Esophageal Foreign Bodies in the Pediatric Population: A Comprehensive Review of the Literature
Authors: Donald T. J. Godbold, MD, MS, FAAEM, Chairman and Medical Director, Emergency Medical Services, Department of Emergency Medicine, Mercy Medical Center Merced, Merced, CA; and Christopher D. Berg, DO, FAAEM, Attending Physician and EMS Medical Director, Department of Emergency Medicine, West Suburban Hospital Medical Center, Oak Park, IL.
Peer Reviewers: Ann Dietrich, MD, FAAP, FACEP, Associate Clinical Professor, Ohio State University, Attending Physician, Columbus Children’s Hospital, Associate Pediatric Medical Director, MedFlight, Columbus, OH; and Larry B. Mellick, MD, MS, FAAP, FACEP, Vice Chairman for Academic Development and Research, Department of Emergency Medicine, Medical College of Georgia, Augusta.
Children who present with a history of foreign body ingestion frequently offer both a diagnostic and management challenge to the emergency medicine physician. Esophageal foreign bodies can result in significant injury to or the death of a child. What follows is a review of the literature on the subject of esophageal foreign bodies in children.—The Editor
Anatomy and Physiology Involved with Esophageal Foreign Bodies
Anatomically, the esophagus can be divided into the upper, middle, and lower thirds. The upper one-third, or cervical esophagus, contains striated muscle and terminates below the pharyngeal constrictor muscles. The middle one-third, or upper thoracic esophagus, and the lower one-third, or lower esophagus, contain smooth muscle only, with the lower esophageal sphincter (LES) defining the distal boundary of the esophagus.
There are five anatomical sites of narrowing in the pediatric esophagus, which are: the cricopharyngeus muscle level at C6; the thoracic inlet at T1; the cardioesophageal level or aortic arch at T4; the tracheal bifurcation at T6; and the gastroesophageal junction or hiatal narrowing.1 These sites of esophageal narrowing are where most foreign bodies become lodged.
Of all esophageal foreign body ingestions, the most common site of lodgment is located within the upper one-third of the esophagus at the lower border of the cricopharyngeus muscle.1
When a food bolus or foreign object is swallowed, strong striated muscle contractions are able to forcefully propel the food bolus or object to the junction of the upper and middle thirds of the esophagus. Peristaltic contractions of smooth muscle below this area are relatively weak and often are unable to sustain forward progression of the ingested body.
Another common site of anatomic narrowing with subsequent impaction is the gastroesophageal junction. Lodgment of food boluses or foreign bodies occurs at this site usually as the result of the size and shape of the object, or due to an LES malfunction or anomaly, such as a Schatzki’s ring, strictures, webs, or varices.1,2
Epidemiology of Pediatric Foreign Body Ingestion
It is not known exactly how many foreign body ingestions occur each year in the pediatric population, as many ingestions go unnoticed by parents, and most foreign bodies pass uneventfully through the digestive tract. For the year 1999, the American Association of Poison Control Centers reported 182,105 ingestions of foreign bodies by persons younger than 20 years of age.3 There are approximately 1500 deaths from foreign body ingestions per year in the United States.3
Age Range. Pediatric patients have been shown in various studies to comprise 14-83% of all patients ingesting foreign bodies. This wide range depends upon the population being studied.2 Most ingestion cases occur in the age range of three months to 12 years, with a median age of 38 months.2,4 The child’s normal developmental milestones of using the hand to rake an object and to grasp with a pinching motion are seen at 6 months and 7 months of age, respectively. Both of these milestones are important in the etiology of foreign body ingestion. Higher incidence of ingestions and greater age ranges were found in pediatric populations that were psychotic, prisoners, or had histories of suicide attempts.
Gender. Previous studies have found that male and female children were about equal in incidence of foreign body ingestion.5
Temporal Relationships. Most foreign body ingestions occur in the summer months, with July, August, and December being the first, second, and third most predominant months, respectively. This pattern is thought to be related to the coinciding times of school vacations.2
The time of day at which foreign body ingestions occur is significant. Most foreign body ingestions have been shown to occur during the after-school hours. The greatest time periods for incidence of foreign body ingestion (as seen in one study) were noted to be between 4 p.m. and midnight (67%), and also between noon and midnight.4
Risk Factors. Risk factors for foreign body ingestion include mental and developmental retardation, hyperactivity, history of esophageal disease (e.g., tracheoesophageal fistula), esophageal atresia, gastroesophageal reflux with esophageal stricture and history of recurrent ingestions. High-risk social situations such as maternal delinquency, documentation of poor maternal care, parental psychoses, history of physical or sexual abuse, maternal prostitution and drug abuse are all statistically significant risk factors as well.4
Types of Foreign Bodies
Many various types of ingested foreign bodies have been recorded. Table 1 shows the more common types of foreign bodies, as noted from previous studies.2,6-8
|
It has been shown that 5% of cases of foreign body ingestions by children involved more than one foreign body.9 Coins are by far the most common foreign body object swallowed by children and coin ingestion dominates the literature on esophageal foreign bodies. Coins widely are accessible to the general pediatric population, and adults often unwisely give young children coins for various reasons.
