Hospitals and surgery centers throw punches at national, state, local level
Hospitals and surgery centers throw punches at national, state, local level
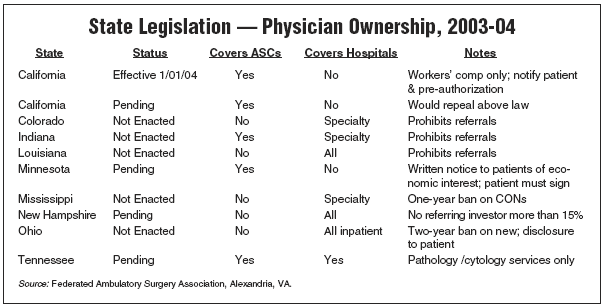
Regulations and legislation target physician-owned facilities
County commissioners in Sheridan, WY, are seeking a moratorium on ambulatory surgery centers (ASCs) after the hospital and physicians planned competing facilities. Communities in Kansas and Oklahoma have passed similar moratoriums.
Economic credentialing actions have been taken by hospitals in Ohio, Idaho, Arkansas, and elsewhere against physician owners of competing facilities, says David Shapiro, MD, president of the Johnson City, TN-based American Association of Ambulatory Surgery Centers (AAASC).
A group of doctors who say they were blocked from building an outpatient surgery center is suing a Lancaster County, SC, hospital for $15 million.
And the list goes on. (For more examples, see box, below.)
What’s going on?
"I think that the actions are part of a concerted effort by hospitals to impose restrictions on ASC development and generally make physician investment in ASCs less appealing," says Eric Zimmerman, JD, partner with McDermott, Will & Emery (MWE) in Washington, DC.
According to sources interviewed by Same-Day Surgery, hospitals have increasingly become concerned about competition from specialty hospitals, including surgical hospitals. This concern has caused hospital associations at the national and state level to seek legislative and regulatory relief against physician-owned facilities, which sometimes includes ASCs.
Congress recently imposed an 18-month moratorium against new specialty hospitals and limited expansion of existing ones retroactively beginning Nov. 18, 2003.
The moratorium on specialty hospital development is counterproductive, anticompetitive, restricts patient choice, and harms the nation's health care system, according to Michael J. Lipomi, MSHA, president of the San Diego-based American Surgical Hospital Association.
"The moratorium itself is based on misinformation provided by hospitals, health care systems, and their associations to protect and preserve their monopolistic strangle hold on the health care system to the detriment of the patients," he explains. The United States needs a system that encourages competition and innovation, Lipomi says. "Specialization improves patient care, lowers costs, and increases quality and patient satisfaction," he adds.
Surgery center leaders are swift to criticize the regulatory and legislative restrictions that include ASCs.
"It’s a huge, unnecessary threat to high-quality, efficient, patient-preferred surgery centers," says Craig Jeffries, Esq., executive director of AAASC. In fact, several states, including Massachusetts, are underserviced by ASCs because of the state regulatory burdens to development, he maintains.
Additionally, the response of hospitals is unnecessary because the growth of outpatient surgery provided in hospitals exceeds the growth in ASCs, says Kathy Bryant, executive director of Federated Ambulatory Surgery Association in Alexandria, VA. ASC leaders also point to many successful hospital-ASC joint ventures.
Where will it end? In a worst-case scenario, ASCs potentially could lose their safe harbor protection under the anti-kickback law, Shapiro warns.
Michael Romansky, JD, partner in the health law department of MWE, says there is only a small chance of those safe harbors being lost, but he adds that this was the same prognosis he gave when assessing the hospital industry’s prospects for obtaining a moratorium on surgical hospital development.1
For its part, leaders of the American Hospital Association (AHA) in Washington, DC, insist that they are not targeting ASCs.
"In terms of what AHA has been doing, our legislative agenda in that respect has been focused on the specialty hospitals," says Ellen Pryga, director of policy. However, AHA has brought together state hospital associations to discuss issues that are common, including a meeting on specialty hospitals in fall 2003. She says that ASCs were discussed briefly.
