontaneous resolution is well documented. Diarrhea and rash are uncommon. Death usually occurs in immunocompromised or elderly individuals, often greater than 10 days after onset of the disease. There have been reports of transmission via blood donors in China.24 Fulminant infection with multiorgan system failure, or meningoencephalitis leading to death is less frequent with HGA than it is with HME.
Diagnosis
The diagnosis of HGA is made based on clinical and laboratory findings. Basic laboratory tests are non-specific, and may show leukopenia, lymphopenia, thrombocytopenia, transaminitis, and elevated alkaline phosphatase. The quickest method of diagnosis is via direct examination of the blood smear, which will show the characteristic intracellular morulae. However, this test is often insensitive due to the scarcity of directly observable morulae. The most sensitive test is by performing an indirect immunofluorescence assay in the acute and convalescent phases of illness. Culture in malignant granulocytes (HL-60 line) and PCR are other diagnostic modalities.15
Treatment
Oral doxycycline 100 mg BID for 7-14 days is the standard treatment regimen for HGA. This is the recommended regimen in patients of all ages, as the benefit of treatment outweighs the risks in pregnant women and children. In addition, doxycycline covers other rickettsial infections (such as Rocky Mountain spotted fever) that may present similarly to HGA.23 Intravenous treatment is often indicated for hospitalized patients. There is limited evidence to suggest the use of rifampin to treat HGA in children and pregnant women; however, doxycycline is still the preferred antibiotic.25 Levofloxacin has been shown to have activity against Anaplasma phagocytophilum in vitro, but there are no in vivo studies to suggest its use in infected patients.15 There is usually prompt response to doxycycline. If a patient fails to improve, other diagnoses should be explored. Prophylactic treatment for HGA following a tick bite is not indicated, although it may be given to prevent Lyme disease.23
Summary of Anaplasmosis:
- Transmitted by the same vector as Lyme disease;
- Anaplasma phagocytophilum is an obligate intracellular organism that can be identified as intragranulocytic morulae on smear;
- Patients typically present with nonspecific symptoms
- Diagnosis is made with blood smear or serology;
- Treatment is with doxycycline for all patients;
- Rifampin, which does not cover other diseases caused by I. scapularis, can be considered in children and pregnant patients.
Babesiosis
The patient is a 32-year-old HIV-positive woman from Cape Cod who presents with jaundice for one day. She states that she has been having flu-like symptoms for the past three days. She noticed that her skin became yellow, she was very dizzy, and progressively fatigued. She is febrile and hypotensive. On exam, she is has hepatosplenomegaly, jaundice, and diaphoresis.
Introduction
Babesiosis is a zoonotic infection caused by the intraerythrocytic protozoa of the genus Babesia. The first identified case of infection with Babesia microti, the primary organism that causes human babesiosis, in the United States occurred on Nantucket Island in 1969.26
Epidemiology
The epidemiologic data for babesiosis are limited, as national surveillance by the CDC did not begin until January 2011. Its primary vector is Ixodes scapularis. Although initially called "Nantucket fever" due to the number of cases on the island, it is now known to occur throughout the distribution of the Ixodes tick. (See Figure 2.) More than 100 species of Babesia are known to exist; however, only a few infect humans. Babesia microti causes the majority of babesiosis, mostly localized to the Northeast and Midwest. Babesia ducani and Babesia divergens have been identified as disease-causing agents on the West Coast and southern United States. There have been reported cases of transmission through blood transfusions.26
There were 1,124 cases reported to the CDC in 2011. Ninety-seven percent of these cases were reported from Minnesota, Wisconsin, and five northeastern states. More than half of the cases were in individuals older than 60 years of age, and the majority had symptoms starting in the mid-summer months. The male to female gender ratio was approximately 2:1. Ten cases were transfusion-related, and one reported case was thought to be congenitally acquired.27
Clinical Presentation