In terms of bone ingestion, chicken and fish bones are the two most common types involved. Bone ingestion has been associated with poor table eating habits, as well as adults not completely removing meat from bones before feeding it to children. Cultural eating habits also are significant. A Hong Kong study involving 2394 cases of foreign body ingestions showed duck and goose bones to comprise 2.6% of foreign body ingestions.10
Meat boluses, such as beef strips and hot dogs, also are major offenders. Children often swallow insufficiently chewed food during meals. In general, round, smooth food boluses greater than 21 mm in diameter and food boluses longer than 6.5 cm tend to lodge in the esophagus.
Other foreign bodies ingested include buttons, beads, marbles, button batteries, can pull-tops, open and closed safety pins, toys and their parts, glass, straight pins, screws, nails, and eraser heads. Safety pin ingestions have become a less common occurrence, presumably due to the advent of disposable diapers.4
Pull-tops. Aluminum can pull-tops, once commonplace and a potentially serious form of foreign body ingestion, now no longer are widely available in the United States. In the past, these shiny aluminum objects were readily available, found in the home and on the ground, and ingestions of them often were not witnessed. Most ingested pull-tops pass uneventfully through the gastrointestinal (GI) tract; however, several cases have been reported in which the pull-tops were ingested and became lodged in the proximal esophagus. One documented death from a pull-top ingestion occurred when a fistula formed between the esophagus and a branch of the aorta.11 Aluminum pull-tops poorly absorb x-rays and are relatively radiolucent, making them difficult to detect radiographically.
Since most objects that do not pass the esophagus become impacted in the thoracic inlet or above the aortic arch, where the esophagus is projected over the anterior vertebrae, a pull-top easily may be missed on most posteroanterior (PA) or anteroposterior (AP) chest x-rays. On a lateral chest x-ray, a pull-top in the esophagus is about 14 mm in its greatest diameter. The pull-top is not as easily obscured by bone on lateral chest x-ray. The lateral chest x-ray, therefore, is better than PA or AP views in terms of radiographic pull-top detection.11
Button battery ingestion is a common occurrence in the pediatric population. One study examined 2382 cases of battery ingestions reported to a national registry during a seven-year period.12 Hearing aids were the most common source of ingested batteries in that study, comprising 952 (44.6%) of the 2382 cases. In 312 (32.8%) of those cases, the child had removed the battery from his own hearing aid. In that same study, only 9.9% of those children were symptomatic from the battery ingestion. Two children who were symptomatic, experiencing severe esophageal burns from the ingestions, necessitated repeated esophageal dilatations during follow-up care.12
Most of the lodged batteries noted in the study were of large diameter (20-23 mm). Neither battery diameter nor symptom occurrence could identify all patients in which the battery lodged in the esophagus. Eventual outcome was not determined by battery discharge state but, essentially, was influenced by the chemical composition of the battery.
Lithium batteries, for example, carrying a larger voltage and being of a larger diameter, were disproportionately related to adverse effects.
In this study, mercuric oxide batteries were noted to be more likely to break into small pieces after ingestion, compared to other types of battery cells.12 One case noted an increase in serum mercury levels, yet no cases of mercury toxicity were recorded in this series. This series also noted 10 prior reports of battery ingestion in which all of the patients who had elevated mercury levels had ingested mercury-containing batteries that had fragmented, and radiographic studies had revealed mercury droplets in the bowel. The authors concluded that any person ingesting mercuric oxide battery cells 15.6 mm in diameter may require special monitoring.12
In the cases examined in this study, the authors also noted that with 37 button cell ingestions, syrup of Ipecac was administered. This therapy resulted in only one expulsion of the battery ingested. In one case in particular, the Ipecac was noted to cause retrograde movement of the battery from the stomach to the esophagus, necessitating emergent endoscopic removal of the battery. During that particular study time period, endoscopic and surgical removal of ingested batteries incidentally had declined five-fold. Expectant observation of children who had ingested batteries apparently was becoming more acceptable management.
