Discharge Planning Advisor: Successful CM program gets JCAHO approval
Discharge Planning Advisor: Successful CM program gets JCAHO approval
Database demonstrated processes were in place
With a care coordination program in place that has dramatically reduced acute care and emergency department (ED) utilization by the chronic frail elderly while enhancing patients’ quality of life, Sutter Health Sacramento (CA) Sierra Region (SHSSR) was looking for a way to take the program to yet a higher level, says Jan Van der Mei, RN, care management director.
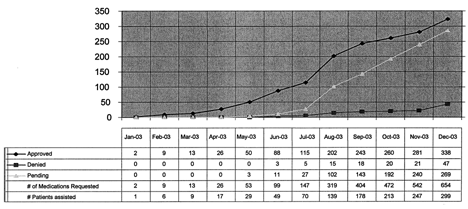
The Sutter Care Coordination Program (SCCP) — profiled in its early stages in the April 2001 issue of Discharge Planning Advisor — assisted more than 3,000 patients in 2003, she notes.
A list of outcomes for the report period from June 2002 to June 2003 includes a cost of $598.61 per member per month less for SCCP patients than for the baseline group, while ED costs for SCCP participants were 40.7% less and acute inpatient costs were 52.6% less. After subtracting program costs, Van der Mei adds, there was an annual saving to SHSSR of $935,000.
At an American Case Management Association (ACMA) conference in early 2003, Van der Mei heard about the Disease Specific Care (DSC) certification offered by the Joint Commission on Accreditation of Healthcare Organizations.
In June 2003, she and SHSSR’s manager for disease management and care coordination supervisor attended a Joint Commission conference on how to be certified.
By November 2003, the health care organization had attained certification for the Sutter Heart Failure Telemanagement Program, the Sutter Anticoagulation Program, and the Sutter Asthma Management Program, as well as for its care coordination program.
"When we decide to do something, we want to get it done," Van der Mei said with a laugh when asked about the short time frame. "We wanted to accomplish this in 2003."
What the Joint Commission certification reflects, notes Cheryl Phillips, MD, medical director of the Sutter Medical Group, an association of physicians that is aligned with SHSSR, is the recognition that care coordination and case management are critical elements of patient care.
"For the first time, we recognize case management as having some of the elements present in disease management — especially the structure of evidence-based models," she says. "Part of the criticism of case management in the past has been that its effectiveness is dependent on whether you have a good case manager.
"Now, there is some evidence-based structure so the case manager is not winging it every time with every problem," Phillips adds.
A structured process
The algorithms and decision trees Van der Mei has developed, she notes, illustrate that "care coordination is not just doing nice things for people but a fairly structured process that can be replicated."
Certification of SHSSR’s care coordination program represented a first for the Joint Commission process, which previously had focused only on programs with clear, easily demonstrable guidelines, Van der Mei points out.
"To be certified, you need to show you’ve based your program on evidence-based guidelines. That’s easy to do with heart failure and with asthma and anticoagulant programs, because [the guidelines] are out there," she adds.
"But a program dealing with the chronic frail elderly," Van der Mei explains, "is not disease-specific. Most patients have at least three or four chronic diseases and a couple of comorbidities, so we weren’t sure how we would be able to show them that our program is based on evidence-based guidelines."
As part of that effort, Van der Mei provided JCAHO with information on problems the program had identified as common to the care of the frail elderly and the accompanying interventions taken by SCCP.
With some problems — advance care planning, abuse and domestic violence, AIDS/HIV, and Alzheimer’s disease, for example — established evidence-based guidelines do exist, Van der Mei notes. For bereavement, however, or inadequate caregiving support, such established guidelines were not available, she adds.
What impressed the JCAHO reviewer, Van der Mei believes, is that SCCP had guidelines for most of the problems and that the processes used are detailed in a comprehensive database that SCCP makes available to the physicians with whom it works.
"[The database] is part of the physician’s medical record," she points out. "We’re linked to the physicians, so they know what we’re doing with their patients. We’ve built in the care plan, the problems identified by the physician, nurse, or social worker, and the interventions. That, as well as meeting the other standards, is how they were able to certify us.