The clinical spectrum of babesiosis ranges from an asymptomatic, self-resolving infection to a fulminant, life-threatening disease. Symptoms develop after a one-week to one-month incubation period following a tick bite.28 They occur as a result of hemolysis secondary to the reproduction of babesia within erythrocytes. Constitutional symptoms, including fever, fatigue, chills, and headache, are common. There may be concurrent photophobia, sore throat, and conjunctivitis. Abdominal symptoms, including pain, nausea, vomiting, and anorexia, are less frequent.1 Similar to malaria, hemolysis occurs intermittently, corresponding to intermittent hemolytic anemia, sweats, myalgia, and headache.20
On exam, patients can have hepatosplenomegaly, joint swelling, jaundice, pallor, and dark urine. The acute illness lasts 1-2 weeks; patients may have fatigue that persists for months, and subclinical parasitemia can persist for months to years.28 The acute illness can be complicated by multiorgan dysfunction. This includes DIC, liver failure, splenic rupture, ARDS necessitating intubation, renal failure requiring dialysis, congestive heart failure/myocardial infarction, and shock. Babesiosis appears to be most debilitating in the elderly, immunocompromised, and those who are functionally or anatomically asplenic. It is fatal in 5-9% of cases.1,26,29
Diagnosis
Babesiosis should be suspected in patients with a consistent clinical presentation and basic laboratory work consistent with hemolytic anemia (normocytic anemia with elevated reticulocyte count, elevated LDH, reduced serum haptoglobin), thrombocytopenia, and urinalysis with hemoglobinuria and proteinuria.1,26 A definitive diagnosis can be established by observing the organisms on a Giemsa- or Wright-stained blood smear. The Babesia microti trophozoites are seen as pleomorphic intraerythrocytic rings that are indistinguishable from malaria trophozoites. The pathognomonic finding to clinch the diagnosis is the intraerythrocytic "Maltese cross" (see Figure 6), which is formed by tetrads of merozoites arranged in a cross-like pattern.26
Figure 6: Maltese Cross Finding Pathognomonic for Babesiosis
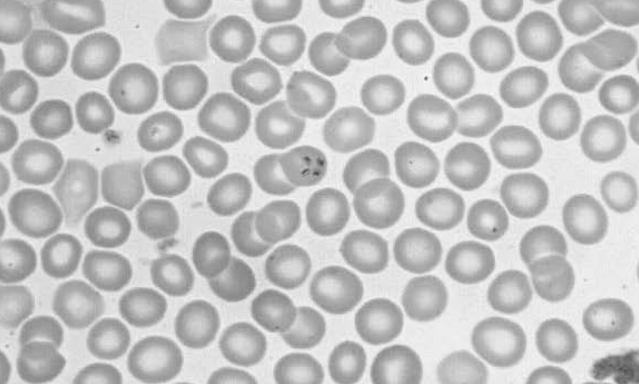
The center of this image shows the pathognomonic finding in babesiosis, the "Maltese cross." It is caused by the tetrad of merozoites of Babesia microti within red blood cells.
Source: US Centers for Disease Control and Prevention (CDC), Atlanta, GA, USA. CDC Public Health Image Library.
The Maltese cross sign is rare, and may require multiple thick and thin blood smears to find. If the clinical suspicion remains high in the setting of multiple negative blood smears, detecting antibodies via indirect fluorescent antibody test can make the diagnosis. PCR of the patient's blood for Babesia species, and isolation of the organism by inoculating the patient's blood into hamsters or gerbils are other methods of diagnosis.26,30
Treatment
The treatment regimen of choice for mild to moderate babesiosis in immunocompetent patients is the combination of oral atovaquone (750 mg BID) and oral azithromycin (500-1000 mg on day one, then 250 mg daily) for a total course of 7-10 days. This regimen is the same for children, although it is dosed by weight. Immunocompromised patients may require a prolonged course of treatment lasting greater than six weeks. Intravenous clindamycin and oral quinine was previously the regimen of choice, but has been replaced due to significant side effects. This combination is reserved for severely ill patients.
Patients with moderate to severe babesiosis should be admitted to the hospital for monitoring and treatment. Those with high-grade parasitemia (> 10%), significant hemolysis, or renal/pulmonary compromise should undergo RBC exchange transfusions.15,26 Treatment for coinfection with Lyme disease and anaplasmosis with doxycycline should be considered.
Summary of Babesiosis:
- Transmitted by the same vector as Lyme disease and anaplasmosis;
- Babesia microti, an intraerythrocytic parasite, is the main pathogen;
- Symptoms and laboratory findings are due to hemolysis and parasitemia (similar to malaria);
- Can lead to multi-organ failure and death, especially in the elderly and immunocompromised;
- Diagnosis is via blood smear showing "Maltese crosses" or via serology;
- Treatment is with oral atovaquone and oral azithromycin;
- Patients with severe illness require IV clindamycin and oral quinine.
Tick-Borne Encephalitis (TBE)
A 19-year-old woman presents with a headache for four days associated with fever, nausea, vomiting, and worsening confusion. She is a student at West Point. She is febrile and hemodynamically stable. The exam reveals an ill-appearing woman with meningismus.