Battery location played a major role in the success rate of endoscopic removal. Batteries in the esophagus were removed more easily than those in a more distal location along the GI tract (90% success rate with esophageal location compared to 46.7 % success rate with locations distal to the esophagus).
Esophageal burns have been shown to occur when a battery has been lodged in the esophagus for only four hours, with esophageal perforation occurring in as few as six hours after time of ingestion.13 There have been two deaths documented in the literature from batteries ingested by children.13 Because of this potential for serious harm, a commonly accepted management strategy advocates immediate endoscopic removal if the battery is noted to be lodged in the esophagus. A non-invasive approach is indicated if the battery is beyond the esophagus and the child remains asymptomatic, i.e., expectant observation and close follow-up is recommended.12 If the child becomes symptomatic after the battery has passed beyond the esophagus, or if the battery has remained in the stomach for more than 24-48 hours, then removal is recommended.12,14
Signs
Depending on the study examined, 20-83% of patients with a history of foreign body ingestion have no signs or abnormalities noted on physical exam.4,15-17 The findings on physical exam can include the following: drooling, erythematous throat, crying, palatal abrasions, palpable foreign body, or even airway obstruction. Other less commonly seen signs are rhonchi, multiple burns and/or lacerations, otitis media, tachypnea, and/or cervical adenopathy.
Symptoms of Foreign Body Ingestion
The litany of possible symptoms of children with foreign body ingestion include dysphagia, vomiting, abdominal pain, cough, localization or foreign body sensation, and refusal of the child to take solids and liquids.16-19 Anorexia, irritability, crying, poor sleep, and drooling are the most common symptoms noted in children younger than 1 year of age. Less frequently reported were hematochezia, melena, cyanosis (from tracheal compression), stridor, voice change, bleeding gums, hemoptysis, and fever.
Previous studies have shown that 38-49% of patients with witnessed or subsequently documented foreign body ingestions showed no symptoms at all.15,17 One study involving 663 children with a history of foreign body ingestion showed that 22% of the children requiring removal of the foreign body were completely asymptomatic. Conversely, in that same study, fewer than 50% of the children presenting with dysphagia or vomiting did indeed have an identifiable foreign body lodged in the oropharynx or proximal esophagus.20
The presence of symptoms is significantly associated with esophageal foreign bodies, but the absence of symptoms does not reliably exclude the possibility of an esophageal foreign body.3,7,17 A child may have a foreign body lodged in the esophagus and be completely without any signs or symptoms, and for this reason radiological studies can be beneficial in the management of suspected foreign body ingestions.16
Radiological Studies
The benefits of obtaining x-rays on a child with a known or suspected foreign body ingestion are well described.3,4,7,16,21,22 Soft-tissue neck x-rays, chest x-rays, and abdominal views are helpful in detecting the type and location of foreign bodies, or complications such as pneumothorax, subcutaneous emphysema, lung abscess, atelectasis, or free peritoneal air.
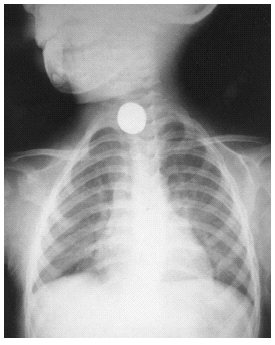
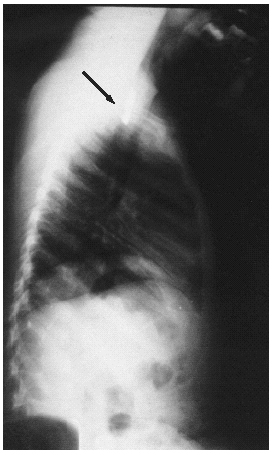
X-rays are particularly helpful in detecting the location of coins, as coins in the esophagus generally appear in the coronal alignment on anterior-posterior chest films.16 Coins in the trachea tend to become aligned in the sagittal plane.16
|
The location of coins in the esophagus (i.e., whether in the proximal, middle, or distal esophagus) can determine the best management. X-rays can be performed to help determine the specific coin location and, therefore, can help determine the proper strategy for removal of the coin.