"What’s unique about our programs," Van der Mei goes on to explain, "is that we are able to incorporate all of the interventions that we do in care coordination into our disease-specific programs. The case managers collaborate, so if someone is in the heart failure program, we not only manage those signs and symptoms, but if there are other issues — like the patient is not compliant, can’t afford meals, or has other psychosocial problems — the care coordination team can address those issues as well."
She points out, for example, that patients in the heart failure program have 68% fewer admissions for any reason — not just heart-related problems — than a group of like patients who are not in a care coordination program.
Reevaluating processes, outcomes
Part of the value of the JCAHO certification process, Van der Mei says, was the accompanying growth and learning that took place. "We knew we would benefit by meeting the standards of another body and evaluating the things we were doing. It made us look at all of our processes and say, Do we have a policy to support these?’"
One of the biggest challenges for SCCP — which uses a nurse/social worker model — was looking at how its program supports patient self-management, which is an integral part of the Joint Commission's philosophy, she says.
"It’s important to [JCAHO] that patients are involved in the plan of care," Van der Mei adds. "Our social workers are good at doing that, at saying [to the patient], Which goal do you want to work on first?’"
A different perspective on outcomes
But while social workers are better at working with patients to identify their goals, she notes, nurses tend to provide more direction and to base it on what they believe are the most urgent medical conditions.
Going through the Joint Commission certification, Van der Mei says, "helped us get the nurses to be more cognizant of being less directive and more soliciting of patients’ willingness to make changes."
Another benefit, she points out, was the opportunity to take a different perspective on program outcomes. While Sutter has always had outcomes that reflect both quality and utilization, she notes, it did not necessarily have the measurements to fully document its emphasis on quality.
The Joint Commission was not interested particularly in utilization standards, which addressed such results as the amount of money saved because patient visits to the ED were reduced, Van der Mei says.
It was more focused on other outcomes, "which we did have, but we had to come up with some additional measurements," she adds.
For example, SCCP patients are given an initial assessment, but the program wasn’t measuring exactly when the assessment was done, Van der Mei explains.
"Was it in the first month?" Similarly, the program already did advance care planning with patients, she adds, but as a result of its Joint Commission process, identified that it would measure whether that discussion took place within 90 days.
"For our disease-specific programs, we do a lot of patient education around heart failure, asthma, and the consequences of being on anticoagulant drugs," Van der Mei continues. "We want to make sure that education happened within a certain time frame, so we had policies for that, but we weren’t measuring when it took place. We found we weren’t documenting it as well as we should, that nurses weren’t indicating in the database [that they had done patient education].
"We know we have the policies and procedures in place," she says, "but until you do the measurement, you don’t realize you have a problem. So [the certification process] helped us identify that we had a documentation problem."
Staff supportive of process
Her staff were actively involved in looking at the different JCAHO standards and determining whether the program met them, and if so, how to show that compliance, Van der Mei notes.
"Sometimes, they were worded a little different, so we’d have to think about it and say, Oh, yeah, we’re doing that — we’re just not calling it that.’"
She says the SCCP nurses and social workers understood that obtaining the JCAHO certification "helped us move to the next stage of our development and would provide us with a standard we could say — [to insurance companies, for example] — that we meet."
The fact that Sutter’s care management programs are part of a hospital system that goes through JCAHO’s accreditation process makes disease-specific certification a little easier than for, say, a disease management company that might be seeking certification, Van der Mei points out.
"In fact," she says, "JCAHO gives organizations a discount if they’re part of a hospital system that’s accredited." And, Van der Mei adds, the care management program was able to adapt the hospital system’s sentinel event policy to meet the JCAHO requirement for disease-specific programs. "There are some other [hospital system policies] that just needed to be tweaked," she notes.
[For more information on Sutter’s care management programs, contact:
- Jan Van der Mei, Care Management Director, Sutter Health, Sacramento (CA) Sierra Region. Phone: (916) 854-6896. E-mail: [email protected].]
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