Introduction
There are multiple encephalitis-causing viruses in the genus Flavivirus transmitted by Ixodes and other ticks, which are collectively referred to as the tick-borne encephalitis (TBE) group. Other more well-known flavivirus species include the West Nile virus, yellow fever virus, and dengue fever virus. Tick-borne encephalitis is one of the most dangerous CNS infections in Europe and Asia. The aptly named tick-borne encephalitis virus is the culprit in at least 11,000 cases of TBE in Russia, and 3,000 cases in the rest of Europe. Similar viruses spread Ixodes ticks are also known to cause fatal hemorrhagic fevers in Russia, India, and the Middle East.31
In the United States, the organisms responsible for all of the known cases of TBE are the Powassan virus (PV) and its close relative, the deer tick virus (DTV). DTV, which is serologically identical to but genetically different from PV, was isolated from the adult deer tick, Ixodes scapularis, in 1997. PV has been found in other Ixodes species. These two viruses are highly similar in physical characteristics; however, they are often referred to as different entities in current literature.32,33
Table 1: Summary of Tick-borne Diseases Endemic to the United States
| Disease/Organism | Vector | Presentation | Laboratory Findings | Diagnosis | Treatment |
|
Lyme Disease Borrelia burgdorferi |
Ixodes scapularis Ixodes pacificus |
Early localized: Erythema chronicum migrans, constitutional symptoms Early disseminated: Multiple ECM, constitutional symptoms, neurological symptoms, carditis Late disseminated: Arthritis, encephalopathy, dermatological changes |
Blood: • Nonspecific findings CSF: • Consistent with aseptic meningitis |
Serology: • ELISA • Western blot • Can be performed on CSF • Urine antigen • PCR • Immunofluorescence |
Nonpregnant adults, children > 8 years old: • Doxycycline • Amoxicillin • Cefuroxime axetil Pregnant adults, children < 8 years old: • Amoxicillin • Cefuroxime axetil Any neurologic or cardiac involvement: • Ceftriaxone • Cefotaxime • Penicillin G |
|
Anaplasmosis Anaplasma phagocytophilum |
Ixodes scapularis Ixodes pacificus |
Constitutional symptoms, altered mental status. Immunocompromised patients may have multi-organ dysfunction, and meningoencephalitis |
Blood: Leukopenia, lymphopenia, transaminitis, elevated alkaline phosphatase |
Blood smear: • Intracellular morula • Immunofluorescence • Culture • PCR |
• Doxycycline • Rifampin may be considered in pregnant adults and children |
|
Babesiosis Babesia microti Babesia ducani Babesia divergens |
Ixodes scapularis |
Constitutional symptoms, jaundice, abdominal pain, anorexia, nausea, diarrhea, photophobia, neurovegetative symptoms |
Blood: • Hemolytic anemia • Thrombocytopenia Urine: • Hemoglobinuria • Proteinuria |
Blood smear: • Maltese cross • Immunofluorescence • PCR |
• Atovaquone and azithromycin • Clindamycin and quinine for severe disease |
|
Tick-borne Encephalitis Powassan virus Deer tick virus |
Ixodes species |
Meningoencephalitis |
CSF: Similar to aseptic meningitis |
CSF: • Detection of viral genome • Positive viral serology |
• Supportive care • Empiric treatment for other causes of meningoencephalitis |
Epidemiology
Since its discovery in 1958, TBE (caused by DTV or PV) has occurred sporadically throughout the United States, Canada, and Russia. There have been approximately 70 reported cases of PV encephalitis and three reported cases of DTV encephalitis as of 2013. Most cases of PV encephalitis since 2010 were diagnosed in the states of Minnesota and Wisconsin. Two out of the three known cases of DTV encephalitis occurred in New York state. The general distribution of TBE appears to be in the northeastern/midwestern United States, corresponding to the distribution of Ixodes scapularis and related species. Its incidence in the United States appears to be increasing, with 1.3 cases per year from 1999-2005, as opposed to 0.7 cases per year between 1958-1998. It is important to note that TBE reportedly due to PV may actually have been caused by DTV, as genetic sequencing was not employed to diagnose this condition in the past.32,33
Clinical Presentation
Infection by viruses of the tick-borne encephalitis group can present with a range from mild symptoms to meningoencephalitis leading to death. Following an incubation of 8-34 days, patients present with a prodrome of headache, lethargy, and confusion, leading to encephalopathy with various progressive neurological symptoms. Sudden onset of fever, nausea, and vomiting is characteristic. Overall, TBE is associated with 10% mortality and long-term neurological sequelae in half of survivors.31,34
In reported cases, CSF studies have shown findings consistent with aseptic meningitis. MRI has shown changes in the cerebellum, brain stem, and basal ganglia in patients with TBE. Biopsy (usually performed at autopsy) shows necrotizing meningoencephalitis with infiltrates of predominantly CD8+ cytotoxic T cells.33,34
Diagnosis
The diagnosis of TBE can be difficult, as it mimics the presentation of many viral, bacterial, or fungal meningitis/encephalitis. Testing for PV or DTV is not routinely indicated in patients presenting with encephalitis. However, several milliliters of CSF can be collected in excess in the ED to be saved by the laboratory for further testing by the inpatient team.34 The diagnosis of TBE can be made with any of the following:33
- PV/DTV RNA presence in CSF;
- PV/DTV-specific IgM in CSF;
- Greater than fourfold increase in PV/DTV-specific neutralizing antibodies in serial serum assays;
- PV/DTV-specific IgM in serum and PV/DTV-specific neutralizing antibodies in the same or later serum specimen.