The problem is that some physician-owned facilities, particularly specialty hospitals, have the less complex, better-insured patients, Pryga says.
"When they’re uninsured, or covered by Medicaid, or not paid well under Medicaid, or a more complex patient, they go to community or full-service hospitals," she says. The better-paying patient and the better-paying procedures are the ones that help hospitals cover the ones that don’t have coverage, are Medicaid-reimbursed, or are not fully reimbursed, Pryga points out.
"When it comes to overall viability of including broad range of services and access to the entire community, the proliferation that are very narrowly focused on specific populations and specific procedures, and pulling out only those populations and procedures put the ability to maintain services for entire community at risk," she adds.
The AHA stance is reinforced by the Federation of American Hospitals in Washington, DC. "The [federation] board has talked about surgery centers and given attention to oppose incidents where there are referrals by physicians to facilities where they have an ownership interest," says Richard Coorsh, spokesman. "We believe it increases an unlevel playing field that ultimately is detrimental to patients and other consumers."
ASC leaders are not taking legislative and regulatory threats lightly. They are hiring lobbyists at the state and national level, educating state and congressional lawmakers, and better organizing their state associations.
When the Colorado Health and Hospital Association in Greenwood Village began formulating a bill against physician referral to "limited service hospitals," including surgical hospitals, it spurred the Colorado Ambulatory Surgery Association to become more active, says Rebecca Craig, RN, CNOR, CASC, president of the association and administrator of Harmony Surgery Center in Fort Collins.
"We were afraid that the next thing on the agenda would be for them to say that for physicians to own surgery centers is a conflict of interest," she points out.
The group organized and hired a lobbyist, who was successful in tabling the bill. Now another bill is being developed to prohibit ASCs from obtaining a convalescent care license, which allows extended recovery care with no time limit in Colorado. The ambulatory surgery group is educating state legislators with statistics and benchmarks and providing them tours of ASCs to demonstrate the quality of care.
"I think [ASCs] will continue to grow in the state of Colorado, due to the quality product we have to offer," Craig says. "I think that will speak for itself. But of course, we’re going to have to continue to fight for the ability to do that."
In terms of future scrutiny, ASC leaders don’t expect much more to come from the Medicare Payment Advisory Commission (MedPAC), despite the fact that at MedPac’s January hearing, a commissioner asked whether physician investment in ASCs should be scrutinized.
"They may discuss it some more, but my guess is that it’s not an important policy discussion," Jeffries says.
In fact, MedPAC’s recent report to Congress did not address physician ownership of ASCs.
In the meantime, hospitals and ASCs need to work together to meet the surgical demands of tomorrow’s patients, Bryant maintains. "One study is predicting 15% growth in ophthalmic surgery by 2010, and by 2020 a 47% growth, which is incredible,"2 she says. "If those kinds of estimates are true, we needs lots of growth to meet those needs."
Physicians, hospitals, and ASCs should have discussions on how to meet increasing demands, Bryant notes. "Hospitals are going to need ORs to meet growing inpatient demands," she says. "I think, based on the procedures we can do in ASCs, the overall population will benefit."
However, in the short term, don’t expect hospital groups to stop pursuing legislative and regulatory restrictions against physician-owned facilities.
"I think the issues that we’re all dealing with are intensifying not diminishing," Pryga says. "I would guess [future restrictions are] probably a safe bet."
References
1. Conn J. Hospitals moving aggressively against surgery centers: AAASC. MP Stat, March 4, 2004. Web: www.modernphysician.com.
2. Etzioni DA, Liu JH, Maggard MA. The aging population and its impact on the surgery work force. Ann Surg 2003; 238:170-177.
County commissioners in Sheridan, WY, are seeking a moratorium on ambulatory surgery centers (ASCs) after the hospital and physicians planned competing facilities.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
