A Comeback for Colistin?
A Comeback for Colistin?
Abstract & Commentary
Synopsis: The 50-year-old drug colistin was used successfully in 14 of 23 cases of serious infections caused by multiply resistant Pseudomonas aeruginosa .
Source: Linden PK, et al. Use of parenteral colistin for the treatment of serious infection due to antimicrobial-resistant Pseudomonas aeruginosa. Clin Infect Dis. 2003;37:e154-e160.
Colistin was used as salvage therapy for 23 critically ill patients with serious hospital-acquired pneumonia caused by Pseudomonas aeruginosa uniformly resistant to the b-lactams piperacillin, ceftazidime, cefepime, aztreonam, imipenem, the aminoglycosides gentamicin and tobramycin, as well as the fluoroquinolone ciprofloxacin. All patients had been admitted to an abdominal organ transplantation unit at the University of Pittsburgh Medical Center between January 1996 and February 2003. All patients were in intensive care, and all had evidence of pneumonia as defined by the American Thoracic Society.1 Twenty-two of the patients were receiving mechanical ventilation, and 21 were being given artificial kidney support at the start of therapy. Infections at additional sites affected 5 patients. Colistin was administered intravenously via catheter at a dose of 2.5 mg/kg q.12h. when serum creatinine was < 2.5 mg/dL, the same dose once daily when the serum creatinine was between 2.6 and 4 mg/L, or as a single 1 mg/kg dose per day when the serum creatinine was > 4 mg/dL for a median of 17 days (range, 7-36 days). The drug was given as monotherapy in 10 cases or combined with amikacin in 4 cases or a ß-lactam in the remaining cases. A favorable clinical response was observed for 14 patients (61%); 3 patients experienced relapse, and 7 patients died during therapy. Bacteremia affected 8 patients and was the only significant factor associated with treatment failure (P = .02). Colistin proved safe and was well tolerated by all except one patient who developed diffuse weakness that resolved after temporarily stopping therapy. Colistin affords salvage therapy for those patients with infections due to P aeruginosa that might otherwise have prove untreatable.
Comment by J. Peter Donnelly, PhD
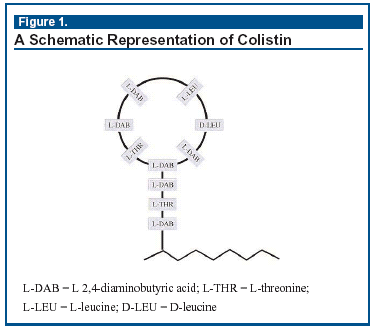
Colistin is a basic cyclic polypeptide (see Figure 1) also known as polymyxin E and is a relative of polymyxin B. The drug originates from the Gram-positive spore-forming rod of Bacillus polymyxa var. colistinus. It is not surprising that all Gram-positive bacteria such as Staphylococcus aureus are resistant. Some Gram-negative bacteria including Proteus species and Burkholderia cepacia are also inherently resistant. Hence, colistin is a narrow-spectrum drug active against enteric Gram-negative bacilli such as Escherichia coli and, of course, P aeruginosa.
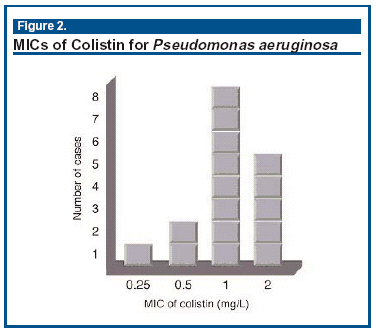
Despite celebrating 50 years of use, its exact mode of action remains incompletely known, but it appears to disrupt cell membrane function. This may be because its use was superseded by the introduction of the anti-pseudomonal aminoglycosides and penicillins and later the cephalosporins, carbapenems, and fluoroquinolones. The MICs of colistin for P aeruginosa lie close together between 0.25 and 2 mg/L (see Figure 2) and are no different today than they were 50 years ago. So, despite P aeruginosa being very adept at developing resistance to a whole range of antimicrobial agents, the polymyxins seem to remain a notable exception. Others have also resorted to colistin for similar reasons1-7 prompting the headline "Colistin: An antimicrobial for the 21st century?"8 The answer seems to be affirmative for settings similar to those described here.
The pharmacokinetics of the drug are poorly defined.9 A variety of adverse drug reactions have been ascribed to colistin, including neurotoxicity (apnea, perioral and peripheral paraesthesia, vertigo; rarely vasomotor instability, slurred speech, confusion, psychosis, visual disturbances) and nephrotoxicity. Hypersensitivity reactions have also been reported (www.x-gen.us/ProductInserts/Colistimethate_info.pdf). However, the development of such reactions is thought to be due to not following the manufacturer’s instructions carefully enough. Moreover, the fact remains that experience with this drug is limited because its use was largely abandoned once safer and better alternatives were available. Linden and colleagues use phrases like "resurrection" and "agent of last resort" to underscore the desperation encountered when faced with a "dangerous therapeutic void," as in their case. The drying up of the pipeline for new drug products to tackle multiple resistance only adds to this sense of doom. Whether they are right in their assessment, the dearth of new antibacterial agents looks set to continue. The message also seems clear. We are just going to have to make the best of what we have in our antimicrobial armamentarium. With drugs like colistin, we may even have to learn not only when, but also how, to use them safely and most effectively.
Dr. Donnelly, Clinical Microbiologist University Hospital Nijmegen, The Netherlands Section Editor, Microbiology.
References
1. Conway SP, et al. Intravenous colistin sulphomethate in acute respiratory exacerbations in adult patients with cystic fibrosis. Thorax. 1997;52:987-993.
2. Markou N, et al. Intravenous colistin in the treatment of sepsis from multiresistant Gram-negative bacilli in critically ill patients. Crit Care. 2003;7:R78-R83.
3. Conway SP, et al. Safety and tolerability of bolus intravenous colistin in acute respiratory exacerbations in adults with cystic fibrosis. Ann Pharmacother. 2000;34:1238-1242.
4. Levin AS, et al. Intravenous colistin as therapy for nosocomial infections caused by multidrug-resistant Pseudomonas aeruginosa and Acinetobacter baumannii. Clin Infect Dis. 1999;28:1008-1011.
5. Evans ME, et al. Polymyxin B sulfate and colistin: Old antibiotics for emerging multiresistant gram-negative bacteria. Ann Pharmacother. 1999;33:960-967.
6. Ledson MJ, et al. Four years’ experience of intravenous colimycin in an adult cystic fibrosis unit. Eur Respir J. 1998;12:592-594.
7. Frederiksen B, et al. Antibiotic treatment of initial colonization with Pseudomonas aeruginosa postpones chronic infection and prevents deterioration of pulmonary function in cystic fibrosis. Pediatr Pulmonol. 1997;23:330-335.
8. Stein A, Raoult D. Colistin: An antimicrobial for the 21st century? Clin Infect Dis. 2002;35:901-902.
9. Hermsen ED, et al. Polymyxins: Pharmacology, pharmacokinetics, pharmacodynamics, and clinical applications. Infect Dis Clin North Am. 2003;17(3):545-562.
The 50-year-old drug colistin was used successfully in 14 of 23 cases of serious infections caused by multiply resistant Pseudomonas aeruginosa .Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