Although the definitive diagnosis cannot be made in the ED, some of these laboratory studies can be considered in the initial work-up of a patient presenting with meningitis or encephalitis.
Treatment
There is currently no standardized treatment regimen for TBE outside of supportive care. Pegylated interferon alpha and ribavirin have been administered with unclear results. Empiric treatment for patients presenting to the ED with TBE should be the same as for any patient presenting with meningitis or encephalitis, as TBE is relatively rare compared to other treatable causes of CNS infection. In current practice, this is with a combination of intravenous vancomycin, ceftriaxone, acyclovir, ampicillin, and dexamethasone, depending on the clinical context. Vaccines for TBE are available in Europe, but not in the United States.34,35
Summary of Tick-borne Encephalitis:
- Transmitted by the same vector as Lyme disease, anaplasmosis, and babesiosis;
- The known causative pathogens are closely related viruses in the genus Flavivirus;
- Rare, with about 70-80 total cases reported in the United States;
- Clinical/laboratory findings are similar to findings for other causes of viral meningoencephalitis;
- Diagnosis is via detection of viral genome or antibodies in the CSF;
- Treatment is supportive;
- Empiric treatment for other causes of meningitis should be implemented.
References
- Amsden JR, Warmack S, Gubbins PO. Tick-borne bacterial, rickettsial, spirochetal, and protozoal infectious diseases in the United States: A comprehensive review. Pharmacotherapy 2005;25:191.
- Stafford KC. Tick Management Handbook. The Connecticut Agricultural Experimentation Station. 2007.
- Patnaude MR, Mather TN. Bootlegged tick or deer tick. The University of Florida. 2000. Last updated January 2013. http://entnemdept.ufl.edu/creatures/urban/medical/deer_tick.htm. Accessed November 21, 2013.
- Ticks: Geographic distribution. Centers for Disease Control. Last updated November 22, 2013. http://www.cdc.gov/ticks/geographic_distribution.html. Accessed November 22, 2013.
- Burgdorfer W, Barbour AG, Hayes SF, et al. Lyme disease: A tick-borne spirochetosis? Science 1982;216:1317.
- Centers for Disease Control and Prevention. MMWR Surveillance Summaries- Surveillance for Lyme disease: United States — 1992 to 2006. 2008;59:1.
- Steere AC. Chapter 173. Lyme Borreliosis. In: Longo DL, Fauci AS, Kasper DL, Hauser SL, Jameson JL, Loscalzo J, eds. Harrison's Principles of Internal Medicine. 18th ed. New York: McGraw-Hill; 2012.
- Nadelman RB, Nowakowski J, Forseter G, et al. The clinical spectrum of early Lyme borreliosis in patients with culture-confirmed erythema migrans. Am J Med 1996;100:502.
- Graham J, Stockley K, Goldman RD. Tick-borne illnesses: A CME update. Pediatric Emerg Care 2011;27:141.
- Hengge UR, Tannapfel A, Tyring SK, et al. Lyme borreliosis. Lancet Infect Dis 2003;3:489.
- Castaldo JE, Griffith E, Monkowski DH. Pseudotumor cerebri: Early manifestation of adult Lyme disease. Am J Med 2008;121:e5.
- Lelovas P, Dontas I, Bassiakou E, et al. Cardiac implications of Lyme disease, diagnosis and therapeutic approach. Int J Cardiol 2008;129:15.
- Hu LT. In the clinic. Lyme disease. Ann Intern Med 2012;157:ITC2.