An additional benefit is that x-rays sometimes may help define a foreign body’s physical characteristics (i.e., sharp or smooth, small or large, etc.). It is helpful for the physician to know the physical characteristics of a foreign body, as this will determine the proper method of removal.
|
X-rays not only can help to determine the location and physical qualities of a foreign body, but also (in some instances) can help to determine if there is more than one foreign body ingested. Lastly, repeat or subsequent x-rays can help the physician determine the natural progression of a swallowed foreign body if a child is being observed for a period of time rather than having the foreign body removed immediately.
An important point for the physician to remember is that a child still can have an esophageal foreign body even though the x-ray (as with radiolucent swallowed objects) and the child both may seem perfectly normal.
Aside from plain x-rays, contrast-enhanced x-rays can be employed in the evaluation of certain cases of esophageal foreign bodies. Contrast enhanced x-rays can be helpful in cases of food boluses or radiolucent object impactions. Water-soluble contrast media such as gastrograffin should be used if esophageal perforation is suspected to minimize complications from leakage into the mediastinum or pleural space. If leakage outside the gut and/or aspiration is a concern, non-ionic contrast media has been shown to cause no more histological changes than normal saline when introduced into the mediastinum and respiratory tract. Contrast media is especially important in the detection of radiolucent gastrointestinal foreign bodies that are made of plastic (e.g., buttons and toys).23 Barium soaked cotton wisps have been used in patients younger than 1 year of age to define masses in the GI tract suspected of being foreign bodies.
Other Methods of Esophageal Foreign Body Detection
Metal Detectors. In recent years, some studies have been done regarding the efficacy of metal detectors to detect and locate esophageal foreign bodies. One rather recent study used metal detectors to predict coin foreign body location, and then used radiographs to confirm the location of the coin. The study enrolled 91 children ages 9 months to 17 years. The operators of the metal detectors were physicians who had brief (less than one minute) training in their use. The study determined that the metal detector had a sensitivity of 98% (53/54) in detecting a coin ingested, and 98% (81/83) in determining that the coin was in the esophagus. The same study also concluded that symptoms alone were a poor indicator of coin location. In six out of eight cases of asymptomatic coin ingestion, there was spontaneous passage of the coins. It was concluded that metal detectors are good initial screening tools for coin detection, and also are useful in determining if the coin still is in the esophagus.24
Methods of Foreign Body Removal
Endoscopy remains the treatment of choice for foreign body extraction when used by those trained in this technique.25-27 The literature of the otolaryngology specialty clearly advocates the use of esophageal endoscopy in the removal of foreign bodies. Endoscopy usually is considered to be a safe, non-surgical method for removing impacted, sharp, or other types of foreign bodies. Benefits include the ability to visualize multiple and/or non-radiopaque foreign bodies. Endoscopy also allows for visualization of esophageal pathology, such as mucosal lacerations or granulation tissue. There are two types of endoscopy that are used, depending on the situation, in the management of esophageal foreign bodies. These two types are rigid and flexible endoscopy. For quite some time, rigid endoscopy was used primarily for the removal of any foreign body in the esophagus. The rigid endoscope has been shown to be more successful in the management of sharp, penetrating, or impacted foreign bodies. In the 1970s and 1980s, flexible fiberoptic endoscopy became more popular in usage, primarily because physicians preferred the latter for its ease of use compared to the rigid endoscope. The flexible endoscope seems to be more manageable in the hands of the average endoscopist and also is useful for more distal esophageal foreign bodies than the rigid scope.27 The rigid endoscope, on the other hand, enables the endoscopist to perform actual ensheathment of sharp points of foreign bodies prior to removal.28 One study comparing the two types of endoscopy showed that flexible endoscopy had a success rate of between 76% and 98.5%, with 0% morbidity and mortality noted (only one previous study showed an esophageal perforation rate of 0.5% with flexible endoscopy). Rigid endoscopy has been noted to have a success rate of between 94% and 100%, with an estimated rate of esophageal perforation of 0.34% and mortality rate of 0.05%.28
Drawbacks of endoscopy include the need for at least some period of post-procedure hospitalization or observation, pre-operative labs, general anesthesia, and potentially prohibitive costs compared to less invasive measures. With endoscopy also comes the risk of instrumentation damage to the esophagus or other parts of the GI tract.29
The Foley catheter method of removing esophageal foreign bodies first was described by Bigler in 1965 and has since become a widely used technique. In the past its usage has been controversial in the literature.30 This technique certainly is enhanced if performed with the aid of fluoroscopy, if available. The pediatric specialty areas of radiology, surgery, ENT, and general pediatrics are divided as to whether the procedure is preferred over endoscopy. The concern primarily involves the potential risk of aspiration of the object as it is pulled up through the oropharynx because the coin possibly can be "flipped" into the trachea just prior to retrieval. Despite the potential for aspiration, numerous large and prospective studies have shown the Foley catheter method to be a safe and effective technique in specialized cases.30,31 The object first should be localized radiographically if possible. The duration of foreign body esophageal lodgment should be fewer than 24 hours if the Foley catheter method is to be employed.26 Sharp, ragged, radiolucent, or unknown foreign bodies; esophageal disease; or complete obstruction are absolute contraindications to catheter use for removal.32 The Foley catheter method also is not recommended if there is more that one foreign body involved. The patient should be cooperative or otherwise restrained from making any sudden movements.