- Centers for Disease Control and Prevention. Notice to readers: Caution regarding testing for Lyme disease. MMWR Morb Mort Wkly Rep 2005;54:125.
- Wormser GP, Dattwyler RJ, Shaprio ED, et al. The clinical assessment, treatment, and pregention of Lyme disease, human granulocytopenic anaplasmosis, and babesiosis: Clinical practice guidelines by the Infectious Diseases Society of America. Clin Infect Dis 2006;43:1089.
- Hayes EB, Piesman J. How can we prevent Lyme disease? N Engl J Med 2003;348:2424.
- Nadelman RB, Nowakowski J, Fish D, et al. Prophylaxis with single-dose Doxycycline for the prevention of Lyme disease after an Ixodes scapularis tick bite. N Eng J Med 2001;345:79.
- Feder HM, Johnson BJ, O'Connel S, et al. A critical appraisal of "chronic Lyme disease." N Eng J Med 2007;357:1422.
- Brooks GF, Carroll KC, Butel JS, et al. Chapter 26. Rickettsia and Related Genera. In: Brooks GF, Carroll KC, Butel JS, Morse SA, Mietzner TA, eds. Jawetz, Melnick, & Adelberg's Medical Microbiology. 26th ed. New York: McGraw-Hill; 2013.
- Meredith JT. Chapter 155. Zoonotic Infections. In: Cydulka RK, Meckler GD, eds. Tintinalli's Emergency Medicine: A Comprehensive Study Guide. 7th ed. New York: McGraw-Hill; 2011.
- Pritt BS, Sloan LM, Johnson DH, et al. Emergence of a new pathogenic Ehrlichia species, Wisconsin and Minnesota, 2009. N Eng J Med 2011;365:422.
- Anaplasmosis — Statistics and Epidemiology. Centers for Disease Control. Last updated August 29, 2013. http://www.cdc.gov/anaplasmosis/stats/. Accessed December 1, 2013.
- Anaplasmosis — Symptoms, diagnosis and treatment. Centers for Disease Control. Last updated August 29, 2013. http://www.cdc.gov/anaplasmosis/symptoms/index.html. Accessed December 1, 2013.
- Krause PJ, Wormser GP. Nosocomial transmission of human granulocytic anaplasmosis? JAMA 2008;300:2308.
- Chapman AS, Bakken JS, Folk SM, et al. Diagnosis and management of tickborne rickettsial diseases: Rocky Mountain spotted fever, ehrlichioses, and anaplasmosis- — United States: A practical guide for physicians and other health-care and public health professionals. MMWR Recom Rep 2006;55:1.
- Vannier E, Krause PJ. Human Babesiosis. N Eng J Med 2012;366:2397.
- Centers for Disease Control. Babesiosis surveillance — 18 states, 2011. MMWR Morb Mort Wkly Rep 2012; 54: 505.
- Shah RG, Sood SK. Clinical approach to known and emerging tick-borne infections other than Lyme disease. Curr Opin Pediatr 2013;25:407.
- White DJ, Talarico J, Chang H, et al. Human babesiosis in New York state — Review of 139 hospitalized cases and analysis of prognostic factors. Arch Intern Med 1998;158:2149.
- Parasites and Health — Babesiosis. Laboratory identification of parasites of public health concern. Centers for Disease Control. Last updated July 20, 2009. http://www.dpd.cdc.gov/dpdx/HTML/Babesiosis.htm. Accessed December 1, 2013.
- Gritsun TS, Lashkevich VA, Gould EA. Tick-borne encephalitis. Antiviral Research 2003;57:129.
- Ebel GD. Update on Powassan virus: Emergence of a North American tick-borne flavivirus. Annu Rev Entomol 2010;55:95.
- El Khoury MY, Hull RC, Bryant PW, et al. Diagnosis of acute deer tick virus encephalitis. Clin Infect Dis 2013;56:e40.
- Tavakoli NP, Wang H, Dupuis M, et al. Fatal case of deer tick virus encephalitis. N Eng J Med 2009;360:2099.
- Brooks GF, Carroll KC, Butel JS, Morse SA, Mietzner TA. Chapter 38. Arthropod-borne and rodent-borne viral diseases. In: Brooks GF, Carroll KC, Butel JS, Morse SA, Mietzner TA, eds. Jawetz, Melnick, & Adelberg's Medical Microbiology. 26th ed. New York: McGraw-Hill; 2013.
Lyme disease is the most common vector disease. It often presents with erythema chronicum migrans in its earliest and most treatable stage.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