In a review of the studies on the Foley catheter method, the median age of the patient was 7 years, with a range from 6 months to 20 years of age. The Foley catheter method of foreign body removal begins with establishing IV access and then applying topical anesthesia and/or giving systemic sedation. A number 12 to 16 Fr Foley catheter then can be passed either nasally or orally. The patient should be in the sitting position initially for the Foley catheter placement, but then he or she can be placed in the prone oblique Trendelenburg position during actual object withdrawal. Preferably with the aid of direct fluoroscopic guidance, the catheter is passed beyond the visualized foreign body. Once the balloon end of the catheter is beyond the foreign body, the balloon is inflated with a water-soluble contrast agent. The catheter then is withdrawn with moderate steady traction. If the catheter slips past the object, it is reinserted and the procedure is repeated. When the foreign body appears in the hypopharynx, it may be expelled by vigorous cough or grasped with forceps. Resuscitation equipment, such as a laryngoscope, blades, and forceps, should be at hand when the procedure is performed. The physicians involved in this procedure should be skilled in the use of such equipment. It is recommended that physicians who use the Foley catheter method be competent in airway management as well as pediatric advanced life support.
Complications of this method are rare but include minor esophageal mucosal injury and risk of aspiration into the trachea. Benefits of the Foley catheter method include low cost, no need for general anesthesia, and avoidance of the risks of endoscopic instrumentation.
The bougienage method involves the use of a lubricated esophageal dilator essentially to push the foreign body past the esophagus into the stomach. The non-sedated child sits upright during the procedure. The ingested object must be round or smooth (such as a coin); its ingestion must have been witnessed; and its impaction must be fewer than 24 hours. Of course, with the bougienage technique, there must be no anatomical esopha-geal anomalies present.14
The technique is considered by some to be potentially uncomfortable for the non-sedated child, and carries its own potential for esophageal injury as well. The bougienage method does not seem to be utilized now as frequently as Foley catheter removal or endoscopy in the management of esophageal foreign bodies.14,26
In a comparison of endoscopy, Foley catheter removal, and the bougienage method, a recent study involving 1746 pediatric patients examined the three methods in terms of success and complication rates. Endoscopy was performed on 1005 of these patients, with a 100% success rate and a 2.5% complication rate. The Foley catheter method was performed on 658 patients, with a 93.9% success rate and a 12% complication rate. The bougienage method was employed on the fewest patients (83), with only an 83% success rate, yet this method had a 0% complication rate.26
Another removal technique for esophageal foreign bodies mentioned in the literature is known as the "penny pincher." With the aid of fluoroscopy, an endoscopic forceps ensheathed in a catheter is inserted into the esophagus. The forceps are used to firmly grasp the coin. The catheter over the forceps is meant to protect the oropharynx during the procedure.
One study describing the technique mentions that the procedure was performed without the aid of anesthesia or sedation. By using the penny pincher technique, the total time of removal from start to finish was 41 seconds on average, with 20 coins removed from 19 children. The mean age of the children studied was 34 months. The penny pincher, although not studied as thoroughly as the other techniques described, is claimed to provide the simplicity, cost effectiveness, and speed of Foley catheter or bougienage techniques, as well as the safety and sure grip of endoscopic forceps removal.33
Another method used for the retrieval of esophageal foreign bodies mentioned in the literature is the magnetic probe.6 This probe can be used, of course, to retrieve only those objects that are metallic as well as magnetic. The frequency of its usage and the success rate of the magnetic probe are not widely discussed in the literature.
Medications Used in the Management of Foreign Body Ingestion
Papain is a proteolytic enzyme derived from the papaya plant and is the main ingredient in commercial products such meat tenderizer. It has been used since the 1940s as a controversial agent for removal for known or suspected meat bolus impactions in the esophagus.2
Complications involved with the use of papain include erosion or perforation of the esophagus; dissolution of the meat portion of a meat bolus with a subsequent bony spicule eroding in the esophagus; and rupture or leakage of the solution into the mediastinum, which may cause mediastinitis and also may lead to great vessel rupture. Aspiration of the solution also has been shown to cause hemorrhagic pulmonary edema.2 Because of these associated risks and possible complications, papain has fallen out of favor and now is very rarely used by most institutions.
Another medication sometimes used in the management of certain esophageal foreign bodies is glucagon. Glucagon is a naturally occurring substance that relaxes the esophageal smooth muscle and lessens lower esophageal sphincter tone. As stated earlier, the upper third of the esophagus contains striated muscle and, therefore, glucagon is ineffective for foreign bodies in this proximal portion of the esophagus. Foreign bodies in the middle third minimally may be affected by the use of glucagon. One recent study, involving only 14 subjects, found no benefit in the use of glucagon with foreign body ingestion, yet previous data reviewed suggest that glucagon has been shown to be successful in 30-50% of patients treated for esophageal foreign bodies.34,35 Side effects of glucagon, such as nausea, vomiting, and dizziness, usually are minor and transient. No fatalities have been reported with the utilization of glucagon for foreign body ingestion.
Radiographic contrast studies should be obtained prior to glucagon usage to help localize the obstruction. Glucagon, if it is to be given, should be given IV in doses of 0.5-2.0 mg following a small test dose to evaluate for hypersensitivity. The patient should be sitting upright and given water to swallow after the injection. If repeat contrast esophagram shows that the obstruction no longer is in the esophagus, and no underlying pathology is demonstrated, the patient may be discharged home with close follow-up during the next 24 hours. If the offending body or food bolus remains in the esophagus despite administration of glucagon, then endoscopy is indicated. It should be noted that glucagon should not be used if there is a possible bony or sharp component to the esophageal foreign body, nor should it be used if there is a pre-existing esophageal anomaly. Although there is some theoretical benefit in the use of glucagon for certain food boluses and smooth objects at the gastroesophageal junction, this medication has not been proven to be consistently successful in the treatment of esophageal foreign bodies.26,34
Management of Esophageal Foreign Bodies
Airway management should be of primary concern initially in the evaluation of any potential foreign body ingestion. Once the airway has been determined to be patent and stable, then definitive management of the esophageal foreign body should be addressed.
Studies have shown that more than 80% of foreign bodies ingested will pass through the esophagus and eventually will be eliminated, with little or no adverse sequelae.2
Expectant observation usually is indicated when a foreign body is ingested, yet the decision to watch and wait for symptomatology also, of course, depends on the type of foreign body ingested, as well as the location of the foreign body, and its potential for harm. Rounded or smooth foreign bodies, for example, reasonably can be expected to traverse the GI tract safely, if these objects can get past the gastroesophageal junction.
As coins are the most common type of esophageal foreign body encountered, the ED physician should be familiar with the management of coin ingestion. Although the potential for morbidity or even death exists, ingested coins usually pass after a benign course, if they can pass the gastroesophageal junction. Coins usually can remain in the distal esophagus without serious sequelae, as long as the child is relatively asymptomatic, for up to 24 hours. Coins may be removed from the esophagus with the Foley catheter method or bougienage method (if lodged fewer than 24 hours) or with endoscopy. A practical method of esophageal coin management that has been proposed is as follows: as long as the patient remains asymptomatic, the child with an esophageal coin foreign body can be given small sips of water or even a small amount of food, and be observed. A repeat x-ray can be done in 6 hours or sooner, if the child expresses improvement.6,26 Endoscopic removal (or Foley catheter or bougienage technique, whichever is most appropriate and available) can be utilized if there is little or no progression of the coin out of the esophagus.26
Localization of the swallowed coin is important. The literature suggests that coin lodgment in the distal esophagus can be watched longer than those in the more proximal esophagus.7,26 The observation period while the coin is in the distal esophagus safely can be extended to 24 hours, according to most studies.9,26 Coins lodged in the proximal or mid-esophagus should be removed sooner than 24 hours, if not immediately, as more proximal lodged esophageal coins have been shown to be less likely to progress naturally to the stomach.26
Prior to removal, repeat x-rays are recommended, especially if the child has to wait awhile before endoscopy or other removal method is performed, to ensure that the coin has not already passed on to the stomach on its own.26
As stated earlier, batteries lodged in the esophagus should be removed promptly, preferably by endoscopy. Expectant observation at home, as long as the child is asymptomatic, is recommended for battery ingestion only if the battery has passed beyond the esophagus. Repeat x-rays in 24-48 hours should be considered for mercuric acid battery ingestion, and in cases involving children ages 6 years and younger who ingest batteries greater than 15 mm.12 Repeat x-rays also should be done to be certain that the battery has not become lodged in the stomach. Recommendations for removal of gastric batteries depends on the study examined; some studies recommend removal 24-48 hours after ingestion if the battery still is in the stomach.12,14
Esophageal food boluses, or objects that are impacted, spiculated, long (greater than 3-4 cm), or sharp in nature, as well as those foreign bodies that result in perforations, require prompt endoscopist and/or surgical consultation.6
Once the foreign body has passed into the intestines, expectant observation at home is recommended. Repeat follow-up x-rays can be done at 48 hours and in 1 or 2 weeks if the object is not seen in the stools by the parents. There have been reports of perforation of bowel once a sharp foreign body has passed beyond the stomach, but these incidences are rare, and fewer than 1-2% will require surgery.3
A proposed algorithm for the management of various types of esophageal foreign bodies is shown in Figure 3.
Summary
Foreign body ingestions in the pediatric population are a common occurrence. The different types of ingested foreign bodies are wide and varied, with coins being the most common type.
Signs and symptoms are varied, and the child even may be asymptomatic after ingesting a foreign body. Initial emergency department evaluation of the child with suspected or known foreign body ingestion may include the use of metal detectors, plain x-rays, or contrast-enhanced x-rays.
Certain foreign bodies, such as those causing airway compromise, significant discomfort or distress, or those objects that are sharp or impacted, should be removed as safely and quickly as possible. Button batteries, with their potential for serious harm or death if they are lodged in the esophagus, also should be removed promptly.
The management of esophageal foreign bodies is varied, and may include expectant observation, endoscopy, Foley catheter removal, or the bougienage method. Relatively newer methods of removal, such as the magnetic probe and the penny pincher, have been described in the literature for certain esophageal foreign bodies. The particular management and removal of a foreign body from the esophagus is dependent on the severity of symptoms, the type of foreign body ingested, as well as its physical characteristics.
The physician should be able to decide when it is possible to watch and wait for natural passage of an ingested foreign body, provided that the child is not in distress and the foreign body is not of a type that has the potential for serious harm to the child.
Finally, the physician also should be familiar with the various resources, equipment, and consultants available at his or her own institution, prior to facing the challenge of a child with an esophageal foreign body.
References
1. Gaasch W, Barish R. Swallowed Foreign Bodies. In: Tintinalli JE, et al, eds. Emergency Medicine—A Comprehensive Study Guide. 3rd Edition, New York:McGraw Hill; 1992: 310-312.
2. Taylor RB. Esophageal foreign bodies. Emerg Med Clin North Am 1987;5:301-311.
3. Chen MK, Beierle EA. Gastrointestinal foreign bodies. Pediatr Ann 2001;30:736-742.
4. Binder L, Anderson WA. Pediatric gastrointestinal foreign body ingestions. Ann Emerg Med 1984;13:112-117.
5. Chaikhouni A, Kratz JM, Crawford FA. Foreign bodies in the esophagus. Am Surg 1985;51:173-179.
6. Arana A, Hauser B, Hachimi-Idrissi S, et al. Management of ingested foreign bodies in childhood and review of the literature. Eur J Pediatrics 2001;160:468-472.
7. Macpherson R, Hill JG, Othersen HB, et al. Esophageal foreign bodies in children: Diagnosis, treatment, and complications. Am J Radiol 1996;166:919-924.
8. Reilly JS, Walter MA. Consumer product aspiration and ingestion in children: Analysis of emergency room reports to the National Electronic Injury Surveillance System. Ann Otol Rhinol Laryngol 1992; 101:739-741.
9. Crysdale WS, Sendi KS,Yoo J. Esophageal foreign bodies in children. 15-year review of 484 cases. Ann Otol Rhinol Laryngol 1991; 100(4 Pt 1):320-324.
10. Nandi P, Ong GB. Foreign body in the esophagus: Review of 2394 cases. Br J Surg 1978;65:5-9.
11. Burrington JD. Aluminum "pop tops": A hazard to child health. JAMA 1976;235:2614-2617.
12. Litovitz T, Schmitz BF. Ingestion of cylindrical and button batteries: An analysis of 2382 cases. Pediatrics 1992;89:747-757.
13. Litovitz TL. Button battery ingestions: A review of 56 cases. JAMA 1983;249;2495-2500.
14. McGahren E. Esophageal foreign bodies. Pediatrics in Review 1999;20:129-132.
15. Humphries CT, Wagener JS, Morgan WJ. Fatal prolonged foreign body aspiration following an asymptomatic interval. Am J Emerg Med 1988;6:611-613.
16. Hodge D, Tecklenburg F, Fleisher G. Coin ingestion: Does every child need a radiograph? Ann of Emerg Med 1985;14:443-446.
17. Bailey P. Pediatric esophageal foreign body with minimal symptomatology. Ann Emerg Med 1983;12: 452-454.
18. Virgilis D, Weinberger J, Fisher D, et al. Vocal cord paralysis secondary to impacted esophageal foreign bodies in young children. American Academy of Pediatrics 2001;107:E101.
19. Schunk JE, Corneli H, Bolte R. Pediatric coin ingestions: A prospective study of coin location and symptoms. Am J Dis Child 1989;143:546-548.
20. Panieri E, Bass DH. The management of ingested foreign bodies in children—a review of 663 cases. Eur J Emerg Med 1995;2:83-87.
21. Gracia C, Frey CF, Bodai Bl. Diagnosis and management of ingested foreign bodies: A ten-year experience. Ann Emerg Med 1984;13: 30-34.
22. Brown L, Dannenberg B. A literature-based approach to the identification and management of pediatric foreign bodies. Pediatr Emerg Med Reports 2002;7:93-103.
23. Fernandes ET, Hollabaugh RS, Boulden T. Mediastinal mass and radiolucent esophageal foreign bodies. J Pediatr Surg 1989;24: 1135-1136.
24. Bassett KE, Schunk JE, Logan L. Localizing ingested coins with a metal detector. Am J Emerg Med 1999;17:338-341.
25. Tam PK, Saing H. Pediatric upper gastrointestinal Endoscopy: A 13 year experience. J Pediatr Surg 1989;24:443-447.
26. Roberts JR. The swallowed coin: Treatment and removal. Part II in a series. In: Hoffman L, et al, eds; Emergency Medicine News; Philadelphia: Lippincott, Williams&Wilkins; 2001;23:30-34.
27. Bendig DW. Removal of blunt esophageal foreign bodies by flexible endoscopy without general anesthesia. Am J Dis Child 1986; 140:789-790.
28. Roffman E, Jalisi S, Hybels R, et al. Failed extraction of a sharp esophageal foreign body with a flexible endoscope. Otolaryngol Head Neck Surg 2002;128:1096-1098.
29. Bigler FC. The use of a Foley catheter for removal of blunt foreign bodies from the esophagus. J Thorac and Cardiovasc Surg 1966;51: 759-760.
30. Campbell JB, Quattromani FL, Foley LC. Foley catheter removal of blunt esophageal foreign bodies: Experience with 100 consecutive children. Pediatr Radiol 1983;13:116-119.
31. Campbell JB, Condon VR. Catheter removal of blunt esophageal foreign bodies in children: Survey of the Society for Pediatric Radiology. Pediatr Radiol 1989;19:361-365.
32. Dunlap LB. Removal of an esophageal foreign body using a Foley catheter. Ann Emerg Med 1981;10:101-103.
33. Gauderer MW, DeCou JM, Abrams RS, et al. The "penny pincher": A new technique for fast and safe removal of esophageal coins. J Pediatr Surg 2000; 35:276-278.
34. Mehta D, Attia M, Quintana EC, et al. Glucagon use for esophageal coin dislodgement in children: A prospective double blind, placebo-controlled trial. Acad Emerg Med 2001;8:200-203.
35. Glauser J, Lilja GP, Greenfeld B, et al. Intravenous glucagon in the management of esophageal food obstruction. JACEP 1979;8: 228-231.
Children who present with a history of foreign body ingestion frequently offer both a diagnostic and management challenge to the emergency medicine physician. Esophageal foreign bodies can result in significant injury to or the death of a child. What follows is a review of the literature on the subject of esophageal foreign bodies in children.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.